In spring 2011, an expectant Melissa Case left her family home in the tiny Upper Peninsula town of Brimley, Michigan, and headed to a hospital in Petoskey.
“I was considered a high-risk pregnancy because of a pulmonary embolism I had had years ago, so I wanted to go to a larger hospital,” Melissa said. “The nearest hospital to Brimley is in Sault St. Marie. And that’s not large.”
The baby, which would be her first, had shown no signs of trouble during pregnancy.
And the delivery went well.
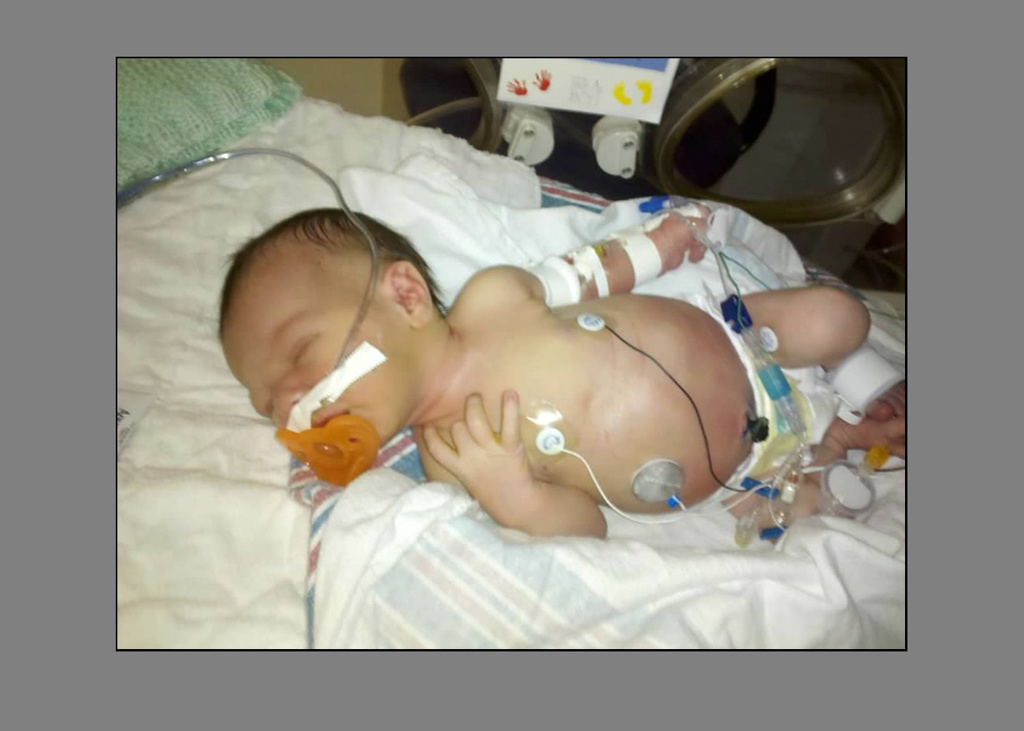
Wyatt Case entered the world on April 4, 2011, weighing a healthy 7 pounds, 9 ounces.
But Wyatt and his mother and father, Nate, wouldn’t stay at the Petoskey hospital for long.
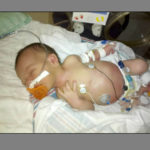
Within 24 hours of his birth, doctors noticed some troubling signs.
“He developed a fever and his bowel wasn’t working,” Melissa said. “He vomited green bile.
“They sent us immediately to Spectrum Health Helen DeVos Children’s Hospital in Grand Rapids,” she said. “The doctors did a biopsy and they were pretty sure Wyatt had Hirschsprung’s disease.”
At 6 days old, Wyatt underwent his first surgery.
Building routines
According to the National Institutes of Health, one in 5,000 newborns develop Hirschsprung’s disease.
It’s a congenital condition of the large intestine, or colon, caused by missing nerve cells that would normally help the muscle pass stool.
The first symptom doctors notice: a newborn fails to pass stool within 48 hours of birth. The baby may also vomit and become bloated from gas.
“This was all such a shock,” Melissa said. “The pregnancy had been entirely normal and we had no family history of such a disease.
