For Addison Weith, a bright-eyed 6-year-old, every day seems to hold the excitement of Christmas morning.
At least that’s how one of her teachers described what it’s like to be around Addy. Her mom attests that it’s true.
“The smallest things are just so exciting for her,” said Lisa Weith of Hudsonville, Michigan, mother of Addy and her twin sister, Norah.
“She absolutely loves school and everybody loves her—and Norah.”
Though Norah and Addy share a birthday and many of the same traits—brown hair, a sweet smile, and a love for snuggling—the sisters differ in a significant way.
Addy has mitochondrial disease, an incurable inherited disorder resulting from genetic changes in the mitochondria—the part of each cell that generates the energy the body needs to function.
Patients with mitochondrial mutations face an unpredictable future. They experience a range of symptoms in many of the body’s organs.
“We tend to say that (patients with mitochondrial disease) can show up with any symptom in any tissue at any time,” said Stacie Adams, MD, section chief for biochemical genetics at Spectrum Health Helen DeVos Children’s Hospital, who oversees Addy’s care.
“We always have to be on the lookout for new symptoms that could be due to the underlying disease.”
Addy’s mutation, in a gene called MT-ND5, causes symptoms that look like an overlap of two mitochondrial disorders, Dr. Adams said.
The first, called MELAS—short for mitochondrial encephalomyopathy with lactic acidosis and stroke-like episodes—primarily affects the nervous system and muscles. The second, Leigh syndrome, affects the central nervous system and is linked to lesions in the brain.
Addy’s major issues these first six years have been neurologic and developmental—challenges that have done nothing to dim her spirit.
She’s unsteady on her feet. She needs help with writing and other activities. She has a short attention span. She needs her liquids thickened.
So far, she remains free from the heart problems, diabetes and hearing loss that many children with mitochondrial disease experience.
And Addy finds sources of joy every day, whether she’s reading, painting, watching “Daniel Tiger’s Neighborhood” or playing with Norah.
“Out of the blue, she’ll just say, ‘I love you,’ and that might happen 15 to 20 times a day,” Lisa said. “She’s just a true blessing to everyone.”
Early signs
Life didn’t start out easy for Addy.
From the time she and Norah were born, nine weeks early, Addy struggled. Both girls spent a few weeks in the neonatal ICU in Albuquerque, New Mexico—the closest NICU to the family’s home at the time. But while Norah settled in and found her rhythm, Addy couldn’t get comfortable.
“There was just a difference about Addy. She screamed a lot, she just was not happy, she didn’t like to eat,” Lisa said.
“Pretty much her first year of her life she was screaming or she was sleeping—one or the other.”
Her parents, Lisa and Eric, tried everything they could think of to help Addy: swaddling, rocking, feeding in the dark. Pediatrician after pediatrician advised them to wait it out, assuring them Addy would settle down eventually.
When she reached 9 months with no relief in sight, the Weiths pushed harder for answers. At last, a new pediatrician got Addy admitted to the regional children’s hospital, where she would spend the next 17 days.
“The doctors couldn’t calm her down. The massage therapist couldn’t work his magic,” Lisa said.
Ultrasounds and X-rays revealed nothing, yet Addy continued to arch her back and refuse food. Halfway through her stay, doctors placed a feeding tube in her stomach.
The difference that made in her disposition was like night and day.
“Life was pretty much good after that,” Lisa said.
A grim diagnosis
In 2015, after the twins had turned a year old, the Weiths moved to Michigan to be closer to family in Ohio and Ontario.
In her new home, Addy worked with early intervention specialists to address her developmental delays. They noted some ongoing neurologic issues, Lisa said.
“Sometimes she stares off and isn’t focused on anything. She still had feeding issues. There were still a lot of things going on.”
Lisa took Addy to see specialists in neurodevelopment and neurology. An MRI showed defects in her brain stem, but doctors couldn’t yet assign a diagnosis. They favored watching and waiting.
Lisa, however, felt a sense of urgency. A former nuclear medicine technologist, she wanted a medical explanation for her toddler’s symptoms. Following her gut and doing some research, she began to suspect Addy had a metabolic or mitochondrial disorder.
