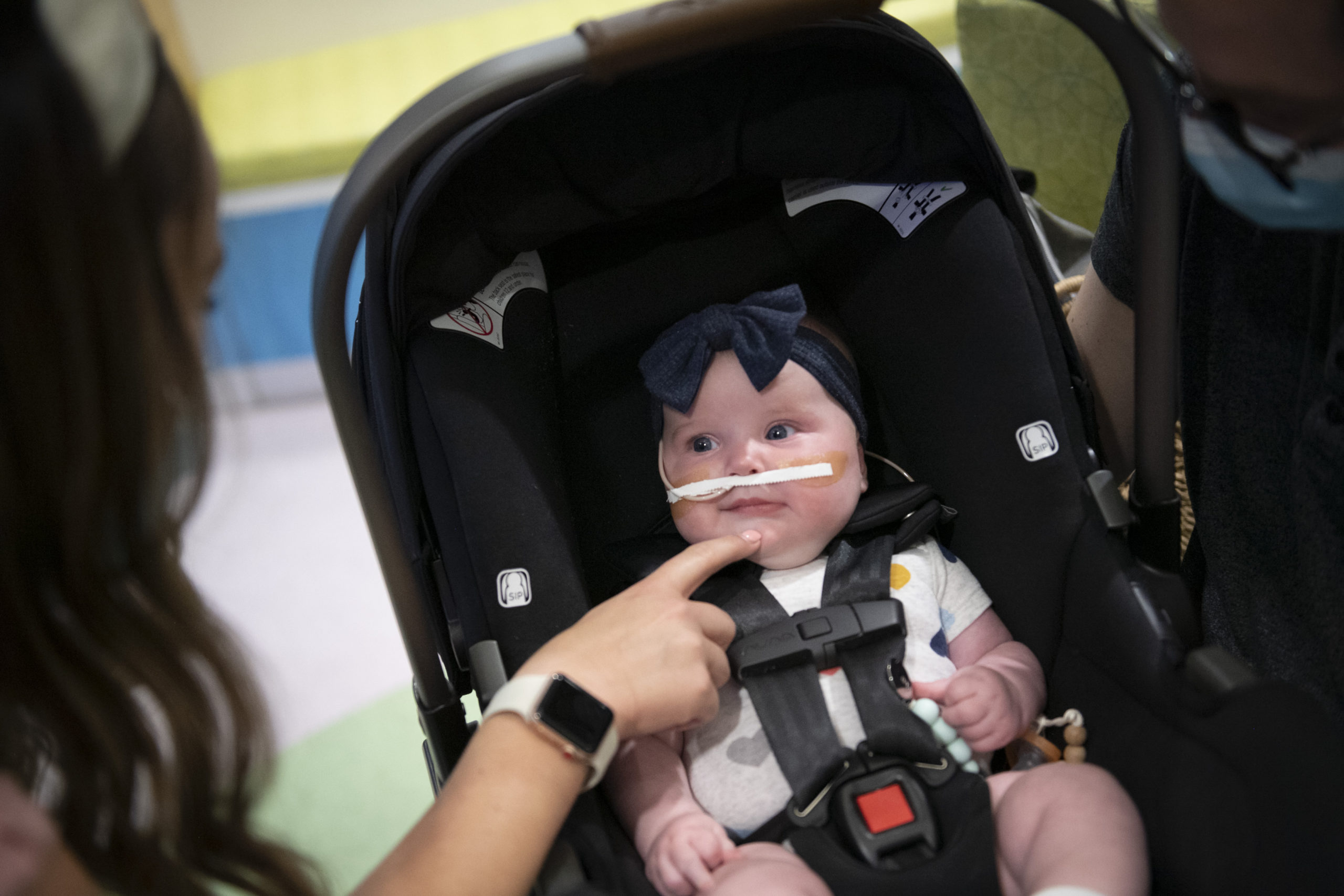
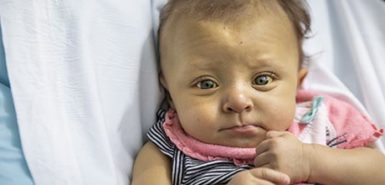
Watch Riley Bosma smile and stretch. Listen to her happy coos.
Look into her sparkling eyes.
You will be charmed. But don’t be fooled.
Beneath this baby’s carefree personality beats the heart of a champion.
