As Marilyn Ondersma cleaned up her kitchen one evening last November, she started to feel sick.
She told her husband she wanted to lie down for a bit.
“As soon as I did,” she said, “I realized I could barely breathe.”
Rather than wait for an ambulance, her husband, called their close friends and neighbors. One is a physician assistant and the other, a professor of sports medicine. They got Marilyn in the car and sped straight to a hospital in Holland, Michigan.
Ondersma, 73, remembers very little about that night, except for a doctor leaning over her, explaining she’d had a heart attack.
She experienced an acute infarction and a torn valve. Cardiologists at Holland Hospital stabilized her using an Impella, a small heart pump.
Immediately afterward, Ondersma transferred to Spectrum Health Butterworth Hospital.
She remembers constantly being asked if she had COVID-19.
“I’m normally a patient person, but it was so irritating,” she said. “And I just kept repeating, ‘No, no, I don’t have COVID.'”
Except, she did. Testing quickly confirmed it.
Imaging also revealed the urgent need for heart surgery.
The type of tear she experienced has a high mortality rate, says Spectrum Health cardiothoracic surgeon Tomasz Timek, MD, He praised the Holland Hospital team’s use of the Impella. “That allowed her to get here for surgery. They had a great part in saving her life. This was coordinated team care for a very complex patient.”
On Nov. 4, he performed a mitral valve replacement and bypass graft surgery on two coronary arteries.
The procedures saved her life. But it didn’t slow the effects of COVID-19. Her symptoms intensified.
Doctors put her on a ventilator to help her breathe. They also induced a coma.
In addition to the COVID care team, the cardiovascular health team continually monitored her lungs, kidneys and heart function.
By Nov. 19, Ondersma’s family opted for a tracheostomy, a procedure to open her windpipe.
After nearly four weeks, she began to wake up from the long coma.
Ondersma remembers almost nothing about that period, except for occasional flashes of caregivers tending to her in full protective gear.
“I remember seeing goggles and sometimes thinking, ‘Wait. Are these aliens?’” she said. “And at one point, I did see a brilliant white light. Something told me to be calm and relax.”
Meaningful care
Once she regained consciousness, Ondersma found it increasingly difficult to relax.
She had become so weak she couldn’t use the buttons to raise and lower her bed. She felt cooped up.
“I had nervous legs, so they jiggled all the time,” she said. “People would ask if I wanted something, but I couldn’t answer.
“The only thing that calmed me down was repeating the words, in my head, to songs I knew as a little girl—simple songs, like ‘Jesus Loves Me.'”
Long weeks in intensive care and the subsequent rehab period in the COVID-19 care unit felt endless.
After 15 days, however, she finally got off the ventilator.
Dale, her husband, sat by her side each day, holding her hand.
“I kept saying, ‘I can’t do this,'” she said. “He kept saying, ‘Yes, you can.'”
Only later did she learn she had about a 40% chance to live.
The nursing team called her “Miracle Marilyn.”
“We see many patients through often the most difficult days of their lives,” said Rachel VanStrien, a physician assistant in the cardiothoracic critical care unit, who worked with Ondersma.
“And to see her on the other side of these terrible illnesses is a welcome reminder to our ICU team that the work we do is meaningful.”
Health teams knew very little at that time about outcomes with COVID and open-heart surgery, VanStrien said.
“But Marilyn’s resilience and perseverance is no doubt what allowed her to survive,” she said.
By Jan. 11, doctors had removed her tracheostomy tube. She recovered enough to move to the Blodgett Inpatient Rehab Unit, without the assistance of an oxygen pump.
