The words sounded like a death sentence.
When Gary Cunningham’s doctor said he had idiopathic pulmonary fibrosis, he didn’t need to consult a dictionary.
The lung disease killed his mother at age 61.
It killed his grandfather at 63.
Neither lived long after diagnosis.
But even in the shadow of fear, Gary felt a sense of determination rising. He would do everything in his power to beat the odds.
“I made a promise that this disease was not going to take down a third generation,” he said.
“This disease was not going to take me.”
Deep breaths.
They come more easily now.
A new set of lungs, delivered in a transplant performed at the Spectrum Health Fred and Lena Meijer Heart Center, brought the second chance he doggedly pursued for so long.
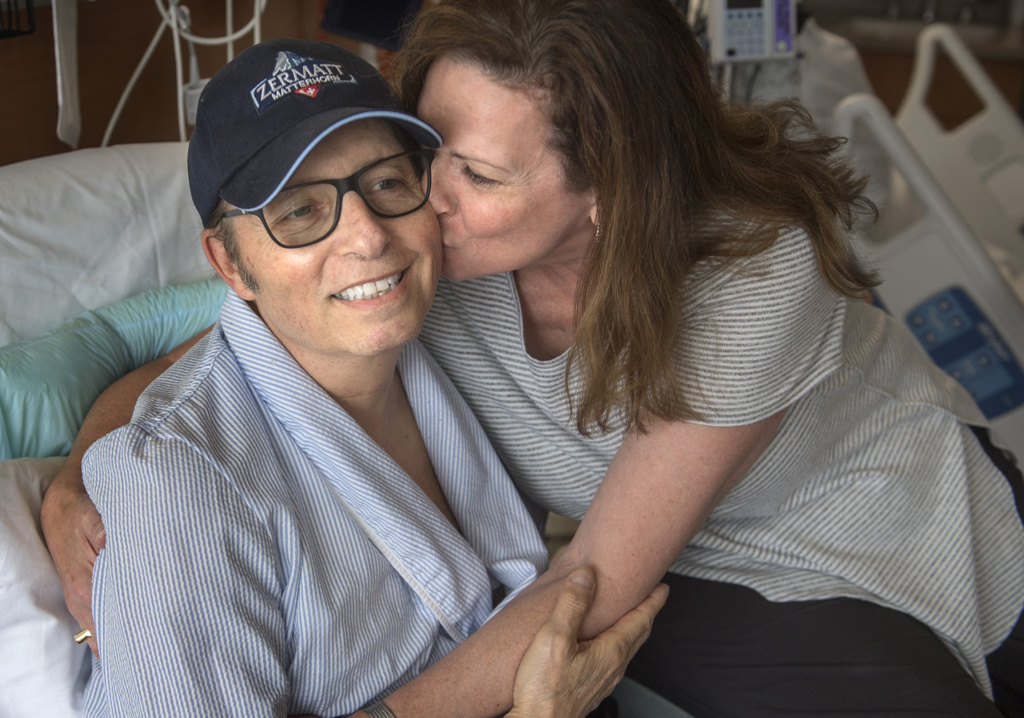
“I am relieved I got it,” he said, sitting up in his hospital room on a sunny summer day, a week after the transplant. “I was going to be dead by Labor Day if I hadn’t.”
His mind reeled with plans for the future—of fun and family and a renewed sense of mission in life.
And also of a letter he planned to write. Words tumbled through his mind—the many things he wanted to say to his donor’s family.
“You can’t even begin to express your gratitude,” he said, his voice filled with emotion. “It’s going to take a long time to compose the words of that letter.
“They will understand how important it was to me to get this transplant.”
The shock of diagnosis
The first signs of trouble showed up in his legs.
Gary, an attorney in the Detroit area, always skipped the elevator and climbed the stairs to his law office. All 10 flights. He wanted to stay strong—to sail, ski, drive fast cars, and in general, to keep up with his three kids.
But when he turned 58, he could no longer make the climb. His legs became weak and wobbly.
Suspecting problems with his circulation, he checked with heart and vascular specialists. But they found no cause in his veins and arteries.
He talked it over with his primary care doctor. When he mentioned his family history with idiopathic pulmonary fibrosis, a disease marked by scarring in the lungs, his doctor referred him to a pulmonologist.