Her parents, Allie and Jon Bosma, look forward to the day they can tell Riley how strong she is—of the many challenges she overcame, while in the womb and in her first weeks of life.
“I think we will tell her about how scary it was, but also how much peace we had knowing whatever happened, it was going to be OK,” said Allie, an emergency department nurse in Spectrum Health Helen DeVos Children’s Hospital.
“It really is impressive that she already made it through two open-heart surgeries,” said Jon, a pastor.
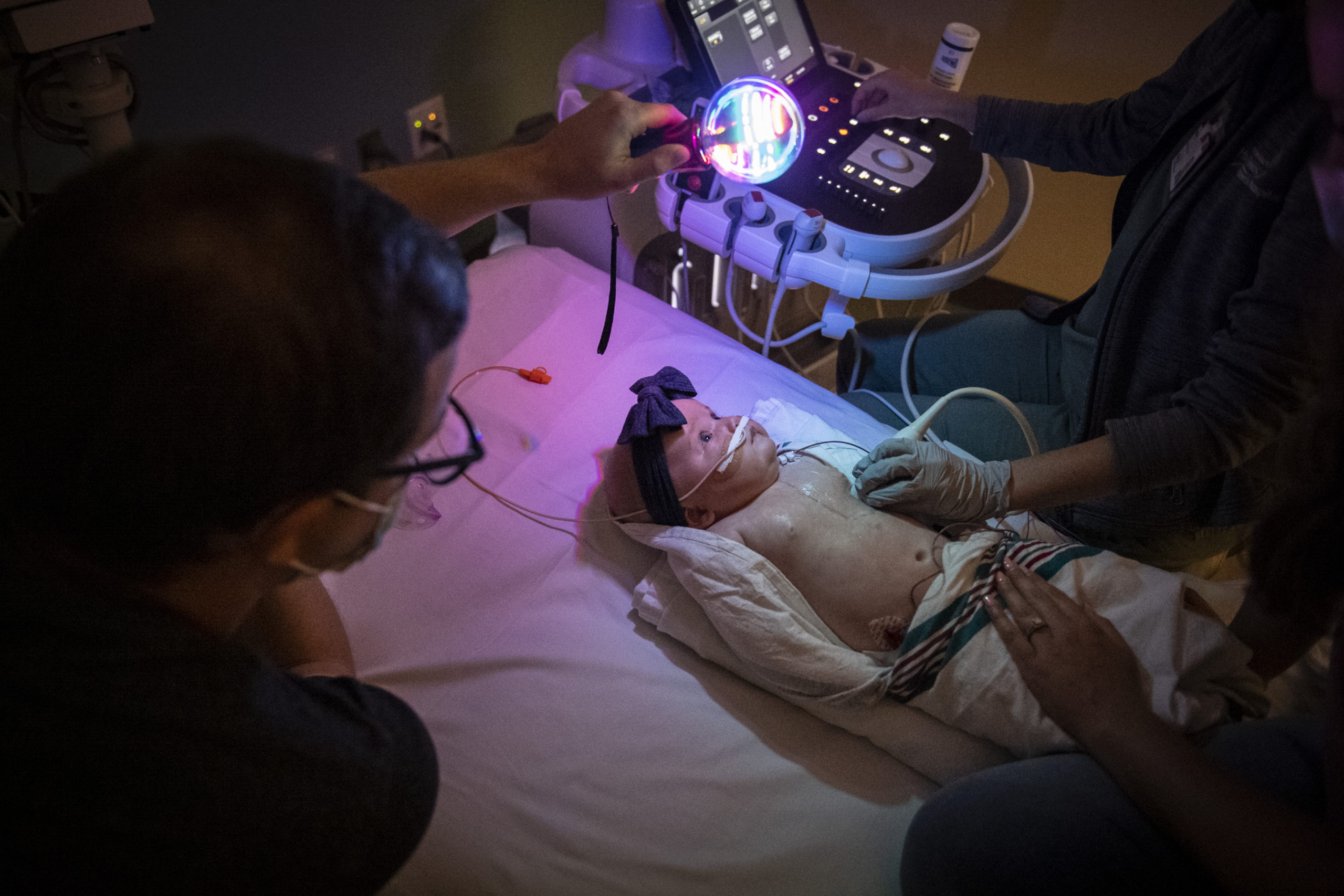
The story of Riley’s amazing heart began when a routine ultrasound revealed Riley’s aorta was enlarged. At 25 weeks gestation, she underwent her first echocardiogram.
