Lonnie Martin stepped off a cruise ship last October, after a seven-day voyage to the Eastern Caribbean.
She returned to her Grand Rapids, Michigan, home with much more than memories and souvenirs.
The feeling of being on the high seas never left her. She felt constantly seasick, on land.
“I’ve been on eight or nine cruises,” said Martin, 48. “The only difference I noticed with this cruise was I was a little bit tired. I didn’t feel weird or anything until we debarked. Within hours, I started feeling strange. It was almost like a pulling sensation. It’s hard to explain. My body felt like I was being pulled.”
Martin had no idea what could be wrong. Perhaps, she thought, celebrating her dad’s 70th birthday during the voyage with other family members had tired her.
“I got off the boat on a Saturday morning and got home late that night,” Martin said. “By the next day, I couldn’t stand up properly. I was leaning to the left and I felt very disoriented.”
She trusted the sensation would pass.
On Monday, the symptoms continued, so she visited her doctor, who prescribed medication to treat vertigo. It didn’t help.
By Wednesday, she landed in the Spectrum Health Butterworth Hospital emergency department.
A stroke?
“I had gotten to the point where I couldn’t walk without hanging onto something. I would rock back and forth, side to side, my body would just move on its own. I was really sensitive to light and I had to wear sunglasses all the time.”
Doctors initially feared Martin had suffered a stroke and ordered an MRI and CT scan.
“They were asking me questions in the hospital,” she said. “’Who is the president? What day is it? What year is it?’ I had no recollection. I thought the president was Obama. I don’t remember what day and year I said. I was just so disoriented.”
The scans came back normal. Next, a neurologist assessed Martin.
“They asked me to stand up and I couldn’t stand up,” she said. “I couldn’t walk a straight line. They said, ‘Stand up and close your eyes.’ I closed my eyes and I immediately fell over. I had no balance. They caught me.”
Knowing Martin’s recent history of cruise travel, the neurologist diagnosed Martin with Mal de Debarquement syndrome.
“I was like, ‘What on earth is that?’” she said. “From what I understand, it’s a neurological condition that when you’re on a boat, your brain adapts to that motion of going back and forth. When I got off the ship, my brain never switched back. My brain still thinks it’s on a cruise ship.”
While that may sound like a happy place, a brain believing it’s still on a cruise ship can be a shipwreck for the body.
“It was hard to hear, but there’s no cure,” Martin said. “There’s nothing they can do to help.”
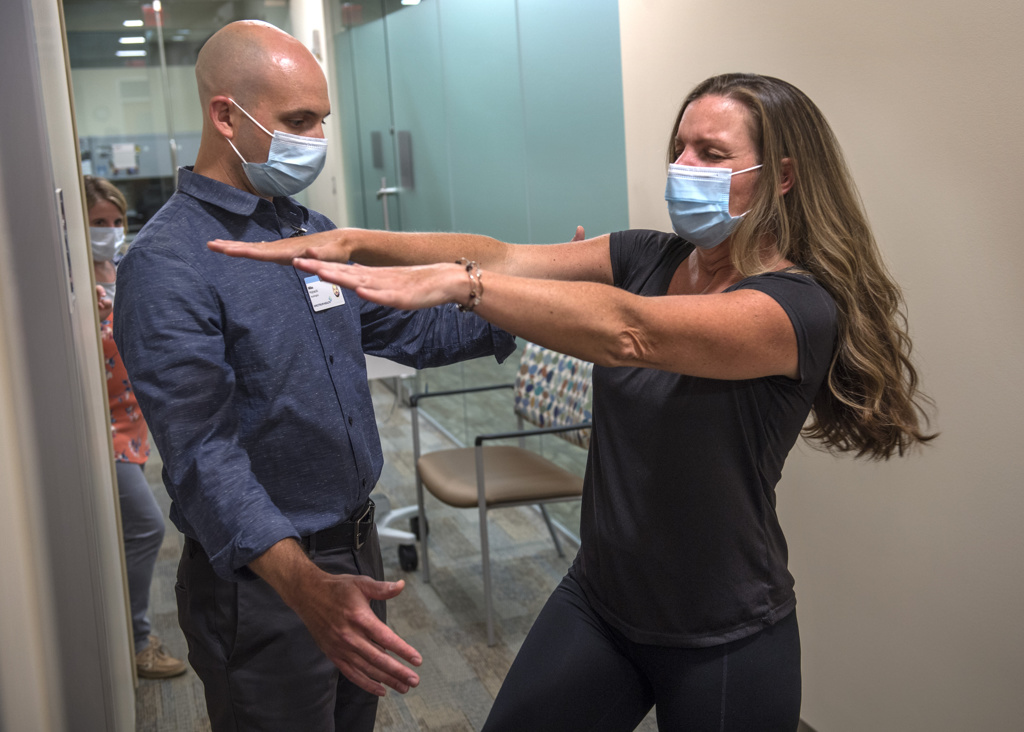
She tried medication and attended physical therapy sessions at the Spectrum Health Integrated Care Campus at East Beltline.