“But here we were at the hospital for a seven-week stay. Nate traveled back and forth every few days to his work back in the UP, while I stayed at one of the hospitality houses for the hospital.”
In a six-hour surgery, doctors removed Wyatt’s colon and connected the small intestine to the rectum.
It took about two weeks before his intestine and bladder “woke up” and started working again.
“I had to pump milk to keep up with his nursing, but it was important to me that he have all the advantages of being breastfed,” Melissa said.
Over time, the Case family came to understand more about Hirschsprung’s disease.
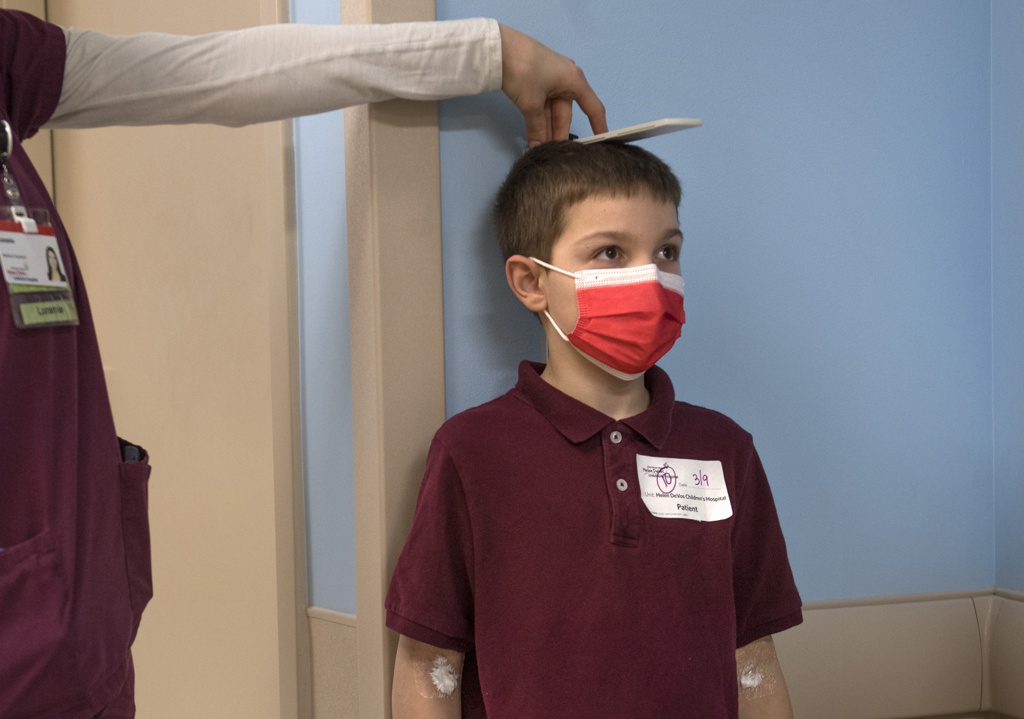
Wyatt grew slower than other children his age.
For a few years, life seemed to settle into a routine.
“He was chubby and healthy, if a little short on the growth scale,” Melissa said. “Our biggest battle was diaper rash.”
By age 3, new problems arose.
Wyatt, still unable to adequately express his needs, would cry out in pain.
“Wyatt’s belly got distended, bloated with gas,” Melissa said. “It gave his belly an alien appearance, with gas bubbles so big that you could see them move down through his abdomen. We tried antibiotics, probiotics, we tried everything, but nothing seemed to help.”
Another troubling development arose after they noticed what at first appeared to be a small pimple on Wyatt’s behind.
It soon turned into an abscess, then into a fistula—an abnormal connection, or opening, between two hollow organs. In this case, it was an opening to Wyatt’s intestine.
Digging deeper
By November 2014, Wyatt had become ill and in pain.
Following a visit to a doctor that month, a Spectrum Health Aero Med helicopter transported Wyatt from the north part of the state to Helen DeVos Children’s Hospital.
“By then, we had two more children—two daughters,” Melissa said. “Family in Brimley helped watch the girls while I drove to Grand Rapids and Nate flew in Aero Med with Wyatt.”
At the children’s hospital, doctors discovered Wyatt had developed two bowel perforations and scar tissue in his intestine, along with the fistula.
They removed the scar tissue and repaired his bowels.
