Having a baby in a veterinary clinic did not factor into Kelly Dykstra’s birthing plan.
But that’s where she was on a September morning—at Cedar Animal Hospital, where she works as a vet technician—when she suddenly felt “kind of off.”
She went to the bathroom and, moments later, gazed in shock at the infant son she had just delivered on the floor.
Elliot Albert Dykstra, born three months early and weighing a pound and a half, opened his left eye and looked up at his mom.
“He was tiny. He was just so small,” Kelly said. “But he was awake and he was peeking at me.”
That’s Elliot. A boy full of surprises. From day one.
It’s almost like a miracle, because he had such a severe heart defect with so many (other) conditions.
Elliot had a rare congenital heart defect called transposition of the great arteries. The two major vessels that carried blood from his heart were switched.
He charted a rocky path for months. And through those struggles, he cast a net over his parents’ hearts—no surprise there—drawing them in with a bond of love as sweet and clear as that first eye-to-eye moment.
Exactly 10 months after his birth date, Elliot left Spectrum Health Helen DeVos Children’s Hospital for the first time. He went home on a summer day, a chubby-cheeked baby dressed in an outfit as blue as the sky that smiled down on him.
And he boasted a special claim to fame. He is the smallest-born survivor of transposition of the great arteries, said Marcus Haw, MD, FRCS, his pediatric cardiothoracic surgeon and co-director of the Congenital Heart Center at Helen DeVos Children’s Hospital.
“It’s almost like a miracle, because he had such a severe heart defect with so many (other) conditions,” said Christopher Ratnasamy, MD, a pediatric electrophysiologist. “I think it’s just a testament to the medical technology and the medical care.”
Elliot’s journey from surprise preemie to smiling baby boy involved an intricate balance of medication, surgery, high-level neonatal care, doting parents and the prayers and hopes of a wide circle of friends and family.
‘A fishing buddy’
Kelly and Nick Dykstra, who live in Cedar Springs, Michigan, recalled the day Elliot made his debut.
He arrived so quickly, Kelly didn’t even feel any labor pain. From the bathroom floor, she grabbed her phone and called the front office. “You need to come help me,” she said.
The bathroom filled with staff members. They wrapped the newborn boy in the warm towels they keep on hand for animals born by cesarean section. They used a tiny suction device to clear mucus from his throat while they waited for the ambulance to arrive.
Although neither the time nor place factored into Kelly’s birthing plan, she was grateful to be surrounded by medical professionals trained in the care of small creatures. If Elliot had arrived a bit later, she might have been on her way home from work, and delivered her baby alone on the side of the road.
Giving birth in an animal hospital “was the best of the worst-case scenarios,” she said.
As she rode in the ambulance to the hospital, she called her husband, Nick, to give him the news.
A mason, Nick was working inside a chimney, 20 miles away. He took a short break and went to his truck, just in time to receive Kelly’s phone call. He couldn’t hear much over the noise of traffic, but he heard the word “he.”
That’s how he learned they had a baby boy.
“I thought, ‘I’ve got a little fishing buddy,’” he said.
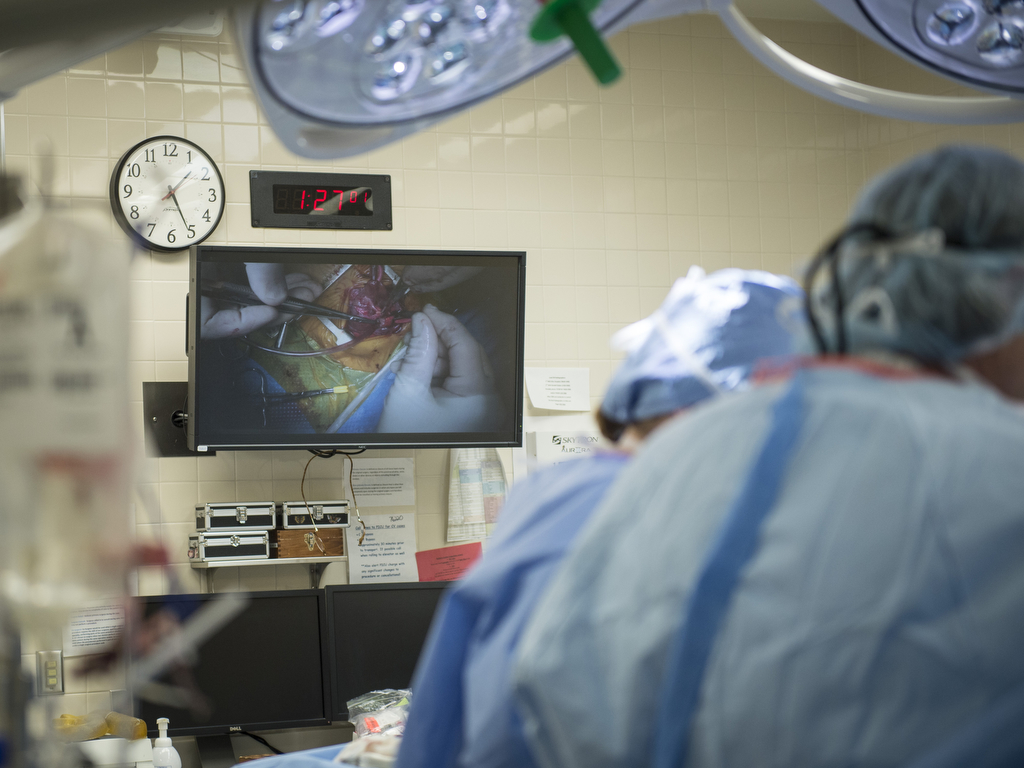
Nick hurried to Helen DeVos Children’s Hospital and watched as the ambulance arrived.
“The EMT was running in, carrying him like a football, yelling off vitals as he came in,” he said. “I was trying to pull out every bit of information I could. There was so much going on, we didn’t have time to be scared.”
Elliott, born at 26 weeks gestation, weighed 1 pound, 11 ounces. His birthday—Sept. 6, 2016—was the day after Labor Day.