“The PT has been helpful, but it took a really long time,” she said. “They gave me a lot of good pointers.”
In January, Martin went to the Spectrum Health Balance Center, also at the East Beltline campus.
Readapting to land life
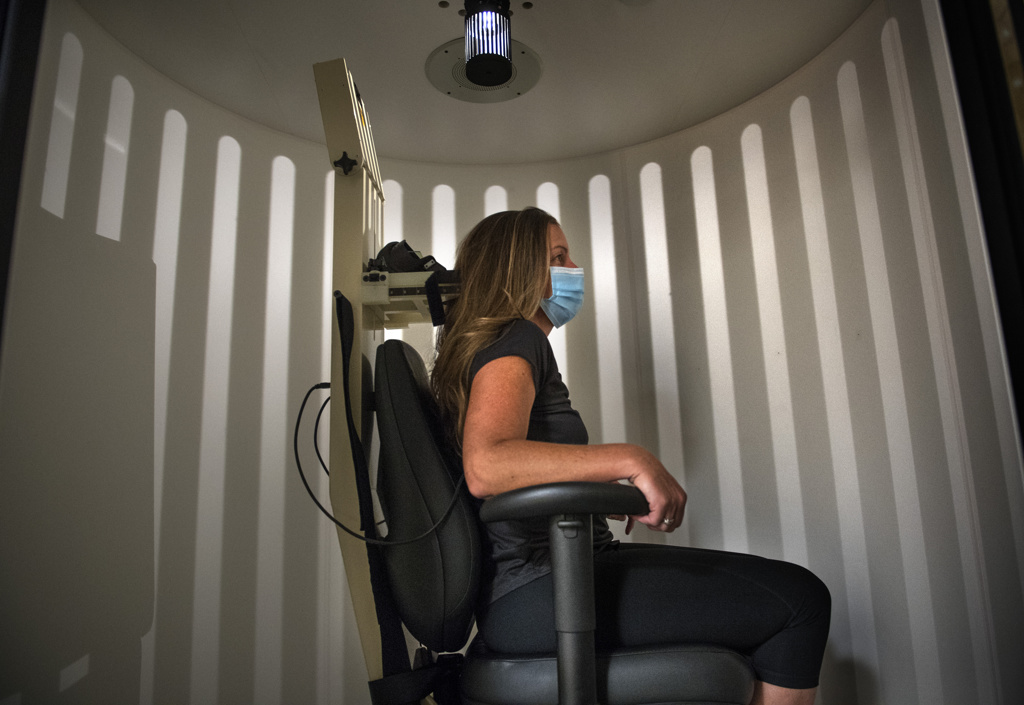
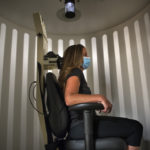
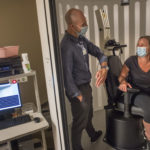
She underwent roll readaptation treatment, also known as the Dai technique, with Michael Hojnacki, AuD, a specialist in audiology with the Balance Center.
“They put on a projector that projects lines and you sit in a chair that rotates,” Martin said. “You have to try to follow the lines. It’s supposed to make you feel more balanced. At first, it made me throw up, but it helped me tremendously.”
Dr. Hojnacki said about 73% of cruisers still feel like they’re on the ocean for about 24 hours after leaving the ship. It’s rare for symptoms to continue long-term like Martin’s have. It’s believed about 150,000 people in the United States suffer from Mal de Debarquement.
“I have seen other patients with Mal de Debarquement, but I have never used the roll readaptation treatment in the past,” Dr. Hojnacki said. “The sole recommendation for patients with this condition in the past was to let time run its course as it’s uncommon for symptoms to persist greater than 12 months.”
