LeAnn Ouwinga sat in a chair in her waterfront home, gazing out the full bank of windows overlooking Spring Lake.
The lake, once fluid with the sounds of summer, had become motionless, a layer of ice covering a season that, on this winter day, seemed so long ago.
Did the silent scene remind her of her own medical journey—of long naps, little energy, minimal movement, a constant layer of heart problems that chilled her ambitions?
She lived this way. She doesn’t want to die this way.
“I was born with a defective heart back in 1950, when defective hearts were pretty much a death sentence,” said Ouwinga, sitting inside her home, surrounded by family photos. Her husband, Steve, sat across from her.
“They didn’t even know it when I was born,” Ouwinga said. “I was blue. Very blue. They put me in an incubator and thought I had just had trouble in the birth canal.”
But beneath the surface, the trouble ran much deeper.
They came to say goodbye
As a youngster, Ouwinga took long naps and had no energy. Her mom took her to a doctor, suspecting anemia.
“The doctor said, ‘Well, you know she has a defective heart,’” Ouwinga said. “My mom didn’t know. She was in shock.”
Ouwinga landed in the hospital on Thanksgiving Day 1957. Her temperature spiked to 107 degrees. Doctors diagnosed infection in her heart and pneumonia in both lungs. She spent three months in the hospital on IV medications.
She remembers her grandparents standing at her bedside in the wee hours, crying. She wondered why they were there when she was supposed to be sleeping.
She later learned they had come to say goodbye.
“They called my family in several times because they thought I wasn’t going to make it through the night,” she said.
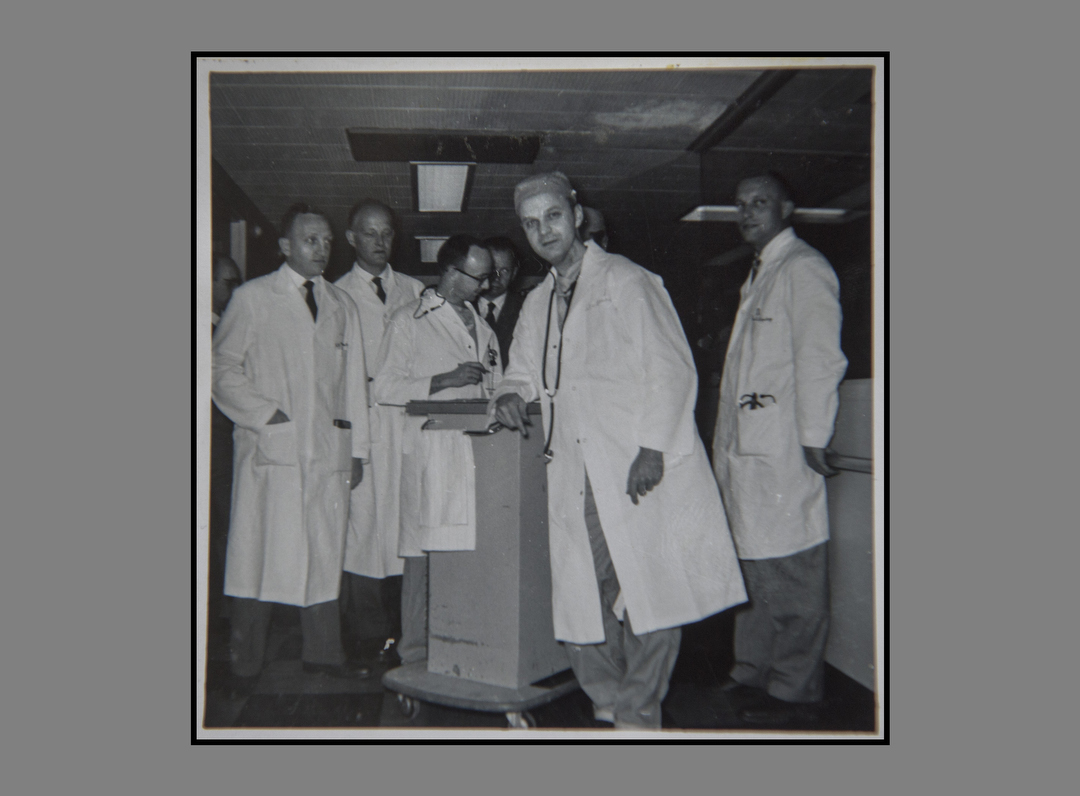
In May 1958, doctors in Minneapolis decided it was time to pull the trigger. Do nothing and the child may die.
