Brenda Tuttle is a hands-on kind of grandma.
She likes to get down on the floor and play. She keeps her toy bin well stocked. The highlight of each week is the time she gets to spend with any of her four grandkids, all under age 6.
“I mean, give me all the babies,” said Tuttle, 52, snuggling the youngest, Graham.
Wednesday afternoons are set aside for playing with the two oldest, Roman and Luca, who, like their younger cousins, live nearby.
Two summers ago, disruption hit the Grandville, Michigan, family’s weekly routines when Tuttle landed in the ICU with a bilateral pulmonary embolism that put a strain on her heart.
With medical treatment and time, Tuttle made a full recovery. By the next summer, she had made up for lost strength through a cardio and weight-training program.
Déjà vu
In June 2018, exactly a year after her last symptoms cropped up, her shoulder began to hurt.
Figuring she’d just pulled a muscle, she tried to stretch and loosen it, but the pain only grew worse.
She iced it. She tried massage and pain medications. Her primary care doctor prescribed muscle relaxants. Nothing touched the pain.
Because of her history with pulmonary embolisms, her doctor sent her for a CT scan. The scan came out clear, ruling out heart or lung issues—but it left her without answers.
“So that was really good news, but I left there still in a lot of pain,” Tuttle said. “I was like, ‘I’m glad to know that I don’t have another blood clot, but now what?’”
Seeing their mom’s relentless discomfort, Tuttle’s three daughters urged their parents to keep pushing to find a remedy.
“It was very frustrating to be helpless and not know what to do,” said their daughter, Jessica Jaroch. “We knew something was wrong.”
Tuttle was equally frustrated—both with the lack of solutions and with how the pain affected her quality of life. She had to stop working out. She couldn’t work as hard at her part-time housecleaning job. She missed out on a lot of summer fun.
Worst of all, she could no longer hold her grandchildren.
By midsummer the pain had stretched from her shoulder into her right arm and elbow. Eventually it extended into her hand, causing numbness and tingling.
“I would massage my elbow and I was just constantly trying to do something to relieve that pain,” she said.
Feeling miserable, Tuttle again reached out to her doctor, who suggested she try the Spectrum Health Medical Group Orthopedic Urgent Care clinic.
During walk-in hours that evening, Tuttle met Tracy Smith, PA-C, a physician assistant with Spectrum Health Medical Group Orthopedics.
Smith got Tuttle an X-ray on the spot. It showed the problem didn’t originate in her shoulder.
To get to the bottom of things, Smith ordered electrical tests of muscles and nerves at the Spectrum Health EMG Laboratory, along with an MRI.
Disc replacement
A week later, Tuttle met with neurosurgeon Hayden Boyce, MD, at the Spectrum Health Medical Group Spine & Pain Management Center.
Based on her MRI and EMG results, which showed nerve and muscle degeneration, Dr. Boyce diagnosed her with a pinched nerve at the sixth and seventh cervical vertebrae, caused by a herniated disc. He recommended surgery to remove the damaged disc in her neck—a procedure called an anterior cervical discectomy.
Dr. Boyce performed the surgery just days later, replacing the damaged disc with an artificial disc.
Tuttle felt instant relief.
“I woke up and the pain was gone,” she said. “I could tell as soon as I was back in my room.”
More than a half-year down the road, Tuttle is well on the way to recovery. She completed her physical therapy sessions in the fall and is ready to jump back into a workout program.
She’s able to pick up her grandkids again, which is what matters most.
“Now it’s just rebuilding muscle slowly, and it’ll take some time, but I feel like I can lift them OK,” she said. “Everything’s good to go.”
An uncommon connection
Her two medical events—two summers in a row—have reinforced for Tuttle the importance of persistence and of advocating for yourself in the health care system.
Unlocking the mystery of her shoulder pain took what felt like a last-ditch trip to the Ortho Urgent Care clinic.
“I needed to get to the right place and for me that was Tracy at the ortho clinic,” she said. “She was like, I can see that you’re in a lot of pain, and I understand, and we’re going to figure this out.”
Smith took time to listen, Tuttle said. As she recounted her experience with pulmonary embolism and heart strain, she sensed that Smith understood her on a deeper level.
“At some point she said, ‘I get it. Like, I really get it,’” Tuttle said. Smith then revealed part of her own medical story.
“We had a connection, because I indicated to her that I had a stroke five years ago,” Smith said. “When something like this happens, you don’t know what to expect, you don’t know what to do, but you want it solved.”
Smith suspected from the start that Tuttle’s shoulder pain wasn’t really a shoulder issue. Typically if patients experience numbness, tingling and radiating pain, she said, there’s a nerve being pinched somewhere.
Her suspicion proved true—it was a neurological problem, not an orthopedic one.
Yet, Smith continued to follow Tuttle’s case.
“She called me herself at least two times to make sure that I got the appointments set up and that I understood what was happening,” Tuttle said. “That just made everything better.”
Smith’s own experience as a patient has made her a more empathetic provider, she said.
“It’s a pleasure to meet people like that—(to know) that maybe I can help them with dealing with something in their life that most people can’t,” Smith said.