“We found out she had critical aortic stenosis,” Allie said. “Her aortic valve was too tiny. It didn’t open properly.”
The aortic valve controls blood flow from the heart to the aorta, which delivers blood throughout the body. Having a valve that is too small or not functioning properly is a bit like “someone putting a thumb over a hose,” Allie said.
The high-pressure blood flow caused the enlargement of the aorta. And in time, the pressure could damage Riley’s heart.
Allie and Jon, eagerly looking forward to the birth of their first child, suddenly had a new set of questions and fears.
“I vividly remember walking down Michigan Street after that, both of us crying and holding hands and knowing this was the start of a long road,” Allie said.
Accompanying them on that road were specialists from the Spectrum Health maternal fetal medicine team and The Karl and Patricia Betz Congenital Heart Center at Helen DeVos Children’s Hospital.
At first, they evaluated Riley for surgery in utero to enlarge the aortic valve. But because her heart function was strong, the doctors advised against the risks of surgery at that time.
The congenital heart and maternal fetal medicine specialists closely monitored Allie and baby—who was not yet named at the point.
A crisis and a decision
At about 32 ½ weeks gestation, Allie and Jon arrived for two appointments back to back.
First, she underwent an echocardiogram of Riley’s heart at the congenital heart center.
The scan showed scarring in Riley’s left ventricle and some fluid accumulation around her heart—both had been detected before. But the heart function and heart rate looked good, said Julie Sommerfield, MD, a pediatric cardiologist.
Allie and Jon took the elevator to the maternal fetal medicine department for an ultrasound.
In the 20 minutes between scans, everything changed.
Riley’s heart rate skyrocketed—from 156 beats per minute to 250.
“It was displayed on the screen above us, and immediately we could tell something was wrong,” Allie said. “We just saw her heart quivering.”
Riley had a condition called supraventricular tachycardia. The extremely fast heart rate likely was related to the aortic valve stenosis and the scarring that it caused in her left ventricle, Dr. Sommerfield said.
Already, it had a dire effect on Riley’s heart function.
“Her heart was beating so fast it couldn’t fill and eject. It was just shaking in her chest,” she said. “Without immediate intervention, the baby would die.”
Doctors admitted Allie to Spectrum Health Butterworth Hospital.
She received medications to lower Riley’s heart rate. But the medications can take time to be effective—they first had to be metabolized by Allie and absorbed through the placenta to Riley.
The medications soon lowered her heart rate, but the high heart rate returned within 24 hours. Allie and Jon discussed their options with their medical team.
If Riley’s heart function continued to deteriorate, they would have to perform an emergency C-section to deliver Riley. But if they could control her heart rate, her doctors preferred to allow Riley more time to develop before birth.
“With every baby born with a heart defect, the outcome is going to be better the longer the baby stays in the womb to allow for growth and development,” said Vivian Romero, MD, a maternal fetal medicine specialist.
Her doctor researched ways to bring the heart rate under control in utero.
In adults, doctors often treat supraventricular tachycardia with a medication called adenosine, which can quickly bring the fast, erratic heartbeat under control.
Dr. Romero investigated whether it had ever been administered directly to an unborn child. She discovered one case report, from Germany in 1995, in which doctors successfully treated the condition by delivering the medication through a needle inserted in the umbilical cord.
“I know that this is not standard of care, but in this specific case, if we can do anything possible to prolong the pregnancy and to allow the baby to grow a little more in utero, why don’t we try this?” asked Dr. Romero.
As a pediatric nurse, Allie had given the medication to children with tachycardia. The standard procedure involves having resuscitation equipment on hand for immediate use if necessary.
“It is a serious medication,” she said. “To think of our baby getting this in utero, when you can’t start life-saving measures without delivery, is kind of terrifying. But I knew this needed to happen for her.”
They sent a prayer request to family, friends and church members. And they agreed to the procedure.
In the operating room, a medical team gathered—including specialists in ultrasound and anesthesia, as well as Dr. Romero, Dr. Sommerfield and Christopher Ratnasamy, MD, a pediatric cardiologist who specializes in electrophysiology.
After Allie had a local anesthetic and pain medicine, Dr. Romero inserted the needle through the umbilical cord. Jon breathed with Allie and helped her stay calm.
The medication went in. But the baby’s heart rate did not slow down.
