Dan O’Connell, 67, would be the first to say he’s had a rough go of things lately.
Relationship problems. Trouble keeping a roof over his head. A series of backbreaking jobs as a younger man that have left him with persistent pain.
Over the summer, things only got worse. After a mental health crisis landed him in a hospital in Alma, Michigan, he faced a future without a home, a car or even a driver’s license.
“Yeah, I’ve been through a lot,” O’Connell said. “I’ve had a heck of a life.”
Rather than discharge him to the streets, the mid-Michigan hospital arranged for O’Connell to stay in the men’s shelter at Mel Trotter Ministries, 80 miles away in Grand Rapids, where he could receive help getting back on his feet.
“I said, ‘Yeah, I’ll take a chance,’” he said. “I didn’t know what Mel Trotter was about. It was all new to me.”
Trouble was, when O’Connell arrived at Mel Trotter in July, his health didn’t cooperate.
He had so much back pain that he had to spend most days sitting or lying down.
Soon he developed shortness of breath. At night, he needed extra pillows to prop himself up and ease his breathing.
Finally, he asked the staff at Mel Trotter for help.
“I had to say something,” O’Connell said. “It was getting worse.”
That’s how O’Connell became one of the first patients to visit Community Partners Medical Clinic at Mel Trotter, in the city’s Heartside neighborhood.
Removing barriers
The clinic, which opened its doors in July 2020, operates as a collaboration between Mel Trotter and the area’s major health care and medical education providers: Spectrum Health, Mercy Health, Metro Health–University of Michigan Health, Grand Valley State University and Michigan State University.
Community Partners Medical Clinic helps round out Mel Trotter’s wellness offerings, which also include dental, vision, chiropractic and detox services.
Open four half-days a week, the clinic provides urgent care services for Mel Trotter guests. In the future, care may expand to others experiencing homelessness, regardless of whether they shelter at Mel Trotter.
The goal is to remove barriers to medical care for “those who are lost to the medical community,” said Beth Makowski, DO, a section chief with the Spectrum Health Medical Group hospitalist team, who played a role in establishing the clinic.
She also volunteers at the clinic in partnership with medical students from Michigan State University’s College of Human Medicine, where she teaches internal medicine.
“We try to reengage and redevelop relationships to help folks get the care that they need,” Dr. Makowski said.
“We see patients there in the clinic, but then we also, for some patients, try to establish them with a primary care physician out in the community.”
Timely treatment
With help from shelter staff, O’Connell made an appointment with Jerilynn Spring, FNP, a nurse practitioner who splits her time between the Mel Trotter clinic and SHMG Family & Internal Medicine – North Muskegon.
“When he came in, he clearly looked ill and had told me that he hadn’t been feeling well for two or three weeks,” Spring said.
His symptoms—irregular heartbeat, shortness of breath, decreased oxygen levels and excessive swelling in his feet and legs—added up to a diagnosis of a dangerous arrhythmia, Spring said.
“We don’t have an EKG available (at the clinic), so I was making an assumption that he was in an abnormal heart rhythm that had caused all the symptoms—so we ended up calling an ambulance to get him transported over to the hospital,” she said.
At Spectrum Health Butterworth Hospital, doctors confirmed Spring’s suspicion, diagnosing O’Connell with atrial fibrillation. His rapid heart rate had weakened his heart, causing heart failure and edema.
The medical team administered IV medications to slow his heart rate and diuretics to reduce swelling in his extremities. Once he stabilized, doctors prescribed a drug to sustain a normal rhythm over the long term.
After a week in the hospital, O’Connell returned to the shelter at Mel Trotter to regain strength and begin rebuilding his life.
Spring has continued to monitor his recovery at the clinic.
“I’ve seen him a couple times, and clinically he’s doing great now that they were able to diurese 40 pounds of water off of him,” she said. “He obviously was feeling a lot better.”
