Mary Beth LaBelle knew her knee had deteriorated.
While living in Colorado for work, she could barely hike 30 minutes before cutting the hike short. Her knee would swell the next day.
She couldn’t walk without pain, let alone dance—one of her lifelong passions.
LaBelle, 59, tried hydrocortisone shots in 2012. She tried pain medication for years.
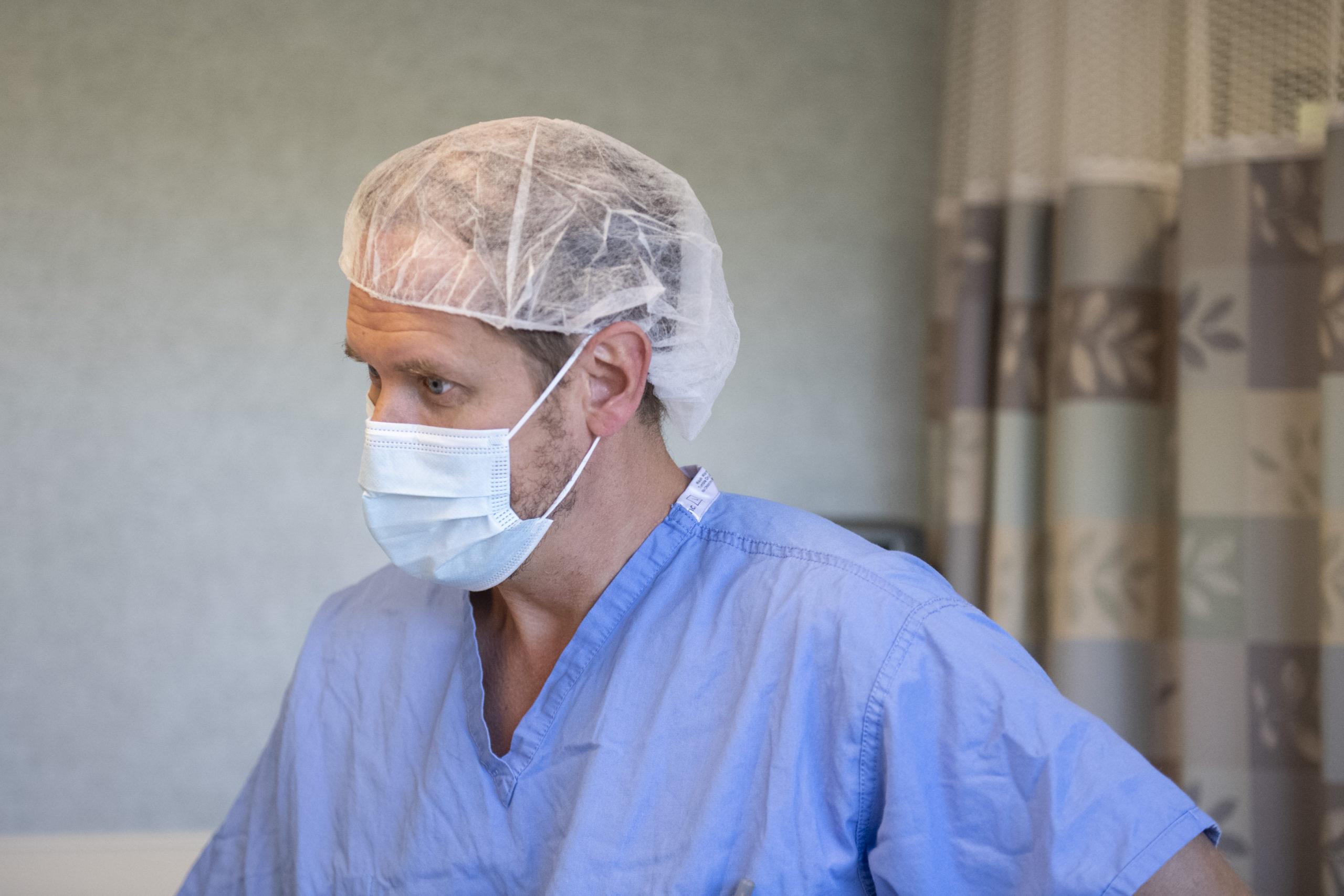
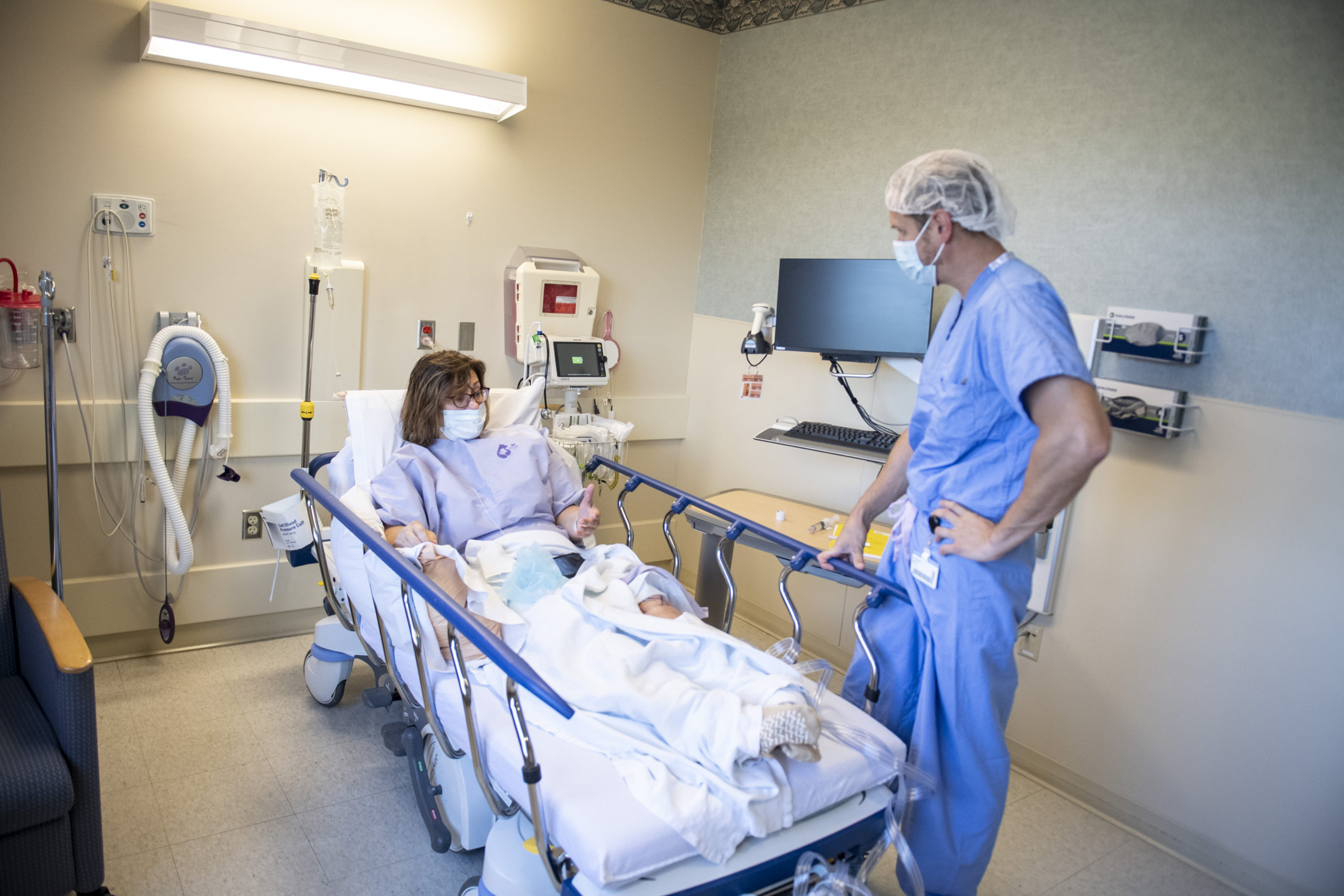
In January 2021, in consultation with her primary care doctor, LaBelle met with Spectrum Health orthopedic surgeon C. Christopher Sherry, DO.