That’s when he heard the diagnosis.
The problem with his legs? His scarred lungs weren’t sending enough oxygen to his muscles.
At home, Gary told his wife, Marianne. They had been married just two years. She had never heard of pulmonary fibrosis or his family’s history of the disease.
What she learned terrified her.
Pulmonary fibrosis kills 40,000 people a year in the U.S. There is no cure. And, at that time, there weren’t even any treatments to slow the progression.
On average, people survive only two to four years after diagnosis.
Marianne and Gary joined a support group for people with pulmonary fibrosis and learned everything they could about the disease.
Pulmonary fibrosis is a broad term that encompasses any disease that involves scarring in the lungs, said Reda Girgis, MD, the medical director of lung transplantation and pulmonary hypertension in the Spectrum Health Richard DeVos Heart and Lung Transplant Program.
Gary’s form of pulmonary fibrosis is called idiopathic, which means the cause is unknown. Researchers are investigating a possible genetic component to the disease.
“It is a distinct entity,” Dr. Girgis said. “Idiopathic pulmonary fibrosis is the most common cause of pulmonary fibrosis. It tends to occur in individuals over the age of 60, but it can occasionally be seen in younger individuals.
“It is a progressive life-threatening condition. Many who have it can be expected to die from it.”
Gary’s family struggled to comprehend such a fate lay in store for their dad.
“He’s the Energizer bunny, all go-go-go,” said his son, Greg. “He’s a fighter, very tenacious.”
But knowing how the disease could progress, he worried whether his dad would survive for the many family milestones that lay ahead.
“I wondered if he was going to meet my children,” Greg said. “I wondered if he was going to meet my wife.”
As his lungs deteriorated, Gary fought six bouts with pneumonia, knowing each one could be a death knell. He kept bouncing back.
He tried to enroll in seven clinical trials, but was denied each time. Because his disease presented in an unusual way—starting with the top lobes of his lungs and progressing downward—he did not fit the criteria for the studies.
When two new medications designed to slow the disease progression received approval, he tried both. He had to stop the treatments because of reactions to the drugs.
As his health declined, he retired from his law practice at age 60. He wrapped up his career with two last jury trials—winning both.
He lost 20 pounds, struggling to keep up with the toll the disease took on his body. For those with pulmonary fibrosis, “their body is working so hard, it’s like running a marathon—lying down,” Marianne said.
But Gary refused to just sit around and wait for death. He did as much as possible, lugging oxygen tanks wherever he went.
He counted his blessings as he lived to witness big family moments. He did meet Greg’s wife—and attended their wedding. He walked his daughter, Stephanie, down the aisle for her wedding.
He and Marianne watched their youngest, Jeffrey Sarazin, graduate from high school and then college. They welcomed six grandchildren.
The couple began to build a retirement home, a condominium in Port Huron overlooking the St. Clair River. They staked their future on hope—that he would outlast his dire diagnosis and live to enjoy watching the boats sail by.
Coming home for a second chance
A lung transplant held the key to long-term survival. Gary knew that from the outset. In 2017, a local hospital listed him on the national transplant list and he began the wait for new lungs.
But to his surprise, the search for new life ultimately led back to where he started—in West Michigan.
A native of Holland, Michigan, Gary always kept close ties with his home base. He followed the growth of Spectrum Health—particularly when it launched the transplant program in 2010 with a gift from the Richard and Helen DeVos Foundation.
Because of his involvement with the Pulmonary Fibrosis Foundation and his leadership in a local support group, he visited Spectrum Health’s support group in its early stages to help out.
By the summer of 2019, Spectrum Health’s lung transplant program had grown steadily—surpassing 150 transplant surgeries.
Gary’s health, in contrast, steadily declined. An episode of pneumonia hit him hard. This time, he could not rebound.
At 66, after fighting eight years to survive, “I was starting to succumb to this disease,” he said.
He contacted Dr. Girgis to see if he could be considered for a transplant at Spectrum Health.
In the next couple of weeks, he underwent testing, became listed for a transplant and assigned a lung allocation score based on the severity of his illness. And he went home to wait.
Less than one month after his first appointment with Dr. Girgis, Gary received a phone call late one night.
“We have a matched set of lungs for you,” a transplant coordinator said.