Dr. Romero delivered a second dose. And Allie and Jon heard the longed-for good news: Riley’s heart rate had converted to a normal rhythm. Relief flooded the room.
“That was wonderful,” Dr. Romero said. “Everyone was really happy in the OR.”
A hearty first cry
The treatment provided the time needed for the oral medications to work.
Allie and Jon went home, where they monitored Riley’s heart rate every night.
One evening, she detected a return of the fast heart rate. She went back to the hospital and, a few days later, her doctors induced labor.
On that spring morning, a team from the neonatal intensive care unit team waited in the operating room as Allie gave birth, at 36 weeks gestation.
Riley arrived, weighing 5 pounds and 14 ounces–a half-pound more than she did when she received the heart medication in utero.
“We had gotten three more weeks of fetal growth,” Dr. Sommerfield said.
Allie’s heart lifted when she heard Riley give her first, hearty cry. And she melted when she saw her beautiful auburn-haired baby girl.
“It was just amazing and surreal,” Allie said. “They put her right on my chest. We got to enjoy a little time as a family of three, to look at her and take everything in.”
“It was just beautiful, honestly,” Dr. Romero said. “This has to be one of the most gratifying stories that I have ever shared.”
Day 2: Open-heart surgery
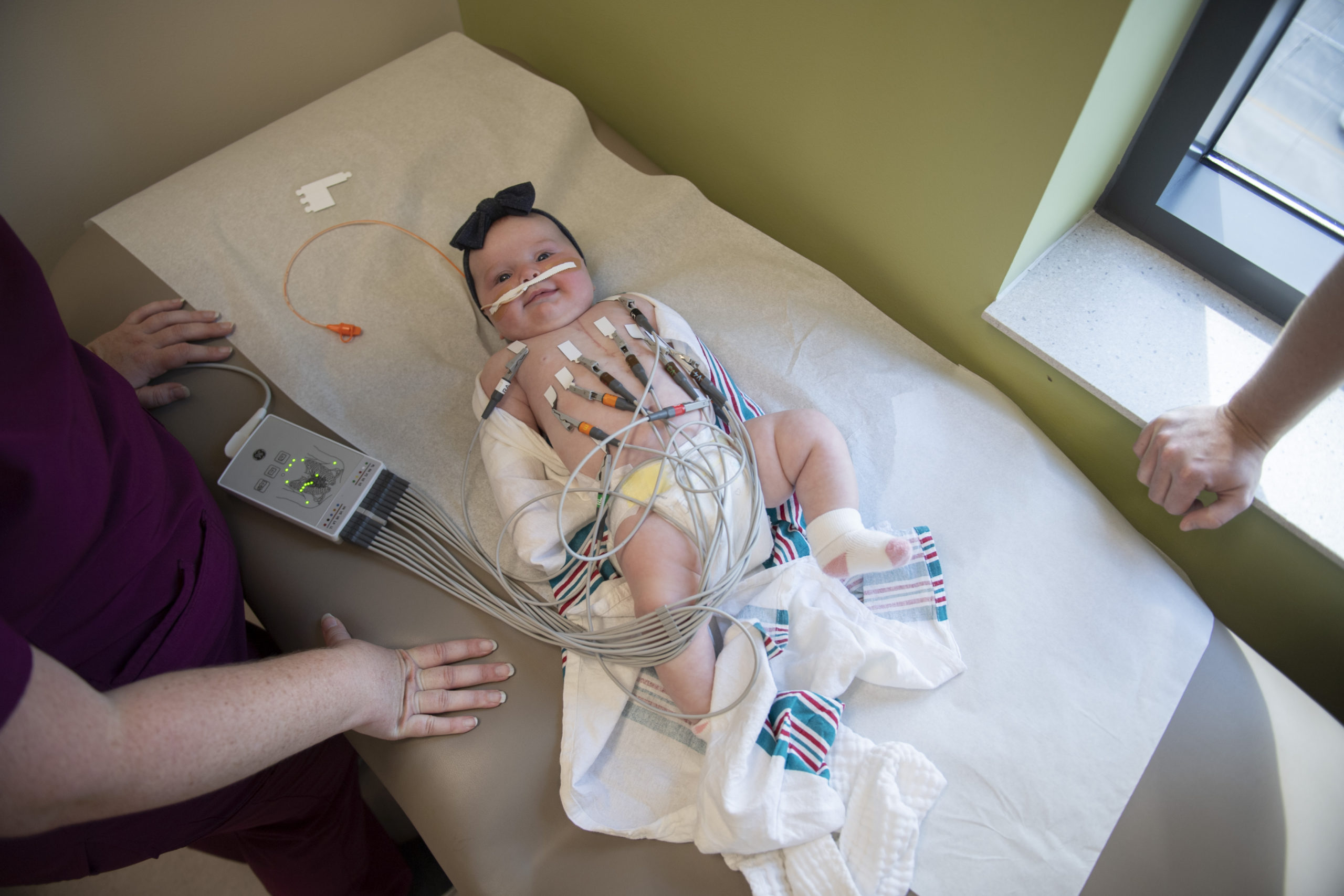
Throughout the delivery, Riley maintained a steady heart rate. But in her first day of life, the tachycardia returned 12 times.
