Brenda Crandall refuses to be caught with her back against the ropes again.
As an advanced ovarian cancer survivor, she knows well the jab-to-the-spirit blow that a cancer diagnosis packs.
She’s lived through the pain, the fear, the uncertainty of not knowing if her next monumental life event would involve celebrating a cancer-free diagnosis, or taking her last breath surrounded by family.
With the conviction of a prizefighter whose ultimate prize is life itself, Crandall is beating her foe.
But the Traverse City, Michigan, woman is not standing still as she does it.
She’s ducking and darting, making every proactive move she can to stay ahead of her enemy.
‘I’ll be back. I promise’
It’s 7:28 a.m. on Sept. 27, 2016.
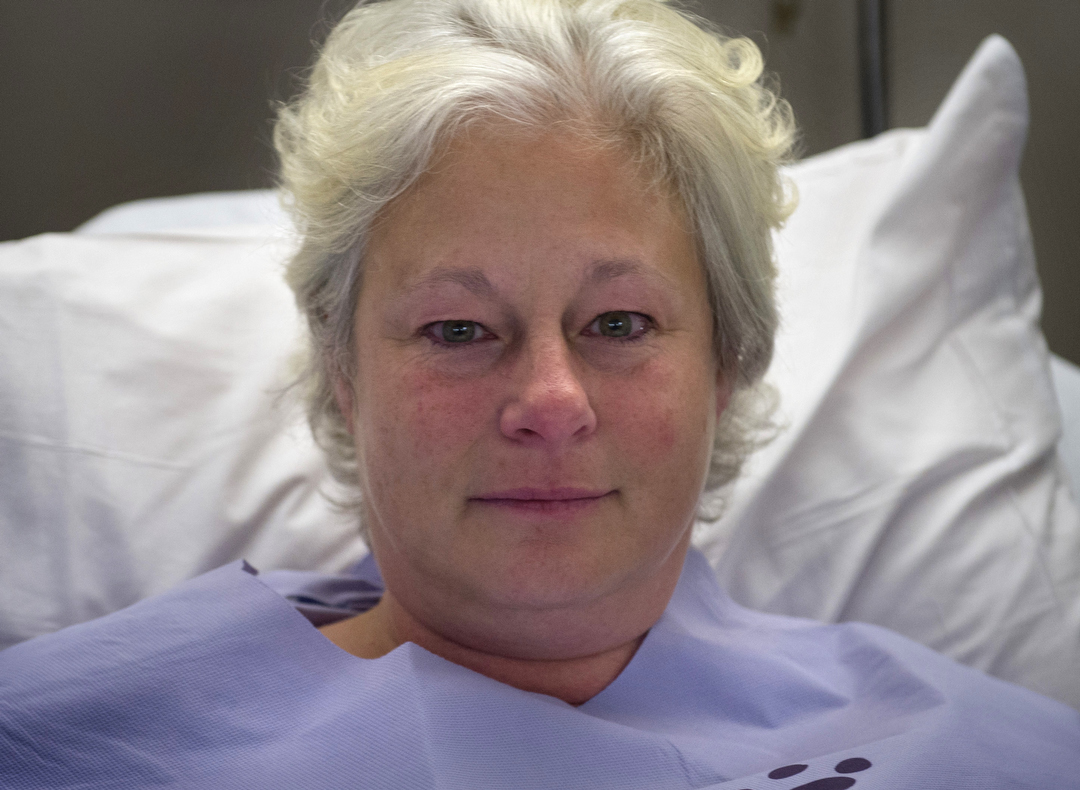
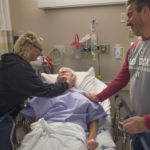
Crandall, 45, is lying on a gurney in the Spectrum Health Butterworth Hospital second-floor surgical holding area, awaiting a double mastectomy.
