Late last summer, Tricia Johnson experienced subtle stomachaches.
Job stress, she thought. Or maybe tight muscles from starting a new workout routine.
“It was kind of constant, but not like pain,” Johnson said. “More like pressure would be the word for it. I kind of blew it off.”
But then, her stools started to change color. And change consistency.
She visited her primary care doctor, who ordered blood work.
“Everything came back pretty OK,” Johnson said. “My white blood count was a little down, but nothing she was concerned about. She chalked it up to my having irritable bowel syndrome. She gave me some anti-cramping pills. I took those for 10 days, but didn’t see any change.”
She returned for a CT scan on Aug. 30.
“I was barely home and I was getting a phone call from the physician,” Johnson said. “He said ‘I have bad news for you.’ My instinct was I thought it was my gall bladder. So when he said, ‘I have bad news for you,’ I thought, ‘Yeah, it’s my gall bladder, I’m going to need surgery.’”
Soul shock
That would have been welcome news.
Instead of hearing about gallbladder issues, she heard unthinkable words spill from her telephone earpiece: “You have pancreatic cancer.”
Johnson sat down on her bed. Shock flooded her soul.
“He must have set me up with an oncologist,” she said. “I just don’t remember much of that day. My husband (Shane) was working in Detroit. I had to call him. He couldn’t believe it. We stayed on the phone with each other that whole three-hour drive home. He even called the doctor to make sure I wasn’t hearing things wrong.”
The first week of September, Johnson met with an oncologist at the Spectrum Health Lemmen-Holton Cancer Pavilion to review her scans and biopsies.
There the news got even worse.
She had Stage 4 cancer in her pancreas, liver, lymph nodes and some of her vessels. And the cancer was too advanced for surgery.
“She told me it was the worst kind,” Johnson said.
Johnson underwent aggressive chemotherapy with four different medicines twice a month. Each session would take between five and six hours. She would return home with a pump that would continue to deliver chemo drugs.
“They told me it was going to be like dropping a hand grenade in my body,” she said. “They only gave me 6 to 9 months to live, depending on how I handled treatment.”
Johnson wasn’t about to let cancer rule her future. She started researching and studying, trying to learn everything she could to combat the criminal in her cells, the one trying to steal her health and life as she knew it.
“I learned we needed to do our part to take care of the rest of me and we changed my diet,” Johnson said. “We were typical Western Americans that ate processed foods, sugars and red meat.
“After reading a lot of different things, we changed to whole foods,” she said. “We still do some chicken and fish and learned about the top 10 cancer-fighting foods. I really do attribute that to helping me get through chemotherapy and keeping me healthy. If people don’t know I have cancer, they wouldn’t know. I don’t look like a cancer patient at all.”
Johnson concluded chemotherapy at the end of January. Scans showed the tumor had shrunk.
Reason for hope
Then, came the most encouraging news of all.
Spectrum Health surgical oncologist G. Paul Wright, MD, was starting a new clinical trial for hepatic artery infusional chemotherapy to the liver. The trial is the first of its kind in the United States and only a few places around the country have an HAI pump program.
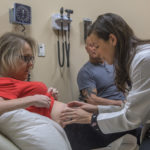
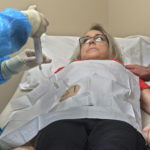
He inserted the pump in late February. During this surgery, he and his partner, fellow surgical oncologist Mathew Chung, MD, performed nanoknife ablation of the tumor in the pancreas. This uses high voltage electrical pulses to shock the tumor while preserving the surrounding structures.
