Owen Bartels lay in the neonatal intensive care unit, struggling to survive.
Ever since he’d been rushed to Spectrum Health Helen DeVos Children’s Hospital from his hometown hospital hours after birth, doctors had tried to stabilize the 5-pound, 7-ounce newborn, but his condition worsened.
No one had an explanation for his critical illness after a normal, full-term pregnancy.
Four days after his birth, his organs began to fail.
Unexplained illness
Owen’s neonatologists decided the time had come to support his heart and lungs mechanically, using an ECMO machine.
They needed more time to figure out the source of Owen’s illness. ECMO could buy them that time, though it came with its own risks.
Just then, an idea flashed through his doctors’ minds: Owen might be a candidate for the hospital’s new rapid whole genome sequencing program, which offers a super-fast turnaround on the most comprehensive genetic testing available.
They called Caleb Bupp, MD, FACMG, the Spectrum Health medical geneticist who leads the program, to discuss Owen’s situation.
Together, Dr. Bupp and the NICU team decided Owen was just the kind of child that rapid genetic testing is made for—desperately ill children whose diagnosis remains a mystery.
“We’re looking for kids that are really sick and we don’t know why,” Dr. Bupp said—kids for whom “knowing what they have as quickly as possible would make a difference on what treatment to pursue.”
Children for whom “every second is precious.”
Children like Owen.
Dr. Bupp visited Owen’s parents, Cerina and Logan Bartels, at the NICU in the Gerber Foundation Neonatal Center shortly before doctors put him on ECMO.
Stunned at the dire situation they found themselves in, the couple listened carefully to his explanation and agreed to the testing.
“We were still facing the (reality that) he might not make it through,” Logan said. “And we were immediately like, ‘Let’s do it, because even if he doesn’t make it through and they find something, it could potentially help another couple if they have similar issues.’”
It was a crushing time for the young parents from Muskegon, Michigan.
“We were crying a lot,” Cerina said. “‘Is he going to make it past all of this? Are we going to be able to go home with Owen?’ … We were very scared at that point.”
Still, they clung to the hope that their baby could pull through—and that rapid genome sequencing could pinpoint what was wrong, informing his treatment.
In July 2018, Owen became the first child in Michigan to participate in the leading-edge genomics program.
In the intervening months, eight more Spectrum Health patients have been tested.
Rapid whole genome sequencing
Helen DeVos Children’s Hospital offers this advanced genetic testing service through a partnership with Rady Children’s Institute for Genomic Medicine in San Diego, which performs the testing and compiles the results for their partner hospitals.
The process unfolds quickly:
- Once Dr. Bupp and his ICU colleagues have identified a critically ill child who could benefit from rapid genome sequencing, they ship blood samples to San Diego overnight.
- First thing in the morning, Rady’s team runs the samples through the genome sequencer and begins analyzing the results, looking for evidence of rare genetic diseases.
- The lab director gives Dr. Bupp initial results by phone, then provides detailed results electronically.
- The team at Helen DeVos Children’s Hospital uses the findings to fine-tune the patient’s care.
This program represents a tremendous leap forward in rare disease detection, Dr. Bupp said, calling it “the biggest, broadest, most expansive genetic test out there.”
It’s the kind of groundbreaking testing that took the Human Genome Project more than 10 years and billions of dollars to complete. Now it can be completed in as little as one day, for only a few thousand dollars.
In the not-distant future, this could become the standard of care for all critically ill children who lack a clear diagnosis, Dr. Bupp said.
“Whether it’s a year or five years or 10 years, that’s where we’re headed,” he said.
“The cost-benefit (ratio) is shifting so much that, you know, a day in the hospital versus a few thousand dollars for this test? It starts to tip pretty quickly.”
Plus, by using a single, comprehensive test, ICU doctors sidestep the need to run many individual tests to search for—and rule out—various disorders.
Which brings us back to baby Owen.
It took only three days for Rady’s lab director to get back to Dr. Bupp with Owen’s report.
The results, though puzzling, ultimately brought good news for Owen.
“The lab director said, ‘We ran it and it came back normal.’ And in that moment, my heart kind of sank, because I had so hoped that we were going to find something,” Dr. Bupp said.