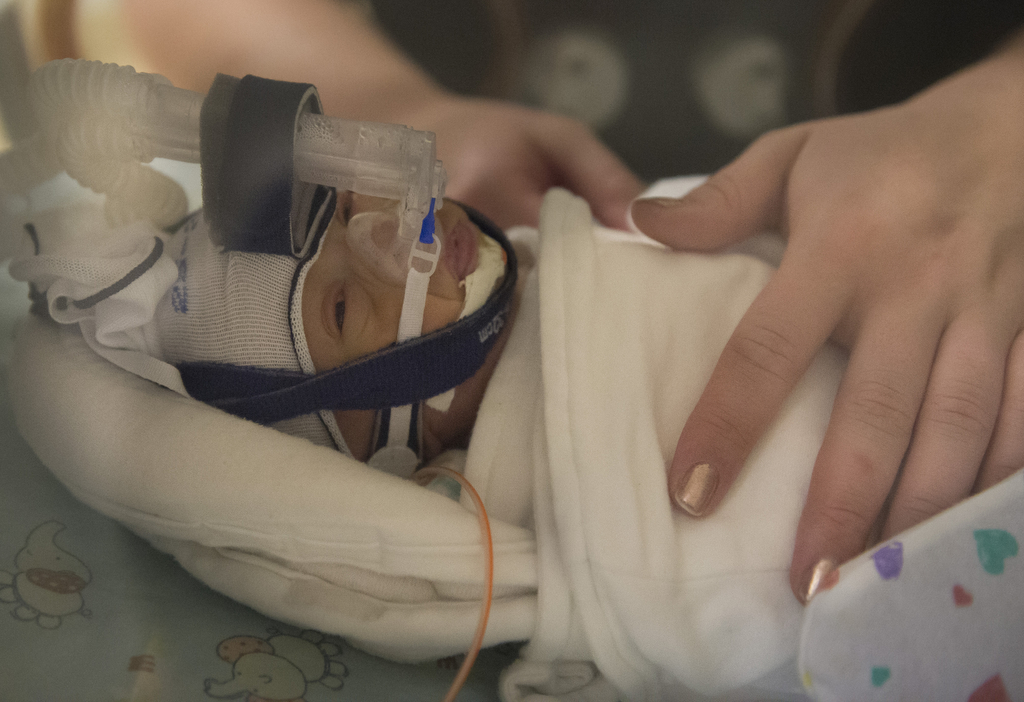
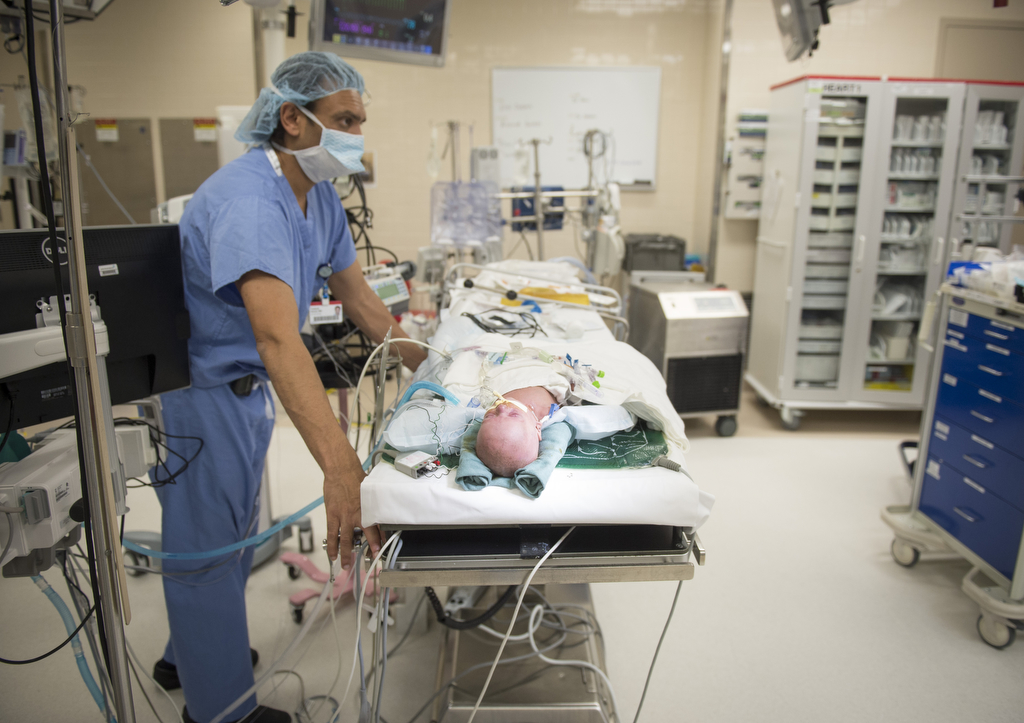
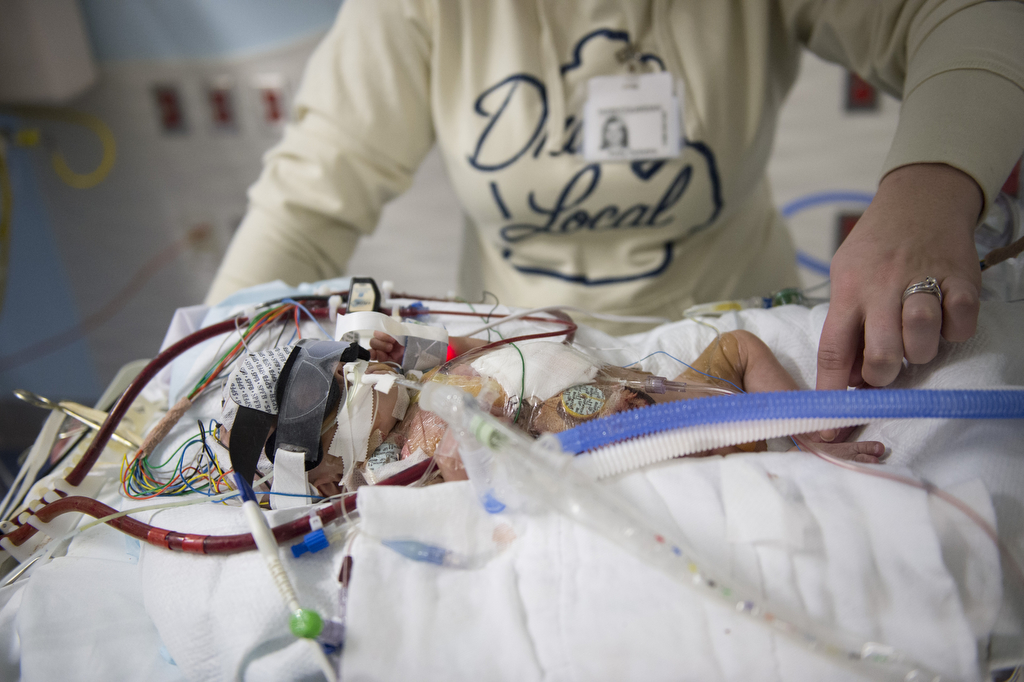
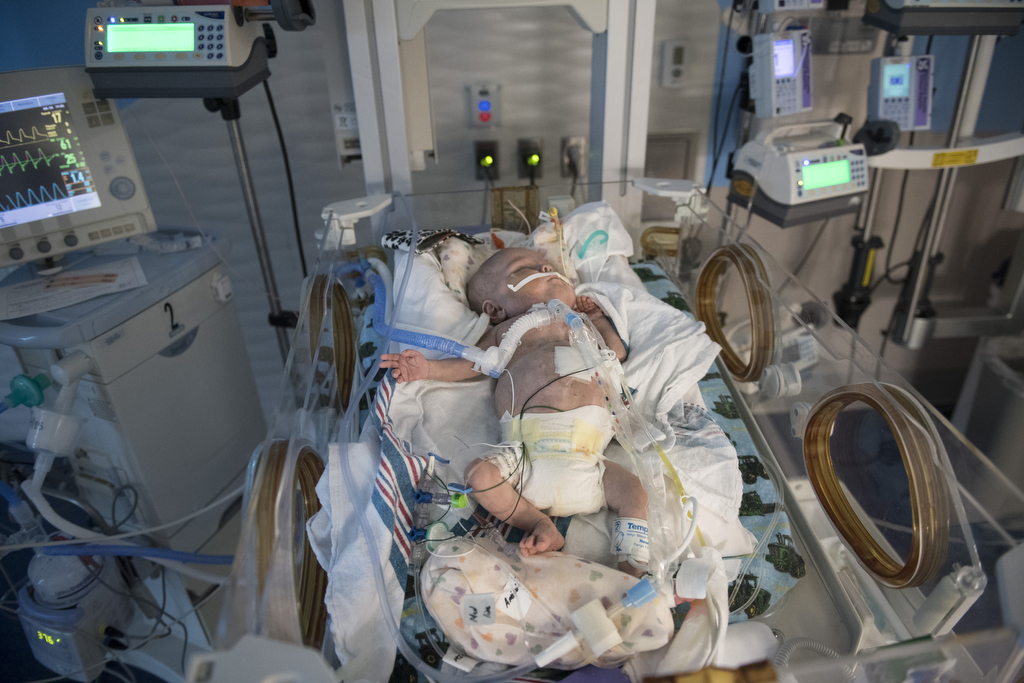
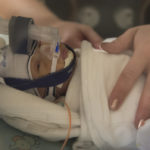
He spent his first weeks in the Small Baby Unit, an area of the Neonatal Intensive Care Unit devoted to the tiniest of preemies. Neonatal physicians and nurses provided the medication, nutrition and oxygen he needed in a warm, quiet environment that simulates the womb.
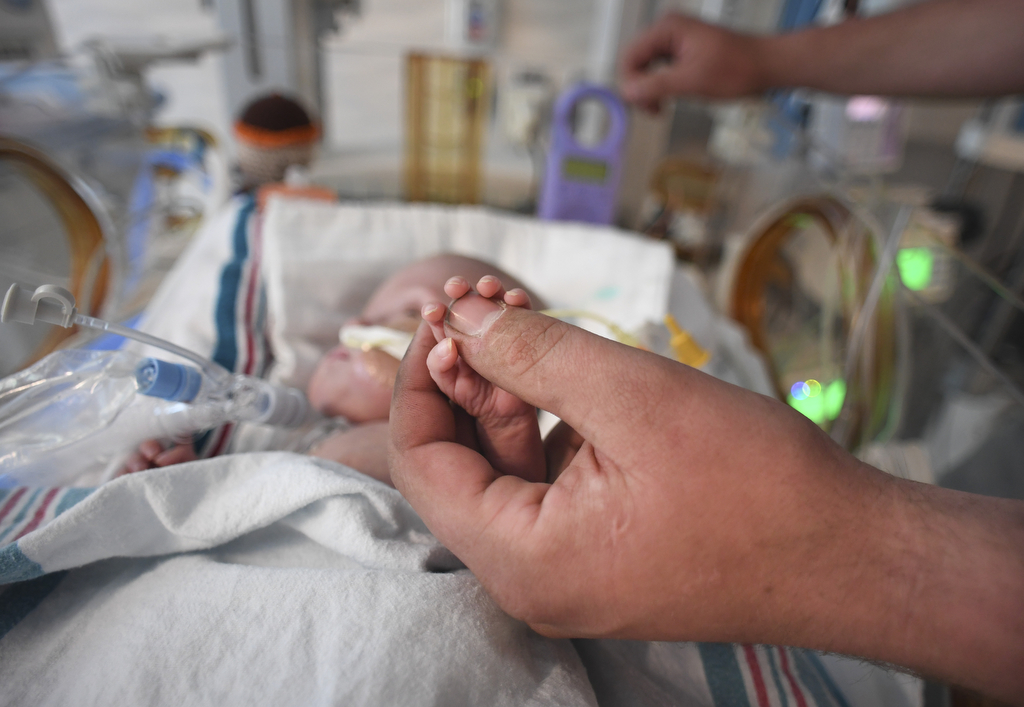
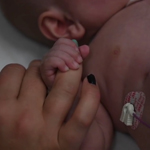
In his incubator, surrounded by tubes and wires, he looked especially tiny.
Nick slipped his hand beside his son, and Elliot wrapped both hands around his dad’s thumb. The teeny hands didn’t even cover the thumbnail.
At first, Kelly and Nick hoped Elliot would make it home by his due date, Dec. 13. Or at least by Christmas.
And that might have happened, if prematurity and low birth weight were his only challenges.
But a week after his birth, an echocardiogram revealed Elliot’s congenital heart defects. In addition to transposition of the great arteries, he had a hole in the wall that separates the two ventricles—the heart’s pumping chambers. And a hole lay between the left and right atrium—the collecting chambers.
He had only one coronary artery—instead of two—supplying blood to the heart.
All his medical challenges, combined with his prematurity and low birth weight, made Elliott’s condition “probably the most complex I’ve seen,” Dr. Ratnasamy said.
So small and fragile, Elliot needed to grow before he could undergo surgery to fix his heart defects.
