Candus Jones looked at herself in the mirror, still shaking from a fall to the bathroom floor and the long struggle back to her feet.
“You’ve got to go to the hospital,” she told herself as tears rolled down her face. “You’re a strong woman, but you can’t push forward anymore.”
For six months, she had gradually lost control of her hands and feet. Mysterious, stabbing pain struck her arms and legs.
“It’s a horrible, horrible pain that I wouldn’t wish on my worst enemy if I had one,” she said.
She was 34 years old. For 15 years, she had worked as a home health aide. She loved caring for her clients and handled the physical demands of the job with ease. But lately, she had begun to feel shaky and weak. She fell repeatedly.
“I was walking like a 92-year-old woman,” she said. “I would fall in my clients’ yard before I’d get into the house. But I would pick myself up and go to work. I provided the best care possible, even being weebly-wobbly.”
On that day in July, when she fell in the bathroom and landed between the toilet and bathtub, she realized the fall could have knocked her out. Maybe killed her.
She knew she needed help. But she had no idea of the rocky road that lay before her—the moments of utter helplessness she would endure. Or the sweet moment of victory a single step would bring.
“I am a walking, living, breathing miracle in the flesh,” she said, her eyes wide and a smile on her face, as she sat in her hospital room. “It’s been an amazing journey for me—totally mind-blowing.”
Losing ground
The first step of that journey was a trip to Spectrum Health Butterworth Hospital emergency room. After an MRI, a spinal tap and an electromyography test, the doctors came back with a diagnosis: a rare neurological disorder called chronic inflammatory demyelinating polyneuropathy.
“It sounds such a tremendous word,” Jones said. “It’s kind of intimidating. It means my body is attacking the nerves in my spine as if they are a foreign body.”
The autoimmune disorder involves damage to the insulation on the fibers of the peripheral nerves, said Paul Twydell, DO, a Spectrum Health Medical Group neurologist. It causes progressive weakness and impaired sensory function in the arms and legs.
I’m from a long line of cast-iron skillet women. I refuse to let life knock me down.
Jones received intravenous steroids and immunoglobulin, the standard treatment for the disorder. And she transferred to the Inpatient Rehabilitation Center at Spectrum Health Blodgett Hospital to improve her muscle strength.
At first, Jones made progress in rehab. But then she began to lose ground. No matter how hard she worked, she grew weaker. She received plasmapheresis, another treatment used for the disorder.
“Usually, these cases respond to plasmapheresis or IV (immunoglobulin) treatment,” said Patrick Mullan, DO, a rehabilitation medicine specialist at the Inpatient Rehabilitation Center.
But Jones continued to decline. She lost so much feeling and function in her hands that she couldn’t hold her phone or pick up a straw. She could not stand or walk by herself. It took two therapists to help her to her feet.
“(The disease) messes with every body function you have,” she said. “Your nerves control everything. That’s your super highway in your body. Just imagine your body attacking your super highway.”
One day in August, working with a physical therapist at the Inpatient Rehabilitation Center, she realized she had become partially paralyzed.
“I cried for two days,” she said. “I didn’t want to face it. Not walking meant I couldn’t take care of myself.”
Jones had just moved to Grand Rapids, Michigan, a year earlier. She loved her new home but wasn’t sure she could manage to live independently. All of her family members lived in West Tennessee. They urged her to come back home, so she could have family support.
In either case, Jones worried she would have to live in a nursing home if she continued to decline.
And then a new option opened. Her occupational therapist, Megan O’Mara, recalled a former patient who had a similar experience with the same condition. When standard treatments failed, he benefited from a course of IV steroids.
Dr. Mullan consulted Dr. Twydell. After follow-up tests to confirm Jones indeed had the chronic condition—and not another disease that mimicked it, Dr. Twydell agreed that Jones should try IV steroids. He believed she had a rare form of the already rare disease.
“There is a small subset of people with (the disorder) who don’t respond to IVIG or plasma exchange,” he said.
Jones received the intravenous steroids every day for five days. Then she received a dose once a week.
Jones quickly dubbed it “my super juice.”
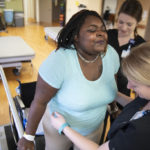
After a few days on the new medication, four therapists helped Jones rise and connect to a Rifton transport and mobility device. The gait system includes a harness, which eliminates the fear of falling for patients as they walk.
Jones struggled to move one leg forward. She took a step. Then another. Five steps in total. A short walk, but a huge milestone for her.
Her progress moved swiftly after that. After a week of therapy using the Rifton, she graduated to an ordinary walker, holding up her own weight as she walked across the therapy gym and down the hall.