He and Marianne quickly began the two-and-a-half-hour drive to the Meijer Heart Center, their hearts in a precarious balance between fear and hope.
“It can be such a gift, but there’s a lot that can go wrong,” he said. “We had been down so many dead-ends over the last eight years.
“Marianne and I knew this was our only salvation.”
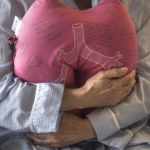
‘That first breath of air’
In the operating room, the surgery was performed by Edward Murphy, MD, the surgical program director for lung transplantation.
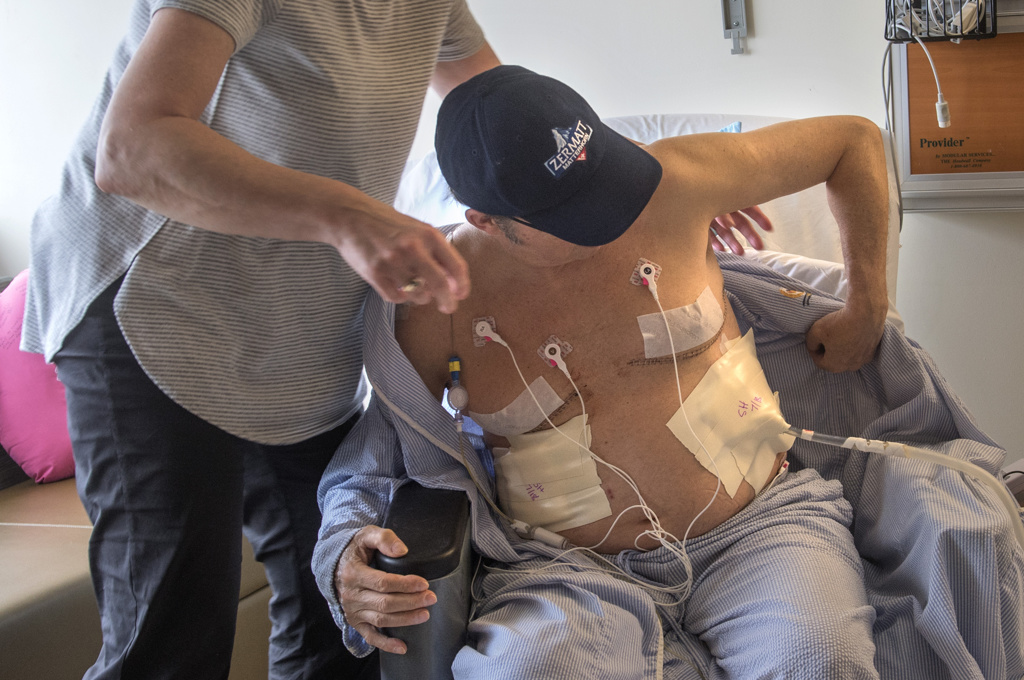
Through 6-inch incisions on each side of Gary’s chest, Dr. Murphy removed the diseased lungs and placed the healthy donor lungs. Once he completed the bronchus, artery and vein connections for each lung, the anesthesiologist inflated it.
“That’s one of the best parts of the surgery: to see that donor lung fill with that first breath of air, knowing what a difference that makes for that patient to now be able to function with a new lung capacity,” Dr. Murphy said.
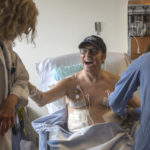
As Gary became awake and alert after surgery, he realized he was breathing easily for the first time in a long time.
“I felt like I did 10 years ago, 20 years ago. Even 30 years ago,” he said. “I felt like I was 16 again and running track for Holland High School.”
Just the sight of Gary’s hands filled Marianne with relief.
“Wow, look at your fingers,” she marveled. “They’re pink.”
For years, his blue-tinted fingertips bore witness to the lack of oxygen in his body.
“This was a real chance at a second life,” Marianne said. “It is such a gift that he received.”
Keeping the lungs healthy
Fourteen days after his transplant, Gary walked into an exam room of the heart and lung transplant clinic. Already discharged from the hospital, he stayed at the Spectrum Health Renucci Hospitality House for a month.