An emergency procedure
His parents settled in for a longer stay. They worked together as they juggled jobs and parenting duties, and tried to be with Elliot as much as possible.
It wasn’t easy. Nick worked as a mason, tended bar part-time and studied for a degree in informational technology. Kelly worked full-time at Cedar Springs Animal Hospital.
But they relied on a sense of teamwork built in the eight years since they first met, at a church youth group in Sparta. Both 25 years old, they had been married three years when Elliot made his early arrival.
Kelly’s knowledge of medical terms, from work and training, helped her grasp the complexities of Elliot’s condition and treatments.
“We definitely have a lot of support from our families and our church,” Nick added.
Elliot reached a crisis point on Nov. 4, just before his 2-month birthday. The oxygen level in his blood dropped dangerously low.
Joseph Vettukattil, MD, an interventional cardiologist and co-director of the Congenital Heart Center, performed an emergency catheterization procedure, using a balloon to enlarge the hole between the atria. The larger opening allowed blood from the two collecting chambers to mix—a temporary fix that boosted Elliot’s blood oxygen level.
Six weeks later, he performed the procedure a second time.
Elliot’s weight inched upward.
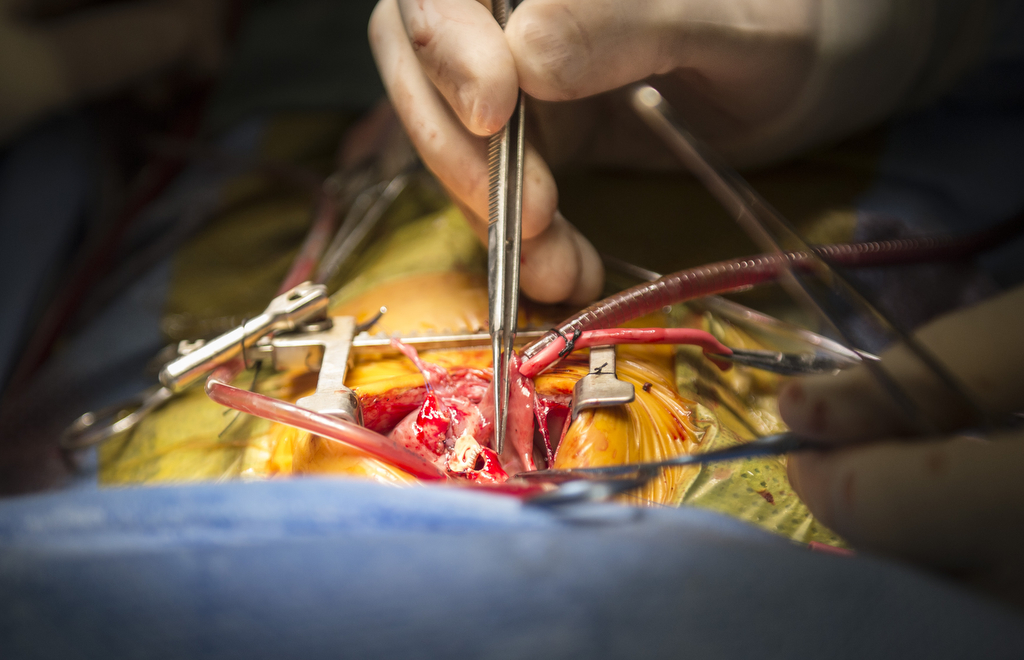
At last, on Jan. 4, with his weight a little over 5 pounds, his medical team prepared him for open-heart surgery. Dr. Haw performed the operation to switch the great arteries and close the holes in Elliot’s heart.
Even when he made it past that hurdle, Elliot still needed intensive care.
He had chronic lung disease and atrial tachycardia, an abnormality in the pattern of the heartbeat. He went into cardiac arrest one day. On another day, he suffered a stroke.
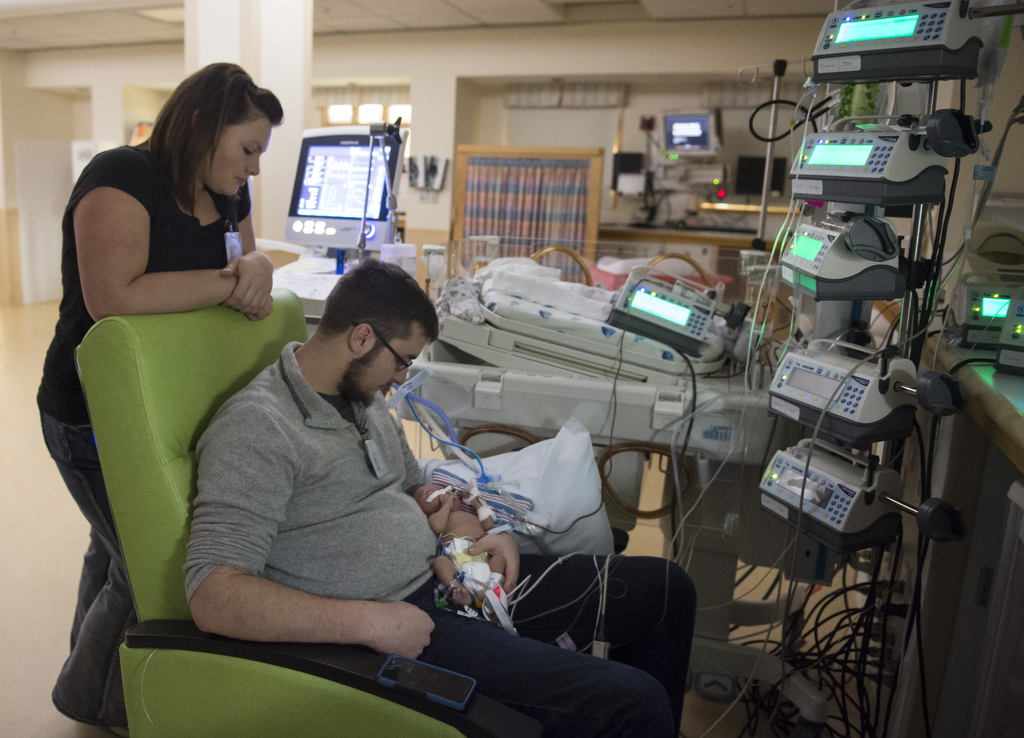
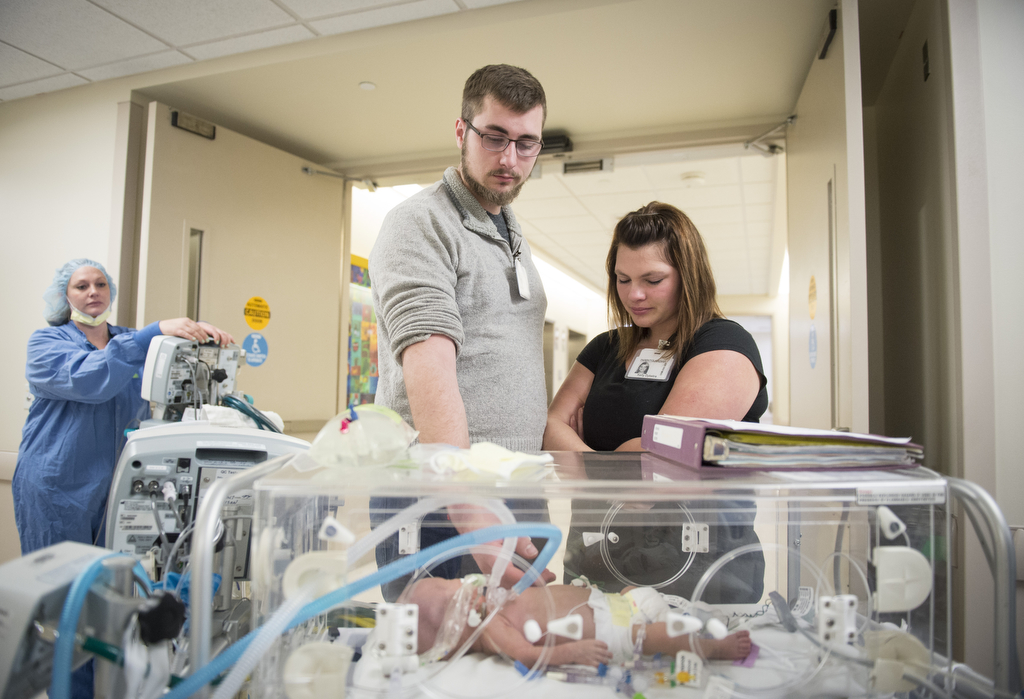
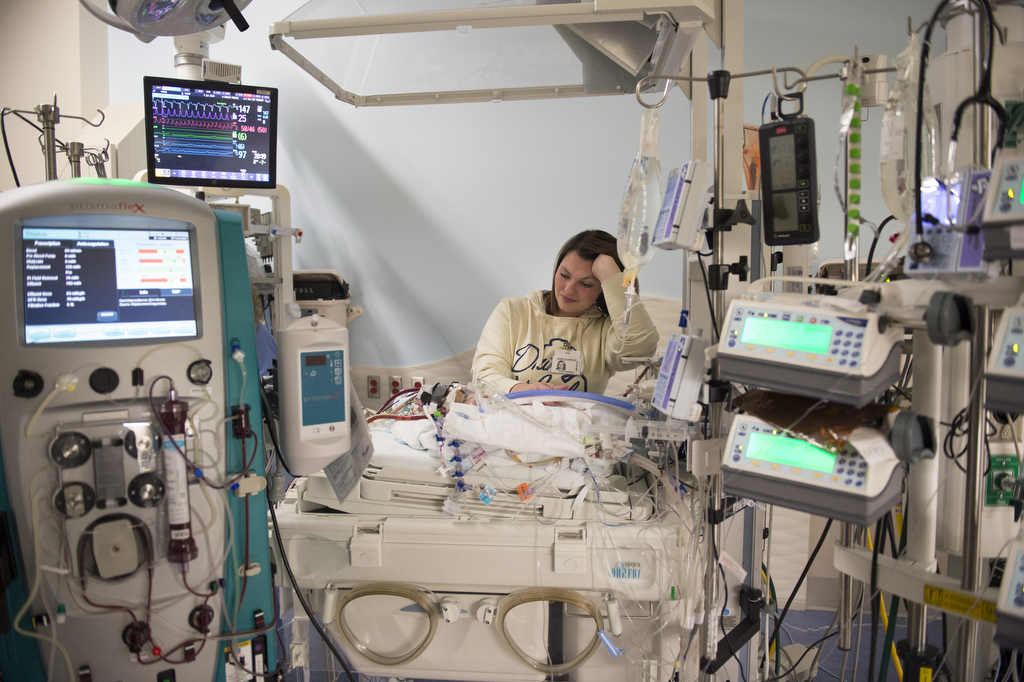
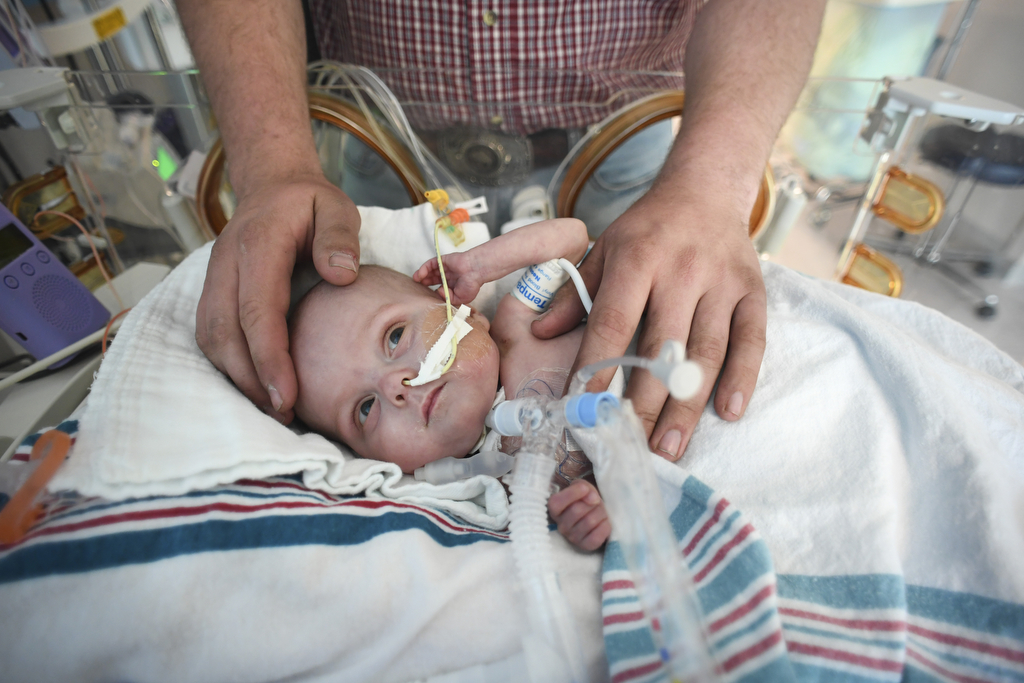
For the next five months, his parents continued their daily treks from Cedar Springs to Grand Rapids to care for him in the pediatric ICU.