Although Martin improved after treatments, she had traditions to follow—the annual cruise she takes for her Feb. 23 birthday. She journeyed to the Bahamas on a seven-day adventure with her boyfriend, Stew, perhaps secretly hoping that a cruise would reverse her symptoms forever.
“On the cruise ship, I felt totally normal—more normal than I’ve felt since all this started,” Martin said. But as soon as I got off the boat, it came back with a vengeance. Worse than ever. I went back to the Balance Center as soon as I got back. They did a really intense therapy, five days in a row. I don’t think it’s a good idea to go on any more cruises, unfortunately. I will definitely miss it.”
By mid-March, with the help of Balance Center therapy, Martin stood on her own two feet.
“It was amazing what that did for me and it was a huge difference from where I began,” she said. “I still lean to the left, but I’m so much better than I was. I think I’m just learning to live my life the way I am now. I still wobble or sway when I’m standing still. If I’m in motion, I’m OK. If I’m standing still, that’s when it hits me.”
Martin has given up cruise ship berths, but even her bed at home can leave her feeling seasick.
“I feel like I might fall out of bed,” she said.
While she won’t be boarding a cruise ship any time soon, she did pilot a small boat in early June to help Stew set buoys at Scalley Lake Campground in Belding. He owns it; she’s worked there for nine years.
“I wasn’t thinking anything of it when I was driving the boat and Stew was putting lines out and dropping buoys in the swim area. We were out there about 20 minutes. As soon as we got back to the dock, I felt it. They say walking helps, so I try to walk a lot.”
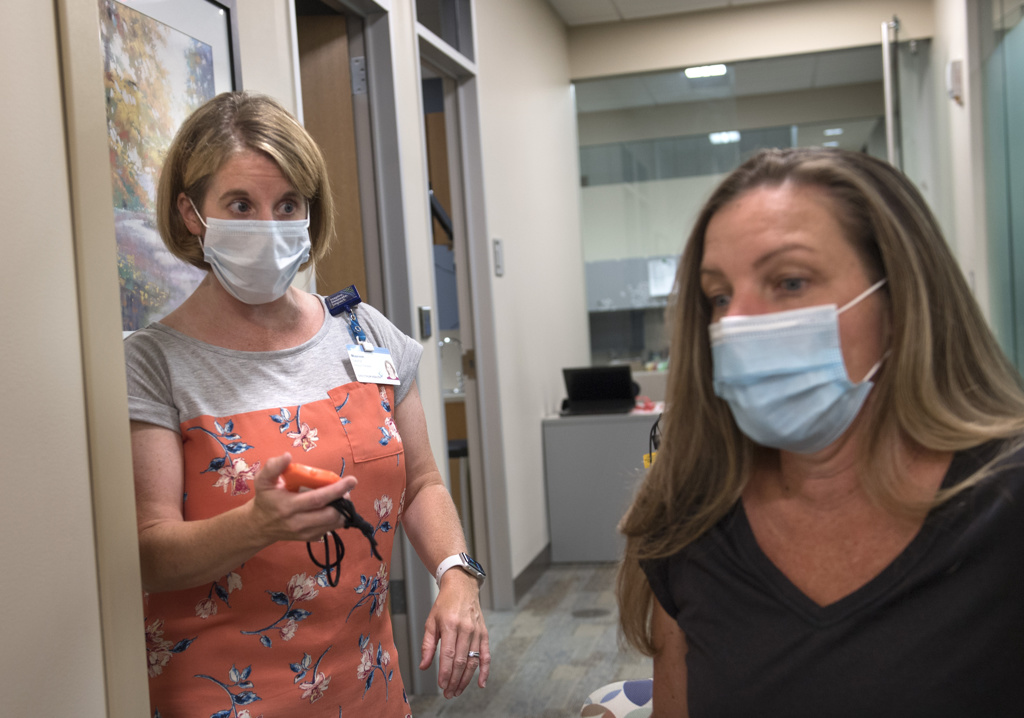
Maureen Gaynor, Martin’s Balance Center physical therapist, said Mal de Debarquement is difficult to treat.