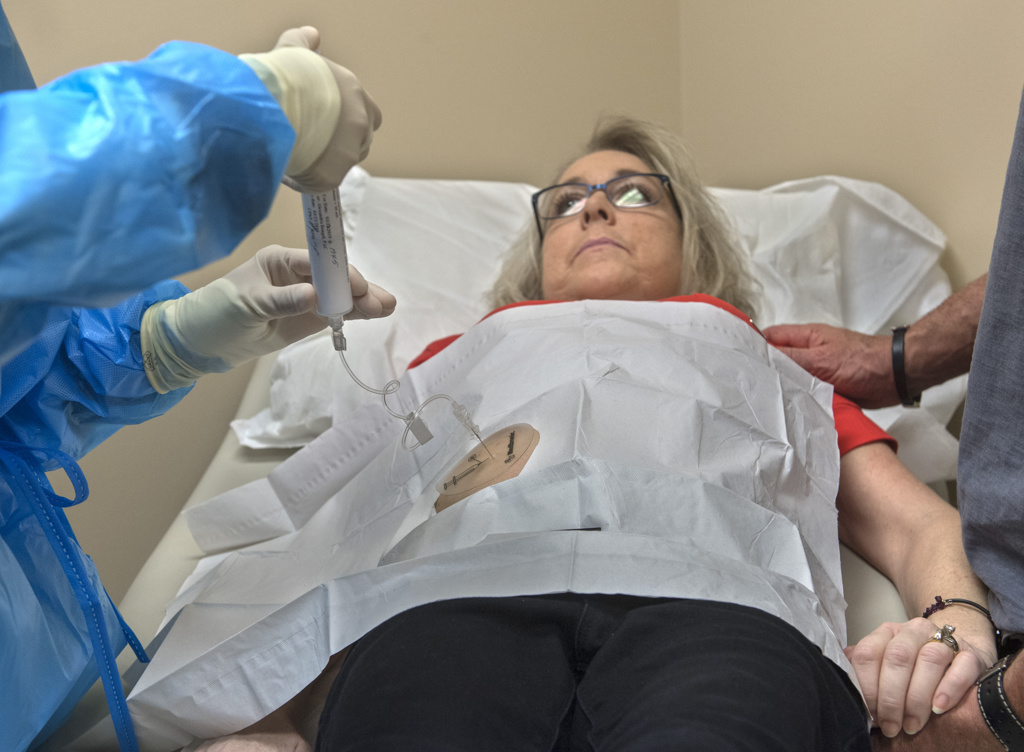
“It’s pumping chemo directly to my liver,” Johnson said. “So far so good with the pump. I haven’t had any side effects. Before with a port, by the time the chemo got to my liver, it was only 25 percent effective. Now, it’s (intended to deliver) 400 times the amount I would be getting through regular chemo.”
Dr. Wright said the hope is to increase longevity for patients who respond to what he called a “very aggressive” treatment.
“One of my primary career interests is the delivery of regional chemotherapy to isolated areas of the body,” Dr. Wright said. “This (aims to) target affected areas while minimizing toxicity that the rest of the body experiences.”