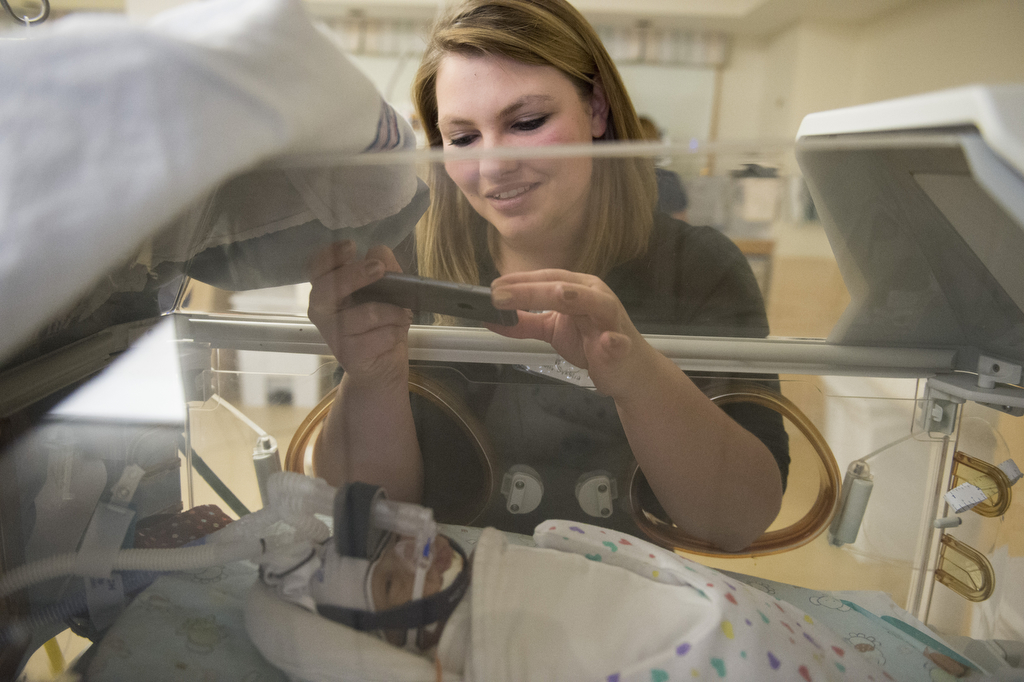
With help from nurses, they lifted Elliot from his crib and held and rocked him. They sang to him. They read books. They documented every day’s progress with photos posted on Facebook.
With their little spare time, they finished the nursery at home. They placed new flooring, assembled a crib and painted the walls.
And they dreamed about Elliot’s future. Nick looked forward to the day he could take his son fishing.
“My grandparents have a farm. He’s going to be throwing hay bales someday,” Kelly said. “Hopefully, he will get into 4-H.”
Grandma time
Shortly after his 7-month birthday, Elliot reached a big milestone: He met his grandmothers.
Nick’s and Kelly’s parents had been visiting him since birth. But on April 24, 2017, they at last had the all-clear to hold him.
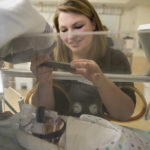
Kelly’s mother, Laurie Pant, sat in the rocking chair as a nurse carefully lifted Elliot from his crib and set the baby in her arms, guiding the tracheostomy tube and IV line to one side.
“It’s been such a long wait,” Pant said. “It just makes it real. Another step toward normal.”
She cradled Elliot, who now weighed 7 pounds.
“He’s a nice little armful,” she said.
Nick’s mother, Lora Dykstra, had tears rolling down her cheeks when her turn came to hold her first grandchild. She kissed his chin.
“You’ve got your first kiss,” she said. “But get used to it. You’re going to get lots of kisses.”
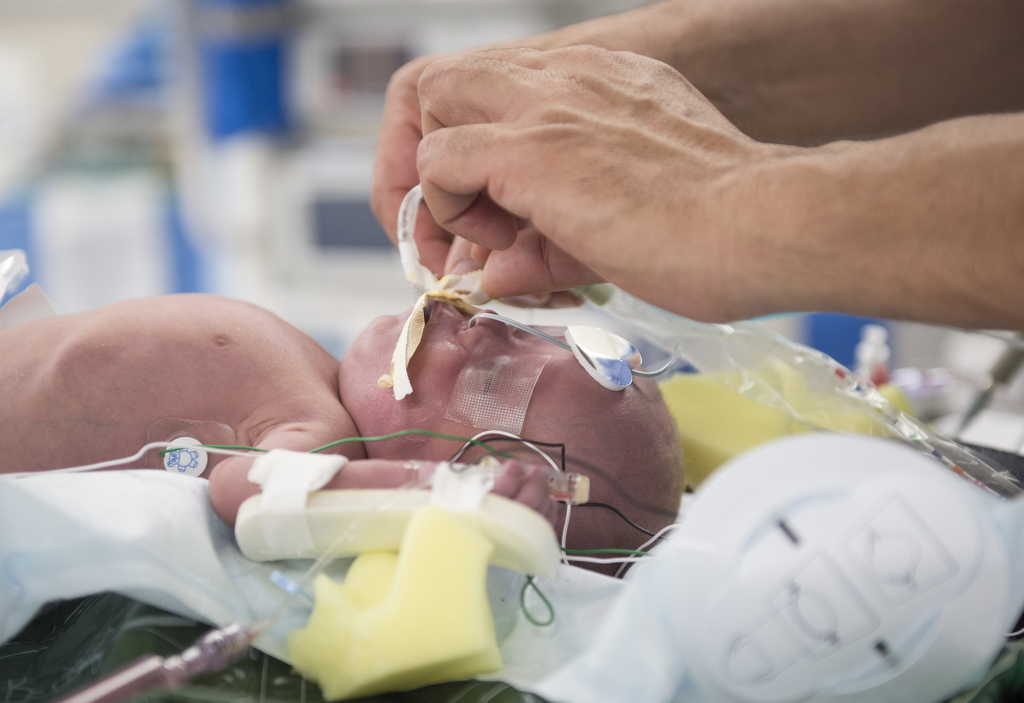
Over the next six weeks, the Dykstras prepared to bring Elliot home, training like athletes for a big race.
