In jeans and a sweatshirt, 10-year-old Trent Ahlefeld hardly looks like a man of mystery.
But his heart, that’s another story.
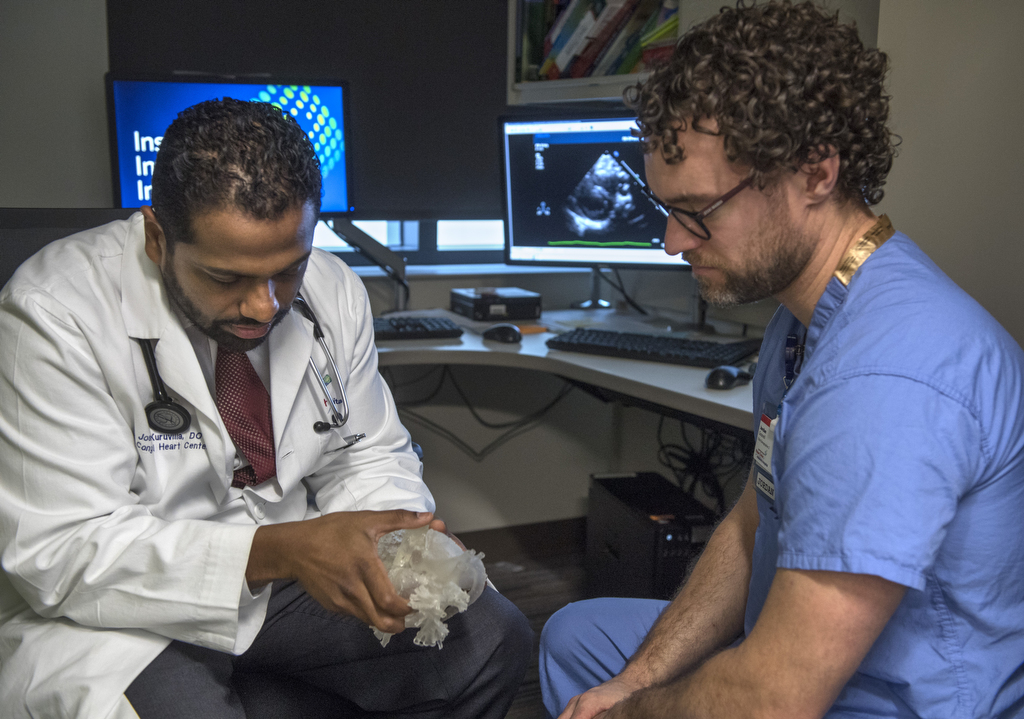
“It’s always been a mystery to a lot of people,” said his pediatric cardiologist, Joseph Kuruvilla, DO.
That’s why Trent was one of the first patients to have a model of his heart created by the new 3D printer at the Congenital Heart Center at Spectrum Health Helen DeVos Children’s Hospital.
When Trent came in for a recent doctor’s appointment, Dr. Kuruvilla picked up the clear plastic model from the counter and held it out.
“That’s your heart,” he said. “That’s what it looks like. It’s a very special and very unique heart. You should be proud of it.”
