It’s easy to picture Dave King at work as a barber, his profession for years in both Ohio and Michigan.
Dave, 69, is a warm, congenial man who enjoys making conversation. He would gladly pass the time of day with anyone who came looking for a cut or a trim.
He always gave a good haircut, even when his hands began to tremor. The shaking wasn’t a big deal. He could manage.
And he did get by—for decades—until about seven years ago, when the tremoring in both hands became more pronounced.
First he gave up cutting with scissors, shifting to the clipper-over-comb method. Then, in 2013, he retired from barbering altogether.
“I’m a barber and I couldn’t hardly cut hair,” he said.
A Vietnam veteran, he had already sought help for his symptoms at a Veterans Affairs medical center. Doctors there diagnosed him with essential tremor, a movement disorder characterized by involuntary shaking.
They prescribed medications to control his tremors, which now affected his head as well as his hands. When the medications failed to help and the shaking worsened, he knew he had to try something else.
“It was getting worse quickly,” Sue King, Dave’s wife, said.
It reached the point where he couldn’t use a screwdriver, cut a steak or pour a cup of coffee without spilling.
And Sue could no longer read her husband’s handwriting.
“The last two years, it just—no. It was very, very difficult,” she said. “He’d write (something) on the calendar or wherever and I wasn’t sure what it said.”
Dave first talked with his VA doctors and then asked his family doctor in Hastings, Michigan, for advice.
She referred him to the movement disorders program at Spectrum Health.
Patient friendly
Thus began Dave’s journey with a treatment called deep brain stimulation.
Deep brain stimulation uses thin wires called leads, implanted deep in the brain, to send an electrical current to a targeted cluster of brain cells controlling tremors. The stimulation can ease the debilitating symptoms of essential tremor, as well as of Parkinson’s disease and, in some cases, obsessive compulsive disorder.
Deep brain stimulation isn’t a new procedure.
The FDA approved it for the treatment of essential tremor in the 1990s, according to Rushna Ali, MD, Dave’s neurosurgeon and a member of Spectrum Health Medical Group.
What’s new about Dave’s procedure is the type of head-frame system she used to perform the surgery.
Dave was the first patient in Michigan to undergo deep brain stimulation using a lightweight 3D printed frame called the WayPoint Stereotactic System. Spectrum Health is the state’s first health care provider to offer this technology, Dr. Ali said.
The slim plastic frame, which sits atop the patient’s head like a crown, is customized to each patient—“tailored specifically for their brains,” she said.
Compared with the more elaborate traditional frames, this crown-style frame is smaller, simpler and exponentially more comfortable for patients, Dr. Ali said.
“You can sit up, you can turn side to side, you can adjust your position. I’ve even given patients shoulder and back massages during surgery if they’re getting sore,” she said.
That’s because a patient’s motion doesn’t interfere with the procedure’s success.
The same isn’t true with a traditional halo-style frame system, which bolts to the patient’s skull, wraps around the head and attaches to the bed, keeping the patient stock-still.
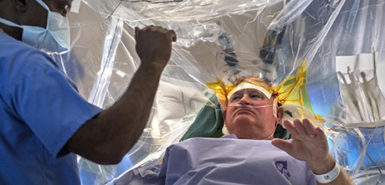
“Imagine your head being restrained in this fashion, stuck to the bed—anxious, nervous and shaking, but you can’t go anywhere,” Dr. Ali said.
“If you’re claustrophobic, you’re done, you’re hosed,” she said, because for this type of surgery patients have to be awake and involved.
“We can record physiological activity from individual brain cells as we’re going from the surface of the brain down to the specific area of the brain that we’re targeting,” she explained. “If the patient’s awake, we can test this. He’ll have a tremor and then, when we turn the current up, the tremor will stop.”
Dave’s deep brain stimulation surgery took place in November 2018, just weeks after his first consultation with Spectrum Health Medical Group Neurosciences.
Because Dave appeared to be a good candidate for deep brain stimulation, he got started right away on the screenings he’d need to pass before the team could greenlight the surgery—appointments with a physical therapist, a speech therapist and a psychologist.