They learned to manage the tracheotomy tube inserted through an opening in his windpipe to provide access for oxygen. They monitored his oxygen level, suctioned him when he became congested and fed him through the tube inserted in his abdomen.
On separate days, each parent handled all his medical care for a 12-hour shift.
“It was stressful prior (to that day),” Nick said. “But as soon as we started, it was plenty easy.”
He’s given us a run for our money. He’s a tough cookie.
The day before discharge, Kelly looked back at the past 10 months. Elliot arrived the day after Labor Day and spent all the major holidays of the next year in the hospital—Thanksgiving, Christmas, Valentines’ Day, Memorial Day and the Fourth of July.
“It’s Independence Day,” she said, as she stroked her son’s forehead. “Let’s bust this joint. Are you ready to go?”
Elliot swung his arms and kicked his legs, as if to say a resounding “Yes.”
First time in his own crib
On July 6, 2017—the day he turned 10 months—Elliot left the hospital for the first time. After hugs with nurses and technologists, Kelly lifted his car seat into their pickup, and Nick drove them to their home in Cedar Springs.
The numbers tell only the surface of Elliot’s story, but they are impressive. Altogether, Elliot:
- Spent his first 303 days in the hospital.
- Underwent 11 surgical procedures, including open-heart surgery.
- Gained nearly 11 pounds to reach a weight of 12 pounds, 9 ounces.
- Went home with discharge instructions that included a regimen of 19 medications, for a total of 31 doses a day.
Bringing him through his challenging first months required intense cooperation between a team of experts.
“I think it’s really the fact that we had so many different people involved in his care who worked well together,” Dr. Haw said.
And Dr. Vettukattil credited Elliot’s parents for working with the clinical team while remembering to be mom and dad, rather than another medical provider, to their baby.
“They are lovely,” he said. “They were supporting us in every decision.”
Kelly and Nick look forward to the day they can bring Elliot to his birthplace for a visit. He has become a celebrity to the staff and clients at Cedar Animal Hospital.
His parents have three cats, two dogs and two parakeets, “so he will definitely be OK with animals,” Kelly said.
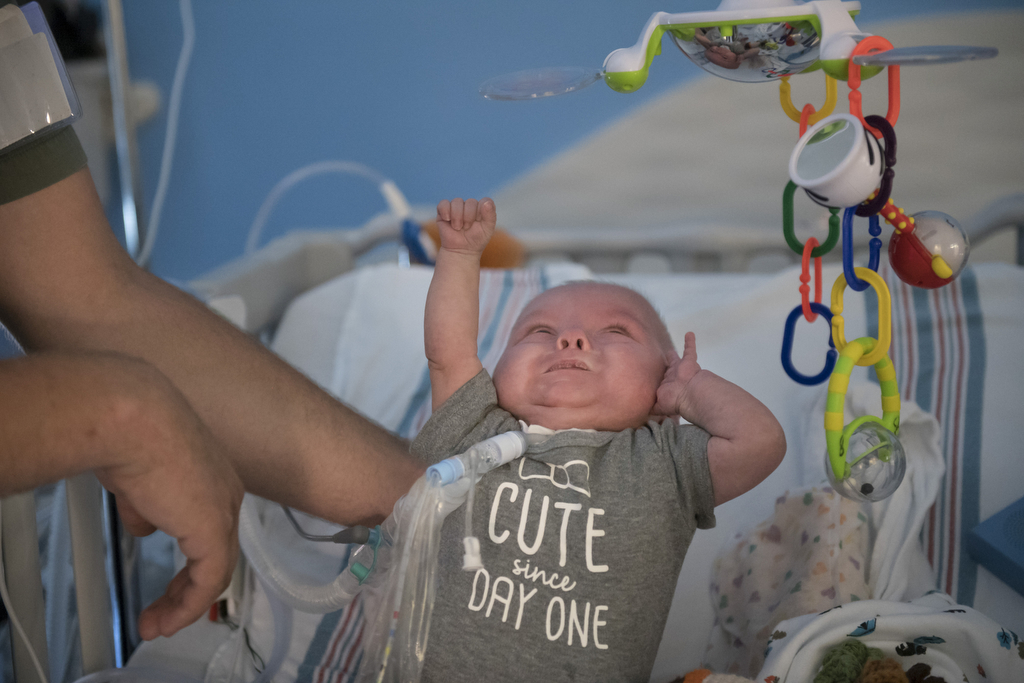
For now, the Dykstras celebrate having their baby under their own roof.
“He’s given us a run for our money,” Kelly said. “He’s a tough cookie.”
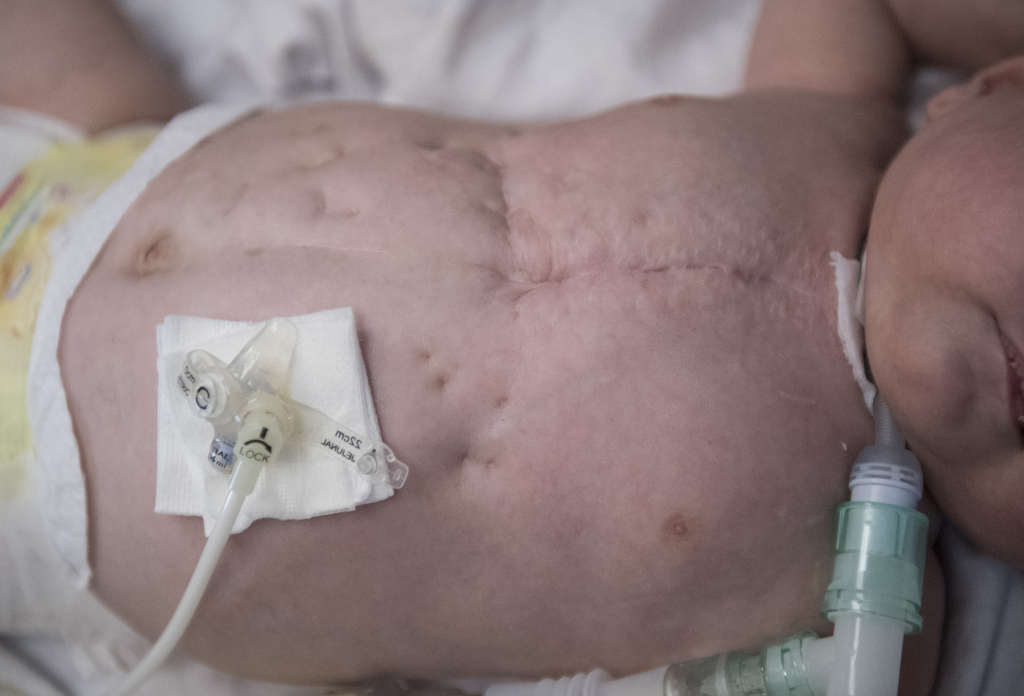
As she changed Elliot’s diaper, she pointed out the incision scar on his chest from his heart surgery. Smaller scars peppered his torso like tiny dimples—reminders of the many tubes and interventions he received.