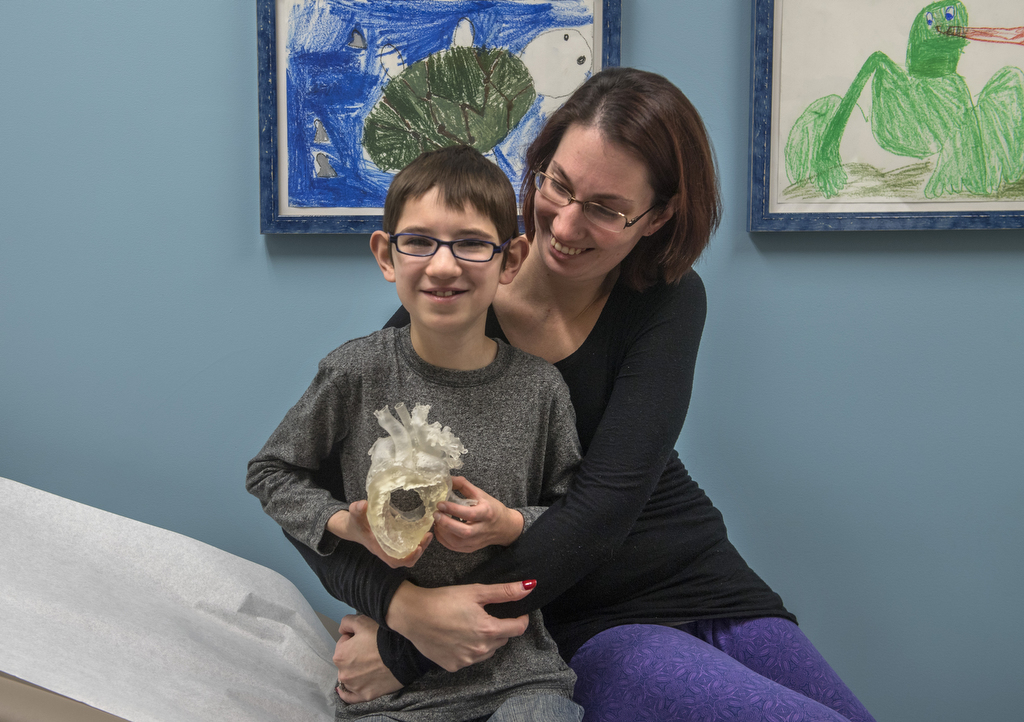
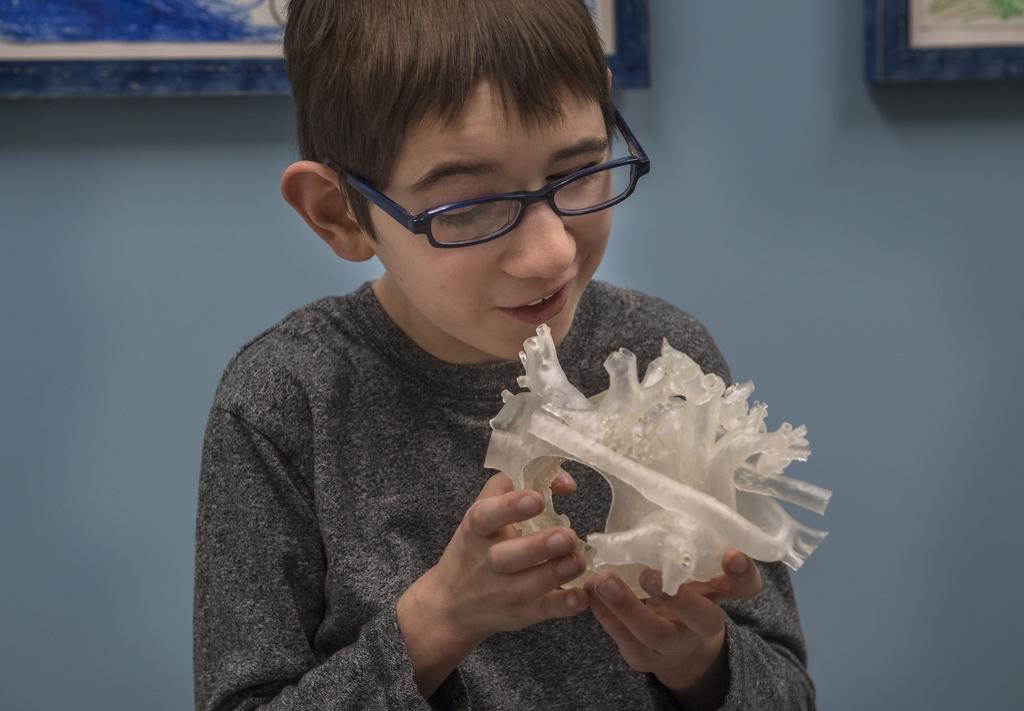
Trent grinned and cradled the chunk of plastic against his chest, right in front of the spot where his real heart beat.
“I really like it,” he said, tracing a finger along the outside. “It feels smooth. And kind of rough.”
The model had just emerged from the printer that morning.
“This is fresh. Hot off the press,” Dr. Kuruvilla said.
He removed the cutaway windows and showed Trent the hole in the wall dividing the left and right sides of his heart and the valve that regulates blood flow between the upper and lower chambers. He showed him the stents doctors placed in his veins when he was younger.
And he pointed out the dilated main pulmonary artery that emerges from the heart and how it branches into smaller and smaller blood vessels carrying blood to the lungs.
“Tiny, tiny, tiny,” Trent marveled.