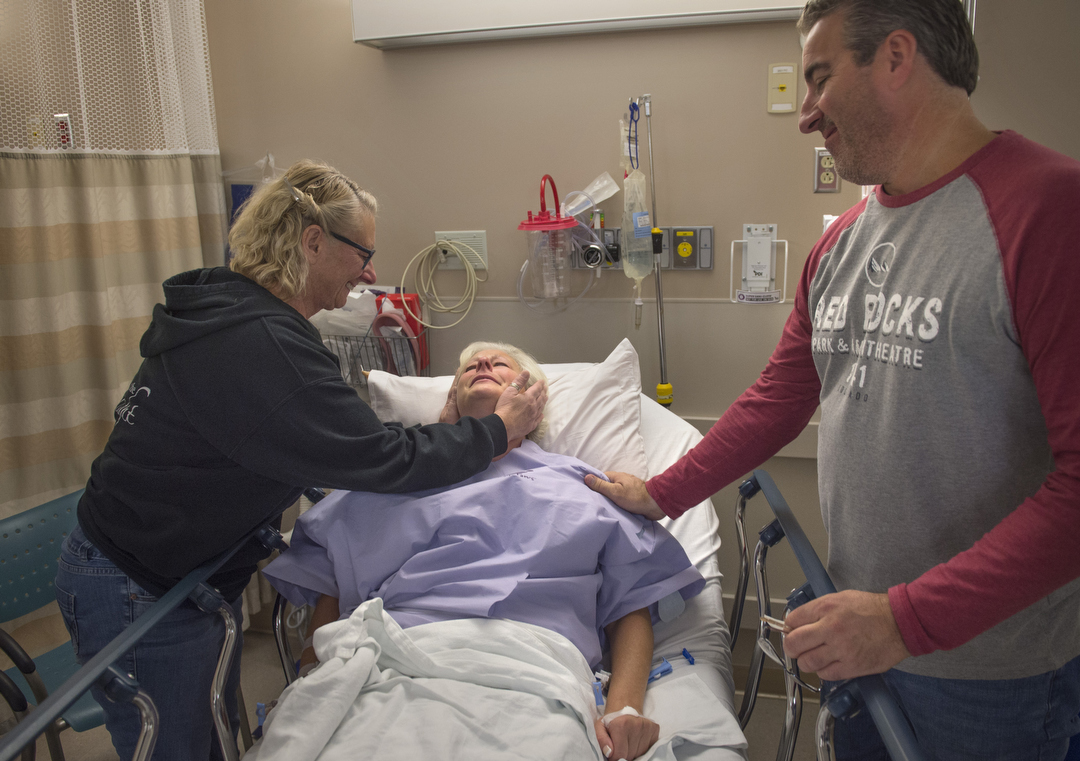
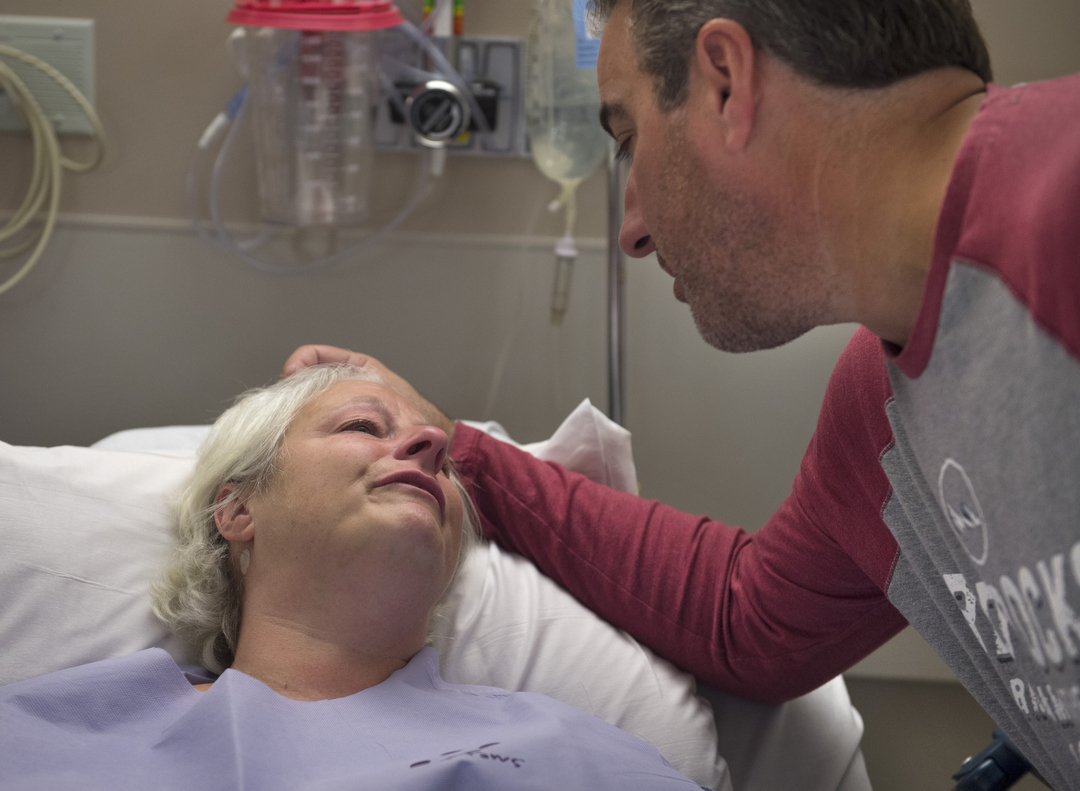
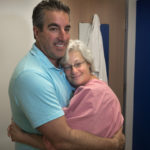
She kisses her husband, Tom, goodbye.
“I’ll be back,” she says through tears. “I promise.”
Her sister, Linda, who came up from Adrian, Michigan, wishes her well.
“See you when you wake up,” Linda says.
“I’ll be there,” Crandall replies, the tears falling harder now. “I’ll be there with no breast cancer.”
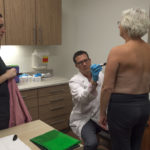
In recent months, she had many discussions with Spectrum Health genetic counselors, Melinda Miller, MD, a breast surgery specialist with the Spectrum Health Cancer Center and Shannon Armstrong, MD, a plastic surgeon with Elite Plastic Surgery.
In the course of those meetings, she learned she’s a carrier of the BRCA 1 gene mutation. It gives her an 87 percent chance of developing breast cancer.