One day, she will use those marks to tell Elliot about his first months of life.
“I have always thought scars are like tattoos but they tell better stories,” she said. “There’s a story behind every scar.”















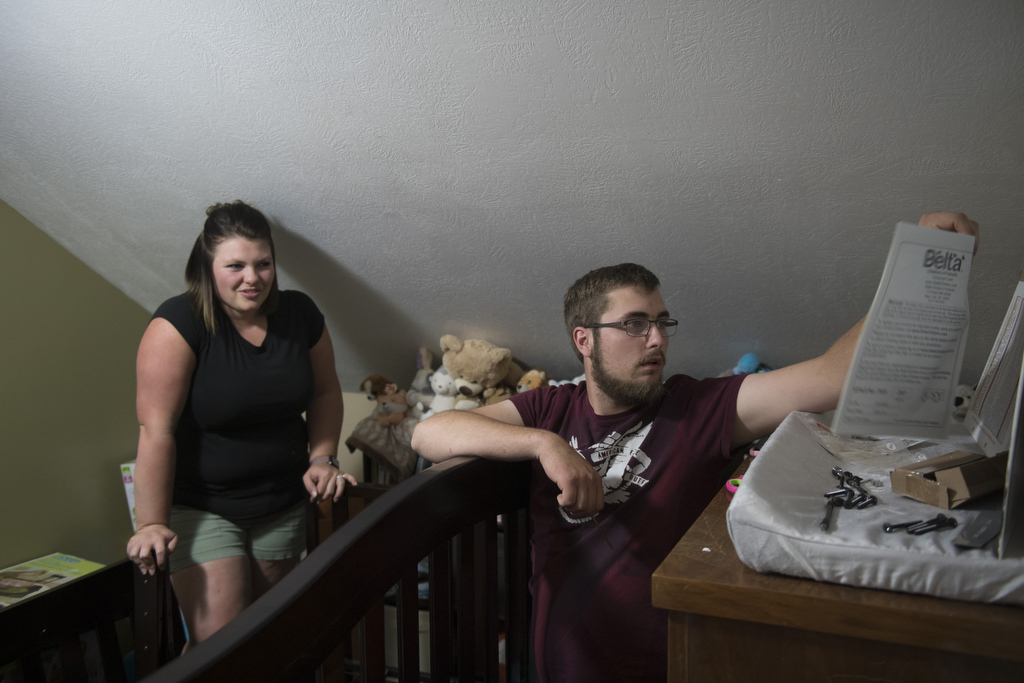












































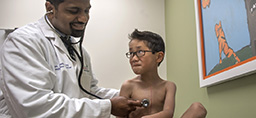 /a>
/a>
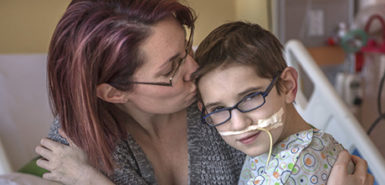 /a>
/a>
 /a>
/a>
And then there is the miracle of the detached-then-attached retina! That is a miracle only the LORD can do. God bless Elliot Dykstra.
The miracles of this little boy’s life are truly amazing.
Thanks for reading!
May God Bless your little boy. We had a son that was born with Transpostion also. He stayed in NICU 48 days . Came home and we had to bring him back 3 days later. He had all the same procedures your little guy did. Came home when he was 3 with a Trach and a feeding tube. He was born in March of 1986 and had open Heart in July 1986. I will pray for your family. From a heart Mom❤️
Thank you for sharing your story, Sheryl. I am sure Elliot’s family appreciates your prayers.
💗💙💚💛💜💟
Thank you for your beautiful story
Dr Vettukattil and the magic he does with those balloons of his!!! What a great bunch of doctors we are blessed with! Continues prayers for Elliot and his family! Great story Sue and wonderful pictures Taylor!
Thank you, Christine and Sherri. Elliot is a beautiful little boy. It’s an honor to share his story.
Thank you, Sherri!
Great story of how far medicine has come to save preemies! All of this care would not be available without millions of dollars from shared responsibility (insurance pools or government assistance), so when praising this “miracle”, please acknowledge the need for subsidized healthcare, whether you call it Obamacare, ACA, Medicaid, etc. Everyone deserves the same amount of subsidized healthcare that Elliot received!
Have a grandson born w/ almost the same issues. He was not a preemie, everything else was the same. Just so you kniw, Joe was 13 thus summer and is a very energetic and loving little boy. Thank God for doctors that care so much for these little guys.
How wonderful, Louise. Thank you for sharing! <3
Our first grandchild was born at 23 weeks. He was 11″ long and weighed all of 1 pound five ounces. It was found due to this little guys being conceived that our daughter had a rare kidney disease and would someday need a kidney transplant. She had it ten years ago, is doing well and even at her sickest before the transplant she never stopped caring for her little boy. This past June our grandson graduated from high school. He is a true miracle and the love of my life. He has been accepted to a local university in a special program for kids like him who were born with similar issues. He is healthy, intelligent, but socially a bit disconnected. His mother and father did an incredible job raising him. I want the parents of this beautiful lift,e baby to know that their little one may surprise them as he grows up. He may be just as intelligent, but in certain ways, than kids born normally. He will certainly be loved and cherished which is why our grandson turned out as well as he has. Our entire family had a hand in helping him from birth on.
My prayers are that this little guy do as well or better than our grandson. God Bless him.
Your story is incredibly touching. Thank you so much for sharing your family’s experience and for your kind words of encouragement!
Thinking of you guys! We love Elliott 🙂