“Wyatt had to have many more surgeries over those first years,” Melissa said. “He had seven surgeries on the fistula alone.”
As the years passed, Wyatt’s health issues seemed to pile up.
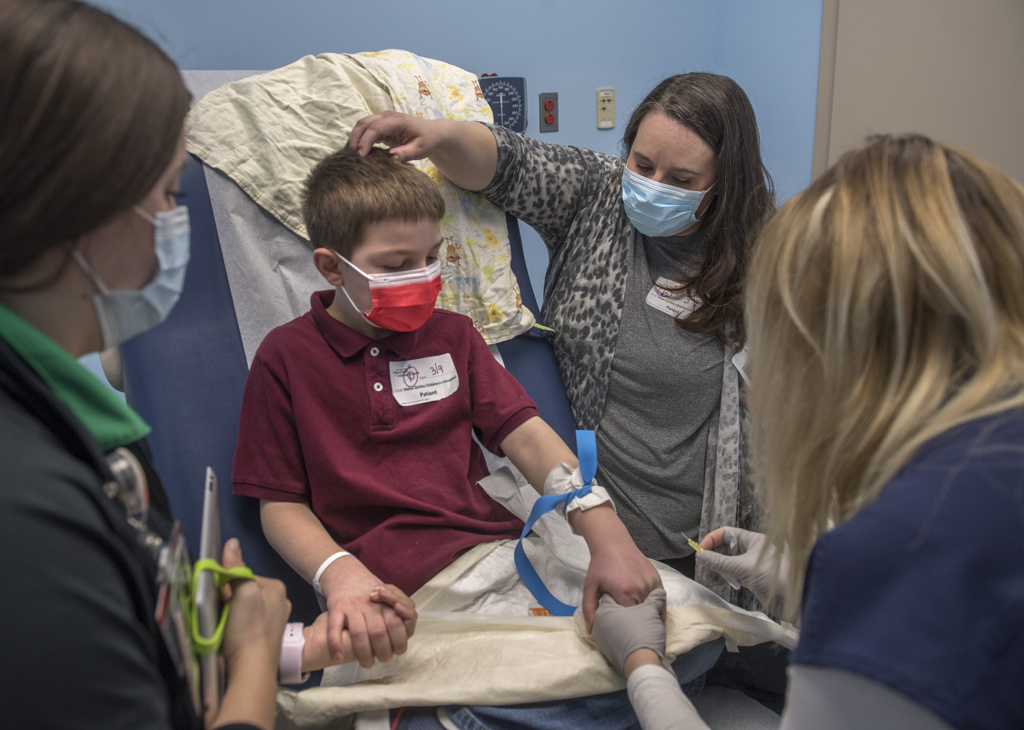
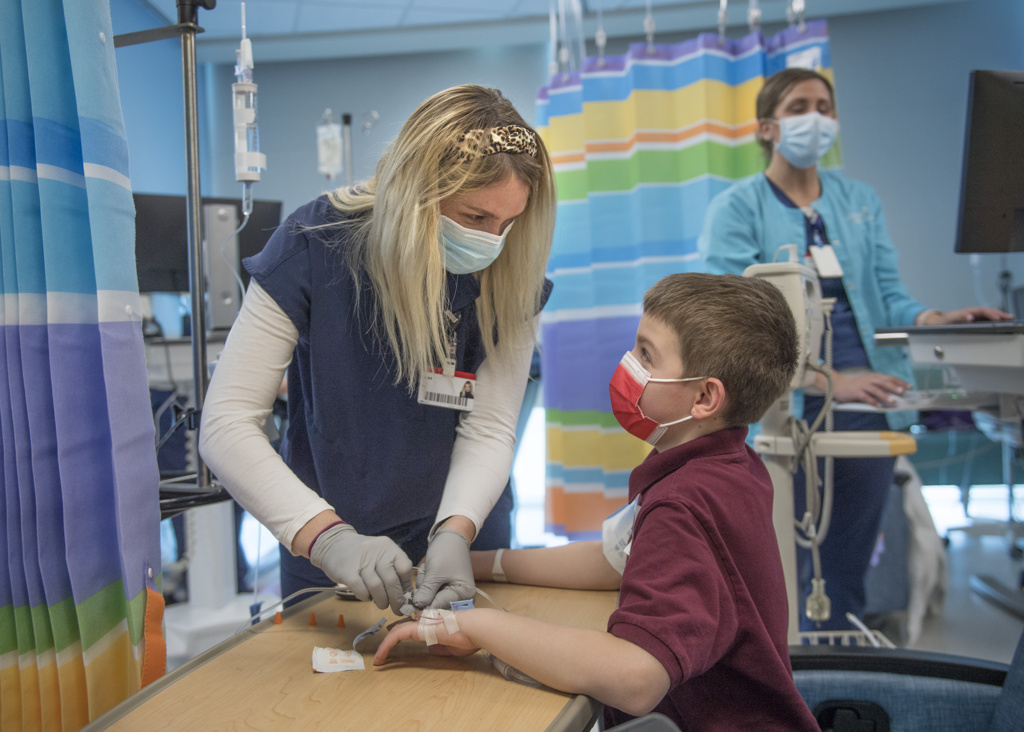
In 2018, at age 7, doctors diagnosed him with Crohn’s disease. It would require infusions, bringing the family back to Helen DeVos Children’s Hospital every eight weeks.