Ouwinga became one of the first 250 open heart surgeries ever performed in the United States.
She became a local celebrity of sorts in her Minnesota hometown. The local paper wrote an article about her upcoming surgery.
Her narrow pulmonary valve needed to be stretched. Some fibers across her upper chamber blocked blood flow.
But if ever there had been a good time for open heart surgery, it was then.
The era marked the debut of the heart-lung machine, designed to provide blood flow during surgery. Prior to that, a child would typically be hooked up to a parent in a neighboring bed, with the child’s blood circulating through the parent’s heart to keep it oxygenated.
“Many of them died or became comatose from lack of oxygen,” Ouwinga said.
Even with the heart-lung machine, Ouwinga’s mom had to line up 12 donors to provide blood for the surgery.
And despite all the preparation and the new heart-lung machine, doctors told her parents the last 12 patients who underwent a similar surgery had died on the table.
Ouwinga was on the heart-lung machine for nearly 30 minutes during surgery, a record at that time.
She survived.
Pregnancy problems
Ouwinga returned home after a few weeks. Although she had to take it easy for a time—lots of napping, no playing outside with neighborhood kids, no going up and down steps—she healed well.
“I never saw a cardiologist again until I was 22 and pregnant,” she said.
At that time, she lived in Grant, Michigan. A doctor measured her resting heart rate at 180 beats per minute. That led to a cardiologist appointment at Spectrum Health Butterworth Hospital.
Medication helped control her heart rate. Bed rest for seven months helped protect the baby.
After Ouwinga had two babies, the doctor told her she should never get pregnant again. So instead, she adopted two more daughters.
Ouwinga didn’t see a cardiologist again until just two years ago.
By this time, the family lived in Spring Lake, Michigan, with their mesmerizing waterfront window on the world.
Life seemed calm, but her heart did not.
Several years ago, Ouwinga felt her heart racing.
“I always had an irregular heartbeat and always had a heart murmur,” she said. “But I started feeling more irregular heartbeats and harder heartbeats.”
She tried walking and biking with friends.
“I could never get any stronger,” she said. “I always felt tired, always felt like I was tagging along behind. I thought, ‘This just isn’t right.’ It would race real fast sometimes and I’d have this tight feeling in my chest.”
Surgery revisited
Then, about two minutes into a stress test treadmill drill two years ago, the doctor told her to stop.
“I was going into ventricular tachacardia,” she said. “That’s what can cause people to drop dead on the basketball court. Your heart can handle it for 30 seconds, then you drop over dead.”
The cardiologist recommended Ouwinga cancel her plans to visit her sister in Texas, and instead opt for immediate surgery.
“My mitral valve was totally shot and my pulmonary valve was leaking bad,” she said. “That’s why I was so tired.”
Ouwinga underwent heart surgery at the Fred and Lena Meijer Heart Center on April 20, 2015, five days before her 65th birthday.
Spectrum Health Helen DeVos Children’s Hospital Congenital Heart Center pediatric cardiovascular surgeon Marcus Haw, MD, repaired her leaking mitral valve and replaced her pulmonary valve.
“I’m doing well,” Ouwinga said recently. “I’m walking. I’m a lot less short of breath. I’m not experiencing rapid heart palpitations and irregular heartbeats as much. I was so bad before, if I got up to go to the bathroom I would have to sit on the edge of the bed until my heart slowed down.”