‘I made it’
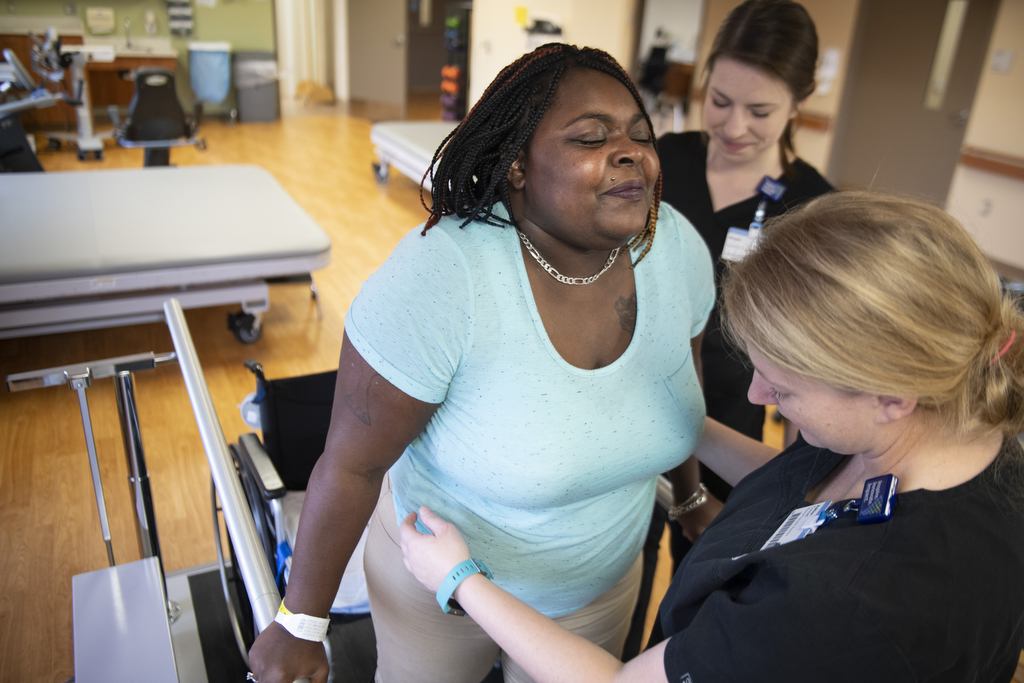
On a September morning, Jones took a step up—literally—in the therapy gym. She held onto the parallel bars and practiced stepping up and down from a 4-inch box, as preparation for climbing stairs.
On the way back to her room, she decided to challenge herself to walk the length of the hall without stopping to sit down. It was more than twice the distance she had walked in the past 2 1/2 weeks. It took a toll.
She moved the walker ahead of her and walked, one painstaking step at a time, followed closely by physical therapy assistant Ashlee Connell and Morgan Hungerford, a rehab technician.
As the double doors loomed closer, tears rolled down her cheeks. Perspiration beaded on her forehead. At Connell’s encouragement, Jones paused to catch her breath. But she remained standing.
“Let’s go,” she said, resuming her push forward. “I’m so excited. I’m going to make it to that door.”
She crossed the doorway and sat back in the wheelchair.
“You just went 200 feet,” Connell announced. “I am so proud of you.”
Jones sobbed and laughed and spoke in a breathless rush.
“I made it. I made it,” she said. “I’m amazed. I’m ecstatic. Two and a half weeks ago, I couldn’t do a thing. And now I’m walking 200 feet without stopping to sit down.”
She attained an even sweeter victory that afternoon. In an occupational therapy session, she whipped up a cheesecake.
She stood at the kitchen counter and measured and poured milk. She stirred the batter and pressed the graham cracker crust into the pan. Her hands and fingers could not have managed those tasks just a few weeks earlier. Jones delighted over her improved fine-motor skills.
“Every little milestone is mind-blowing,” she said.
Jones gave credit to her doctors and the therapists who became like family during her two-month stay at the Inpatient Rehabilitation Center.
“They never gave up on me. They saved my life,” she said. “I believe God absolutely brought me here for this reason and this reason alone. He knew I was sick in my body and I would get the right help at the right time.”
She also drew support from her close-knit family in Tennessee, who kept in contact through regular phone calls.
But still, facing a rare disease can feel a bit lonely. Talking with recreational therapist Shanon Haskins, Jones decided to share her journey through videos posted on her Facebook page.
Support poured in from family, friends and strangers: Her first video received nearly 12,000 views. She connected with others around the world experiencing similar symptoms or the same diagnosis and shared tips and encouragement.
Jones’s inner strength and resourcefulness impressed her medical team.
“All of the therapists who worked with her were so inspired by Candus’ sense of humor, positive attitude and willingness to persevere in the face of pain, uncertainty and loss of independence,” said physical therapist Linda Rusiecki. “The fact that she could still laugh, joke, and be a light and a blessing to those around her, despite going through this terrifying experience, was really uplifting.”