The Crohn’s disease also made Wyatt prone to urinary tract infections and kidney stones.
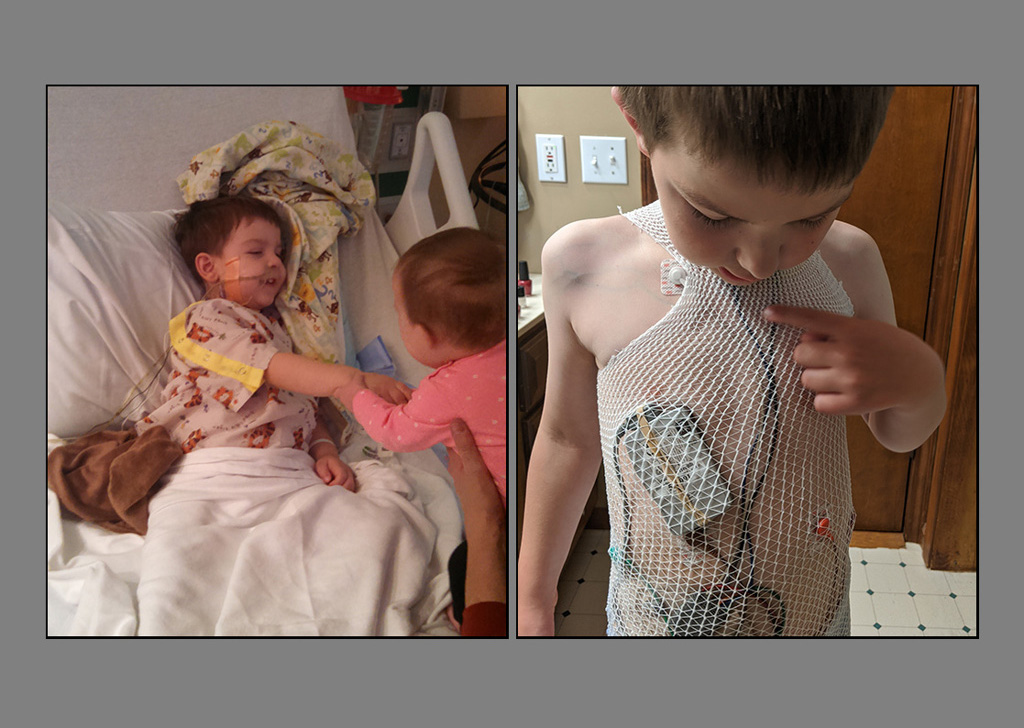
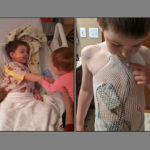
In October 2019, his fistula still hadn’t healed. Doctors surgically placed a pouch, an ostomy, on the outside of his body to allow for expulsion of waste product.
Wyatt’s parents decided the time had come for deeper questions.
In November 2019, they sought a referral for genetic testing.
“We needed to understand why Wyatt was having so many health problems,” Melissa said. “We wanted to know we were doing everything we could for him. We wanted to know what to expect in the future.”