“They take a knee X-ray immediately of both of your knees,” LaBelle said. “And he brought it up right on screen and he said, ‘Oh my gosh—you have no cartilage left.'”
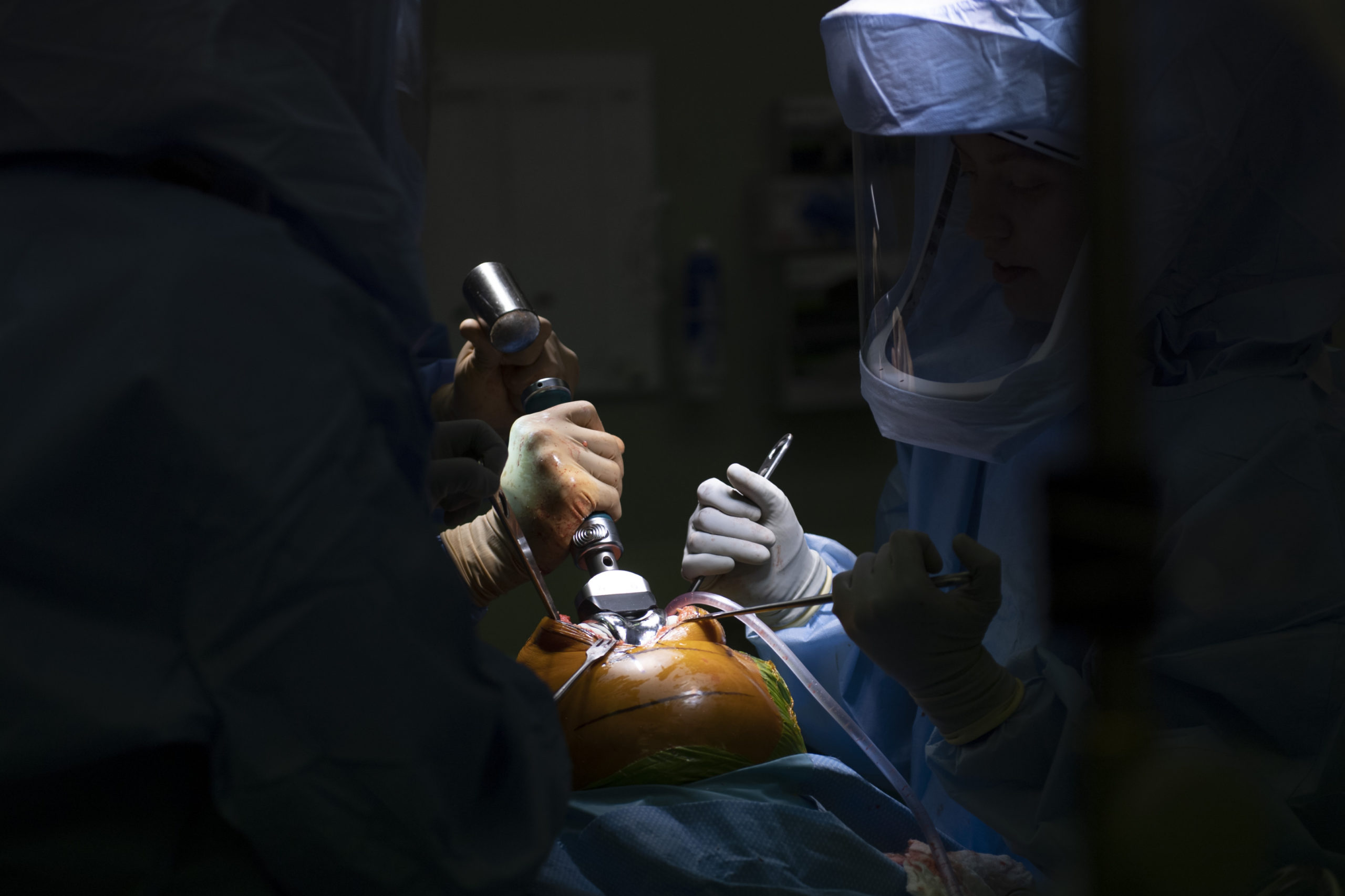
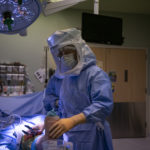
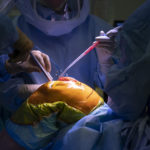
Within a week, Dr. Sherry had her scheduled for surgery.