Bouncing back
By mid-September, Jones made enough progress to move to the Inpatient Subacute Rehabilitation program at the Spectrum Health Rehab and Nursing Center on Kalamazoo Avenue SE.
Sitting in a chair in her room, her feet propped up on the bed, she said she was growing stronger. She could walk farther, her balance had improved and she was relearning basic self-care tasks, such as getting dressed.
Two months had passed since she arrived at the emergency room. She looked forward to her graduation date in two weeks.
Jones will continue to receive medical care for her chronic condition. In some cases, the disease goes into remission.
“Most of the time, people with (the disorder), once treated, can go back to living pretty normal lives,” Dr. Twydell said.
Jones beamed as she talked about the future. She no longer thought about choosing a nursing home. Instead, she and her sister talked about opening a hair salon.
“I’ll deal with this the rest of my life, but I’m not afraid,” she said. “I’m from a long line of cast-iron skillet women. I refuse to let life knock me down.”

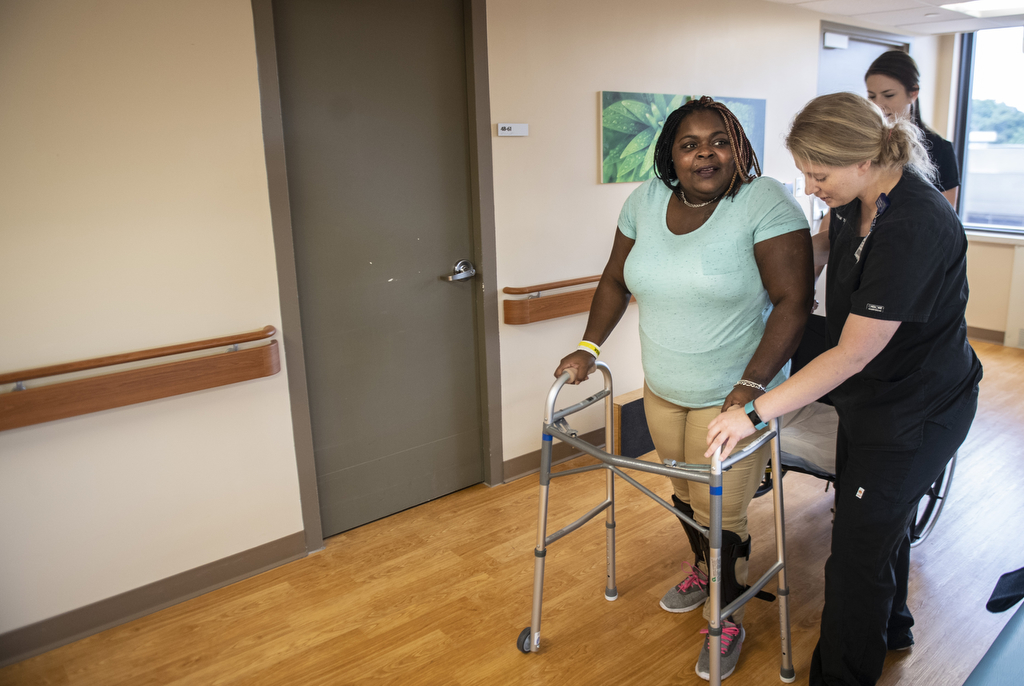






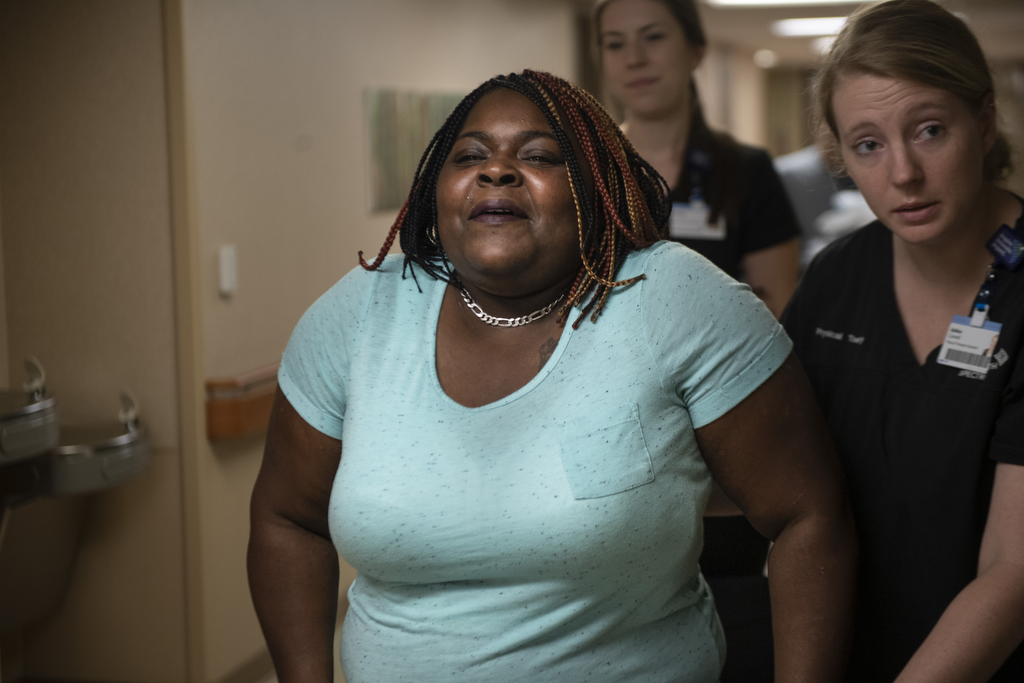






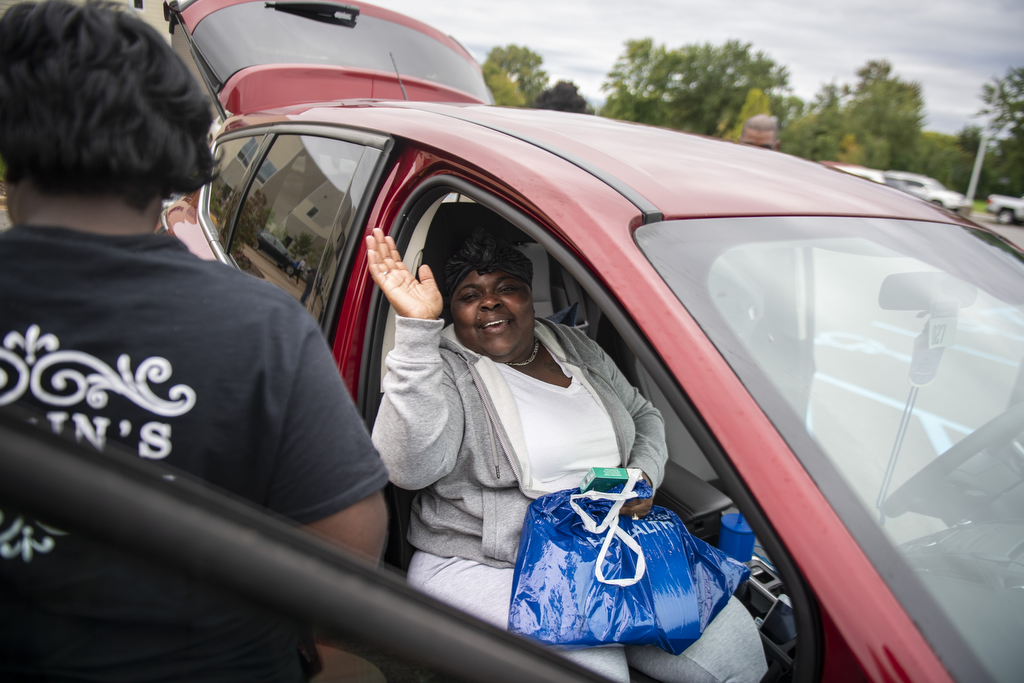



















 /a>
/a>
 /a>
/a>
 /a>
/a>