She knew what had to be done: Remove any vulnerability.
She’d rather lose her breasts than her life.
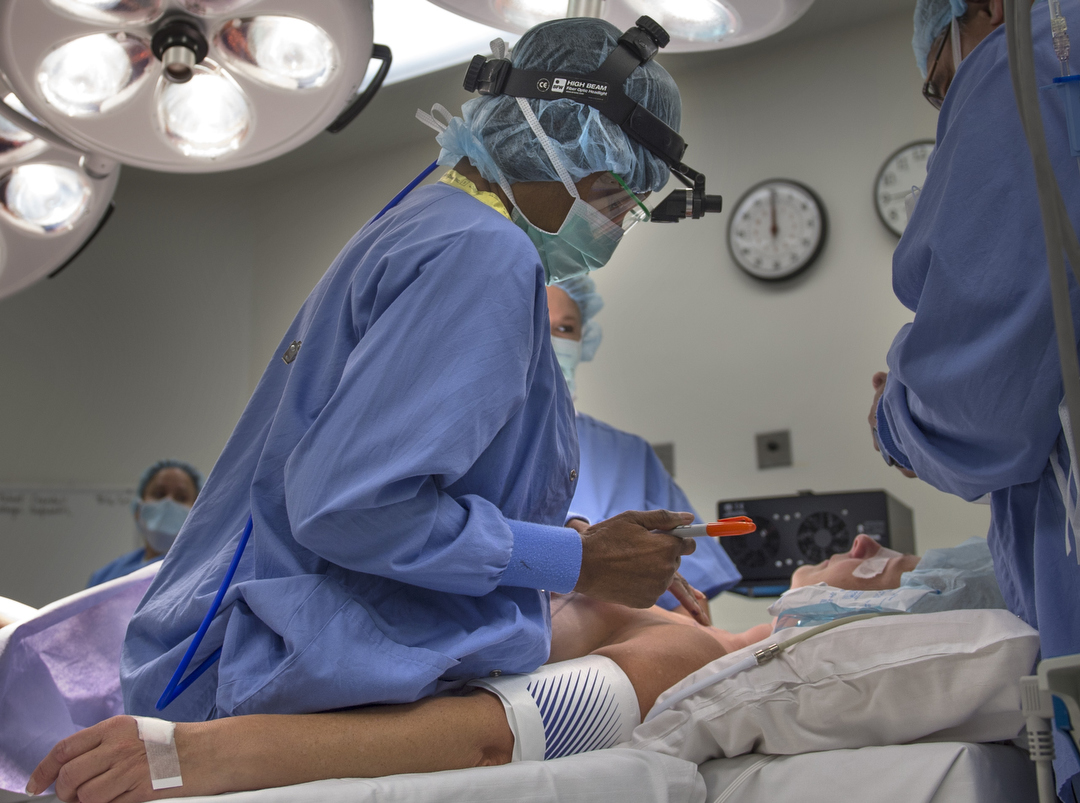
At 7:34 a.m. on this chilly September morning, staff wheel her into operating room 11.
A nurse confirms the procedure about to be performed.
Crandall chats for a few minutes.
By 7:43 p.m., she nods off from the anesthesia.
Six hours in surgery
Shortly after 8 a.m., Dr. Miller begins the procedure.
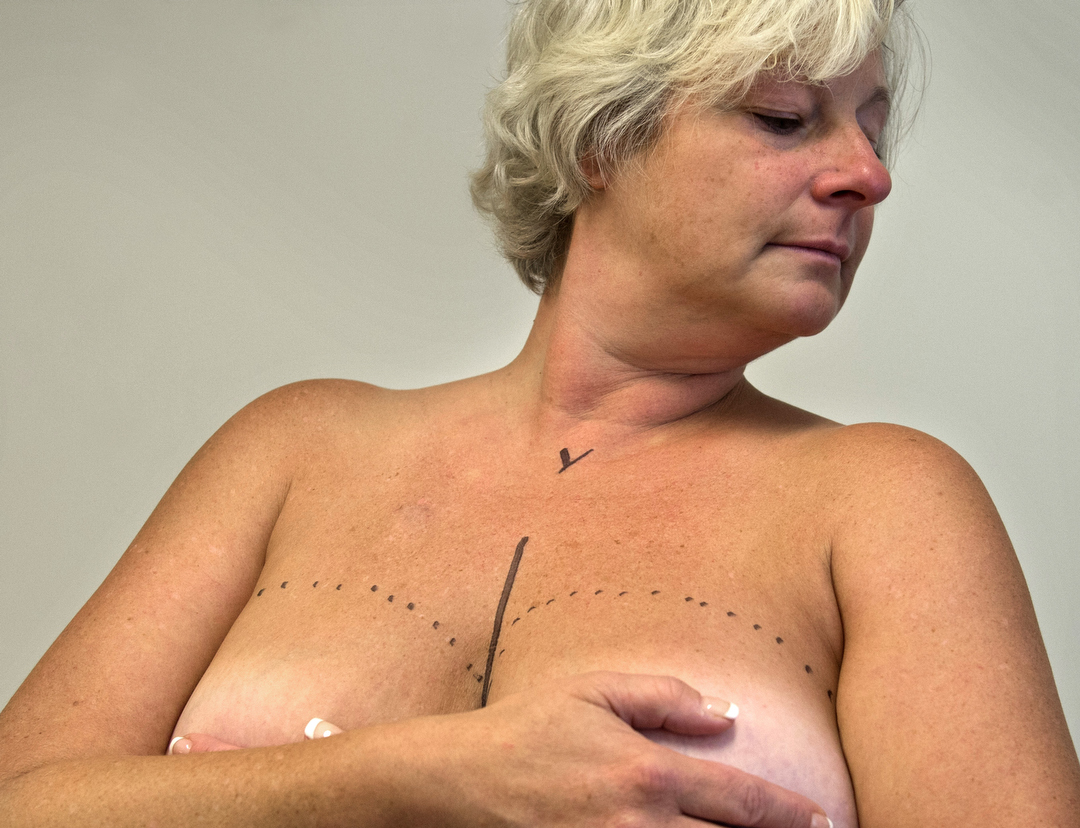
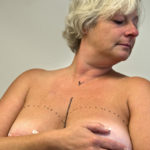
She follows the markings made by Dr. Armstrong a day earlier, and makes incisions above and below Crandall’s nipples.