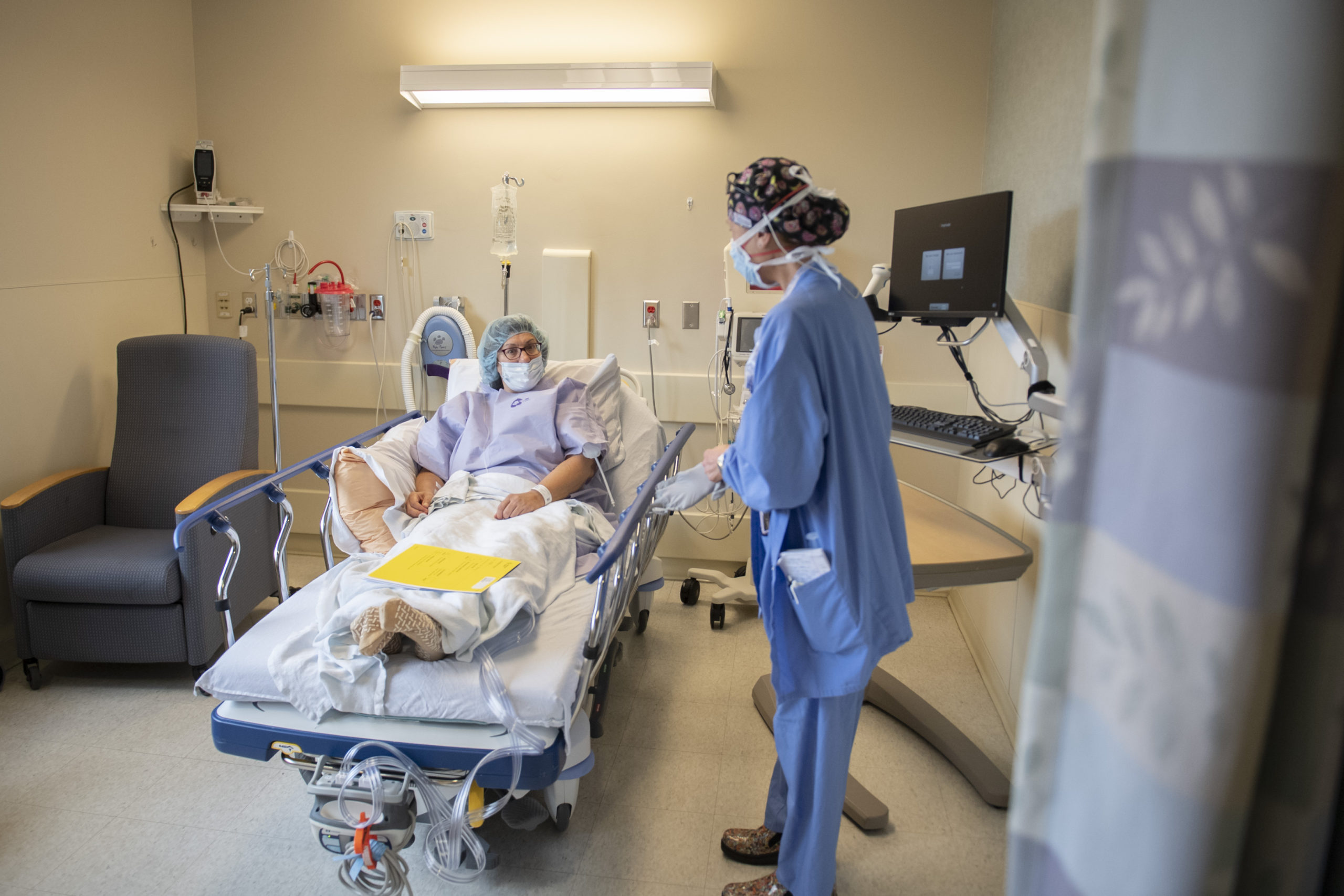
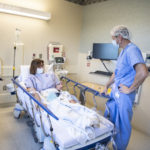
That came Feb. 8. Several hours later, she showed doctors she could walk with a walker and make it safely to the bathroom. She could navigate steps, too.