With each evaluation, Dave and Sue became more comfortable with the idea of an invasive brain procedure.
“Each test that he had to have done, we both felt more assured. It was amazing, because they took such care in seeing what his parameters were for walking, for speaking, for his cognitive ability,” Sue said.
“And Dr. Ali said he passed with flying colors.”
Three-stage process
The WayPoint deep brain stimulation process involves three separate surgeries, typically scheduled in consecutive weeks:
- A preliminary surgery, under anesthesia, to embed in the patient’s skull four small screws that the frame would attach to. The patient also has a CT scan and an MRI, providing images to help the doctors map where to implant the leads and how to design the custom frame.
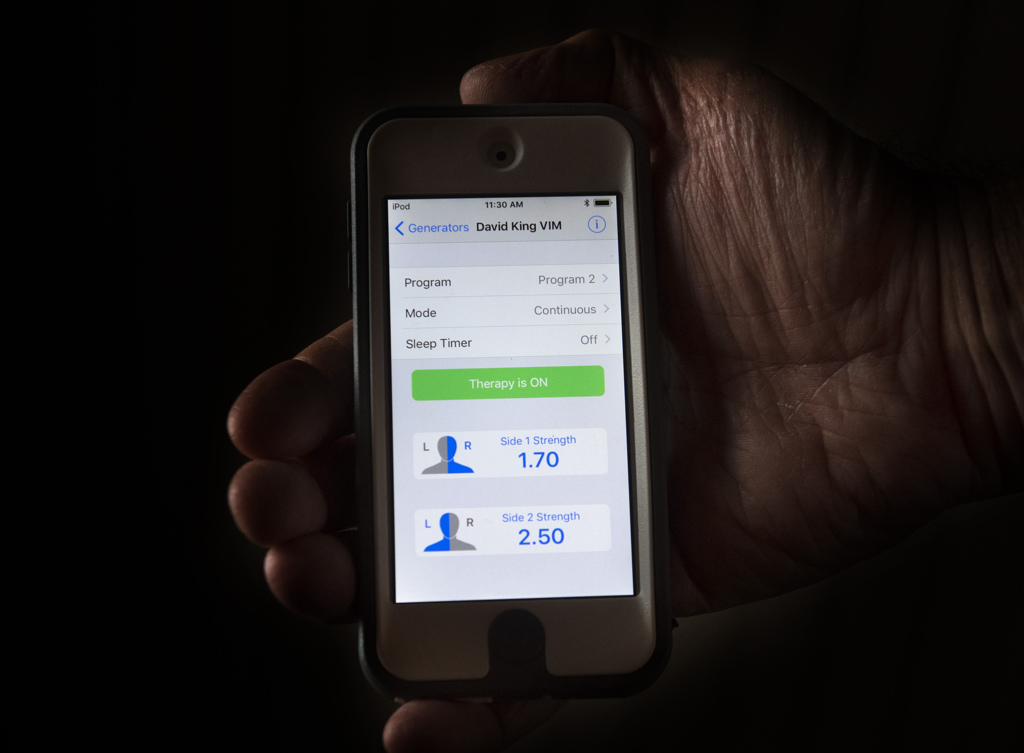
- The main surgery, under conscious sedation, to attach the frame to the screws and then drive through the skull to insert the leads that stimulate the tremor-control nucleus. During this lengthy procedure the patient participates by answering questions and responding to instructions so the doctors can check whether they’ve positioned the leads correctly. In Dave’s case, leads were implanted on both the left and right sides of his brain to control the tremors in both hands.
- A follow-up surgery, also under anesthesia, to implant a small generator under the skin near the patient’s collarbone and connect the implanted leads to the generator.
A week after this three-stage process is complete, the patient returns so the neurology team can turn on the generator and program the software that controls the leads.