The 3D model, as captivating as it was for Trent and his mom, has a serious purpose for the doctors involved in his care, helping them determine the best treatment for the unique challenges of his heart.
“It’s not just the awe factor,” Dr. Kuruvilla said. “That exists, too. But this is incredibly useful.”
Creating the model involved a team of experts, including Joseph Vettukattil, MD, an interventional pediatric cardiologist who has done pioneering work with 3-D heart models.
41 hours to print
The pediatric congenital heart center has used an outside vendor for the 3D printing in the past. But it recently acquired its own printer so it could print hearts for more patients and at a far lower cost.
A patient’s family donated the funds for the $3,500 printer, allowing the doctors to print a clear heart model for about $75. Previous models, which include color, cost several thousand dollars apiece.
The model can be prepared using CT, MRI or ultrasound scans or a combination of them called integrated 3D printing, a technology developed by the team at the congenital heart center. For Trent, the team used a CT scan, which shows the anatomy of the heart in multiple planes.
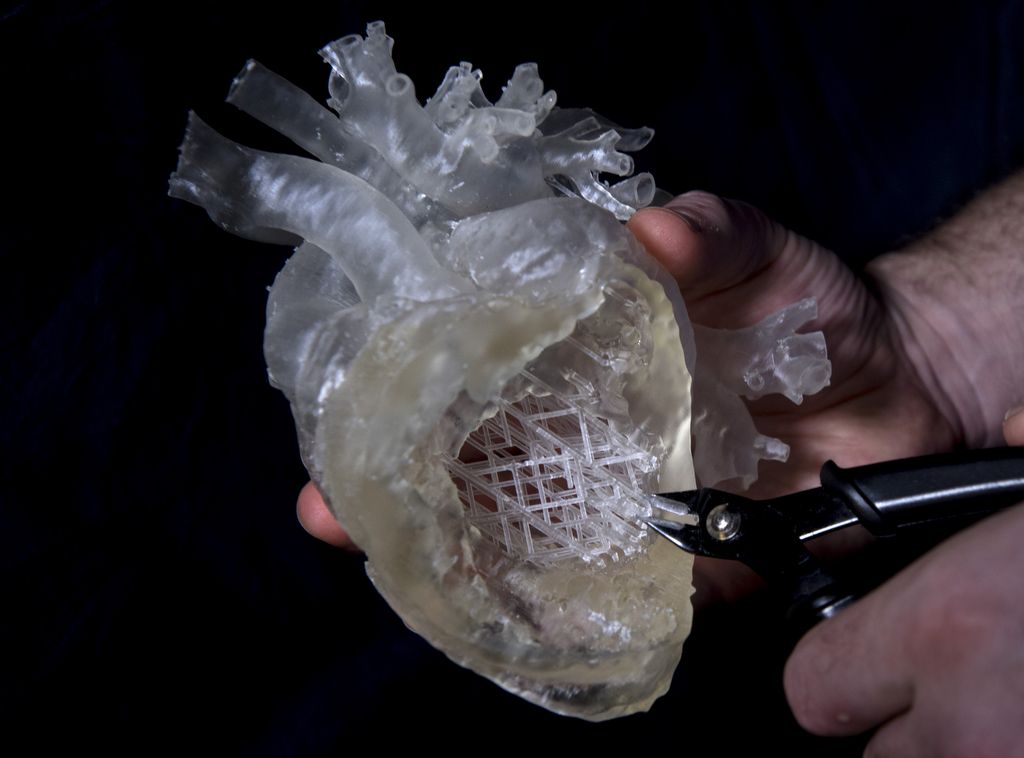
Cardiac sonographer Jordan Gosnell did the computer work, segmenting the areas of focus and putting them together in a model that would be suitable for printing. He also programmed a web of struts to support the model as it emerged from the printer.
Having the printed model of his heart and having the ability to look into the chambers and look at the anatomy carefully, we can now contemplate how best we can help this child.
Once Dr. Vettukattil reviewed and approved the plan, Gosnell hooked the computer to the printer and sent out the file.
The printer looks like an open-ended cube, about 13 inches wide. At the bottom sits a tray of liquid resin.
When the printing began, a 6-inch square plate dropped down into the resin. Light flickered underneath, as a laser created one layer of the model.
The plate rose a moment, then dropped down for the next layer.