Doctors allowed her to return home.
Younger patients
Dr. Sherry, section chief of adult reconstruction in the orthopedics group at Spectrum Health, said LaBelle’s experience—which included outpatient knee replacement surgery—isn’t unusual nowadays.
“It has come a long way,” he said of joint replacement surgery. “We’ve found better ways to optimize patient (outcomes), to decrease risks associated with the surgical procedure.
“We do a better job of mobilizing patients after surgery. We use better multi-modal pain controls.”
It ultimately helps patients get up and moving.
“We’ve dramatically decreased length of stay in the hospital following knee replacement,” Dr. Sherry said. “Ten years ago, the average length of stay was four days. And on average, it’s just over one day now.”
Joint replacement can even be done as an outpatient procedure, as happened with LaBelle.
“We’re doing knee replacements that go home the same day as surgery,” the doctor said.
The average age of a patient has also gotten younger, dropping from 68 to 66 years old.
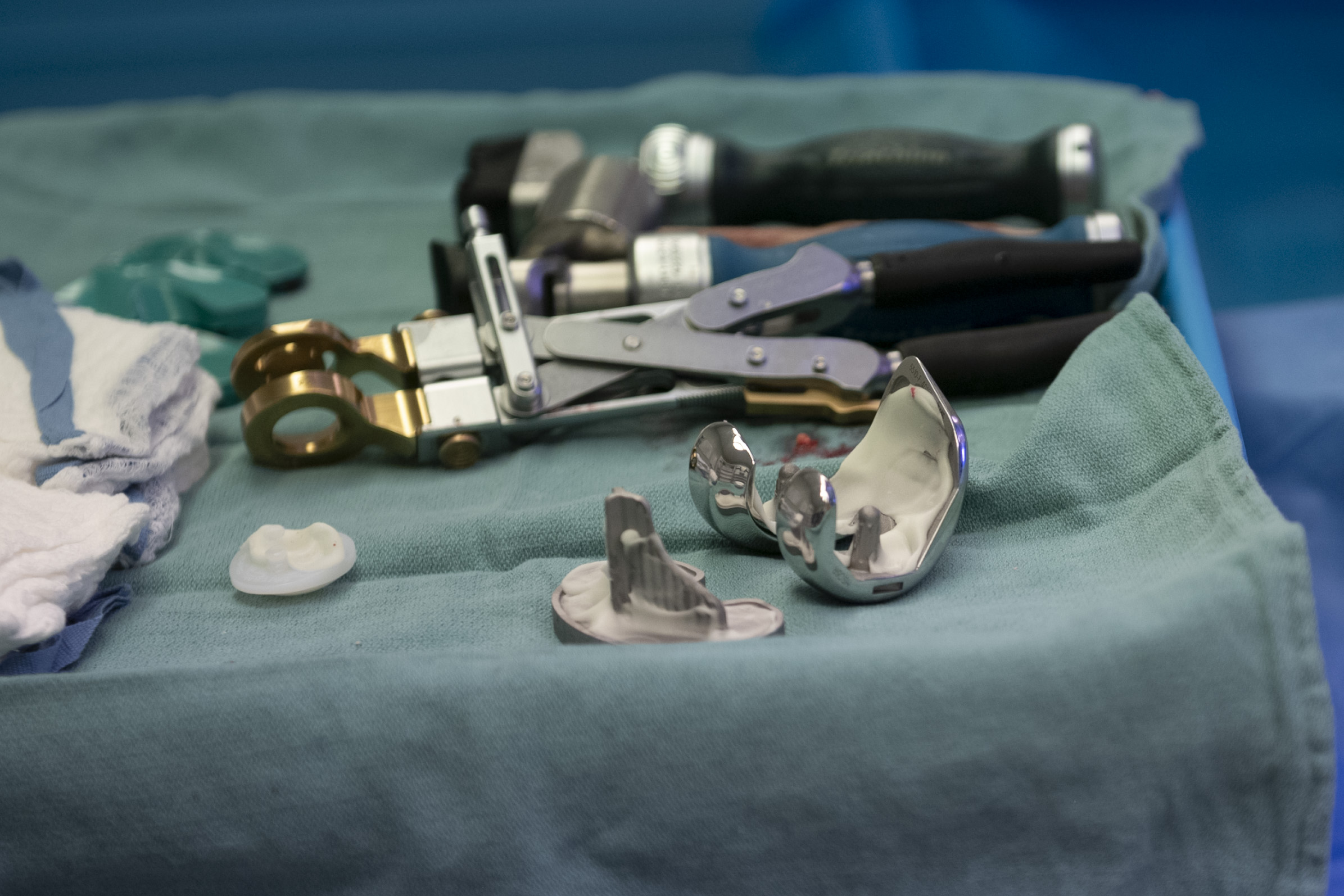
Patients in their 40s and 50s are coming in much more regularly, Dr. Sherry said. In addition to improvements in surgery and post-surgery procedures, the physical quality of the implants has also improved.