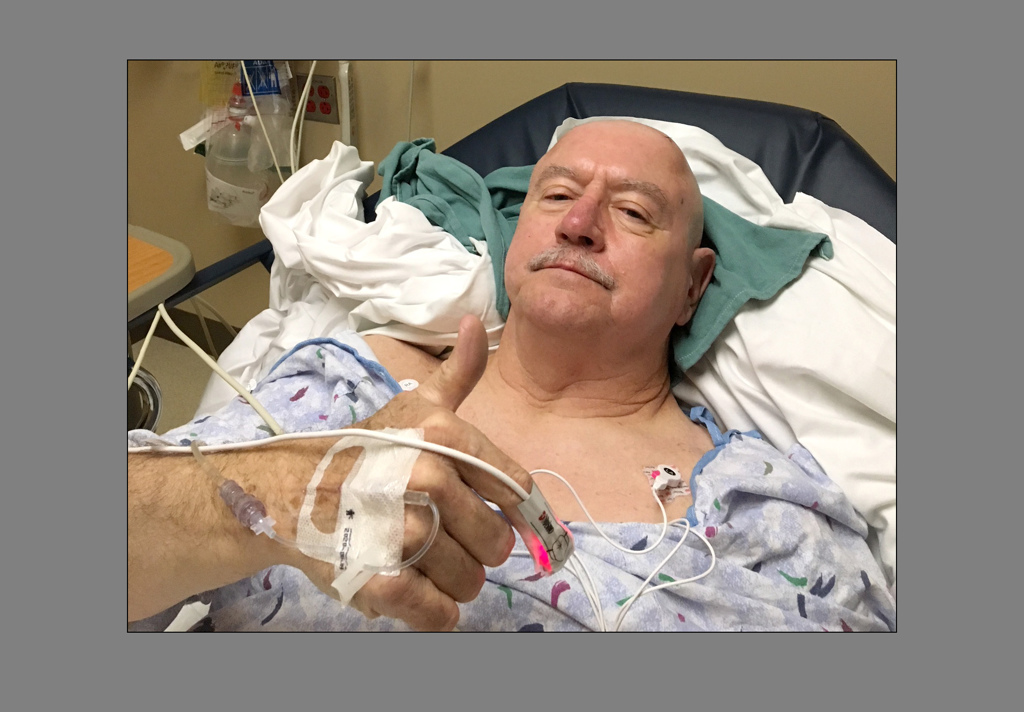
Dave’s surgeries went off without a hitch. Yet, though the surgical team kept him comfortable throughout, he won’t say the procedures were easy—especially the five-hour lead implantation.
“I was praying constantly while I was in there. I was praying for their hands and for wisdom for them to know what they’re doing,” he said. “When I came out, I was nothing but tears because I was so glad it was all over.”
Despite the stress of the surgical process, Dave loves the results he’s seen so far and the promise of continued improvement.
By his own estimation, deep brain stimulation has already resolved 80 to 90 percent of his tremor troubles.
“It’s amazing what I can do and what I couldn’t do (before),” Dave said.
“I used to have trouble cutting my food and using my utensils, but now I don’t really have trouble.”
‘We’ll keep tweaking’
These days, Dave is in what he calls the tune-up phase of deep brain stimulation programming.
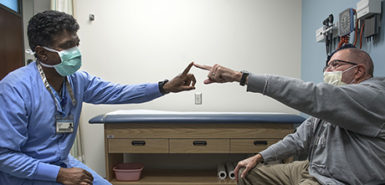
This means he visits the neurology clinic monthly to have the currents adjusted in response to his remaining symptoms.
