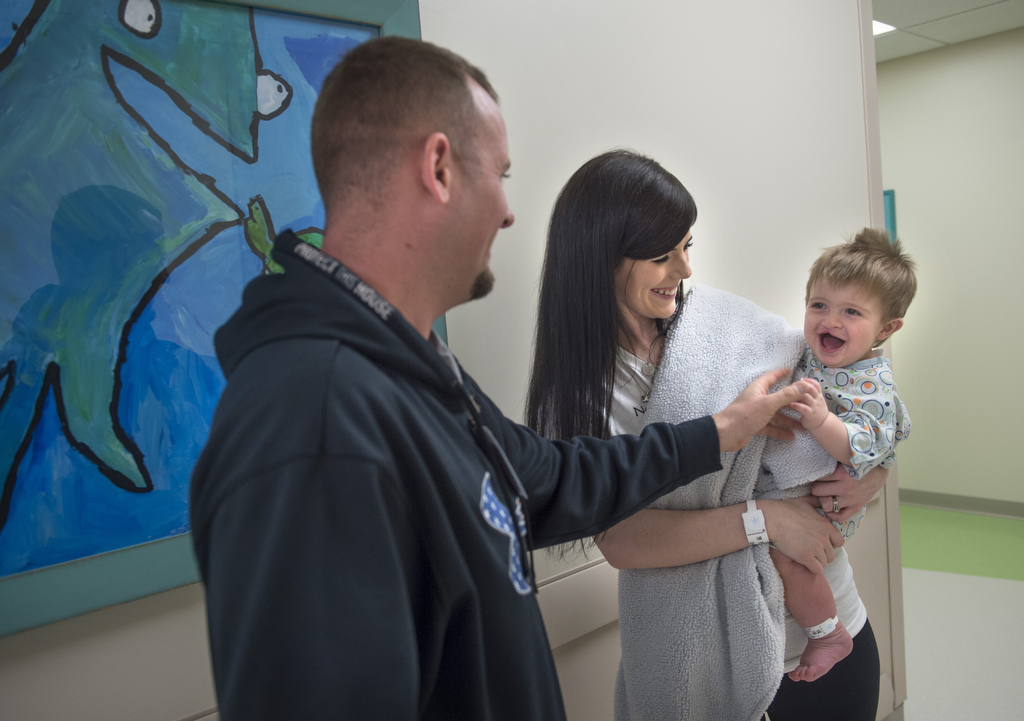
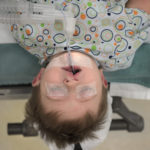
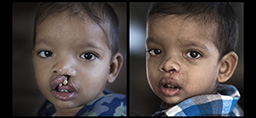
Nikki Roper did not expect to fall in love with her baby’s cleft lip.
But fall she did, the moment she lay eyes on her son John.
Now, as her baby undergoes surgery to his cleft lip and palate, Nikki is loving her baby’s smile through new phases.
“We are so blessed,” she said.
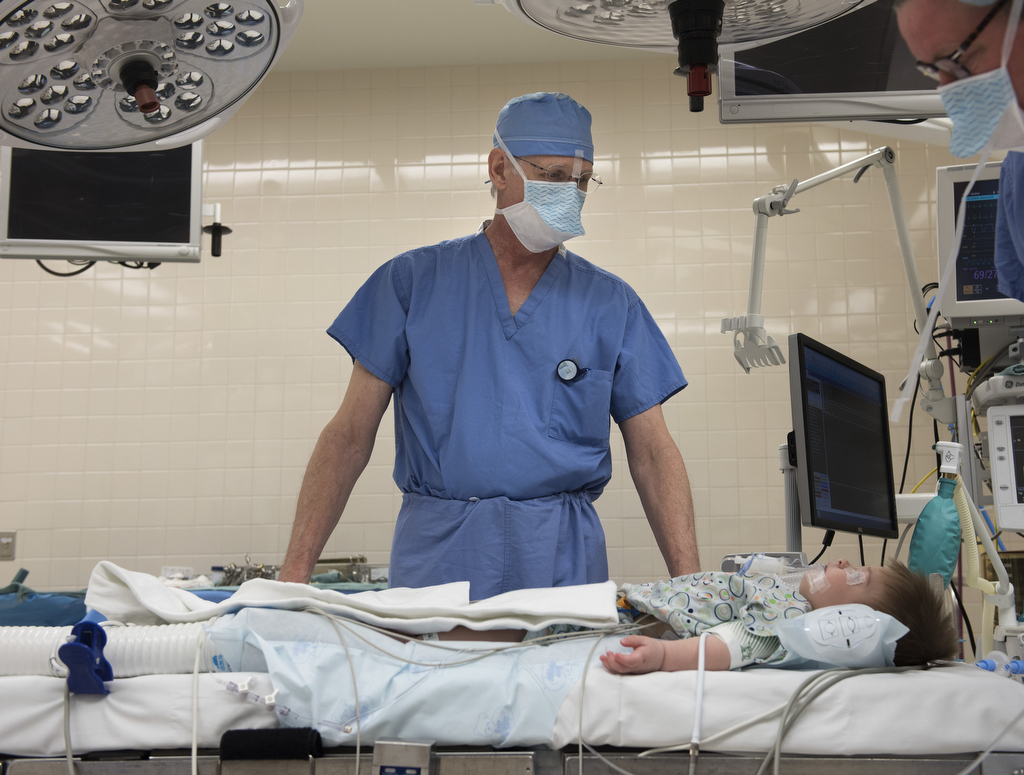
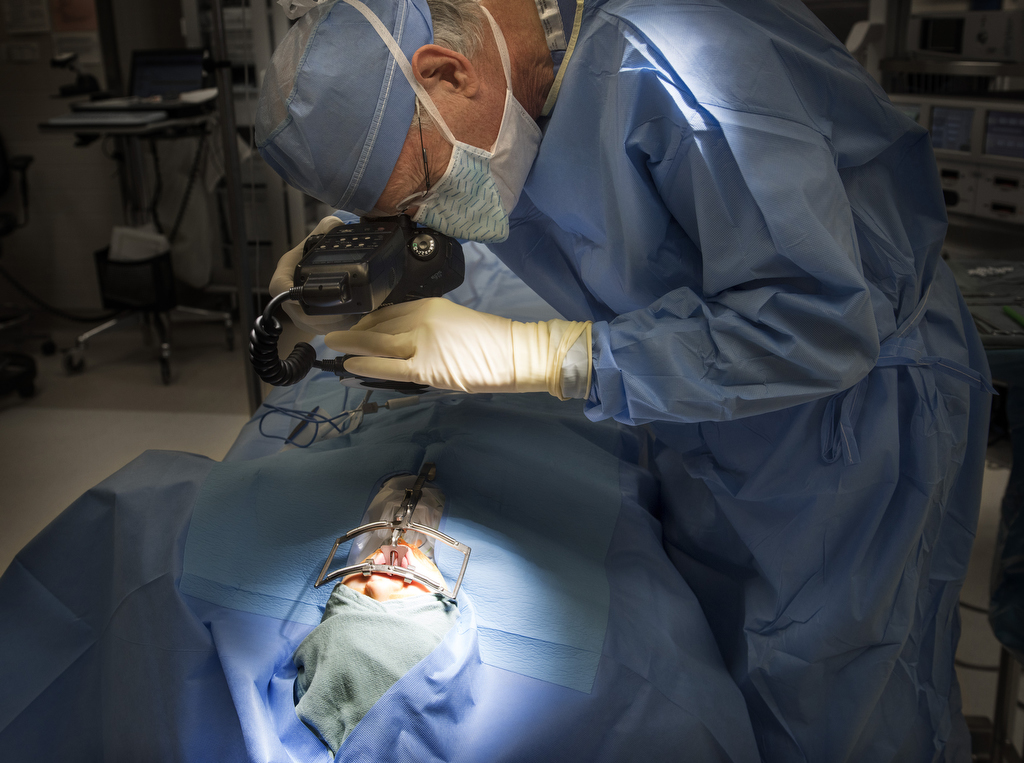
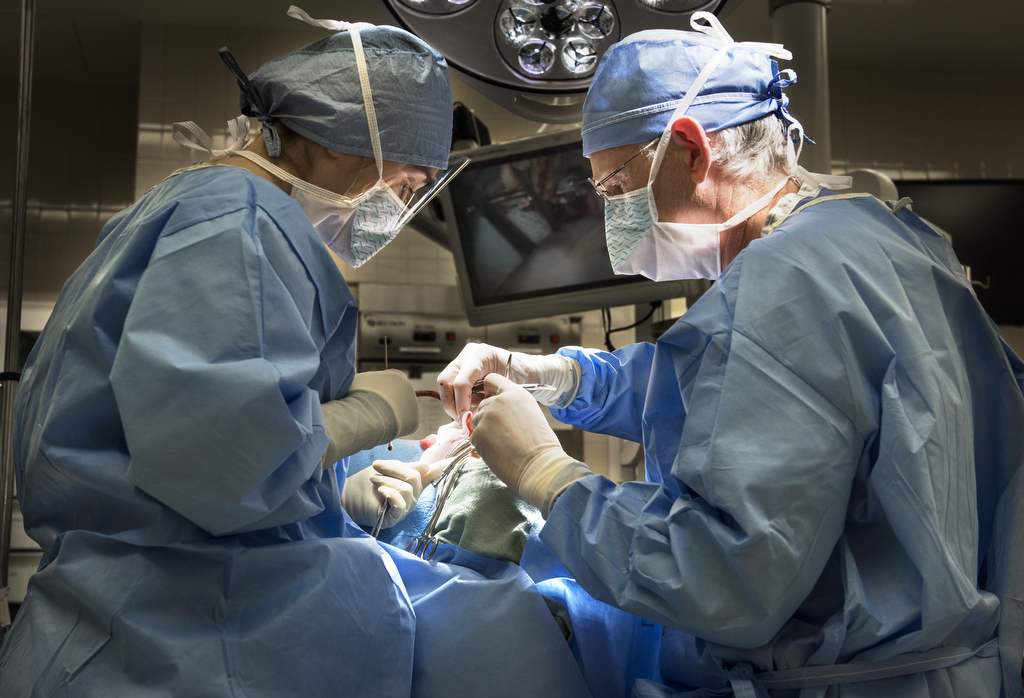
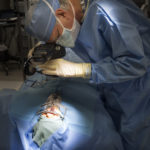
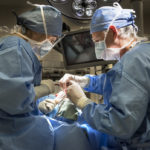
John is among the many babies to benefit from a cleft palate surgery technique developed and refined by Robert Mann, MD, a pediatric plastic and craniofacial surgeon at Spectrum Health Helen DeVos Children’s Hospital.
And now Dr. Mann is sharing that technique, honed over 30 years of practice, to help improve the lives of children worldwide.
Dr. Mann, director of the Helen DeVos Children’s Hospital Oral Cleft program, wants to share the dramatic results he has found in speech and facial development of kids with cleft palates.
He recently spent two weeks at Jubilee Mission Hospital in Thrissur, India, leading workshops with 17 surgeons from all over India brought in by Smile Train, an international charity that provides education and training for kids with cleft lips and palates.