Very, VERY…Inspiring!!! Candace, you are one tough cookie! I admire your strength and to God Be the glory!! Prayers for you continuously, my friend!!
Am so proud of my niece.She has been threw alot.My name is chanelle harris and am her dads sister.Hang in there candace cause god got you.Love you and hope to see you whenever i can keep up with were you be but we love you and thanks to your doctor and staff.
God is Good! Keep up the fight Candus!
Pooh I LOVE YOU soooooooo much and I’m so proud of you I knew you could do it and I never once gave up on you .through the conversations ,video calls, text messages and all the tears we shared I knew you wasn’t giving up on God and he wasn’t giving up on you.Not one time we made contact and you didn’t mention God and that case iron skillet of women so to her family I LOVE YOU AS WELL EVEN THOUGH MOMMA YOU HAVE TO SHARE YOUR SPOT I THE SECOND MOM LOL
As the tears roll down my face, I can’t help but praise God for His blessings. Your story is amazing and can help so many around the world. A true testiment to the power of Jesus. Love you Candus 💕 and thank you for allowing me to share your journey.
What a lovely comment, Judy! We’re so happy to have you as a Health Beat reader. Thank you for sharing your thoughts and warm wishes. Cheers, Cheryl
Many blessings to come
Always loved a cast iron skillet … God bless you Candus 🙏
Thank you for posting, so inspiring.