Rick Freehafer sat wide awake inside the operating room, two Spectrum Health surgeons feeding a series of thin wires into his brain.
The date: Aug. 9, 2019.
The place: Spectrum Health Butterworth Hospital.
Freehafer, 58, of Jenison, Michigan, would remember those moments forever.
R. Ross Coleman, MD, a movement disorder neurologist, and Hayden Boyce, MD, a neurosurgeon, hovered over him with utmost care, guiding the wires that sent electric impulses into his brain.
It’s the day his life finally changed.
‘I just lived with it’
Freehafer first noticed the shaking in high school.
His hands would tremble a bit, especially when he felt anxious or stressed. The involuntary tremors would sometimes travel to his head and neck, affecting his facial muscles and his speech.
“I didn’t pay too much attention to it because my dad had it and so did my sister,” Freehafer said.
Later, two of his three daughters would develop the condition.
When Freehafer’s father underwent testing for Parkinson’s disease, the test results came back negative. Doctors attributed the shaking to essential tremor, a slowly progressing movement disorder that usually affects people age 65 and older.
Freehafer, however, developed the condition at an incredibly young age.
He took medications for high blood pressure during his high school years to help the tremors, but the medications only aggravated his asthma.
“Since high school until this last year, I didn’t take anything for it,” Freehafer said. “I just lived with the tremors.”
As an adult, he’d sometimes down a shot of bourbon to help the shaking.
“But, you know, there are too many people who become alcoholics that way—by self-medicating,” he said.
Over the years, he simply learned to take things in stride.
If he experienced tremors in his hands or facial muscles during a dinner—his tongue and jaw would tremble—he’d joke it off to make things seem less awkward for companions.
His wife of 37 years, Beth, also took her husband’s tremors in stride.
The two became high school sweethearts at age 17.
“Rick’s tremors weren’t that noticeable in high school,” Beth said. “And I was kind of used to that. My grandpa and brother had tremors, too. It was no big deal then, but it got bad so fast.”
The search for solutions
Not long ago, Freehafer learned about a procedure called deep brain stimulation. He heard about it at Grand Valley State University, where he works in the IT department.
“A professor told me about it,” he said.
He then asked his doctor about it, which got him a referral to Dr. Boyce, who in turn connected with Dr. Coleman.
“They built a whole team around me: a neurosurgeon, a neurologist, physical and occupational and speech therapists—even a neuropsychologist to make sure I was a good candidate for the surgery,” Freehafer said. “They were a gift from God.”
After two days of examinations and consultations with the team, doctors deemed Freehafer a good candidate for deep brain stimulation.
He began to absorb knowledge on the procedure, learning how it’s used to treat tremors when medicine isn’t enough.
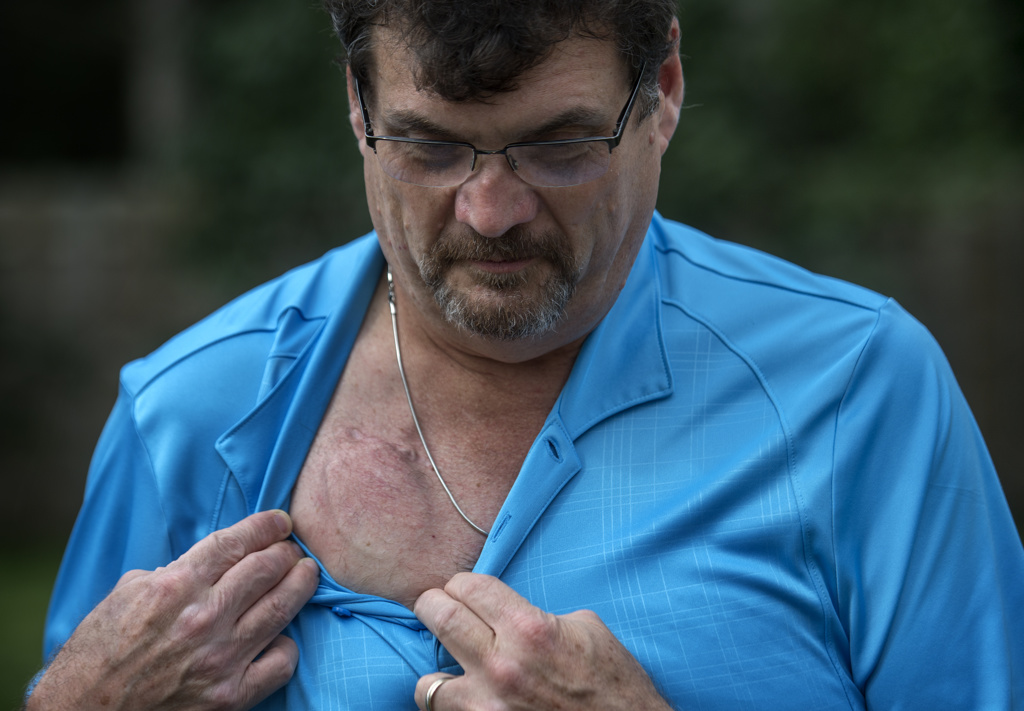
Doctors implant a pacemaker-like device into the patient’s chest, then connect the device to tiny wires they feed to tremor-causing areas in the brain.