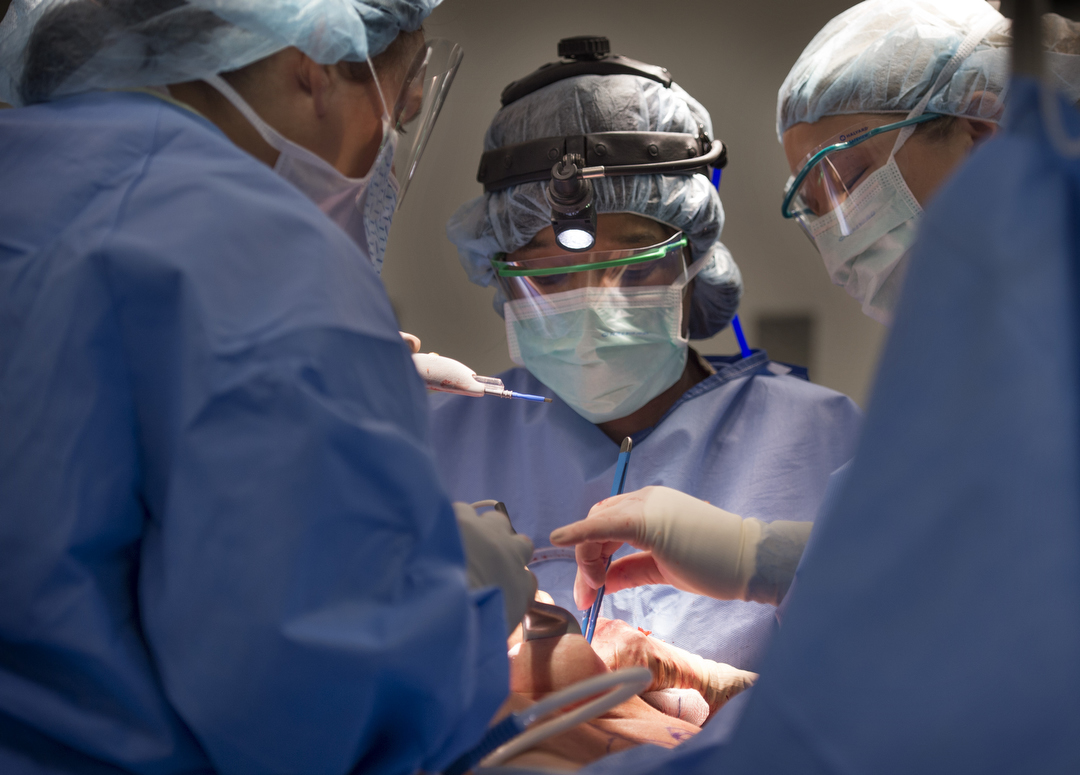
For the next four hours, she carefully separates Crandall’s breast tissue from her skin and muscle, first on her right breast, then on her left.