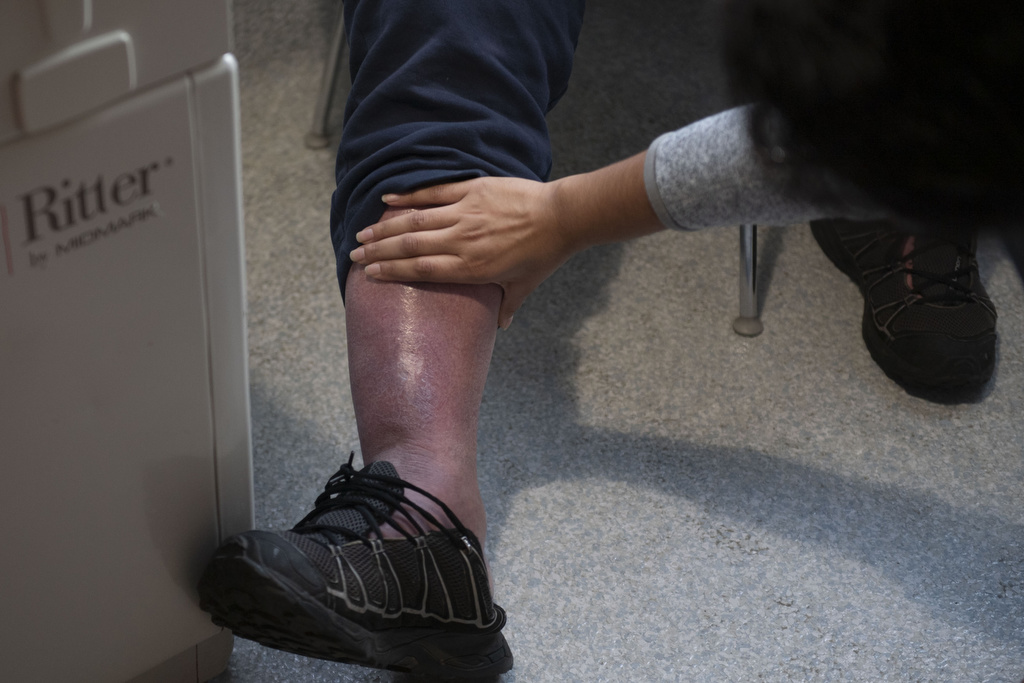
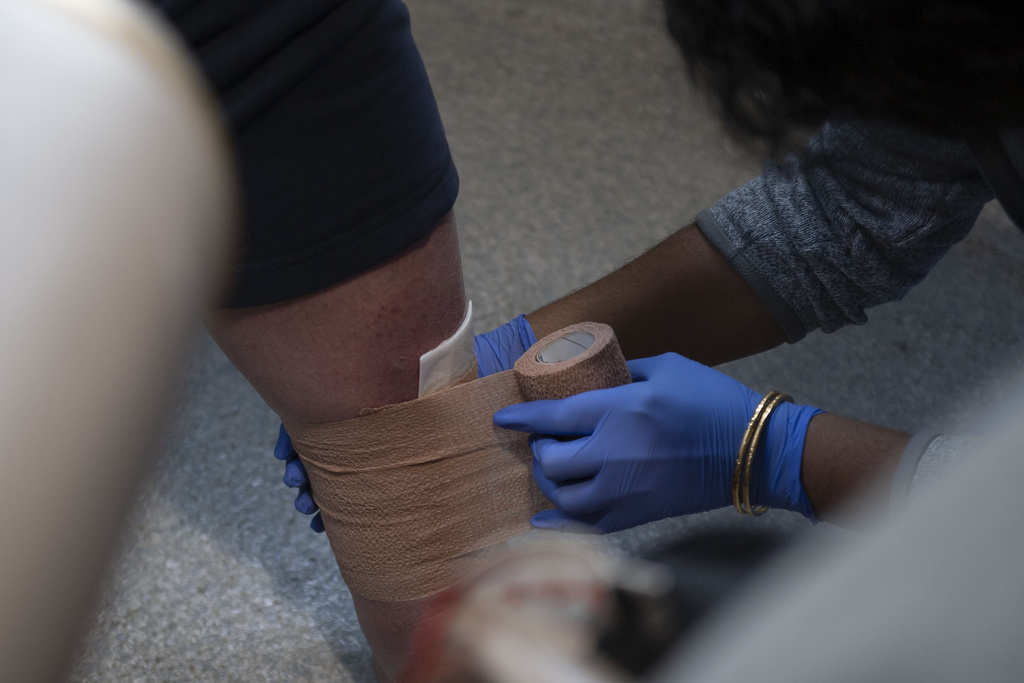
In collaboration with Mel Trotter’s in-house nursing staff, Spring also connected O’Connell with a local wound clinic to help treat a sore on his leg—a result of his skin having been stretched thin from swelling.
O’Connell confirms that he’s on the mend.
“I feel fairly good,” he said. “They’ve helped me out a lot. … I don’t think I could have made it another week without getting some help.”
Persistence and support
Caring for O’Connell and others like him puts Spring right where she wants to be. The clinic lets her pick up where she left off when she relocated from Indiana, where she worked with vulnerable populations in a similar setting.
“I drive an hour to get to Mel Trotter on Mondays, and I do it because I absolutely love it,” she said. “This is why I went into health care.”
For Dr. Makowski, helping to organize the clinic—as well as spearheading a parallel effort in street medicine—has been a way to expand her students’ and colleagues’ learning and outreach in the community.
“Getting the right people involved as a group, we can make a much bigger impact,” she said. “Students, I think, have a really great opportunity for service-learning in this model, too.”
As O’Connell works to pick up the pieces and move forward, he’s adopted a positive attitude.
“I’ve had a lot of problems in my life, but I made it through this far,” he said. “I didn’t want to give up. I wanted to keep going as long as I could.”
This sense of persistence, coupled with support from Mel Trotter and the collaboration clinic, gives him hope for better days ahead.
“It helps,” he said. “If it wouldn’t have been for them, I don’t know what I would have done.”















 /a>
/a>
 /a>
/a>
 /a>
/a>