As a result of Ouwinga’s childhood congenital surgery, she developed abnormal heart rhythms and ventricular tachycardia, said Helen DeVos Children’s Hospital adult congenital cardiologist Stephen Cook, MD, FACC.
Ouwinga suffered from pulmonary valve stenosis, which occurs in 7 to 10 percent of patients with congenital heart disease, according to Dr. Cook.
He said Ouwinga’s experiences illustrate the importance of lifelong follow-up.
“Her condition is now stable and improved, but she still deserves lifelong follow-up to evaluate the function of her replaced pulmonary valve and interrogation of her ICD device to determine if she has any evidence of recurring arrhythmia,” Dr. Cook said.
But Ouwinga’s story doesn’t end here.
She’s part of an adult congenital heart study at Helen DeVos Children’s Hospital. She hopes to help unlock the mysteries so other children can avoid the lifelong heart issues she had to endure.
“I thought once that surgery was done when I was 8 years old that they had fixed what they could and I was good to go,” she said.
Instead, she’s passing along the gift of knowledge, a gift she’s spent a lifetime learning.
“This whole experience has made me feel like I have to make my days count,” Ouwinga said. “God has blessed me so much, including having wonderful, talented doctors and nurses who cared for me throughout my medical journey. Out of gratitude to Him, I have a strong desire to be His hands and feet.”
Besides participating in the congenital heart study, she teaches kids in her church, helps with a bed ministry, sews blankets for new mommy bags for the Alpha Ministry in Grand Rapids. She mentors at Hope House in Grand Haven and goes on works projects with Samaritan’s Purse.
“We praise God and are thankful for Him for His goodness to us,” Ouwinga said. “We’ve been so blessed. I feel like one of my purposes in life is to give to others.”





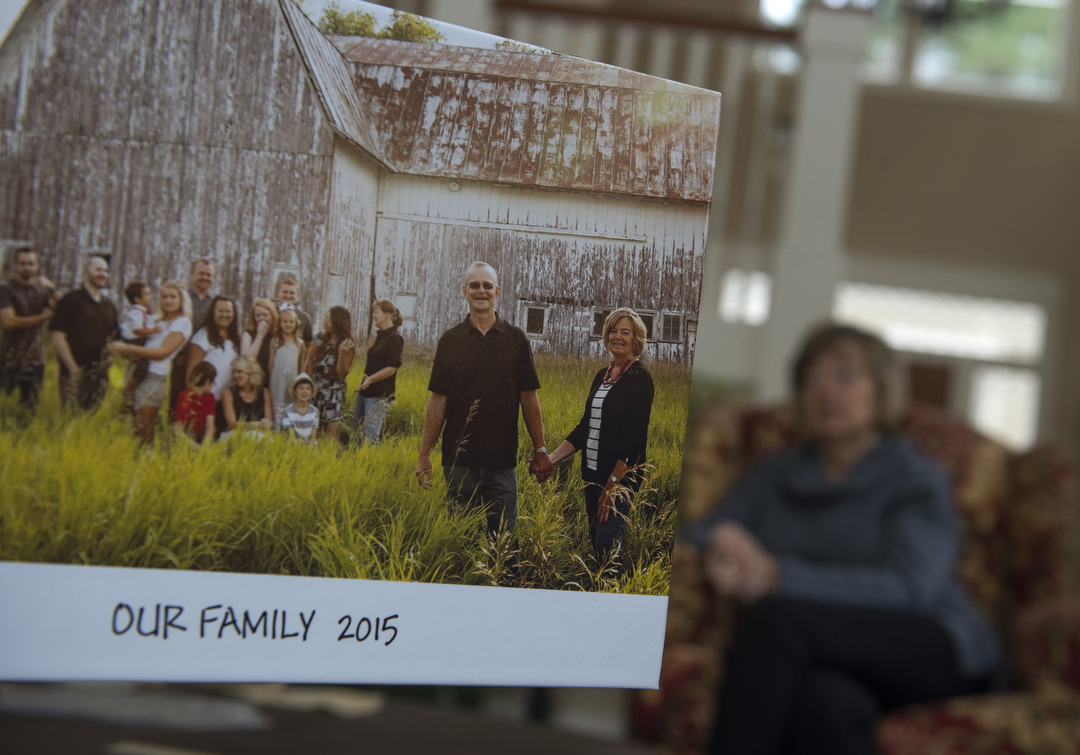






 /a>
/a>
 /a>
/a>
 /a>
/a>
Isn’t it great how far medical technology has come? I have a very similar story. I was born with Tetrology of Fallot. My parents were told I would not live to be one year old. I had surgery in Chicago when I was 8 years old (not open heart). When I was 18, I had open heart to repair all the defects. My surgery was at Blodgett Hospital and Dr. Richard Rassmussen did the surgery. I am now 73, and with the help of a pacemaker for the last 52 years, I am doing well. It was nice to read your story, LeAnn. Isn’t God great!
How wonderful! Thank you for sharing your inspiring story, Carol! We are so happy you’re doing so well. Cheers, Cheryl
