When Susan Calkins travels in her fifth-wheel RV with her husband, Robert, she likes to move around, never staying in one place too long.
But when it comes to life, Calkins would like to stick around.
So far, a clinical trial is helping her do just that.
She has long since learned that life isn’t always so certain.
Doctors diagnosed her with stage 4 ovarian cancer in May 2010. No matter how much she fought, the cancer kept winning. Every time she thought she had pulled away, it set up camp in her body again.
It all began in 2010 with a lump. A simple, innocent-looking lump on the left side of her neck.
“I went to the doctor that week,” the Ionia, Michigan, resident said. “He probably suspected, because he sent me on to another doctor for a needle biopsy.”
The results weren’t what she wanted to hear.
Cancer.
And not just cancer in that particular lymph node. Something much worse.
“It was a secondary cancer they knew came from somewhere else,” said Calkins, 63. “I had a scan. It showed advanced stage 4 ovarian cancer.”
Blindsided
She doesn’t recall any symptoms, any fair warning. But looking back, she does remember feeling a little bloated. But that seemed to coincide with family dinners or the holidays.
“My family gets together for birthdays,” she said. “It seemed like at those big dinner times I wouldn’t feel so good. I attributed it to big meals, different foods and didn’t do anything about it. I just figured it was what I ate.”
The stage 4 cancer diagnosis left her with much more to digest.
“Like everyone, it hits you really hard,” Calkins said. “I felt like I should have been able to do something to prevent it.”
Even now she tears up as she speaks. The cancer threat is still fresh. Still real. Still mind-numbing.
Her doctor referred her to Charles Harrison, MD, a Spectrum Health Medical Group gynecologic oncologist.
“I remember going to the doctor,” she said. “I thought maybe it was stage 2. He said, ‘Oh no, it’s advanced stage 4.’ I thought, ‘That’s like the highest of the scale.’ Like probably a lot of people when they hear that, I thought that was probably the end.”
Dr. Harrison started her on eight rounds of chemotherapy. Then came a complete hysterectomy in December.
Normally a last-minute shopper, Calkins finished all her Christmas shopping before surgery.
“You wonder if it’s your last Christmas,” she said.
After surgery? More chemo.
“I responded really well to chemo,” she said. “After that I showed no sign of the disease.”
She felt incredibly fortunate. Blessed.
But two years later, the cancer returned.
More chemotherapy beat the cancer into submission again.
But not for long. Six months later, it resurfaced.
“I had a scan and sure enough , it was back in the lymph nodes,” Calkins said. “I went back for more treatment. I get six months out of treatments, then it comes back. It came back four times.”
The cancer kept morphing and changing, striving not to die, the same as Calkins.
But the cancer seemed to be winning.
After an RV trip down south in winter 2015, Calkins came back in January 2016 for more chemotherapy.
She grew allergic to one of the effective cancer-fighting drugs. An alternative chemotherapy drug started affecting her heart. So much so that she had to stop taking it.
“My options are starting to get narrower,” Calkins said. “After the fourth time cancer came back, the doctor tried a daily oral chemo pill. I did that for four months but it didn’t help at all. The cancer continued to get worse.”