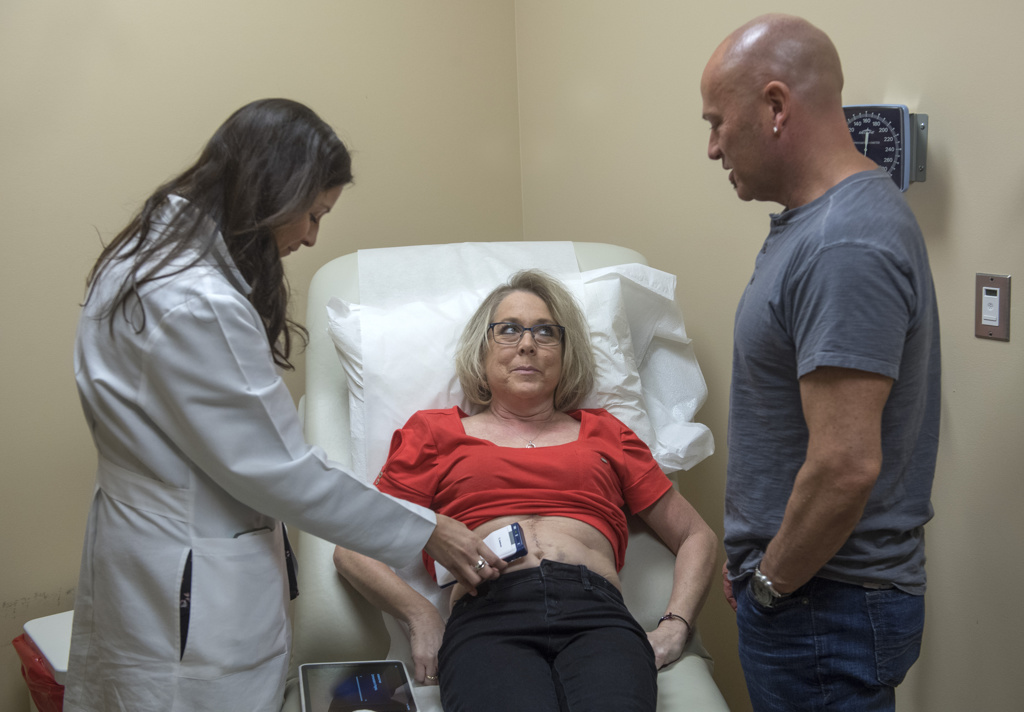
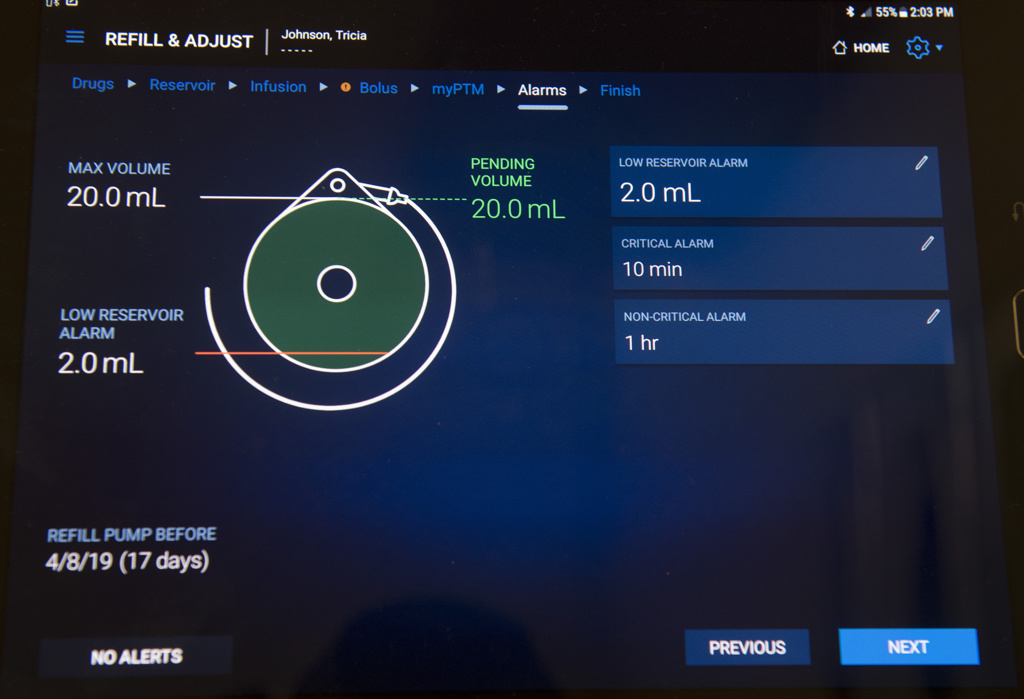
The pump in her abdomen, about the size of a hockey puck, slowly delivers high-dose chemotherapy to the liver over the course of two weeks.
“We then empty the chemotherapy out and take a two-week break before the next pump chemotherapy treatment,” Dr. Wright said. “These treatments are combined with regular chemotherapy through the standard port.”
So far, Johnson’s results are promising.
“As part of the trial we track tumor response using a blood test that is specific to pancreatic cancer,” Dr. Wright said. “So far, early into her treatment, those numbers have already improved by 90% from when she was first diagnosed.”