The device emits electrical impulses that interfere with the abnormal brain signals that had caused the tremors, Dr. Coleman explained.
“The wires are about the size of spaghetti noodles,” he said. “We insert them through a hole about the size of a nickel in the patient’s skull, then wake the patient up so that he can help guide us to precisely the right spot in the brain.”
As the doctors work, they listen to the sound of the electrical impulses to guide their work.
“It sounds like rain on a tin roof,” Dr. Coleman said. “We listen to the rhythm and, when we hear the right rhythm, we put in the (deep brain stimulation) lead.”
During the procedure, the doctors will ask the patient to answer a few questions, or perhaps even perform a task or two to see how the leads are affecting the brain.
In Freehafer’s case, they had him write his name, draw some spirals and pretend to eat and drink out of a cup.
“He also brought a board and screwdriver into the operating room so that we could test that he can perform the same kinds of tasks he does at work,” Dr. Coleman said.
“The surgery takes about four hours for both sides of the brain,” Dr. Boyce said. “And Rick was awake once we started testing—about an hour on each side.”
Laundry duty
And then, it happened.
“I’ll never forget the moment they turned the electric impulses on,” Freehafer said. “The tremors instantly stopped. I must have started to cry, because I heard Dr. Boyce call out, ‘No crying in the operating room.’”
Dr. Boyce smiled.
“Yeah, that sounds like me,” he said. “We joke around in the operating room to alleviate fears.”
Doctors didn’t leave Freehafer’s pulse generator on immediately after surgery. They had to wait for the brain to heal, allowing the swelling to subside.
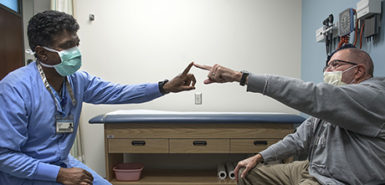
“Believe it or not, I went home the next day after surgery,” Freehafer said. “The pulse generator was turned on about a month later, on Sept. 4. Then I had to go in about once a month to have the doctors fine tune the impulses, until they get it just right.”
He can expect about 70% improvement in his tremors, Dr. Coleman said.
“Results vary depending on the kind of tremor a patient has, but it’s not a cure,” Dr. Coleman said. “Our goal is to improve quality of life and make everyday things easier.”
The deep brain stimulation wires are in Freehafer’s brain for life.
The pulse generator in his chest will need new batteries every three to five years. That requires a simple outpatient procedure.
“It will take six to nine months, I’m told, to get the frequencies to the electrodes set exactly right,” Freehafer said. “My right hand now is completely free of a tremor. I can only say I wish I had done this years ago.
“Now I just wonder who was first to figure out that putting electricity in the brain could do this—and who was the first to say, ‘Hey, do me,’” he laughed.
Beth sidled up next to her husband as he recounted the experience.
“The change has been amazing,” she said. “There are so many things Rick can do now that he couldn’t do before, like putting toothpaste on his toothbrush, or eating soup. And now I have a lot less laundry to do.”
As a token of his gratitude, Freehafer renewed a hobby: woodworking on a lathe.
Using olive wood for one and zebra wood for the other, he made pens for his two favorite doctors.
“I keep my pen in my office,” Dr. Coleman said. “It’s pretty special.”













 /a>
/a>
 /a>
/a>
 /a>
/a>
About 30 years ago my father-in-law was one of the first to try this (he had Parkinson’s). It was still experimental and it was done at the Mayo Clinic. It seemed to help at first, but unfortunately, while threading the wires up through the neck something happened to cause damage and it wasn’t very long after the surgery that he lost his ability to speak and swallow. He eventually required a feeding tube.
He always said he had no regrets, that even though it didn’t work for him at least he was part of working on a solution and providing good information towards perfecting it. Even after more than ten years on a feeding tube, he never once regretted taking the chance. He would be thrilled to know that procedure is working now.