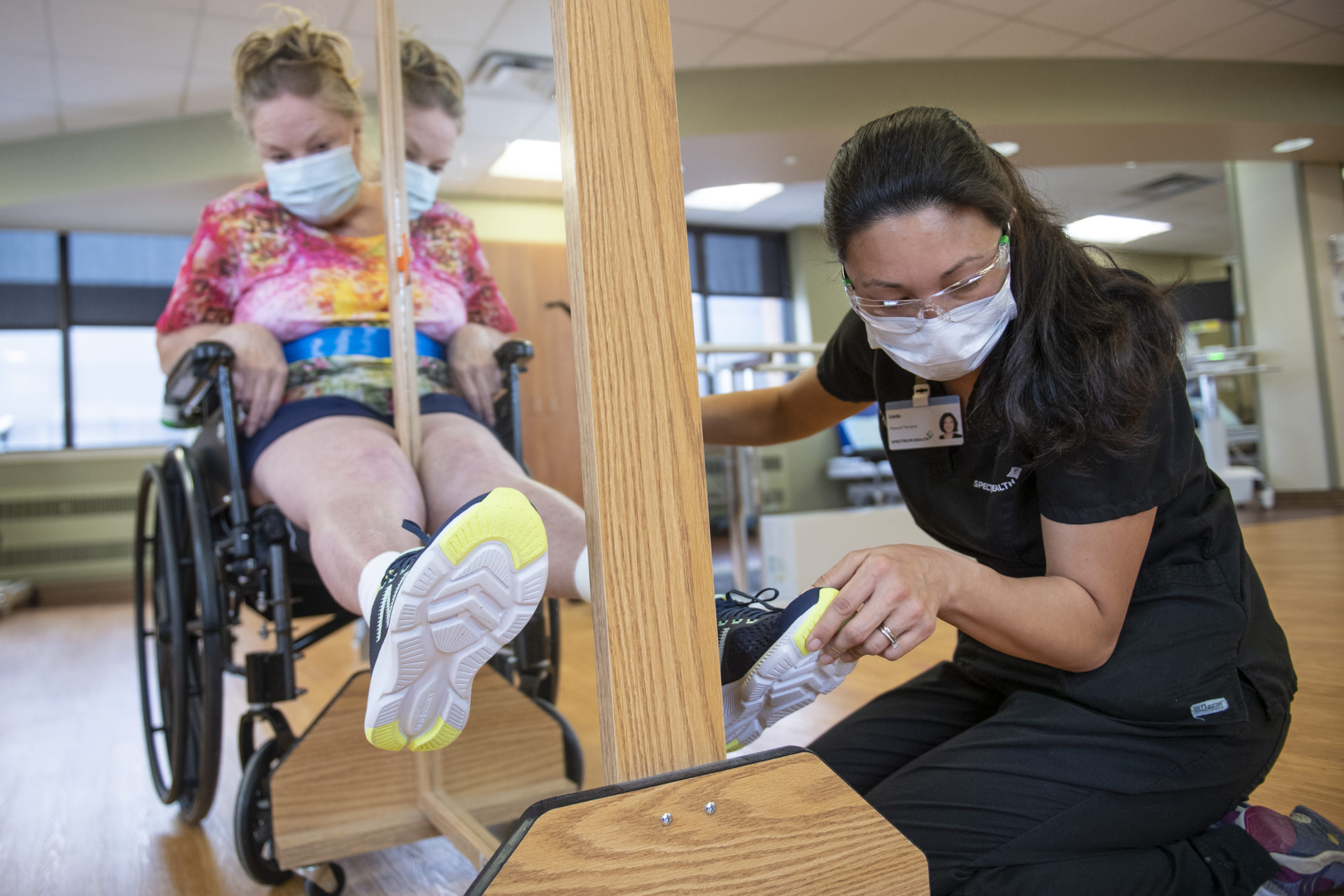
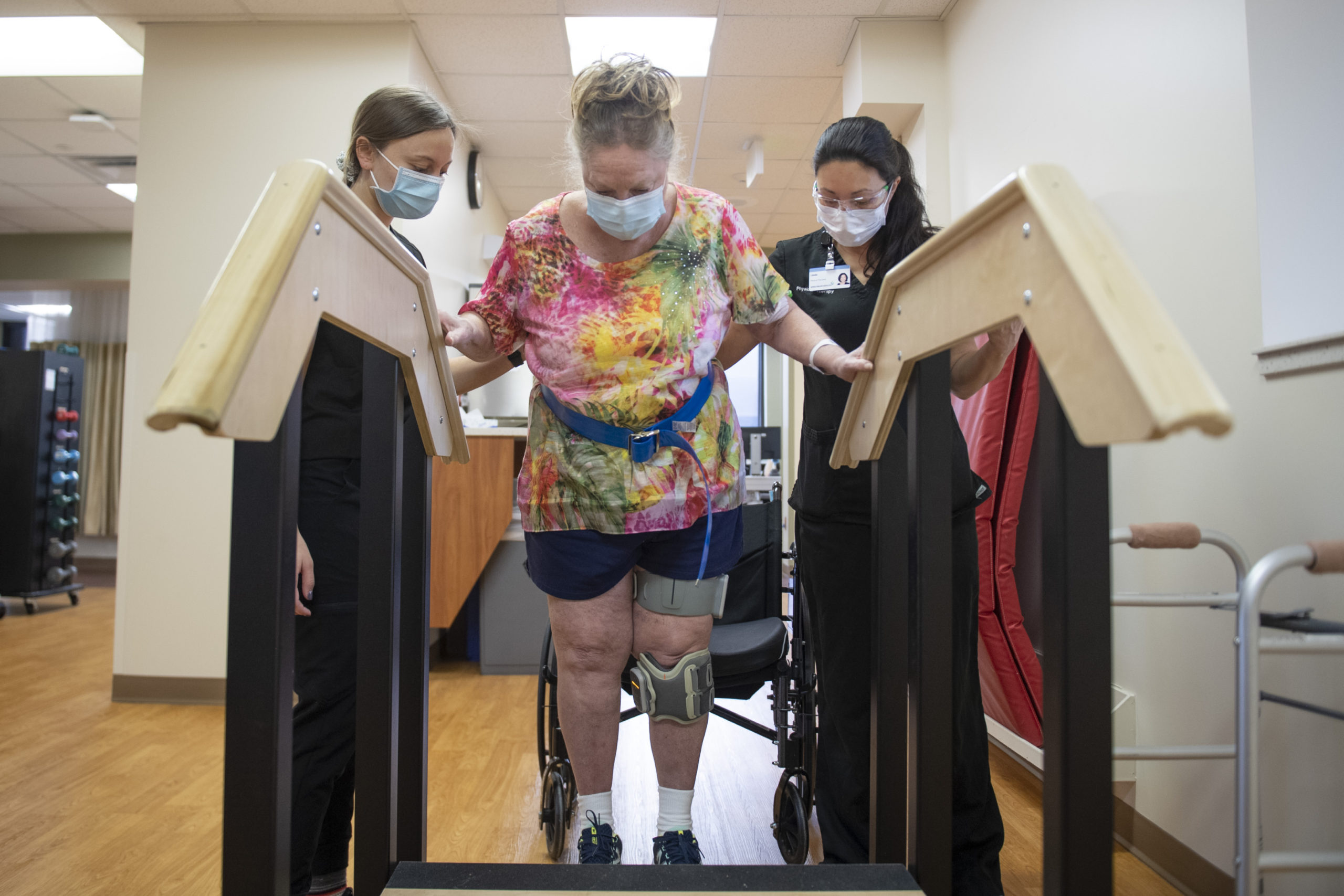
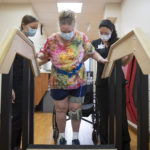
“Rehab is kind of like boot camp,” Ondersma said. “After being in bed for three months, I needed to do a lot of work to get back to myself.”
That regimen included working out on special machines to help her walk, electrical stimulation, as well as occupational and speech therapy.
“We worked on things like washing my hair and simple housework skills,” she said.
Through it all, she relied on an outpouring of support from her family, including Dale, her four kids and 12 grandchildren.
Her son, Gareth, took on the role of personal advocate and decision-maker. He kept up with the details of Ondersma’s therapies and medications, keeping other family members posted.
Kayleigh, 12, her granddaughter, called her every day, often singing “Lavender’s Blue,” sometimes sharing tears over this favorite song from Cinderella.
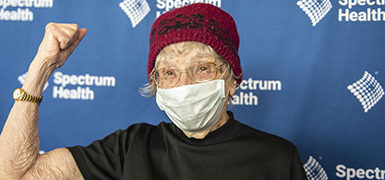
On Valentine’s Day, Ondersma’s husband showed up with flowers, a card and the best gift of all: The all-clear to return to their home in West Olive, Michigan.
Headed toward recovery
When Ondersma returned home, she looked out across Pigeon Lake, with its wintertime ducks and geese. She felt overcome with gratitude—as well as plenty of fear about being out of the hospital.
“After all that time of being so sick, it was hard to believe I’d be able to handle my care,” she said.
She’s managing now, continuing with therapy to regain mobility. She requires a walker and sometimes the use of a cane.
She spends 45 minutes a day on exercises. Ongoing fatigue, common in COVID patients, is still an issue.
Her goal is to walk unassisted again. She’s eager to get back in her garden, too, tending to a crop of zucchini, tomatoes and cauliflower she hopes to have this year.
She said she is full of gratitude for Dr. Timek, the ICU team and the encouraging physical therapists.
“It is tough and there are still days when I feel like giving up,” she said. “But I feel like if the Lord is going to get me through a heart attack and COVID, he’ll restore my leg, too.
“It’s just not going to happen on my timetable.”










 /a>
/a>
 /a>
/a>
 /a>
/a>