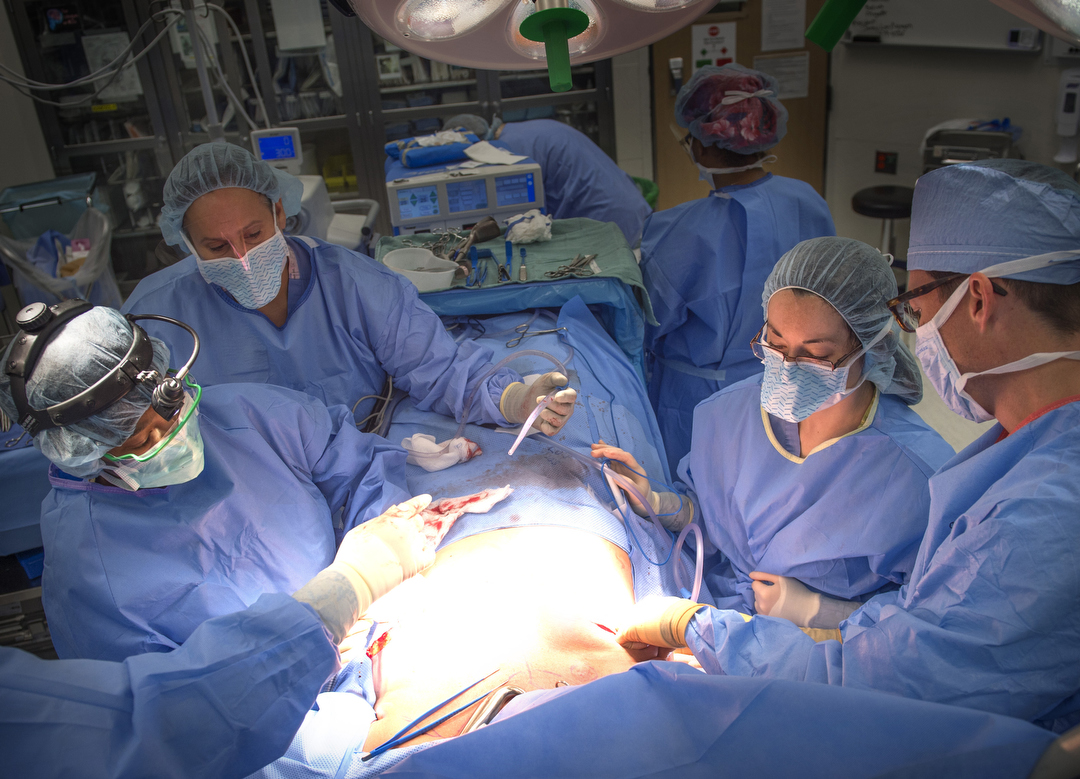
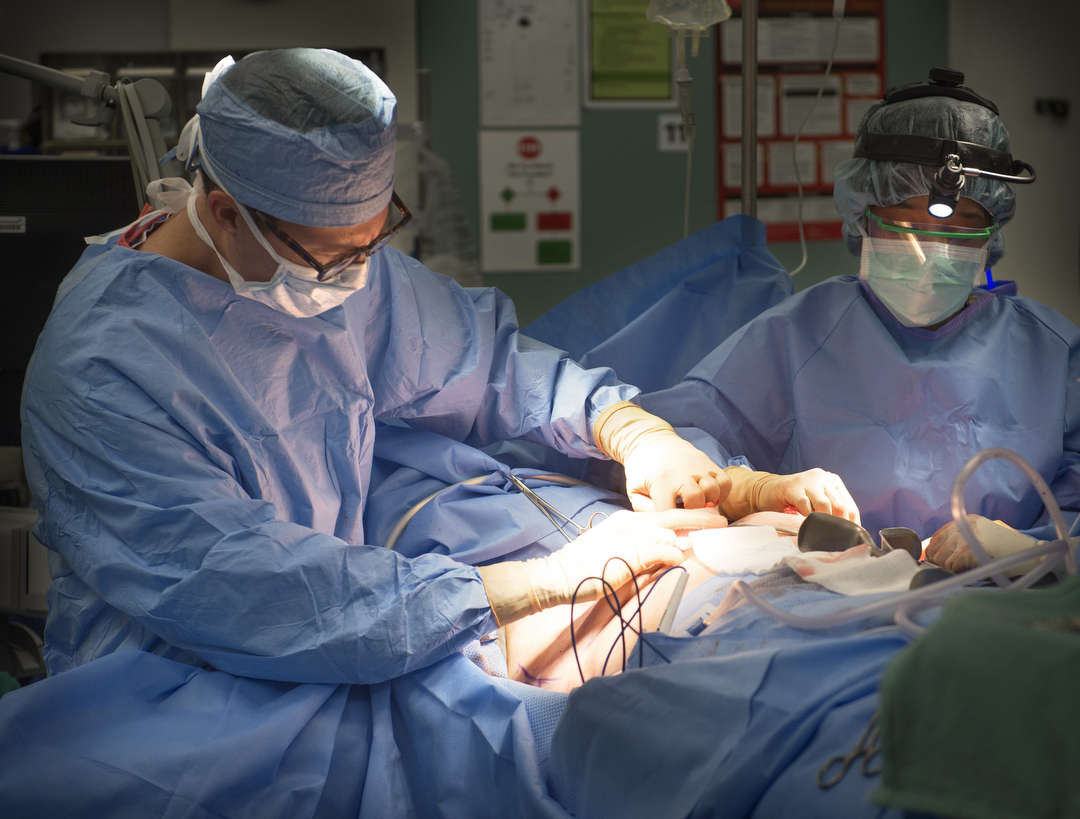
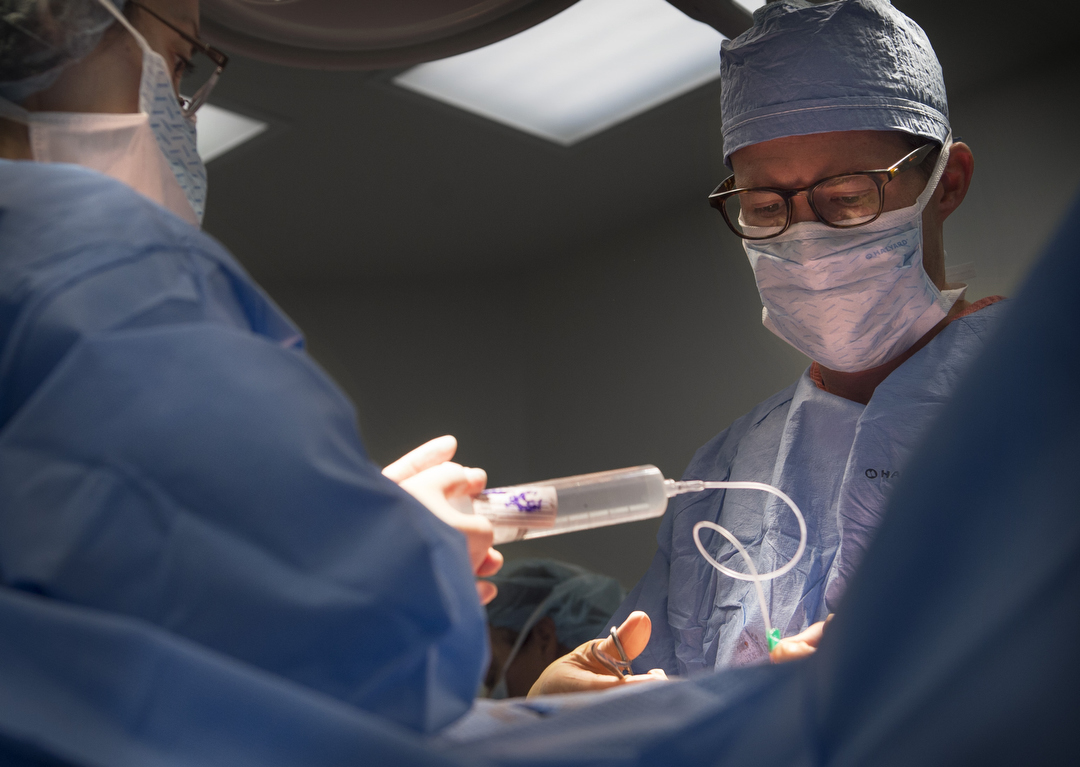
It’s a tedious procedure, but after dividing the layers, she lifts the breast tissue out. Each weighs more than 2 pounds. Dr. Armstrong arrives shortly after 10 a.m. and begins reconstruction. He starts with