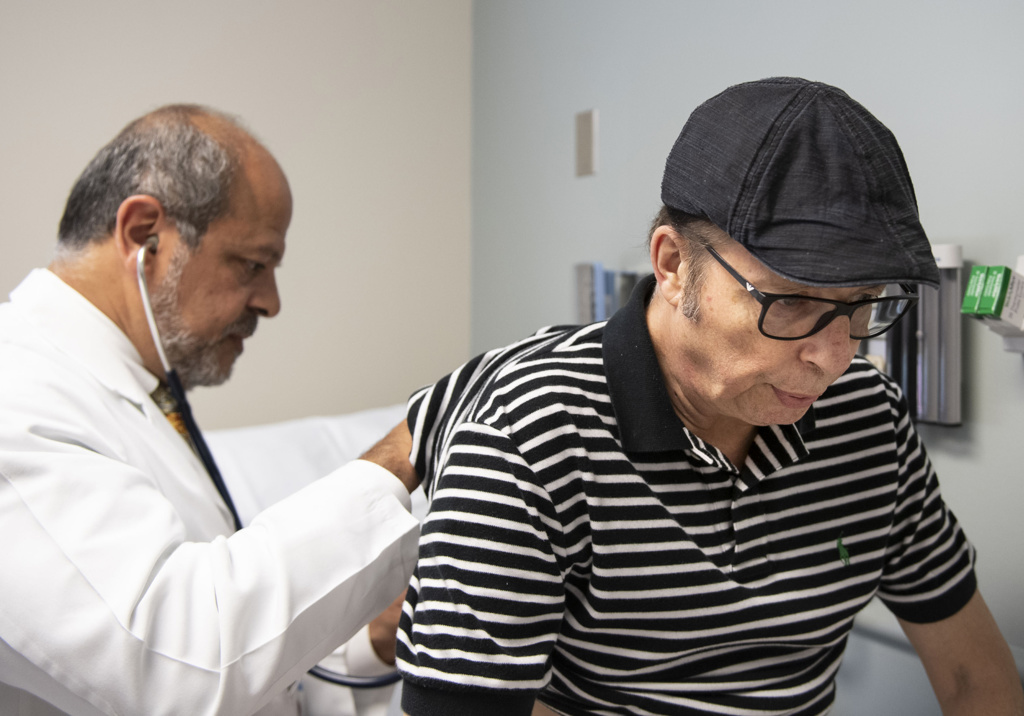
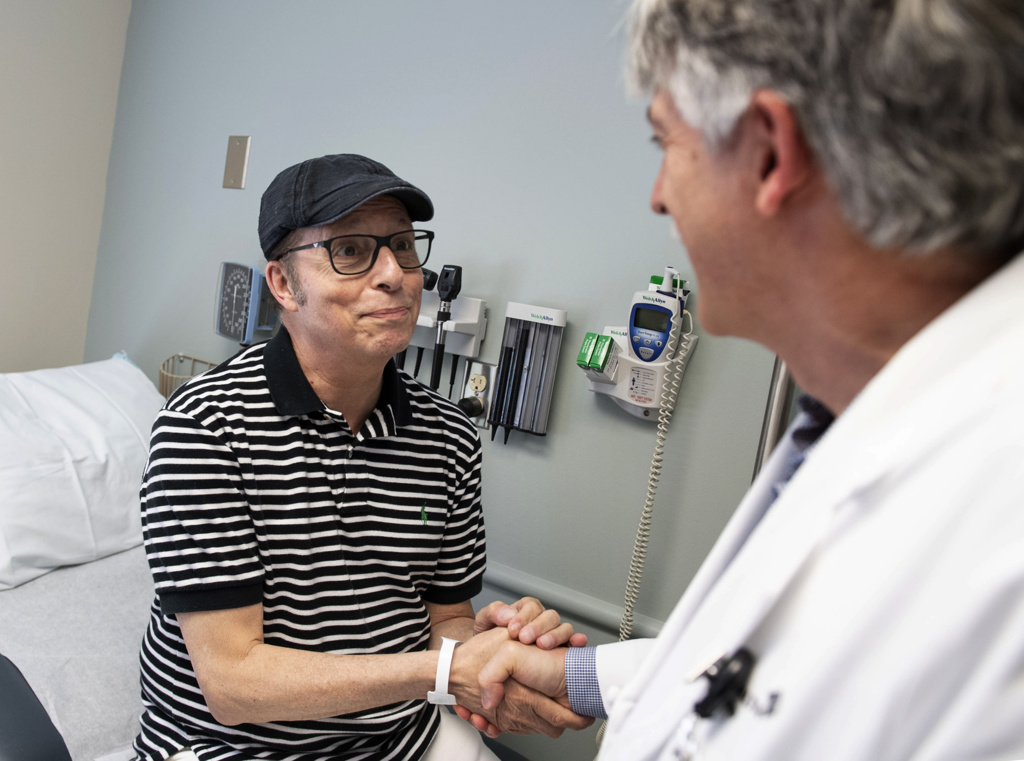
He took deep breaths as Dr. Girgis listened to his lungs.
