
An open appointment and a spur-of-the-moment decision likely saved Lisa Soueidan’s life.
She’ll always remember the date: July 7, 2015.
“That was the day we were training to use our new 3-D mammography technology,” said Soueidan, 43, a radiology technologist at Spectrum Health Gerber Memorial in Fremont. “We asked staff to schedule their mammograms this day so we could learn how to use the 3-D feature with a trainer from Hologic, the machine’s manufacturer.
“Everything was ready to go, and then we had openings for a couple more people,” she said. “So I thought, ‘Why not?’ and I signed up.”
Earlier that year, Soueidan had started as a radiology technologist at Gerber Memorial, a 25-bed critical access hospital in Newaygo County, surrounded by farms, apple orchards, rolling hills, about 200 lakes and more than 350 miles of rivers and streams.
Gerber Baby Products, the baby food maker—unaffiliated with the hospital—is across the street. A hitching post stands outside the hospital’s emergency department entrance, installed for the nearby Amish community.
Every day, Soueidan performs mammograms on patients. She sees the worry in their eyes. She asks them if they’re comfortable, and she reminds them to relax.
She is sometimes one of the first to learn when a person has cancer.
In the cool, dim light of the mammography room on the hospital’s ground floor, Soueidan often finds herself witnessing the precise moment someone’s life has careened off course.
She knows it even before they do. It’s the moment before the doctor tells the patient, before the phone call that sucks the air out of the room.
A full picture
According to the American Cancer Society, one in eight U.S. women will get breast cancer in their lifetime.
On that July day, Soueidan stopped being just a witness.
She became a statistic.
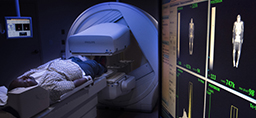
Unlike a conventional digital mammogram, a 3-D version—technically called digital breast tomosynthesis—can peer behind the obscuring layers of dense breast tissue.
This 3-D mammography can overcome what the National Center for Biotechnology Information calls the Achilles’ heel of screening mammography, where non-calcified cancers can be camouflaged by surrounding dense tissue.
In practical terms, conventional mammograms only produce a single image from top to bottom and side to side.
The 3-D mammography—approved by the FDA in 2011—takes multiple images of a breast with a single exposure, recreated by a computer as 1-millimeter-thick slices that provide a complete cross-section image of the breast. It gives radiologists a better look at the interior of a woman’s breast—a look behind and through compressed, dense tissue.
Imagine, if you will, standing in one spot and trying to see a child completely hidden behind a tree during a game of hide-and-seek.
With 3-D mammography, it’s the equivalent of having the ability to step sideways in an arc, peering around the tree and finding the child.
For countless women, 3-D digital imaging is a quantum leap in the world of mammography and in the fight against breast cancer, which claims more than 40,000 lives each year.
“With 3-D images, radiologists are able to look at them as if they were turning pages of a book,” said Maria Frendo, Gerber Memorial’s lead mammogram technologist. “That’s important, because it’s the best way to see through dense tissue.”
Frendo, who has been performing mammograms for more than 30 years, helped acquire and launch 3-D mammography at Gerber’s Betty Ford Breast Care Services.
That phone call
Of the patients in line for their 3-D mammogram on July 7, 2015, Soueidan went last.
Mammography guidelines
The American College of Radiology and the Society of Breast Imaging recommend that women undergo annual screenings starting at age 40 if they’re at average risk of breast cancer.
For those at increased risk of breast cancer, the guidelines for annual screening are very specific.
- Women with certain BRCA1or BRCA2 mutations, or those who are untested but have first-degree relatives (mothers, sisters, or daughters) with proven BRCA mutations: Yearly screening starting at age 30 (but not before age 25).
- Women with less than 20 percent lifetime risk for breast cancer on the basis of family history (both maternal and paternal): Yearly, starting by age 30 (but not before age 25), or 10 years earlier than the age of diagnosis of the youngest affected relative, whichever is later.