Knowing that genetic testing is the best way to diagnose and categorize such disorders, Lisa got a referral to Caleb Bupp, MD, FACMG, a medical geneticist with the Spectrum Health medical genetics team.
The family arrived at Dr. Bupp’s office with a binder full of Addy’s test results, from birth forward. He listened to their story, understood their concerns and recommended three genetic tests: chromosome microarray, whole exome sequencing, and mitochondrial DNA analysis.
“This combination of testing, done from just a small amount of blood, looks at the genetic code from multiple angles,” Dr. Bupp said. “It looks for missing or extra pieces of genetic information, misspellings or mutations in the DNA or changes in a separate piece of DNA that is contained in the mitochondria.”
Two months later, he called Lisa with the test results.
“He said, ‘Yes, it is mitochondrial disease, and this is the kind that it is,’” Lisa said.
Having an answer brought relief. No longer would she have to question her instincts or wonder about the cause of Addy’s issues.
“It was a big journey,” Lisa said, “but once we got that diagnosis, things completely changed.”
Through a series of twists and turns, she connected with an out-of-state pediatric neurologist who specializes in mitochondrial disorders. He ended up following Addy closely until 2018, when Dr. Adams took over her care locally after arriving at Helen DeVos Children’s Hospital.
Now, with mitochondrial disease in Addy’s chart and Dr. Adams quarterbacking her care, doctors know what to watch for and what questions to ask when Addy gets sick.
Unfortunately, Addy is no stranger to illness. She’s especially susceptible to respiratory viruses.
“When she gets sick, she tends to take longer to recover, needs oxygen for longer or is more likely to be admitted to the hospital during those illnesses. And there’s always this fear that a normal childhood respiratory virus could turn into acute respiratory failure,” Dr. Adams said.