In all, the printer created 6,418 layers to build the heart. The process took 41 hours.
After its completion, Gosnell clipped away the strands of the support structure.
“The process can take a while, but it’s really neat. As the struts are clipped away you start to see the heart,” Gosnell said. “Compared to ultrasound, it’s satisfying to be able to hold the work in your hands.”
Life at his own pace
Trent’s parents, who lived in California when he was born, learned about his unusual heart shortly after his birth.
The central portion of his heart did not form completely. Openings existed in the wall that separates the two upper chambers, and between the two lower chambers. Instead of having separate valves on the right and left side of the heart, he had a single common valve.
He is an amazing kiddo. Everyone who meets him loves him. He’s such a positive, caring kid.
His heart also formed on the right side of the chest, instead of the left. And the pulmonary veins that bring blood from the lungs to the heart connected to the right collecting chamber, rather than the left.
The complex challenges make it difficult for his heart to provide his body with the oxygenated blood it needs.
While living in other parts of the country, Trent underwent surgery on his pulmonary veins at 2 weeks old. Then, in his early years, he had several catheterization procedures to provide some relief.
Trent, now a fifth-grader living in Greenville, Michigan, saw Dr. Kuruvilla recently after his heart challenges started to have a bigger effect on his life.
At the beginning of the school year, he began to have more trouble catching his breath with minimal activity. Just a short walk across a parking lot became difficult. At one point, his heart rate shot up to 200 beats per minute.
He underwent a catheterization procedure using tiny balloons to expand his pulmonary veins. That boosted his strength considerably.
During a standard six-minute test, he walked 100 yards farther than he had before, Dr. Kuruvilla said.
His mother, Megan Thompson, admires the way her son bounces back from challenges.
“He just adapts to everything,” she said. “He can ride his bike and play outside. He can handle going up and down the stairs. He is just kind of slower with things he does.
“If we go to zoo and are walking and he gets tired, we stop and wait for him or bring a wagon or stroller.”
Trent also enjoys creative pursuits. He draws. He plays with Legos.
“I build houses for little people and have monsters attack them,” he said.
And he plays with his younger brothers, Aiden, 9, Declan, 3, and Brennan, 2.
With a heart-melting smile and easygoing manner, he wins over anyone he encounters.
“He is an amazing kiddo,” Dr. Kuruvilla said. “Everyone who meets him loves him. He’s such a positive, caring kid.”
Weighing the next steps
Dr. Kuruvilla and the congenital heart team also are exploring other possible treatments for Trent, such as surgery to repair the hole in his heart.
The 3D heart model provides additional insight the doctors can use in deciding the best action to take, said Dr. Vettukattil and Marcus Haw, MD, a pediatric congenital heart surgeon. The physicians are co-directors of the congenital heart center.
“It’s a very complex heart,” Dr. Vettukattil said. “Having the printed model of his heart and having the ability to look into the chambers and look at the anatomy carefully, we can now contemplate how best we can help this child.”
If Trent ends up having surgery to patch the hole in his heart, the model will provide an invaluable preview for the operation.
“All this detail is really, really important and gives the surgeon a heads-up as to what he is going to find,” Dr. Haw said. “This isn’t necessary in every case, but in special cases, it is going to allow us to do more complete repairs than we would have been able to do in the past.
“This technology is amazing.”
A look inside
As Trent marveled at his heart model, his mother and grandmother, Sue Rookus, snapped pictures. Trent took a couple to show his younger brothers.
“This is so cool,” Rookus said.
“I can see his heart racing,” Thompson said.
Thompson recalled how Trent, after his first heart catheterization, studied a booklet about congenital heart defects, trying to understand how his heart worked. It was hard to figure it out.
For Trent, being able to touch a 3D model helped give him a clearer picture of the inner workings of his special heart.
“I always wondered,” he said. “Now I get to see what it actually looks like.”





















 /a>
/a>
 /a>
/a>
 /a>
/a>
Thank you so much for sharing Trents story. This is an amazing and exciting opportunity to have a model Made of his heart.
We loved meeting Trent. He’s a great kid and certainly well loved by everyone who meets him. We really appreciate being able to share his story and the pictures of his 3D heart.
What an amazing story. His 3D heart is incredible!
It is very impressive. Thanks for reading, Pamela.