“You sound pretty clear right now,” he said. “Your lung function looks good. The labs seem to be in order. The X-ray looks good.”
Gary learned how to use a spirometer, a handheld device that measures the volume of air entering and leaving his lungs. Connected to his home wireless device, it will provide daily, real-time monitoring of his lung function for his medical team.
“You’ve got to treat it like a job,” Gary said. “It’s a maintenance job.”
Careful monitoring will be crucial to detect—and treat—early signs of complications, such as rejection or infection, and improve his chance at long-term survival, Dr. Girgis said.
“On average, the outcomes after lung transplant continue to improve nationwide,” Dr. Girgis added.
And at Spectrum Health, the one-year survival rate of 98 percent is the best of the 74 lung transplant programs in the country, according to the national Scientific Registry of Transplant Recipients.
Making that happen takes a team, Dr. Murphy said. In addition to the pulmonologists and cardiothoracic surgeons, the team includes dozens of contributors from the transplant program and the Meijer Heart Center who are dedicated to the preoperative evaluation, intraopereative care and postoperative management of lung transplant patients.
“The reason for the success of a program like this, that is really maturing, is that everyone is working at a very high level,” he said.
Spectrum Health’s transplant team has performed transplants on patients turned away by other centers, Dr. Murphy added.
“Some programs won’t do lung transplants on somebody over 65 years of age, or someone who has had prior coronary artery bypass surgery or who has had prior lung transplant surgery or who has immune sensitization to many possible donors,” he said.
“Since we are comfortable performing transplants on increased-risk recipients, we have a number of patients who have come after being turned down for surgery elsewhere.”
On a mission
With new lungs, new doorways are opening for Gary. He and Marianne plan to finish that retirement home.
He looks forward to gatherings with his children and grandchildren. He has two vintage Jaguars and three antique wooden hydroplanes to restore. He can already foresee family boat races on the river.
“We can have the life we always talked about,” Marianne said. “It’s a renewed hope.”
Gary has no plans to return to his law practice.
“There’s not enough time in the day to go back to work,” he said with a smile.
Instead, he has set his sights on advocacy—for organ donation and to support those diagnosed with pulmonary fibrosis. He plans to lobby for greater awareness and research, pushing for an effective cure.
“This disease kills 40,000 people a year. That’s more than breast cancer, and yet you never hear about it,” he said. “Now, I’ve got a chance to change that scenario.”
“You do have that soul-searching process of ‘What message am I supposed to take from this? What am I supposed to do now?’” he said.
“There is a reason why I’m here. I’ve got to figure that out.”
For Dr. Murphy, Gary’s enthusiasm and sense of mission reinforce the value of organ donation—and admiration to the donors and their families.
“The only option when you have end-stage lung disease is the generosity of strangers,” he said. “Gary has a very keen understanding of what a miraculous gift of life a donation of lungs is.
“It’s a treasure that has been placed in good hands.”