Genetic clues
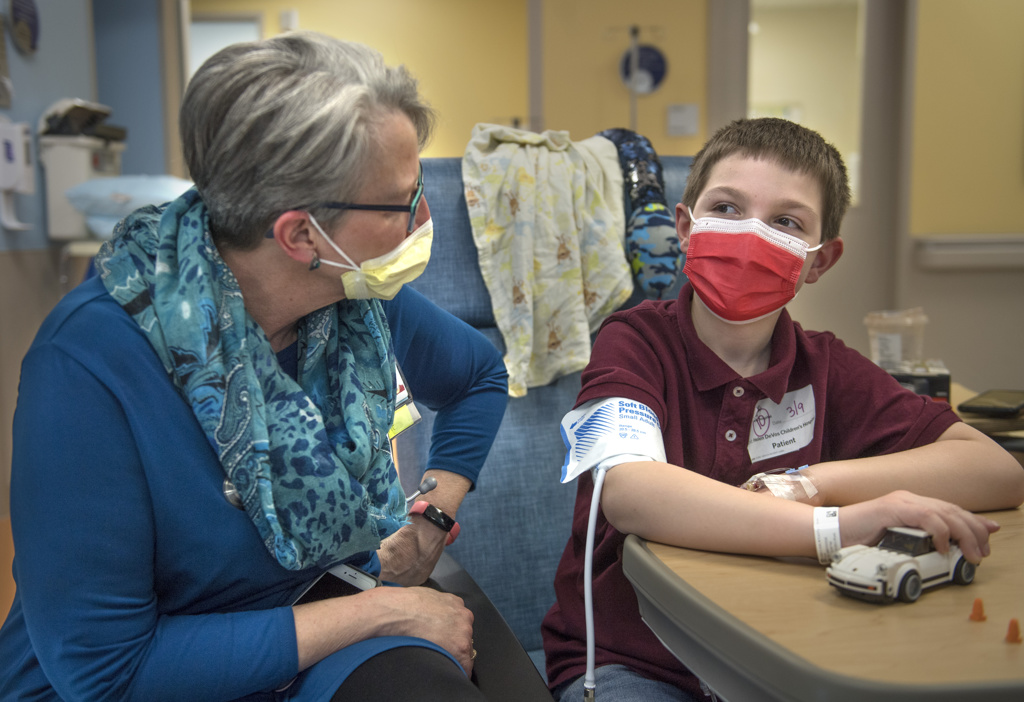
Spectrum Health genetic counselor Christy Bergeon Burns met with the Case family to answer their initial questions and explore next steps.
“The Cases wanted to know if Wyatt’s Hirschsprung’s disease was part of a larger syndrome,” Bergeon Burns said. “Genetic testing could help them understand more about what was happening to their son.”
Bergeon Burns collected information about the family’s medical history and helped the Cases understand the scope of the testing and anticipate potential results.
Laurie Seaver, MD, a medical geneticist in the Spectrum Health Helen DeVos Children’s Hospital Medical Genetics Program, met with the family next.
Dr. Seaver did a physical exam on Wyatt, looking for clues to help guide testing.
“Wyatt’s Hirschsprung’s disease was severe,” Dr. Seaver said. “It can be inherited, but usually is not. That was his originating diagnosis, but genetic testing can provide many answers, including whether it might be associated with other symptoms or health concerns Wyatt might yet develop.”
The genetic test itself is generally simple. A cheek swab kit was sent to the family to collect a sample from Wyatt and send back for the test.
Results take about two to three months to arrive.
Wyatt’s test led to some surprising discoveries.
The results pointed to Wyatt’s PHOX2B gene—also known as neuroblastoma phlox.
This gene provides instructions for making a protein that is important during development before birth. The PHOX2B protein helps support the formation of nerve cells and regulates the process by which the neurons mature to carry out specific functions.
“The genetic test indicated that Wyatt had congenital central hypoventilation syndrome, or CCHS,” Dr. Seaver said. “CCHS affects the drive to breathe. For most of us, that’s automatic—part of the autonomic nervous system.
“People with CCHS often have breathing issues, especially during sleep,” Dr. Seaver said. “And it can also lead to other issues. For instance, he doesn’t sweat very much, which is another autonomic response.”