The technique allows children to have fewer surgeries, a benefit for all kids, but particularly for those with little access to health care. Some kids may get only one shot at an operation in a hospital.
Nikki and Steve Roper found out their second son, John, had a cleft palate after the 20-week ultrasound. In the roof of his mouth, there is an opening to the nasal passage above, which affects a child’s ability to talk.
When she heard the news, Nikki burst into tears. She grieved―but not for long. Within hours, she found support and encouragement in the community and at the Oral Cleft program.
“At first, it was ‘Why us?’” Steve said. “Then we got over it. We knew it was fixable.”
Improving the fix
Dr. Mann began work on the technique, which uses cheek tissue to rebuild a palate, in his early days as a pediatric plastic surgeon. At the time, about 50 percent of the kids who underwent palate repair had speech that was “significantly substandard,” he said. Now, with this new technique, 94 percent of children have no speech problem relative to the palate.
Traditionally, surgeons have closed the gaps in palates by stretching the existing tissue across the open space.
“The wider the cleft, the more tension is on it,” Dr. Mann said. “The more you are pulling it together, the more likely it is going to pop open. Or, if it doesn’t pop open, it’s going to create much more scarring.”
Scar tissue slows the function of the palate muscles, which normally move as fast as a blinking eye.
The palate also supports the face. If the palate does not grow in balance with the lower jaw, a child can develop an under-bite. In some cases, a child needs surgery years later to lengthen the upper jaw.
“The fundamental thing I did 30 years ago is say, ‘Why are we just pulling things together?” Dr. Mann said. “We don’t do that anywhere else.”
If a patient has a wide wound on the arm, for example, plastic surgeons don’t just pull the skin together because it would interfere with arm movement. They add a skin graft.
“We add tissue to open defects. That’s what we do as plastic surgeons,” he said. “Why aren’t we doing that in primary cleft repair?”
Drawing on techniques of other surgeons and his own ideas, Dr. Mann began to use tissue from the inner cheek―a buccal flap―to rebuild the open palate.
Because cleft palate repair is performed on infants, it takes many years to see how surgery affects children as they begin to talk and as they grow into adulthood.
To see how the buccal flap performed over time, he analyzed data from 1,000 surgeries he performed. He also examined the evaluations of the patients done by speech therapists and orthodontists, who assessed the patients’ speech and growth.
- Ninety-four percent of the patients had “normal resonance” in their speech, up from 50 percent with earlier techniques. Normal resonance signifies that the palate is closing properly in speech.