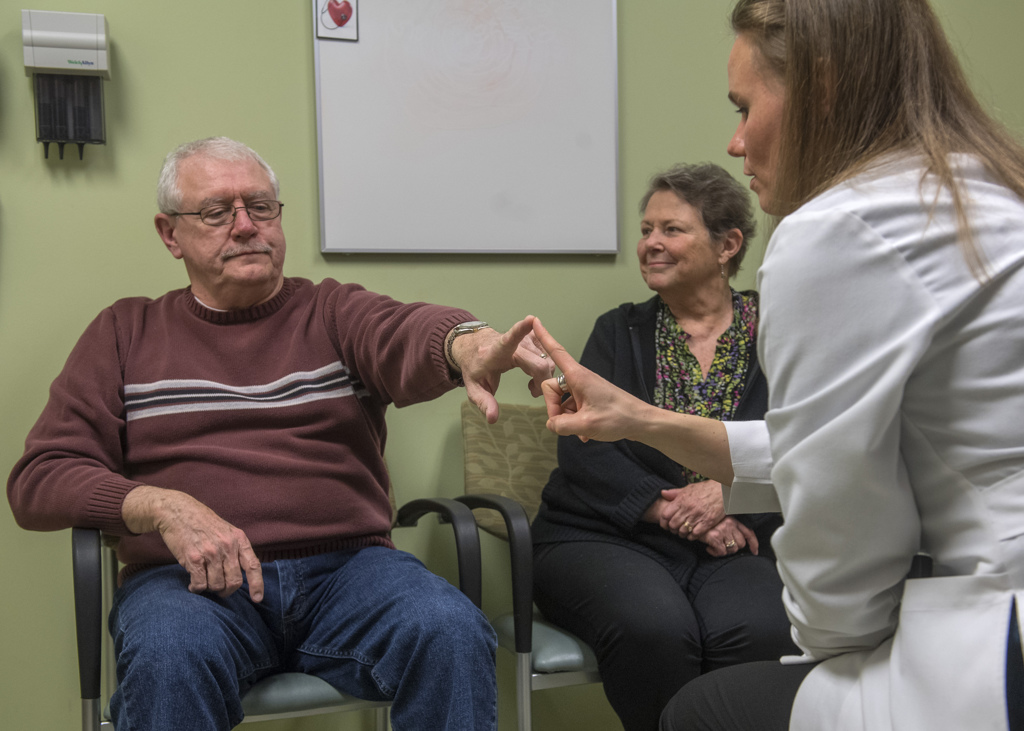
On a recent clinic visit, Angela West, PA-C, worked to correct a slight tremor in his left hand, the slurring that he sometimes notices in his speech and the slight head-bobbing that remains.
“We just have to figure out what stimulation patterns work best. … We’ll keep tweaking it until we get the settings right,” West said. “A year from now you’re gonna say, ‘Oh my gosh, I don’t even remember what my tremor was like.’ But this looks good. This is a good start.”
Sue has her own perspective on Dave’s experience. For her, the best part is that when his tremors disappeared, so did his aggravation at not being able to do simple things like flipping eggs and writing checks.
“I don’t see that frustration anymore,” she said. “All the things that he works with, he just does it now. It’s amazing. It’s a blessing.”
Dave is quickly adjusting to his new, steady normal.
He likes keeping busy, but he has no plans to return to barbering.
He loves his part-time job driving for Barry County Transit.
But Dave’s still a natural at cutting hair, so he’s started to pick up his scissors again, for old time’s sake. As a favor for friends. Because he can.