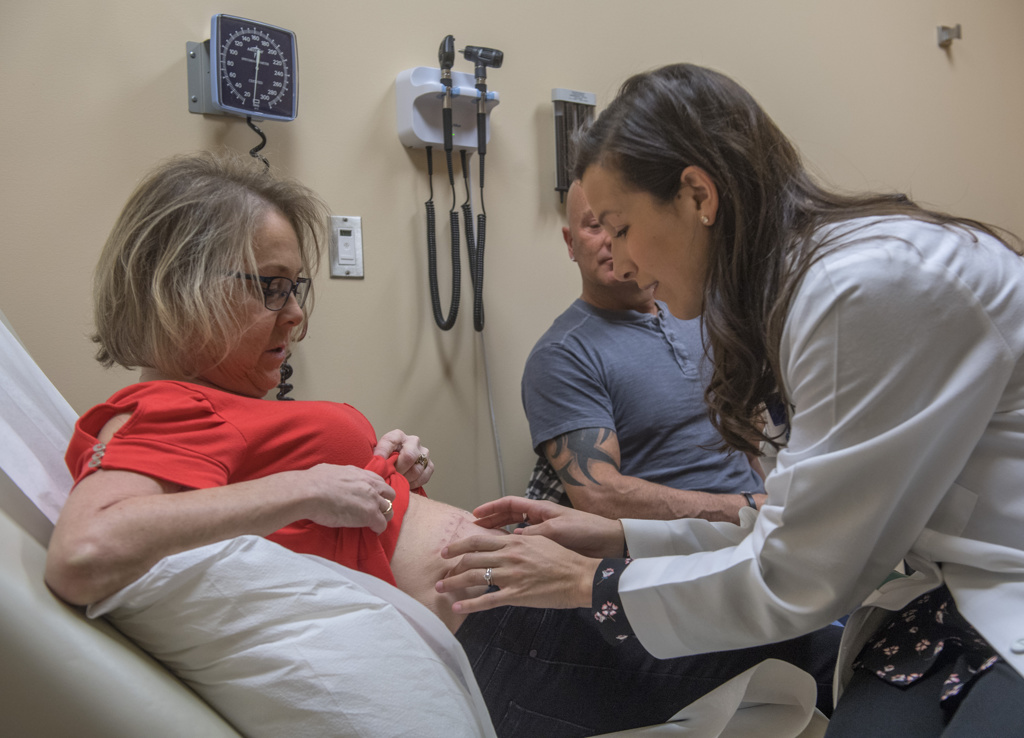
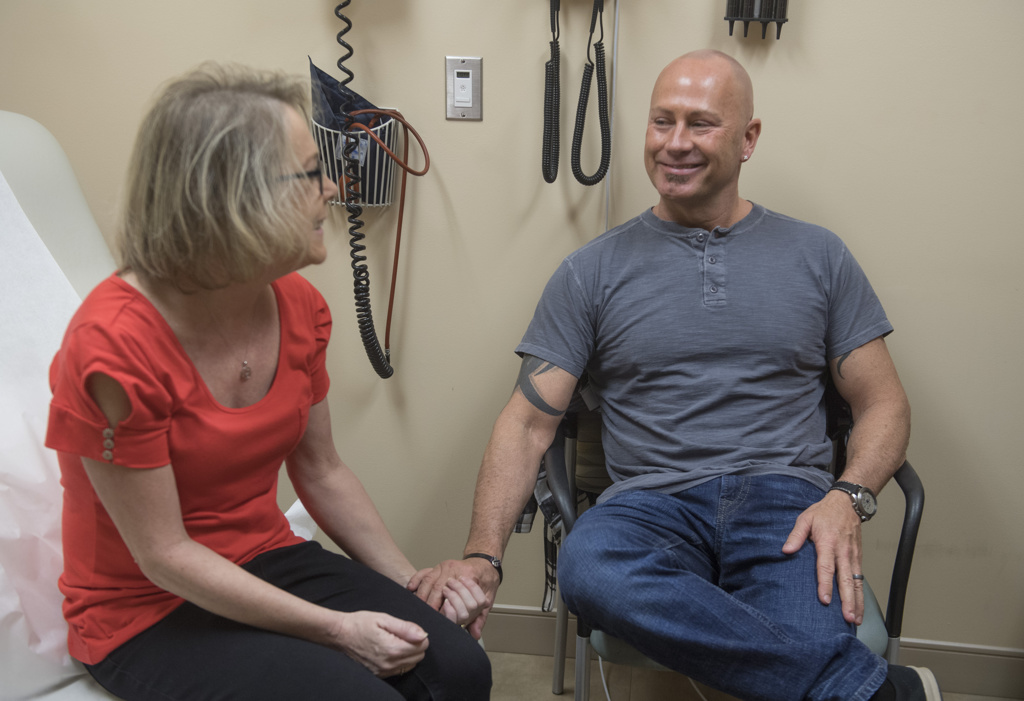
Johnson and her husband recently visited Lemmen-Holton to have the chemotherapy removed and heparin placed in the pump, as a two-week placeholder before the next treatment.