“Historically, it has been a challenging condition for therapists to treat as there wasn’t great research on treatment options or the best treatment approaches,” Gaynor said. “With the advent of the new Dai technique, we now have an excellent treatment option to offer patients at the Balance Center. I have only seen two other patients with Mal de Debarquement and their progress was slow and minimal. Unfortunately, Lonnie was attending therapy when our clinic had to close due to the COVID-19 outbreak and restrictions.”
Instead of seeing her in person, Gaynor checked in by phone during the clinic’s closure.
“She reported feeling markedly better and felt comfortable being done with therapy because her symptoms had dramatically reduced,” Gaynor said.

















 /a>
/a>
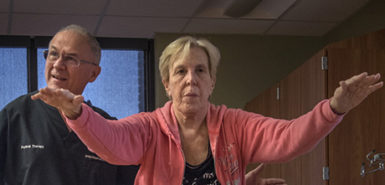 /a>
/a>
 /a>
/a>
Very interested.
What an interesting story and very well written. I heard of this disease and read about it in my therapy books but reading how someone who is experiencing it was very enlightening. Thank you for sharing Ms. Martin and another great story by Marie Havenga.
Thank you also, Health Beat/Spectrum Health.
I have been on five cruises over many,many years .and have never had this situation, nor.have I ever heard of this happening.to.anyone. Pretty scarey! I hope this gal improves.
I suffered from this about 20 years ago. It happened after 3 different cruises. Lasting at least 6 months each time. The doctors could not figure it out. Strange but true the last time it happened I was having a crown put on at the dentist. The process of the dentist tapping the crown on made it go away. I felt it immediately. I believe while on a cruise the the crystals in my ears broke loose. The process of the tapping gently coax the crystals back to were they were suppose to be. The rocking, swaying, and constant feeling of being on that ship was gone.
I am so glad you found doctors that helped you.
For me it was a struggle .
Mall de Debarquement has nothing to do with your inner ear or the crystals coming out of place. It’s numerological.
*Neurological
I’ve had it for almost 3 yrs. i went to Mt Sinai Hosp in NYC. It was sort of helpful. They have a whole dept for MdDS.
I was diagnosed with Mal de Debarquement Syndrome by an ENT doctor after a 7-day Cruise in May 2018. I had an MRI, hearing test, and PT, which did nothing to help. I was at my wits end and started on an anti-depressant 7 months into having it. I am now 28 months in and finally started feeling back to my normal self just after the two year mark. I would say I’m nearly in remission. I will NEVER step foot on any type of boat again, unfortunately.
I was diagnosed with Mal de Debarquement Syndrome after a cruise in 2008. It feels like the ‘gyroscope’ in my head is ‘off’. I still feel like I’m on a boat 24/7. I never had migraine headaches until the MdDs. Along with the balance/equilibrium problem, there is the component of “overstimulation to the brain”. A concert is too loud, movies can be too much motion for the brain to handle. Walking through a store can also be too much of an overload for your brain … it tries to take in so much at once. My brain tends to work slower, and usually I feel foggy. I don’t comprehend information as well as I have in the past. I’ve tried many different medications, vestibular therapy (3 different approaches), acupuncture twice (2 different doctors),hyperbaric oxygen treatments, etc. My depth perception and dexterity have been continually changing. I could no longer preform my dental hygiene duties, I had to retire early February this year. I pushed myself for so many years to continue to work, I hit a wall 🙁 An upper cervical chiropractor, and physical therapy for my head and neck have helped with the migraines. I am still grateful that this is not lethal !!! It has altered how I live, I won’t let it get the best of me !! From what I’ve read over the years, different treatments lessen the symptoms for only some of us . I will continue to try different ‘ treatments ‘ for relief from my symptoms.
I am very blessed to have a helpful and understanding husband ❤️
I was diagnosed in 2000. Luckily a very mild case. I come from a sailing family and spent the better part of every weekend on the water. We had taken a ferry, about a two-hour trip. But after this trip I couldn’t shake that on a boat feeling. A couple days later it felt like I was walking on a trampoline. Then while stirring a pot of jam I had the sensation of falling and . . .fell to the floor. Headed to the doctor and diagnosed a couple of weeks later. Twenty years later I cannot close my eyes and expect to stay upright. So, when washing my hair in the shower I have some part of my arm touching the shower wall. After riding in cars I’ll experience mild symptoms again.