For 28 days—the entire month of February 2011—Christine Cox lay on life support in the Spectrum Health Fred and Lena Meijer Heart Center.
In late January that year she’d come down with a bad case of influenza—the H1N1 strain, which caused a pandemic during the previous flu season. Things quickly went downhill for Christine, resulting in pneumonia and respiratory failure.
An otherwise healthy 48-year-old, she almost didn’t make it.
Seven years later, on a recent Thursday afternoon, Christine and her husband, Steve, returned to the ICU where she was treated. She took a walk around the unit, greeted the nursing staff and reconnected with two doctors who helped save her life: Stephen Fitch, MD, and Greg Marco, MD, both specialists in pulmonary and critical care medicine.
Together, they recalled the roller-coaster ride of Christine’s illness and celebrated her remarkable recovery.
Early success story
Christine’s case stands out as an early victory for Drs. Marco and Fitch, pioneers in Spectrum Health’s use of ECMO in the adult ICU. ECMO is a mechanical system used to reoxygenate the blood of patients with severe respiratory failure or heart failure.
Christine’s case changed the doctors’ understanding of how long a respiratory patient could stay on this form of support—and recover.
“She was one of the early people that really stretched us to say, ‘Yup, you can go this far and you can get totally better,’” Dr. Fitch said. “It helped us sort of bolster the idea that if we just stay diligent and keep doing the right things … we can get to the other side of this and have a totally normal outcome.”
As the foursome gathered to talk, Christine listed the milestones in her life since her recovery: restarting her accounting business, witnessing the marriage of her youngest child and leading the effort to relocate and renovate the library in her town of Reed City, Michigan.
The doctors told her they still refer to her case when treating other patients needing lengthy ECMO support. What they learned from her experience helps them “take care of the next group of people that come through, and do a little bit better job,” Dr. Fitch said. “Take something that seemed unsalvageable and make it salvageable.”
Christine was curious: “Am I still the sickest patient you ever had that lived?”
“You’re right up there, I tell you,” Dr. Fitch said, laughing. “You’ve made the list for sure.”
50-day odyssey
Back in early 2011, Christine felt terrible after several days of bronchitis-like symptoms that didn’t respond to medication. After her third visit to her family doctor, she landed in the emergency department at Spectrum Health Reed City Hospital, a few blocks from home.
The medical team there recognized the severity of her illness and knew she needed specialized care. That same day, they called for an ambulance and sent her to Grand Rapids.
At Spectrum Health Blodgett Hospital, doctors connected her to a ventilator. Despite their best efforts, her blood oxygen levels didn’t rebound.
“Things progressed to the point where that wasn’t enough to support the body’s normal physiology,” Dr. Fitch said, noting that the ventilator also put too much pressure on her lungs.
The outlook was grim. A nurse advised Christine’s husband, Steve, to call the family together.
On duty that night was Dr. Marco, part of a small team of cardiothoracic intensive care doctors who had begun using ECMO at the Fred and Lena Meijer Heart Center downtown. ECMO, which had long been a standard therapy in pediatric care, was just emerging as a viable treatment for adults.
It would be a last-ditch effort, but if Christine could survive the three-mile ambulance ride downtown, the ECMO machine might be able to save her, Dr. Marco said.
It was, his colleague Dr. Fitch recalled, “a bit of a dicey proposition.”
The transport team kept her alive as they shuttled her downtown, and she went straight into surgery with Edward Murphy, MD, a cardiothoracic surgeon.
Thus began a 50-day odyssey in the ICU, most of which she spent in a medically induced coma.
Biding their time
The ECMO system uses a surgically inserted tube to funnel the patient’s blood into a machine that oxygenates the blood before pumping it back into the patient’s bloodstream through a second tube.
It forms a big circuit.
The goal was to get Christine stabilized on the ECMO machine, with added support from a ventilator, and give her body time to heal. For most patients, five to seven days can get them through a lung failure crisis and off the ECMO machine.
Christine proved to be an outlier. She wasn’t better even after three weeks. Instead, she faced complications.
In the course of her illness and treatment, she suffered broken ribs, two collapsed lungs and persistent bleeding in the space around the lung. Twice while on ECMO support, she underwent emergency surgery to evacuate blood from her chest cavity.
The doctors weren’t sure what to expect.
“You start to ask yourself … can this really get better? We don’t know. We didn’t know at that time,” Dr. Fitch said.
For Steve, who drove 140 miles roundtrip daily—leaving Christine’s side only so he could send their son Zack off to school each morning—the emotional toll proved heavy.
“It was up and down,” he said. “I’d get back to Big Rapids and I’d get a phone call saying, ‘You need to get back to Grand Rapids, now.’”
Finally, on the last day of February, Christine’s lungs became strong enough to sustain her without ECMO support.
It took six more days for her to come out of the coma. When she finally did, Steve said he “cried like a baby.”
From that point on, all progress was in the right direction.
“Every time they’d say, ‘Oh this isn’t going to happen,’ and then it would—and it was good things,” Christine said. “It all worked out. God’s guiding hands all over everybody.”
Road to recovery
For Steve and the rest of the family, it was the end of a long ordeal. But for Christine, a long road to recovery still lay ahead.