Crandall’s right breast as Dr. Miller continues to separate tissue on her left breast.
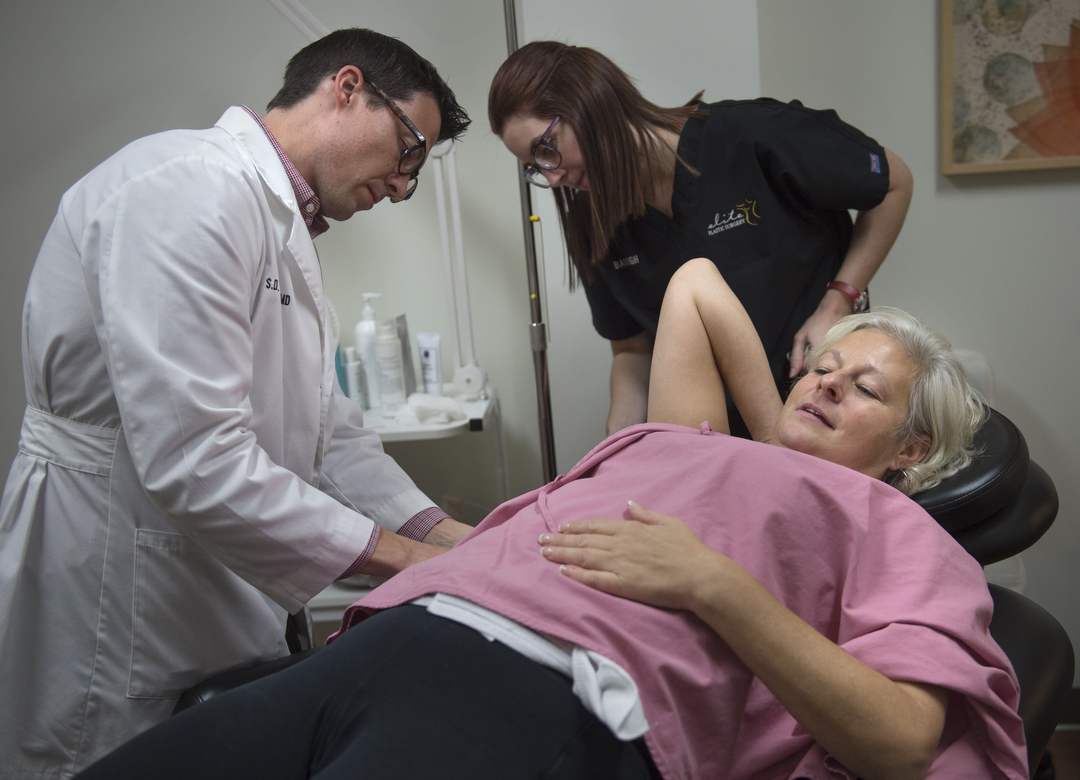
Dr. Armstrong places expanders that can be filled with saline solution, sized to Crandall’s desire. She will visit Dr. Armstrong every week through the end of the year to gradually stretch the area.