In discussing the results with Owen’s NICU doctors, Dr. Bupp saw the other side of the coin.
“I was so focused on finding an answer,” he said, but having the results come back as normal “was a huge help to the NICU, because there’s now this tremendous list of things that we now know Owen doesn’t have.”
Owen’s parents felt the tension of unanswered questions, too.
Like the doctors, they’d hoped for a clear explanation for his problems.
“They had all the issues that they were dealing with—all these individual issues, like the pulmonary hypertension, the tachycardia, the liver failure, the kidney failure—but they didn’t understand how it all worked together,” Logan said. “And we still don’t know.”
Defying the odds
What matters most today is that Owen made a rebound.
After six days on ECMO, he showed signs of improvement and came off the machine. Though he still had serious health issues, he responded to treatment and was discharged after a month in the NICU.
Nurses and therapists from Spectrum Health At Home paid daily visits to provide medical support. Volunteers from the Parent-to-Parent Partnership Program provided emotional support.
Yet, life remained stressful for Cerina and Logan, who faced mounting financial pressures while caring for a medically complex baby.
Unsettling questions lingered: What side effects did ECMO create? How well would Owen bounce back? Would he face disabilities as he grew?
“It was very overwhelming, being first-time parents,” Cerina said.
But Owen kept fighting for his future.
At 2 months, he took a bottle for the first time. At 4 months, he could hold up his head. At 5 months, he recovered the use of a vocal cord paralyzed during the ECMO process.
At 6 months, he began to sit up. And by 9 months, he could rock on his hands and knees.
“A lot of the things they said that they weren’t sure he was going to do, he started doing right away,” Cerina said.
And though doctors recently diagnosed him with infantile spasms, he has responded well to anti-seizure medication.
“Our in-home care says that Owen so far is beating the odds with everything,” Cerina said, competing to be heard over her jabbering baby.
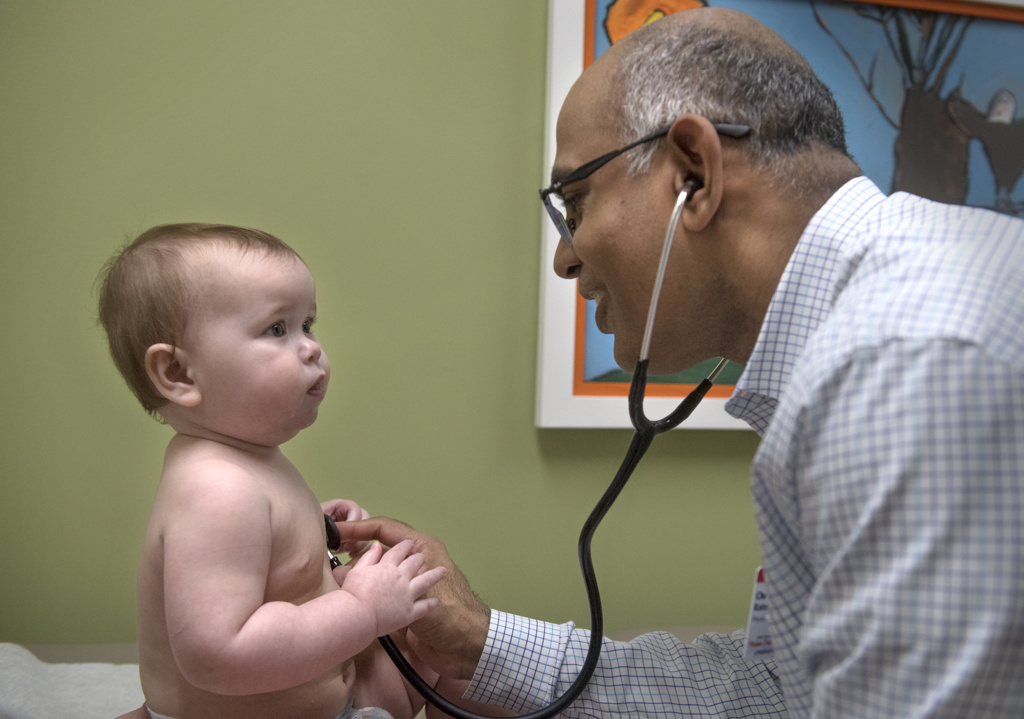
Owen still sees specialists in neurology, neurodevelopment, pulmonology and cardiology at Helen DeVos Children’s Hospital.