New hope
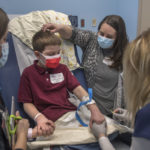
Given the Case family’s five-hour drive to reach the hospital, Dr. Seaver scheduled Wyatt’s visits with specialists in one trip—pulmonary and cardiac evaluations and an oncology evaluation to test for neuroblastoma.
“When we learned about Wyatt’s CCHS, I started to think about how he often had trouble waking up from anesthesia,” Melissa said. “From a sleep test, we learned that Wyatt had sleep apnea—that he stopped breathing 16 times per hour.”
Given that knowledge, Wyatt can be connected with Spectrum Health specialists to best meet his unique needs.
“Genetic testing can help us explain what is happening with Wyatt so that we can treat him proactively rather than reactively,” Dr. Seaver said. “Our hope now is to avoid or at least mitigate complications from his diagnosis.”
Melissa and Nate know there may be hard times ahead, given Wyatt’s unique challenges.
But they also feel like they have a little more control over the outcomes.
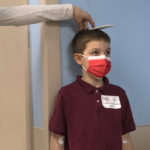
“He’s a happy kid,” Melissa said. “Yes, there have been intense moments in his life, in our lives. But there are also many delightful moments.”
They relish the enjoyment he gets when playing, building with Legos and Lincoln Logs. Wyatt is also enjoying his piano lessons and loves to draw.
Case remembers a moment when her son spoke up about his health struggles.
“He said, ‘Even though it’s bad now, it will not always be bad,’” she said. “We know now what we are up against in the future—and as a family we will handle it.”



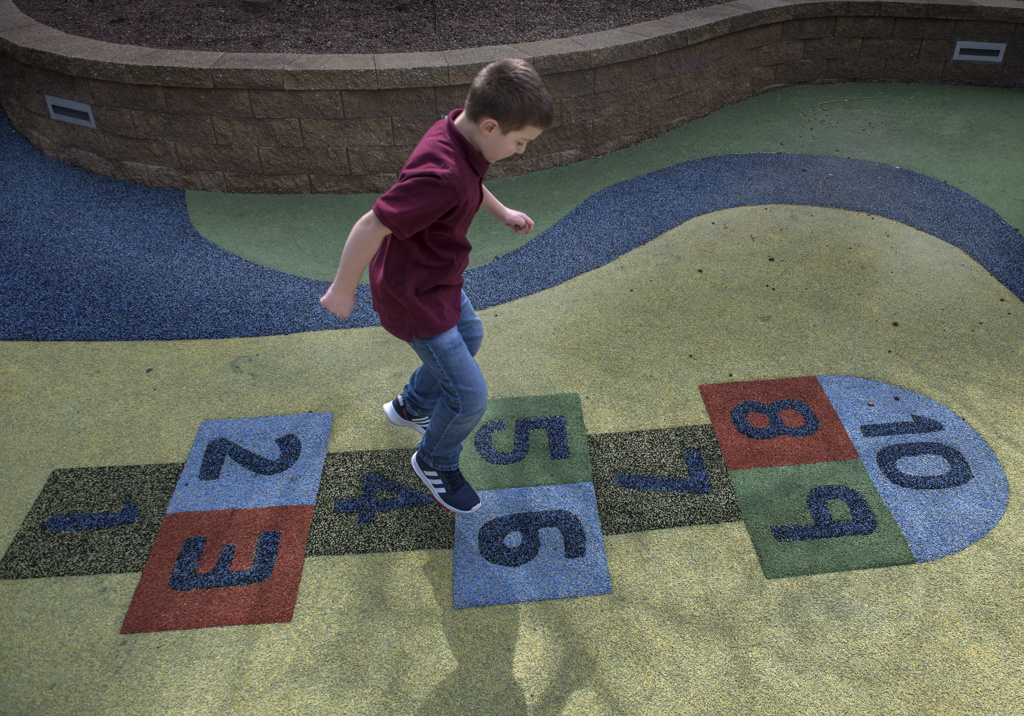















 /a>
/a>
 /a>
/a>
 /a>
/a>
Wyatt and his whole family are a joy to our community. He and his sisters are full of fun. Wyatt told us that his favorite song is “O the deep, deep, love of Jesus.” We are grateful for the excellent medical treatment available for people these days. Great information.