“It’s a big surgery, you don’t want to downplay that,” Dr. Sherry said. “But once you get it done, a lot of patients say, ‘I wish I would have done that five or 10 years ago.’”
It’s an easier road than most patients think.
Pain-free
LaBelle first started experiencing knee pain in 2004, after tearing her ACL and having surgery to repair it.
She waited 16 years to schedule her first knee replacement surgery. Then she had her other knee replaced in October, just eight months after her first surgery.
She had no fear of surgery. In fact, she’d looked forward to it.
“I think the only way I can describe handling surgery: It’s being a new parent versus having your second child,” she said. “When you do not know what to anticipate, the process is overwhelming. Am I supposed to feel this pain? Am I not? … It’s a lot of unknowns.”
But the second time through it, she said, you understand the signals your body sends.
Spectrum Health ensures you have knowledge and comfort at every stage, she said—from the helper sitting in your outpatient surgery suite when you wake up, to the physical therapists, nurse navigators and extensive information packets.
LaBelle recently spent a night dancing at a club for three-plus hours. The next day she walked around Grand Rapids pain-free.
She’s headed to Florida in July with her daughter to see family and visit Disney World.
“Can you imagine?” she said. “That’s non-stop walking. And I’m looking forward to it.
“The whole idea is to live your best life by experiencing what our world offers, in people and places. I want to go, explore and take advantage of this sweet life with strong knees.
“Plenty of people get their knees replaced in their 70s and they wait and wait and are in pain,” she said. “But everyone says the same thing once they get it done: ‘I should have done it sooner. Why did I wait?’”
LaBelle’s decision to schedule her second knee replacement soon after her first is actually not unusual, given the positive benefits of joint replacement.
“A lot of times they’re coming back much sooner, believe it or not,” Dr. Sherry said. “I’ve got patients at their six-week post-op appointment saying, ‘When are we going to do the second one?’”
Each case varies, but generally a patient’s first knee replacement will inspire the second replacement—in short order.
“Once patients starting getting up to speed with their first joint and feeling good and getting back to normal activity, they start noticing their other bad one and how much it’s slowing them down,” Dr. Sherry said. “And they generally don’t hesitate to jump into that second joint replacement.”
Nearly 98% of patients have positive outcomes, but it also helps to have a positive outlook for peak success.