- Only 11 percent of his patients were recommended for jaw surgery by their orthodontists when they reached young adulthood. This compares to the national average of 30 to 50 percent.
The results “are not perfect yet,” Dr. Mann said. “However, I am not aware of anywhere else where there is such a high degree of success when combining normal speech and the most normal facial growth.”
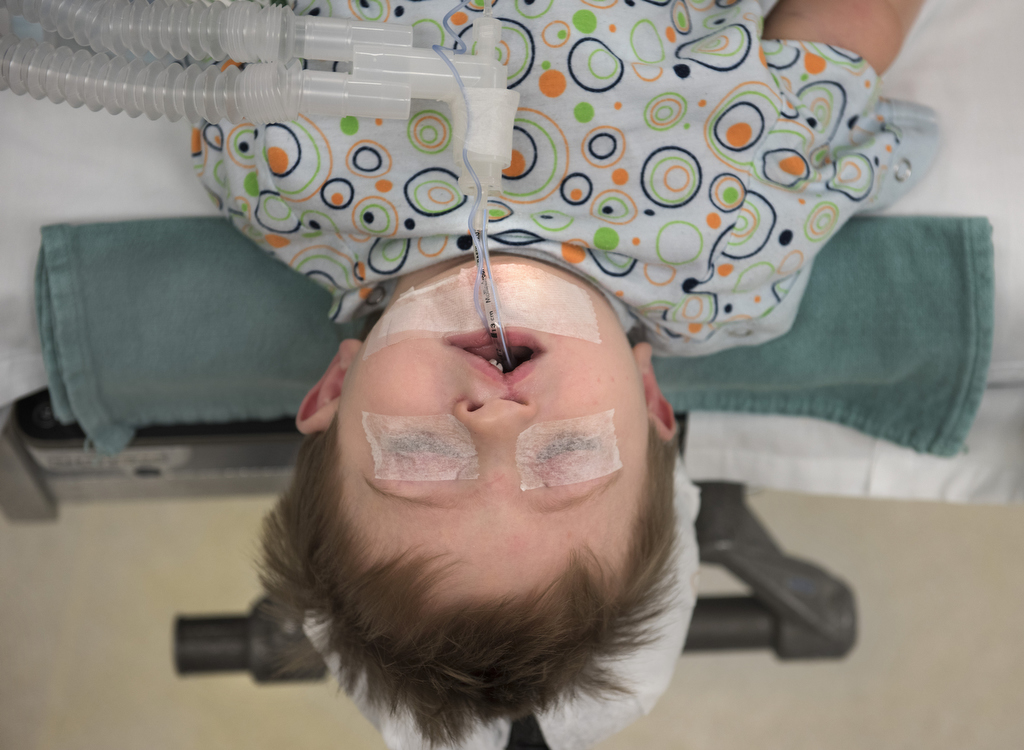
When John Roper was 13 months, Dr. Mann performed the operation on his cleft palate. The day after the operation, John was at home, playing with his 3-year-old brother, Jack.
“He’s so loving,” Nikki said. “He thinks it’s the funniest thing ever if he can make you laugh.”
In a few months, Dr. Mann plans to perform another surgery to straighten John’s lip.
In promoting the buccal flap technique, Dr. Mann hopes to help children born with cleft palates achieve normal speech and facial growth.
“For me personally, the development of this technique has been a great blessing and a privilege,” he said. “The opportunity to have such a positive impact on children’s lives that I directly treat is a wonderful gift. To have the opportunity to have the same impact on children all over the world that I have never even met is amazing.”













 /a>
/a>
 /a>
/a>
 /a>
/a>
My son was born with DiGeorge Syndrome. This resulted in bilateral cleft lip and palate. Dr. Mann is his plastic surgeon. To me he is a miracle worker!
Best wishes to you and your son! Thanks for commenting, Ann. I’m sure Dr. Mann appreciates your kind words.
Dr. Mann is an absolute miracle worker, and he’s so HUMBLE about it! We were so terrified when we found out our daughter had a cleft, but he eased all that fear before she was even born. He did the buccal flap procedure on her and she has never needed any speech therapy, her resonance is perfect, and she has minimal scarring. On top of it, she absolutely adores and trusts him! We go in this week for him to do more work on her nose and lips and there isn’t anyone else in this world I would trust more.
I didn’t realize that surgeons traditionally close gaps in palates by stretching the existing tissue across the open space. I can imagine how adding additional material would make the fix more supple and less impeding to speech functions. It sounds like it would be a good idea to inform yourself on pediatric plastic surgery procedures before choosing a surgeon for your child, so you can make sure that you are getting the type of solution you want.
Well said, Luke! Thanks for reading. 🙂