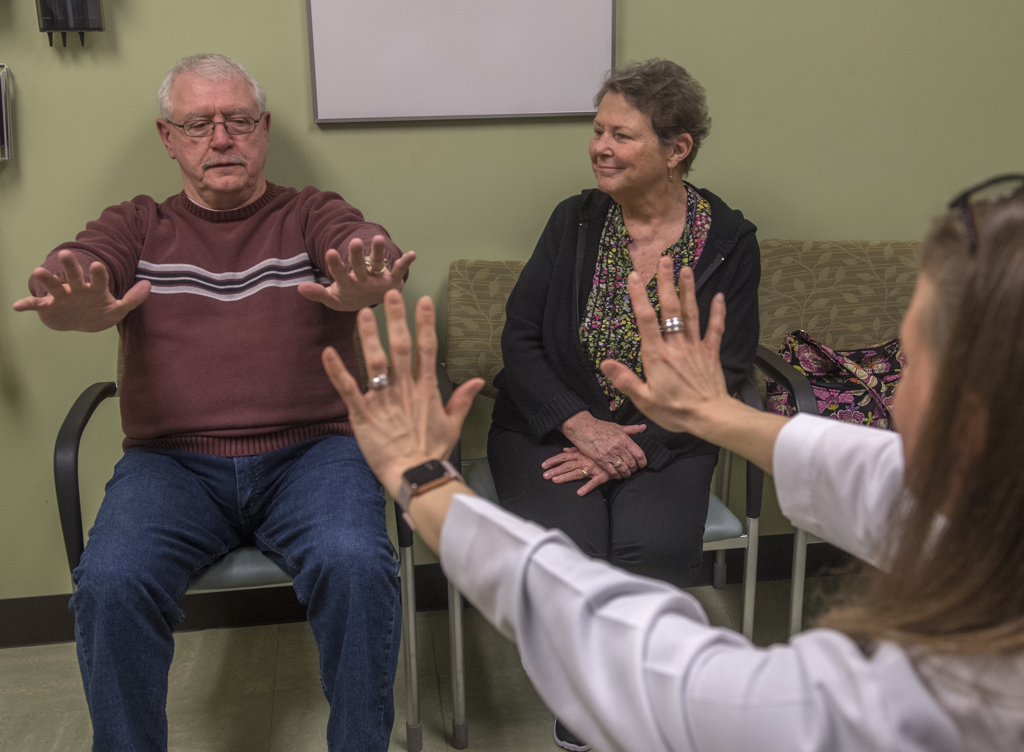






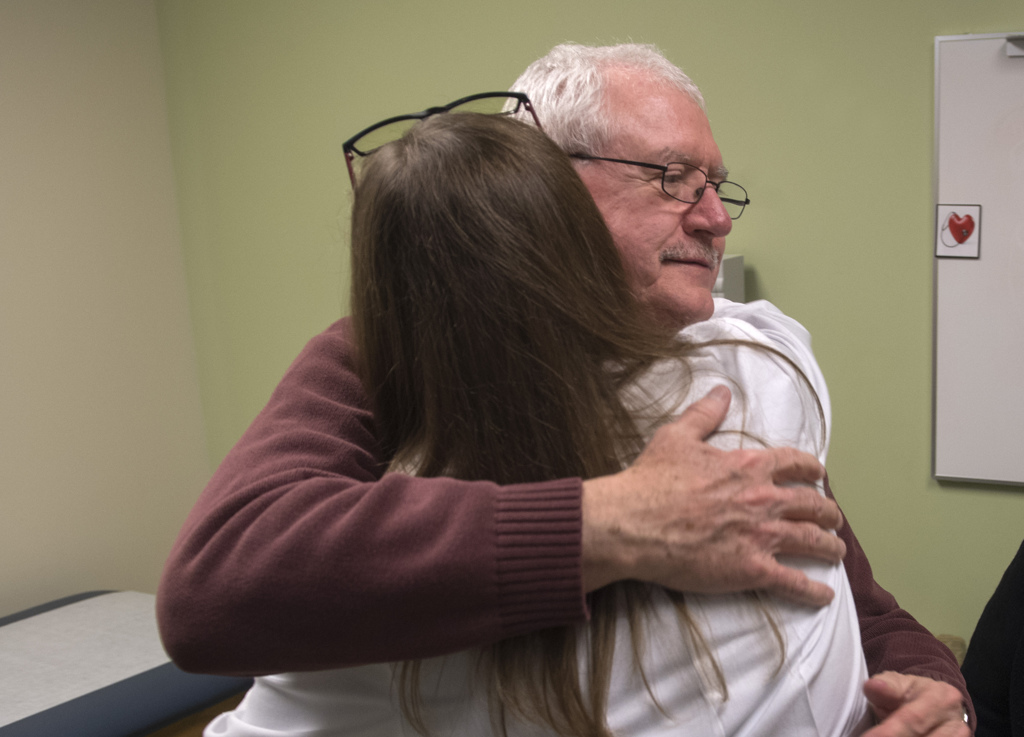












 /a>
/a>
 /a>
/a>
 /a>
/a>