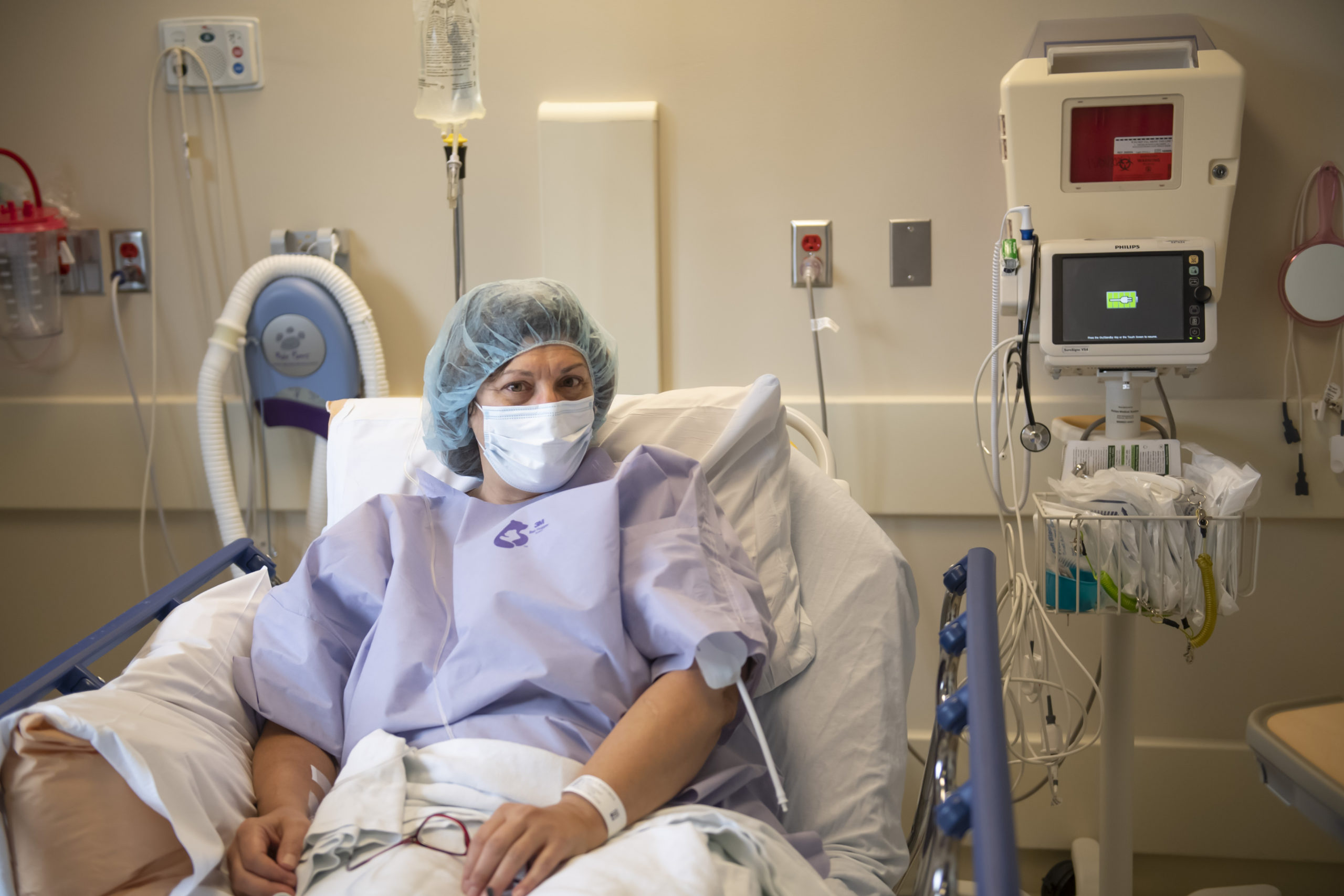
LaBelle had that—and she proved the ideal patient.
“She was a very motivated patient, really had the desire to do well and then did because of what she put into it pre- and post-surgery,” Dr. Sherry said.
The pain LaBelle had been experiencing had affected her quality of life.
“She couldn’t function at a really young age,” Dr. Sherry said.
The joint replacements fixed that, “giving her back everything she wants to do, pain-free,” the doctor said. “And that’s really exciting.”











 /a>
/a>
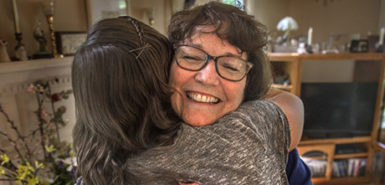 /a>
/a>
 /a>
/a>
What a good story about getting the care you need to get on with your life!