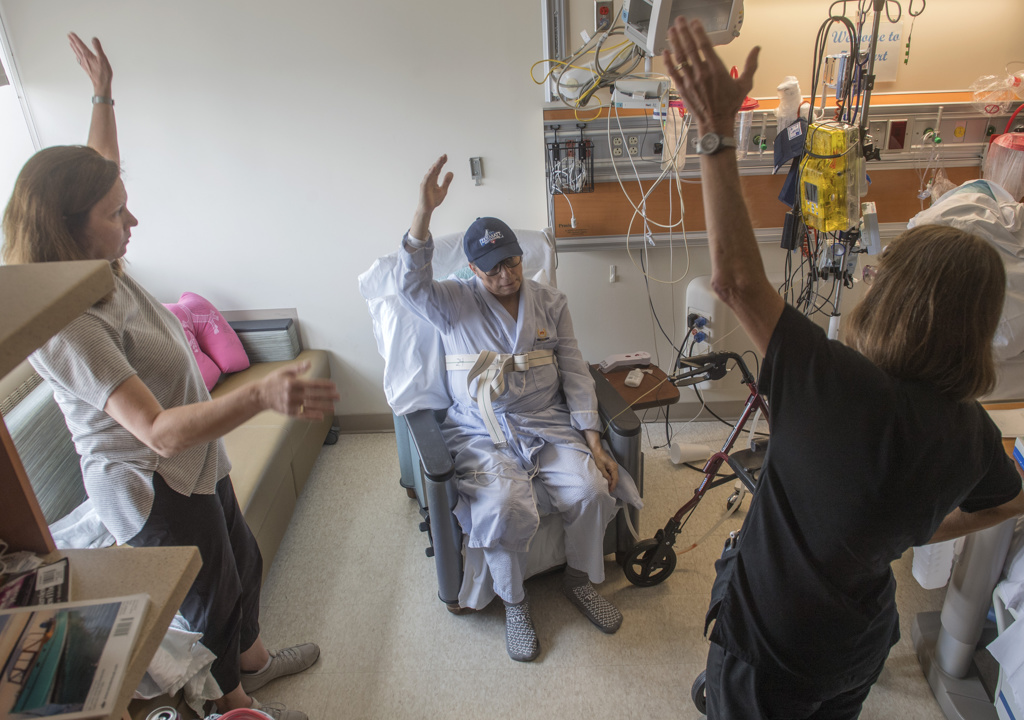

















 /a>
/a>
 /a>
/a>
 /a>
/a>
Such a great story! Praying that he continues to be healthy and strong with his new set of lungs! What a blessing! My 85 year old father currently suffers with idiopathic pulmonary fibrosis and is on Hospice. Wish there was more that could be done for those suffering with this terrible disease.
Melissa- My heart goes out to both you and your father. Having had to watch both my grandfather and then my mother succumb to this disease, I truly understand how difficult it is to have a loved one suffer. That is why I have decided to do even more to raise awareness of pulmonary fibrosis and money to help find the cure. -Gary
Thus is a very uplifting and informative story.
As a long ago retired RN, I was not aware of the huge incidence of this disease and we do not hear about it!
Spectrum Hospital is awesome ! We are so fortunate to have it in this area.
Congratulations Gary – we are so grateful for your kind sharing of both your story here, as well as your involvement with and support of the Grand Rapids Pulmonary Fibrosis Support Group: we are grateful for your support and compassion!
Thanks Jen. There is no doubt in my mind that Spectrum Health saved my life. The quality of care I received during my six-week stay was superlative. Each and every member of the medical staff and all the support personnel went way beyond the call of duty on a regular basis for me. And I observed the same high level of compassion and professionalism directed to all the other patients in the hospital. Please keep up the good work! -Gary
Proud to have been a part of the start of this great transplant team. Not surprised the outcomes are great; great surgeons and the entire team work well together. Keep up the great work!
I have Pulmonary-Fibrosis and have been referred to the transplant team in GR and Dr. Girgis. I am not currently on the list due to my weight and on Blood thinners, however, I have meet with Dr. Girgis and now I have lost enough weight to be qualified for the list and in January it will be 6 months on blood thinner and have a great chance to be able to stop taking it. my heart was jumping for joy when I heard his story. It gave me hope. I am worried for my wife, she is going through this with me. Her comments were: “we are suppose to grow old together, you promised me.”
Thank you, John, for sharing. We are so happy to hear that you found hope in our Health Beat story, and that you’re on a good path to be able to keep your promise to your wife. We wish you the very, very best and will be thinking of you both. Cheryl Welch, Health Beat Editor
You have always been a fighter,way back to traverse city and ann arbor.so glad to hear you are doing better.never give up.
Aunt Dianne, Gary’s sister?