“Steve said, ‘I was so glad when you woke up because that meant the worst of it was over’—and then he realized it was just beginning for me,” Christine said. “I was in ICU 50 days and I only remember the last five.”
First there was a recovery phase in the hospital. Then there was inpatient rehab, with physical, occupational and speech therapy.
And though her rehabilitation went faster than expected—17 days inpatient rather than the estimated two months—her mental and emotional recovery still needed attention.
Christine needed to piece together her story. She needed to process the “bright light” near-death experience she had in the ICU. So about a year after her physical recovery, she sought out a psychologist, who helped her work through some strong lingering emotions.
Today, Christine makes a point of reaching out to other families going through traumatic medical events. She shares tips she’s learned and offers moral support.
“You know how they always say it takes a community to raise a child? Well, I think it takes a community to heal a person who’s sick,” she said. “When you start talking about it, you find out you’re not alone.”
Seven years later, Christine enjoys everything she did before—working, occasional teaching, camping, swimming, traveling. Her lungs are back to normal, with no residual damage. From the outside, her life looks the same as always.
It’s on the inside—the memories, the feelings of gratitude, the empathy for others—that Christine senses the difference that comes with being a survivor.

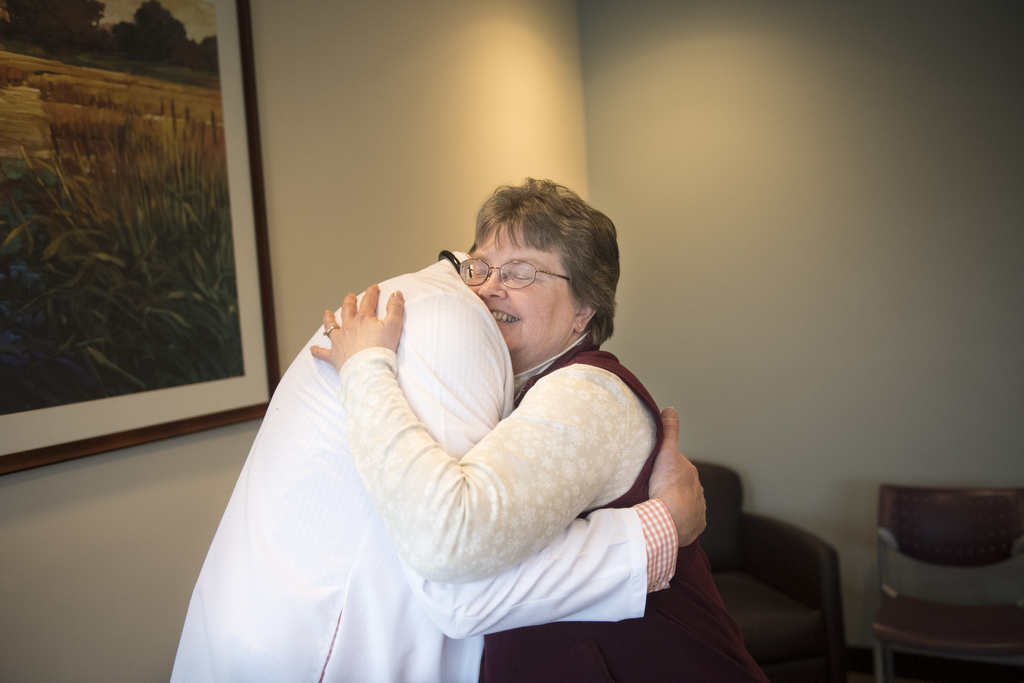











 /a>
/a>
 /a>
/a>
 /a>
/a>
Christine’s mother Connie was with her for nearly all of the time she was hospitalized. I followed Christine’s progress (or lack of ) from regular phone calls from Connie. I cannot imagine watching your child go through this medical catastrophe. Connie was faithful and strong. Reading this story was a tribute to the wonderful medical staff. Thank you.
Christine is such a strong woman. It was scary to watch this sicknesss. She is blessed in so many ways. The power of prayer and wonderful medical staff played a big roll in giving this beautiful lady her life back. Love you Christine!
I don’t know Christine, but I know she is a strong woman to have survived such an ordeal. My father back in the 90s got pneumonia and after just a few days contracted ARDS (Adult Respiratory Distress Syndrome ) It was a nightmare. Bad news just kept coming and one doctor after he was moved to another hospital that could deal with this tried the ventilator on what they would use for newborn babies. After ten days an x-ray came back not completely white, but with a little dark spot of hope. He was coma induced for that time. When he did survive he had had a lot of stories to talk about. It was very confusing to him and it took 3 1/2 months of recovery for him. We got to keep him another nine (9) years. It was precious time we never took for granted because our mother had died in 1983 of breast cancer. You are not alone and there were 20 other cases in that same hospital and two survived. My dad and another man. God Bless you all because it was God who did the divine healing and touched the doctors hands that treated them.
What a great testament to these two fine physicians that they persevered throughout the treatment and never gave up. So thankful for a great recovery for this great lady. I do not know her, but this story is so encouraging.
Thank you for your kind comment, Linda, and we’re so happy this article could be inspiring for you. Thanks for being a Health Beat reader! 🙂 Cheers, Cheryl Welch (editor)