Clinical research nurse Marianne Morrissey told Johnson she’s looking great.
“We’re very hopeful,” Morrissey said.
Johnson announced that she’s ready to go back to work in her role as a restaurant manager at Brann’s in Grandville.
“Your asking is a good sign that you’re ready,” Morrissey told her.
Shane, a martial arts instructor, said his wife works out three days a week.
“I help people with health and fitness and training,” Shane said. “I’ve taken and applied all of that to Tricia, as if she’s one of my fighters. Every day we work at this. Realistically, she didn’t have six months. It was that bad. That white flag is pretty easy to throw in the air. That’s not an option now.”
Including Johnson’s attitude.
Although she felt scared at first to trial the “direct-to-the-liver” chemotherapy pump, she remained hopeful.
“I look at it like, ‘What do I have to lose?’ I’ll do anything I can to be around longer,” Johnson said.
The plan is for Johnson to undergo the clinical trial pump treatments for six months, with a CT scan after three months.
“I think that’s why I’m still here,” she said. “There’s a reason I was chosen to do this.
“Number one, it’s to help with medical research. Number two, I want to give back,” she said. “I can’t wait until I can volunteer at the hospital. Eventually, this disease is going to get me, but if I can help others have better quality of life, that makes me feel wonderful. There are so many people who have touched me, prayed for me, and done amazing things including my family members.”













 /a>
/a>
 /a>
/a>
 /a>
/a>
You continue to fight my friend. I am soo proud of you for not giving up. This is half the battle!!! You too are going to survive and join my survival club. I will continue to keep you in my thoughts and prayers. I love you sweetie. Xoxoxox
We are very happy that Tricia has a great team of Dr’s on her case and that is why she is still here because of it. Tricia also has great family & friends that are praying for her and keep positive feed back. This also goes out to her Husband Shane that has been by her side to make sure she has what she needs and their sons to help where they need it.
Love you all much.
Marjie & Jerry VanPutten (sister in-law)
This is such awesome news Tricia! Your strength is truly inspiring. I just love you to pieces! You are actively paving a road to HOPE for cancer patients everywhere! I will continue to lift you and your family in prayer, as well as your amazing team of doctors. Keep up the good fight!
Love you lady 😘
Amanda Huttinga (VanWyk)
An inspiration for me as I have stage 3 multiple myeloma which is treatable but not curable at this time. Like you my future is uncertain but I live every day to its fullest. Take care and thanks for the uplifting post
We don’t know each other but when you mentioned that your dog sensed something was wrong, we have a connection. We had a black lab named Ruby that had become very protective of me and giving me special attention. She insisted on following me into the bathroom, sit there with her nose in the air. I remember saying to my husband ” what’s the matter with that dog?” In Feb 2017 at age 66 I was diagnosed with early stage uterine cancer. I had a hysterectomy in March, started chemo along with radiation in April. Was finished with treatment end of May 2017. As of now I am 2 yrs cancer free. I was truly blessed that I had no lymph involvement but regardless you fight, maintain a positive attitude, and rejoice in each day you are given. Thank God for a support system including pets! Sadly a year later Ruby developed bone cancer and had to be put to sleep at age 6. And we got through that too with the help of another lab puppy! Be blessed in your journey.
Tricia, everyone just loves you so. You’ve always had a positive outlook and contagious energy. I’m so proud to know you. Keep fighting. Keep being you!
Keep fighting. I just finished chemo treatment 92. Almost 4 years.
Wonderful and encouraging news, Dick! Best wishes to you. 🙂
Such a sweet couple! This all so very amazing! Keep fighting!
Great news to hear Tricia. Glad everything is positive. You’re one walking m miracle. It’s always good to have a good support team, it helps make things easier. Prayers and blessings upon you and your family. PJ