“She’s a lovely individual and I wanted to make sure she was doing fine.”


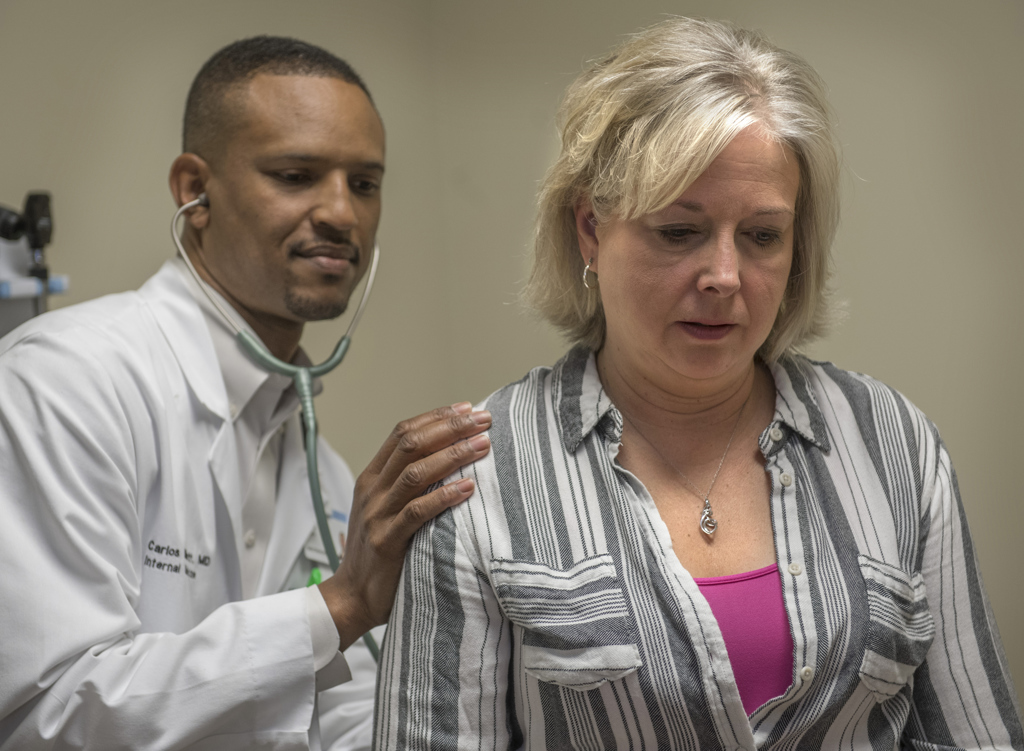
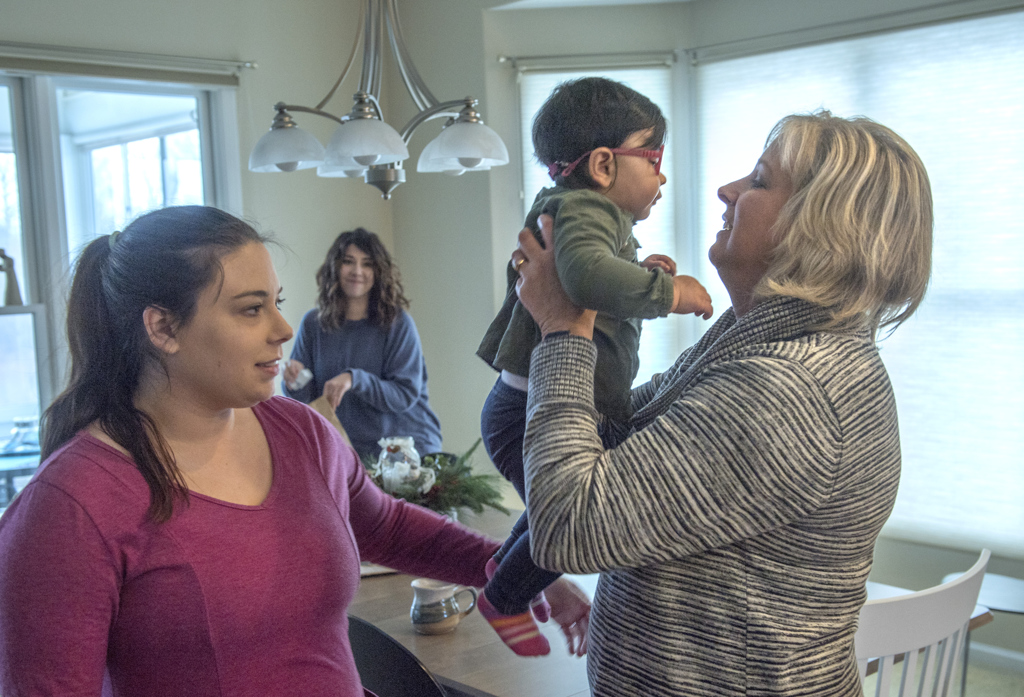









 /a>
/a>
 /a>
/a>
 /a>
/a>
An all-around feel good, positive, and purposeful story with a happy ending!