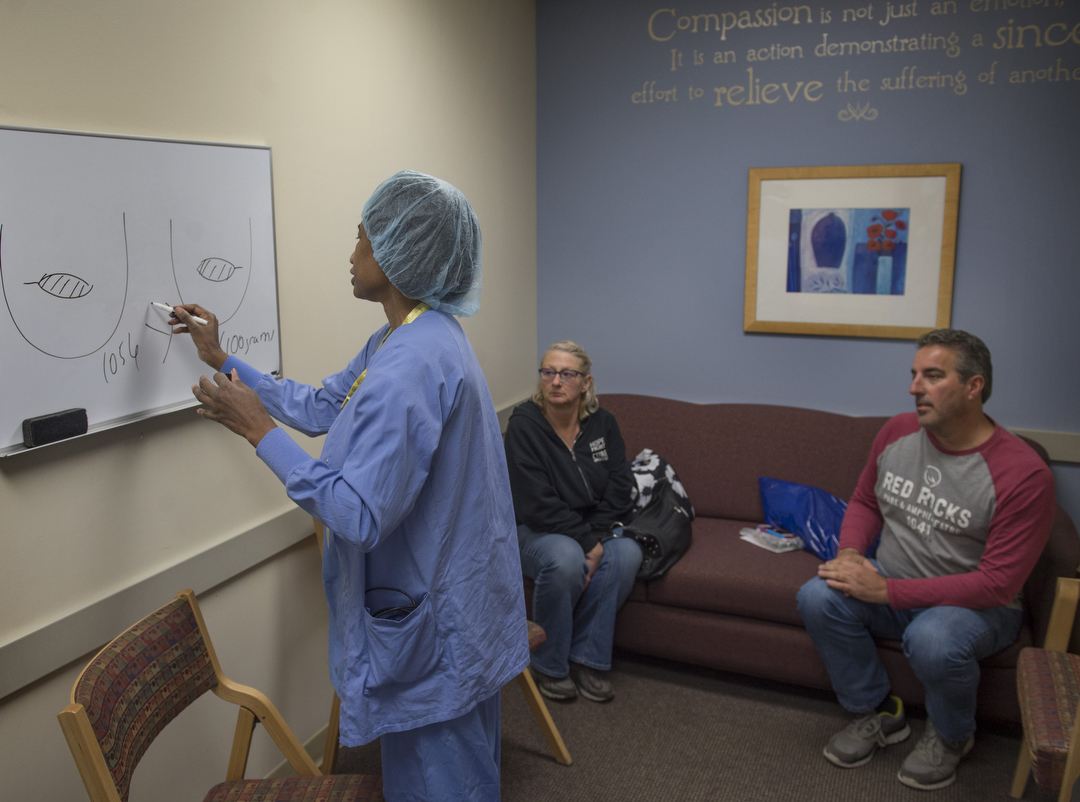
As Dr. Armstrong continues to work, Dr. Miller completes her portion of the procedure and meets Crandall’s family in a conference room to deliver the good news.
“I didn’t see anything in her tissue that looks suspicious,” Dr. Miller tells Tom and Linda. “Everything looked normal.”
She draws diagrams on the whiteboard, explaining the procedure and the post-op realities.
“Her muscles are going to spasm,” Dr. Miller says. “We’ll use medication to relax those muscles and medication to manage her pain. Initially, she may need it around the clock.”
Dr. Armstrong later delivers more good news.
“She did great,” he says. “There were no surprises.”
Listen to your body
And now, Crandall hopes she has no more surprises, like the ugly one she received in late 2014—stage 4 ovarian cancer.
She hopes other women learn from her experience and take a proactive role in limiting their exposure to cancer risk.
The mastectomy effectively dropped Crandall’s chances of developing breast cancer from 87 percent to five percent, according to Dr. Armstrong.
Crandall also encourages women to listen to their bodies. She didn’t at first when she started experiencing subtle symptoms. Retrospect can be a cruel teacher.
“Looking back, I probably had some symptoms but didn’t know they were symptoms,” she said. “I was feeling full fast. I had light flutters that went on in my belly, like little electrical shocks.”
She passed her weight gain off on her 2011 partial hysterectomy, and a summer of barbecue and beer.
But symptoms persisted. It became more difficult to eat and drink. Her pants weren’t fitting. Diarrhea struck almost every day.
The Saturday after Thanksgiving in 2014, Tom took her to urgent care. A nurse practitioner recommended a vaginal ultrasound, because her symptoms sounded like possible ovarian cancer.
The first week of December, scans showed a loaf-of-bread-sized mass on her right ovary.
By mid-December, Gordon Downey, MD, a Spectrum Health gynecologic oncologist, confirmed the dreaded suspicion. Stage 4 ovarian cancer.