“Every time, Riley went from a healthy pink baby to kind of gray and floppy,” Dr. Sommerfield said. “She may have been one of the sickest kids I have ever seen.”
In the cardiac intensive care unit, a nurse remained by Riley’s side, providing the medication that kept her alive.
On Riley’s second day, the congenital heart team attempted a heart catheterization procedure to open her aortic valve. When that was not possible, they brought her immediately to the operating room.
Marcus Haw, MD, a congenital heart surgeon and co-director of the congenital heart center, performed open heart surgery on her valve.
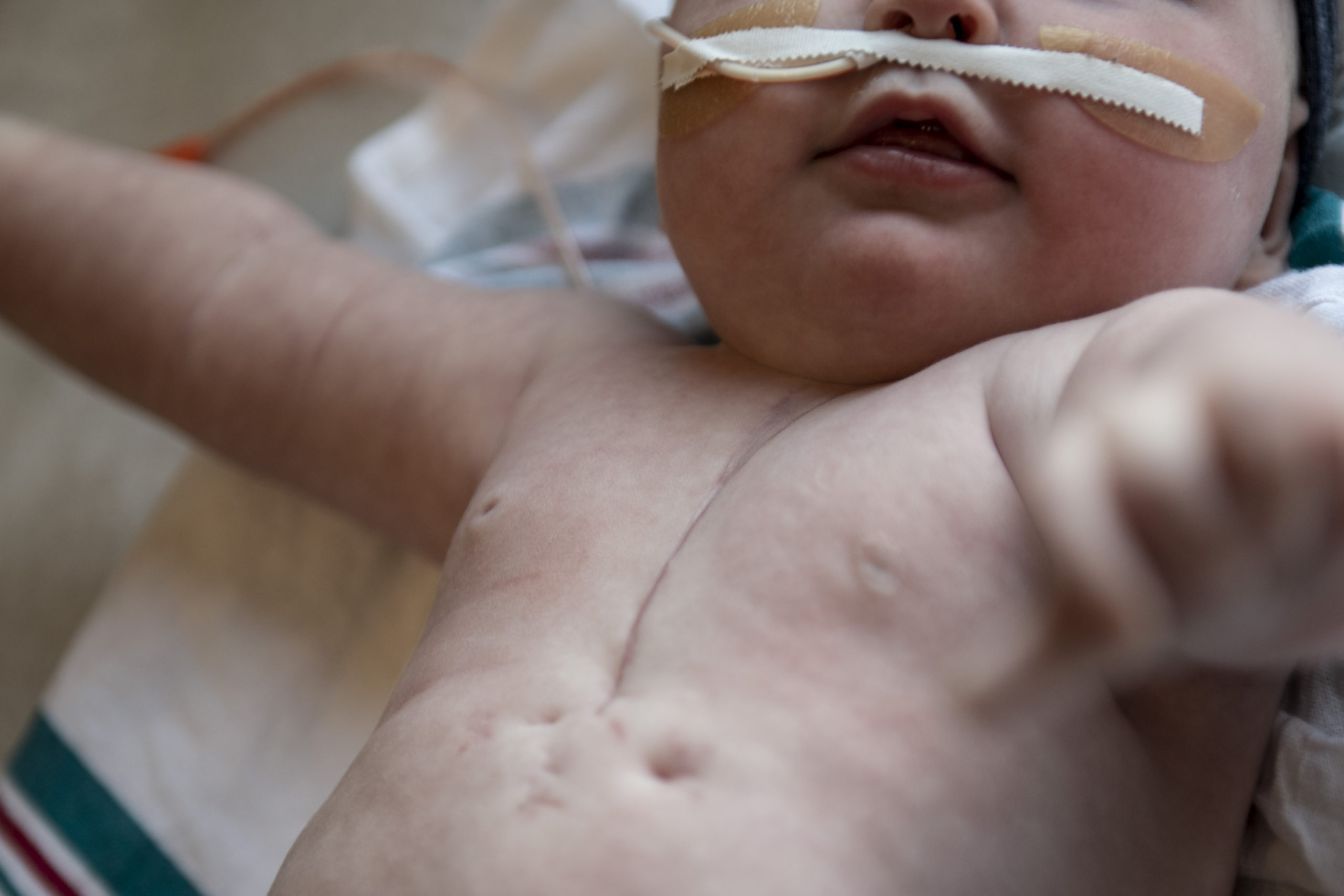
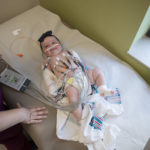
Riley returned to her room in the cardiac intensive care unit surrounded by tubes, lines and wires. Allie recognized them—a PICC line, arterial line, an umbilical arterial line, an umbilical venous line, an intravenous line, a chest tube and an endotracheal tube. The congenital heart team also connected her to monitors to track the function of her heart, brain and kidneys.
“It was kind of a scary sight,” Allie said. “This was her second day of life.”
The operation improved the function of the valve. But Dr. Haw told the Bosmas a future surgery would be needed.
“Dr. Haw described her valve like wet tissue paper,” Jon said. “He couldn’t do all he hoped to do, but it was enough to buy us some time.”
Riley went home two weeks later.
At 3 months old, she underwent a second open-heart surgery.
“The tissue was so much stronger and he could do more that he wanted to do,” Allie said. “We were really grateful for that.”
Riley likely will need surgery in the future, Dr. Sommerfield said. And she will remain under the close care of her congenital heart team.
But her many fans—from her medical team to family and friends—marvel at how far she has come.
Living in the moment
In her office, Dr. Sommerfield keeps a picture of Riley, given to her by the Bosmas. It shows Riley, lying beside a doll that has a matching scar on its chest, with her arm raised in a fist.
“She looks like a warrior,” Dr. Sommerfield said. “It is inspiring.
“To see a child doing so well, despite all the odds, makes it worthwhile for us to do what we do.”