His cardiologist, Christopher Ratnasamy, MD, expects Owen to outgrow the abnormal rapid heart rhythm he’s experienced since his days in the NICU. He hopes to wean Owen off his heart medication in the coming months.
“He’s getting better,” Dr. Ratnasamy said. “He doesn’t have a congenital structural heart disease. Only an abnormal heart rhythm. And we’re thinking it’s probably related to the ECMO cannulation.”
That’s more good news for a spirited baby who refuses to give up.
Despite everything they’ve been through in Owen’s first year, his parents say they would do it all again.
“We are very blessed and honored to be his parents and I don’t think that I would ever change anything that’s happened to us,” Cerina said. “It sounds bad—our story is crazy—but he’s special and he is healthy and he’s doing well and he’s happy, and that’s all we want.”
Dr. Bupp, pleased as he is with Owen’s progress, still puzzles over the test results. He still grapples with the knowledge that for every seriously ill child who gets a genetic diagnosis, there may be a baby like Owen whose symptoms remain a mystery.
“There’s so much more complexity to this,” he said. “I’m excited that we’re a part of helping figure out what’s the future.”







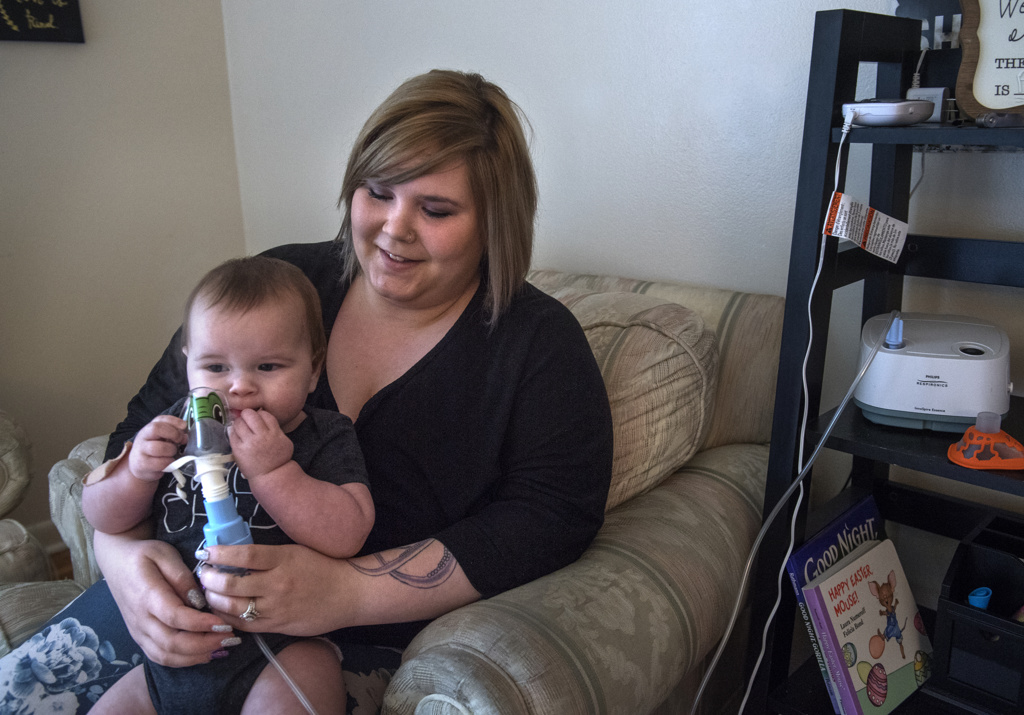











 /a>
/a>
 /a>
/a>
 /a>
/a>
I love u so very much owen and glad yo say I’m ur aunt!