- Women with mothers or sisters with pre-menopausal breast cancer: Yearly starting by age 30 (but not before age 25), or 10 years earlier than the age of diagnosis of the youngest affected relative, whichever is later.
- Women with histories of mantle radiation (usually for Hodgkin’s disease) received between the ages of 10 and 30: Yearly, starting eight years after the radiation therapy, but not before age 25.
- Women with biopsy-proven lobular neoplasia (lobular carcinoma in situ and atypical lobular hyperplasia), atypical ductal hyperplasia (ADH), ductal carcinoma in situ (DCIS), invasive breast cancer or ovarian cancer: Yearly from time of diagnosis, regardless of age.
Learn more about these recommendations at the Journal of the American College of Radiology.
The radiologist looked at the computer reconstructed images, which were processed almost instantaneously.
As the doctor flipped through the pages of her breast, he saw something out of the ordinary. Tissue that would have otherwise remained hidden behind dense tissue had been uncovered in 3-D imaging.
He ordered an ultrasound, which Soueidan underwent about 30 minutes after her mammogram. Right after that, she had her breast biopsied.
Gerber Memorial employees completed all of this, from mammography to reading to biopsy, within a few hours.
The next day, Soueidan’s phone rang.
She listened.
She felt the air get sucked out of the room.
“They told me I had cancer,” she recalled. “You kind of have that feeling even before they tell you. I was worried, but I didn’t get upset about it as much as I thought I would. It is what it is, so let’s take care of this.”
She met her five-member team of experts at Spectrum Health’s Lemmen-Holton Cancer Pavilion in Grand Rapids.
The team gave her a game plan, and Soueidan chose to get treated at the cancer center at Gerber Memorial, closer to home.
She had two different types of cancer in the right breast. She started with chemotherapy, six infusions every three weeks.
When the grueling regimen ended, she underwent an MRI a few months later. It showed no trace of the cancer.
Today, Soueidan is an evangelist for the power of screening and early detection.
“Every woman in my family wanted to get screened after my experience,” she said. “I tell everyone that they need to get screened now. If you wait too long, it could be too late. Your treatment may be ineffective or much harder on your body, or both.”
You need to catch cancer early, she said.
“I thankfully caught mine at the earliest possible stage,” she said. “I’m lucky I work at Gerber Memorial, where we have the technology that basically found a needle in a haystack. It made a difference.”
Early detection
Soueidan hadn’t been the only person affected that first trial day.
Frendo, the lead tech, also underwent testing.
“A 3-D mammogram does a much better job of showing abnormalities, and it also does a better job of showing when something isn’t really an abnormality,” Frendo said.
In Frendo’s case, a cluster of tissue could have been flagged as suspicious on a conventional 2-D digital mammogram, opening the door for a biopsy to further examine the abnormality.
Instead, Frendo’s 3-D mammogram gave the radiologist a multi-angle, multilayered view that revealed nothing more than a knot of normal tissue within her breast.
No confusion, no biopsy, no barriers.
“We have found abnormalities in many women despite dense breast tissue,” Frendo said. “Using the 3-D technology that we have at Gerber Memorial, we have the opportunity to overcome obstacles and save lives by diagnosing cancer at very early stages.”
Some insurance companies, such as Priority Health, cover the whole cost of 3-D mammograms as a preventative screening.
Still, many women whose insurance does not cover the procedure have said 3-D mammograms are worth the roughly $250 price, Frendo said.
Today, Soueidan said she feels great and more energized. Her close call with mortality has rejuvenated her.
She spends her spare time doting on her 12-year-old daughter and 10-year-old son, squeezing joy out of every moment.
She says her encounter with cancer put all the choices she’s made in life into perspective: her decision to move back to Fremont from Dearborn; her decision to work at Gerber Memorial; her decision to have the 3-D mammogram test on that relatively cool summer day in 2015.
“A mammogram takes no more than five minutes, and it can make all the difference in the world,” Soueidan said.
Adds Frendo: “As women, we tend to put others ahead of ourselves. We have to take charge of our health and our own lives.”
 /a>
/a>
 /a>
/a>
 /a>
/a>