Allie and Jon look back on the last few months with gratitude—for their faith and for the prayers and good wishes from a wide group of supporters. They felt a sense of peace, which helped them have good discussions with their medical team about Riley’s care.
And as they delight in seeing their daughter grow and her personality blossom, they realize they have grown through this experience, too.
“We have learned not to make plans too far into the future or to hold to any plans too tightly, because things can change,” Allie said.
“This has challenged us to live in the moment. It helps us to enjoy these moments at home together and just to love on her when we can.”































 /a>
/a>
 /a>
/a>
 /a>
/a>
Our whole family is so grateful for the amazing care Riley has and continues to receive! She wouldn’t be here without you.
Little Riley, or “Miss Feisty” as she has come to be known by my friends, inherited her strength and passion for life from her parents. But she would not be here without the talent and devotion of her medical team. We are so grateful.
What a beautiful story of God’s faithfulness! We prayed generally but these details give a small window into what you’ve been through. Thank you for sharing your story…we will keep praying!
God is so good! Little Riley is a beautiful reminder of His love. I will pray for her continued health.
God has placed in Riley’s life such amazing people. God gifted these special placement of people in specific gifted areas that now enable her to continue God’s plan he set for her life.
I just read your story & it is AMAZING ❤️ Unbelievable what can be done in the womb & out on such a small baby ! I will pray for continued GOOD HEALTH !
As the mom to another heart warrior being taken care of by the team at DeVos, I love hearing these stories! These babies are so remarkable and I am so thankful for the team of people who have dedicated their careers to taking care of these miracles.
What a wonderful story, thanks for sharing. I was so happy to see you had Dr. Romero… She is such an amazing doctor. She helped us with our twin delivery and I couldn’t have imagined a more thoughtful, supportive, educated, and kind doctor. It does not surprise me that she researched a way to help your baby, she would go to the end of the earth to help someone.
Prayers for your baby in the months and years to come.