LeAnn I knew of your heart history but not to this detail. Enjoyed reading how you have been showered in Gods Grace. May He continue to bless you with daily strength.
Thank you for sharing your story, Carol. Yes, God has blessed both of us do much!
Hi Carol,
I’m glad to hear you are doing well.
I believe I know you. I remember a Carol who had heart surgery at 18.
Hi Carol! I lost my sister to a congenital heart and worse yet, my first born daughter passed away in my arms in 1964 from congenital heart – she had only 1/2 of a heart. I am also thankful to God that you are doing well. God has worked miracles through advanced technology over these many years – God is so good and prayer is so powerful!
Hi Carol, Thank you for sharing your experiences with congenital heart and hope for today and tomorrow’s technological advancements in this field. Many warm wishes sent your way from Health Beat. 🙂
LeeAnn,
I met you when Cuyrt had his valve surgery and your parents told of your surgery as a child.
My dad has had his mitral valve replaced twice and his aortic valve replaced once. All three surgeries were successful. The second mitral valve was replaced when the previous implant became defective after years of use.
His sister had the same surgery last year at 93 and is doing well now too.
Knowing of your dad’s valve replacement, I would wonder if there is any study of a genetic connection being studied at this time
Beautiful and inspiring stories ( the actual article as well as the first comment). Congenital heart defects certainly are serious, but the medical advances in this area are truly amazing!
Thank you, Teresa! We appreciate you being a Health Beat reader! 🙂
My daughter is a veteran of three open heart surgeries. She works a fairly physical job at auto zone. Her last surgery was done by dr. haw. doing well all the way around.
So glad your daughter is doing so well, Bernie! Thanks for sharing. 🙂
Great article about Lee Ann. Open heart surgery has come a long way since the 1950s. So glad that she is willing to participate in this group at HDVCH.
Thank you.
Thank you for sharing your “heart-warming” story! Your medical journey spans a lifetime and yet your focus is outwards and on helping others. May God continue to bless you in all that you do!
MAY GOD CONTINUE TO BLESS YOU ! WE LOST A 20 YEAR OLD DAUGHTER FROM WHAT I CALLED A POOR DIAGNOSIS BY A POOR CARDIOLOGIST BACK IN 1990. IT IS GOOD TO SEE ADVANCEMENT OF THE MEDICAL DOCTORS TODAY, THEY ARE GREAT PEOPLE, I KNOW, IN THAT I AM AN AMALOIDOSIS PATIENT .
Hello Michael, We’re sorry to hear about your daughter. It is remarkable how far cardiology has advanced in the past few decades.