There’s also the risk that the stress of illness could trigger new symptoms of her mitochondrial disease.
All of these risks intensified with the events of 2020.
“We were already concerned about her health before coronavirus,” Lisa said. “When everything got shut down, it was very scary.”
With the onset of the COVID-19 pandemic, the family opted for virtual school and stepped up their health precautions across the board. Eric took a two-month leave from his frontline job to minimize Addy’s exposure.
In the fall, the girls stayed with virtual schooling—kindergarten for Addy, first grade for Norah. Without the face-to-face interactions with other kids, Addy experienced her longest-ever stretch of good health—months on end without even a runny nose.
“Now it’s possible we could go a year without her being sick,” Lisa said. “Keeping her healthy, if we can do that, brings a little bit of hope to her and her diagnosis. Like maybe she will be different than the statistics you read about for her syndrome.”
Dr. Adams longs for nothing less for Addy and her family.
“They’re just the sweetest,” she said.
“We hope that she’ll be stable for a long time.”





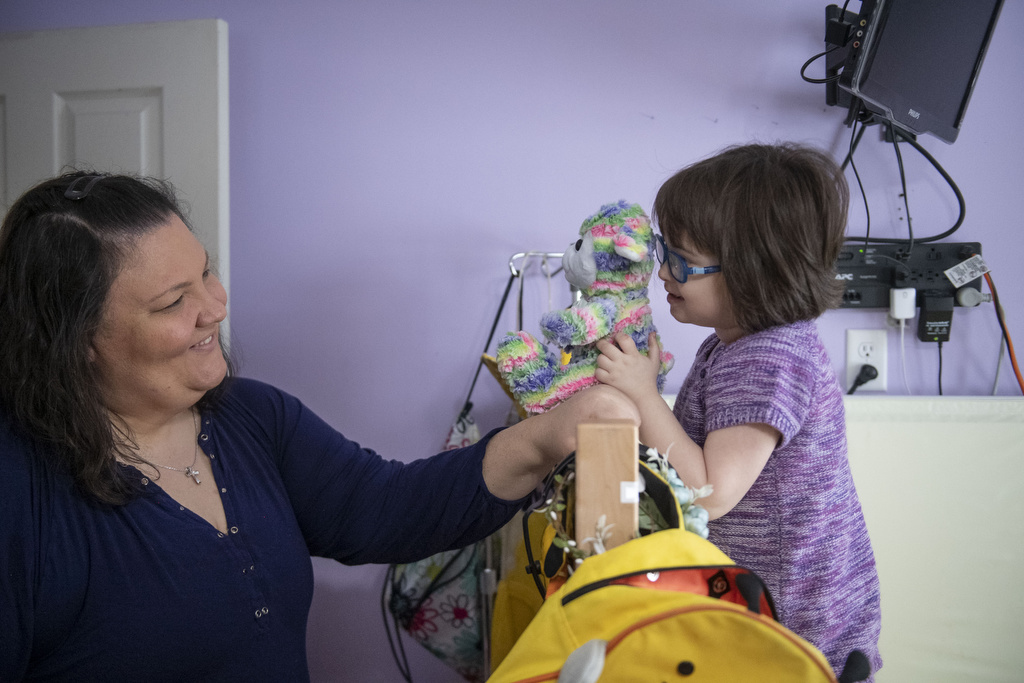
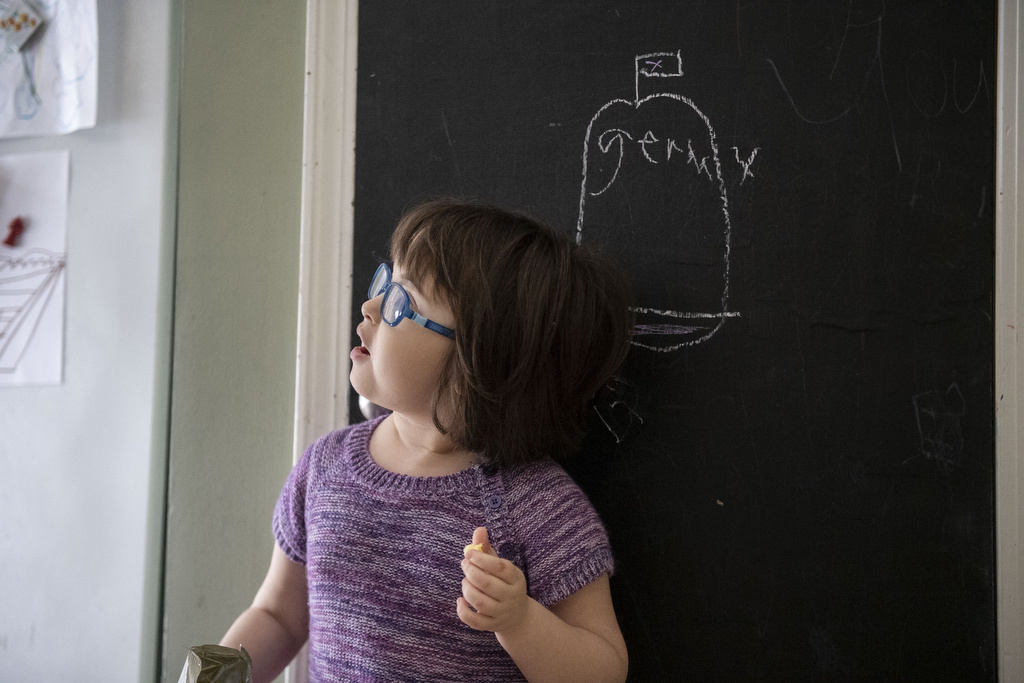















 /a>
/a>
 /a>
/a>
 /a>
/a>
What a beautiful child and amazing family. I pray Addy will remain healthy and happy. Thank you for sharing this story.
ADDY IS OUR MIRACLE GIFT TO ALL OF US .I ALWAYS BELIEVED ADDY WAS GOING TO TEACH THE DR’S ABOUT MITOCHONDRIAL DISEASE.SHE IS A JOY TO BE AROUND AS WELL AS HER SISTER NORAH.LISA AND ERIC ARE FANTASTIC PARENTS.STAY SAFE AND HEALTHY WEITH FAMILYXOXOX
Having worked with Addy while attending PreK, I am totally in awe of Addy, Norah and their parents. I feel very blessed to have the opportunity to spend time helping care for her at school. Sending many hugs, prayers and all my love.
I worked with Addy at a therapy center over the summer. She’s truly a joy to be around.