Ongoing treatment
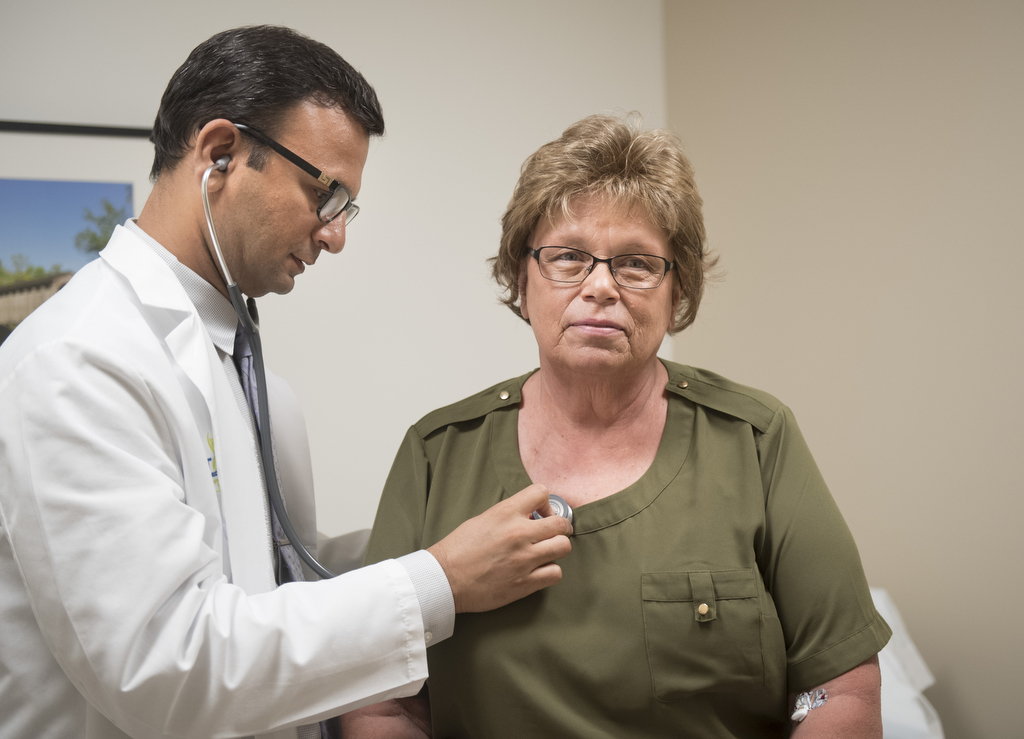
With few options left, Dr. Harrison suggested she take part in a clinical trial monitored by Nehal Lakhani, MD, PhD, director of clinical research at START-Midwest, located in Spectrum Health Cancer Center at Lemmen-Holton Cancer Pavilion.
The first trial was an immunotherapy drug, Calkins said.
“That didn’t help my kind of cancer,” she said. “There was another trial he said I could qualify for—it’s a targeted chemotherapy. I started on that (last December) and I have done wonderful.”
She receives four hours of treatment every three weeks.
Dr. Lakhani told Calkins he would like to treat her cancer as a chronic disease and continue treatment indefinitely.
“It’s a relief, a very big relief,” she said. “As of right this moment, I have no sign of the disease. How long this will last, you don’t know. It’s a new drug. But hey, as of right now, I’ve done well. I don’t get sick and there’s no nausea after the drug. I don’t feel a whole lot different after treatment than I do every other day.”
Dr. Lakhani said the clinical trial explores the effectiveness of an antibody drug conjugate, which seeks out and attaches to a protein expressed specifically on ovarian cancer cells.
“This antibody has chemotherapy molecules tagged onto it, allowing for very specific delivery of chemotherapy to the target site—sort of like a smart bomb,” Dr. Lakhani said.
Calkins will continue in the trial as long as her cancer is under control and she is tolerating the treatment well, the doctor said.
“Susan is doing very well and continues on treatment without any signs of cancer, physically or on CT scans,” Dr. Lakhani said.










 /a>
/a>
 /a>
/a>
 /a>
/a>
Sue, I had no idea. God be with you.
Praise the Lord for Susan !!! She is a fighter!!! I went to school with her. Also we met at a local pool where she worked. I am so happy this is working!!!!
Sue, so happy you’re responding well to this treatment. Praying for you everyday! 🙏 If there’s ever anything I can do for you I’d be more then happy to help. See you again at breakfast soon.
Sue, I am so happy you are doing great! Time to enjoy life, and laugh!! 🤗
That is my Suzy Q!! She is a fighter and one amazing good friend!! Love you to pieces!
Prayers and praise. Wishing you continue health and many years of happiness
Sue, Ernie and I were so glad to see you last week. You look great. Prayers that this new treatment will be the answer for you. I will keep you in my prayers.
Ernie and Marcia Ross