She underwent several rounds of chemotherapy to shrink the tumor. On St. Patrick’s Day of last year, Dr. Downey spent four and a half hours removing cancer from her ovaries, fallopian tubes, colon and belly fat lining.
She didn’t want to replay that scene ever, ever again. Not in her breasts. Not anywhere.
“Early detection is key to some people,” she said. “I’ve already had cancer. For me, it’s being proactive. I might be the only one in the world, but as soon as I heal from this mastectomy, I’m asking for a colonoscopy.”
She’s looking forward to that healing. And getting back to walking the beach in front of their Grand Traverse Bay home. And next summer, boating again.
She hopes the years are many. And kind. And that her proactive measures knock the enemy from the ring.
She vows to keep fighting.
“At almost 46, I hope to live,” she said.







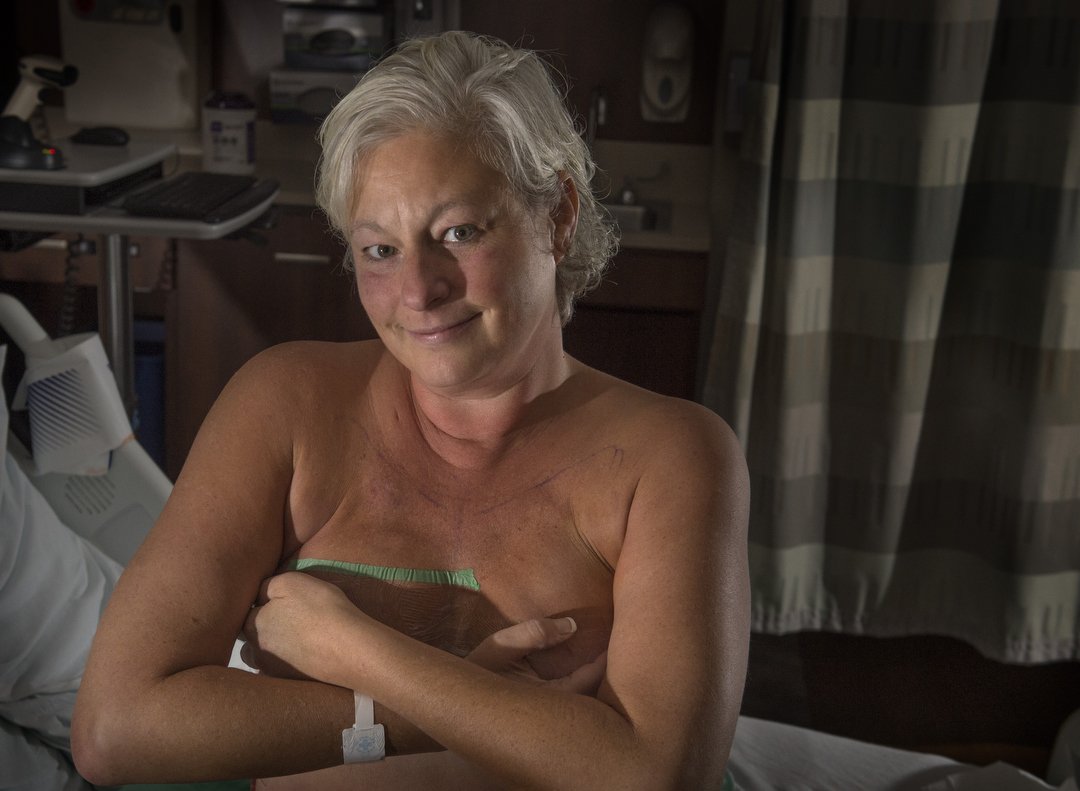





















 /a>
/a>
 /a>
/a>
 /a>
/a>
Iam Grandrapids mi i was 42 i had breast cancer did kemo saw doctor dr.miller had big lump spread kemo kill it had both breast cut off i had br1 gene too now 2years working put implants on frist time it did not working just did every thing too busy now second time iam resting let lord do his work i try God healing hands prayer line total i went thur alot but iam thankfully iam child god and iam live for my kids and they took out ovrs and tubs for br1gene wow my kids got get tesr early but thank god only have3 kids and healthy i wish if was women grandrapids mi talk. Gods not done with every body hope by my birthday party i can have new breasts i be god healthy complete women i tell all women get tested cancer and trust god blessing healing prayer
Best wishes to you, Sue, as you continue your journey. We’re honored to have you as a Health Beat reader and glad Brenda’s story helped give you a little boost today. 🙂
Very inspiring story! So glad that she is a fighter and that being proactive,she gives not only hope to herself but to others who will be faced with some of the same decisions. I know it is difficult to know what one might do when given the diagnosis, but I have to believe that I would make the same choice that this person did. I also have a friend who made that decision and she is living to the fullest.
Thank you for being a Health Beat reader, Diane, and for your awesome comment. We’re so happy this story touched your heart and that your friend is doing so well! Cheers!
Brenny is my best friend since 9th grade. Thank you for taking such good care of her. 🌷
Jennifer,
You picked an amazing best friend early in life. Thank you for being a Health Beat reader. Blue skies and best always!