Willow Eggleston, 66, had long struggled with pulmonary arterial hypertension.
She knew it stemmed from a congenital heart defect. She also knew doctors determined nothing could be done to remedy the problem.
And she remembers precisely the moment her situation tilted from chronic illness to pure terror.
It happened in March 2019.
One minute she was minding Lillian and Evelyn, her two young granddaughters, as they peacefully watched a movie and munched on pizza. The next, she found herself sprawled back in her recliner, one of the girls leaning over her.
“Lilly kept saying, ‘Gramma, wake up! What happened? Are you OK?'” Eggleston said.
Eggleston roused herself enough to know she faced serious trouble.
“I called 911 and I called my daughter to tell her to come and get the kids,” she said. “The two little girls were still there when the ambulance came, lights flashing.”
The ambulance whisked her to Spectrum Health Butterworth Hospital.
There, doctors delivered a dire prognosis.
“When they warned me that they might have to intubate me and put me on a ventilator, it was scary,” Eggleston said. “I tried my best to stay positive.”
While it wasn’t the first time she’d been hospitalized for this condition, it would be the most frightening.
And she found it increasingly difficult to stay positive.
‘That’s just not me’
By her mid 60s, Eggleston had already weathered her share of ups and downs.
Doctors first diagnosed her heart defect, a large hole in her heart known as an atrial septal defect, when she was in her 40s. It helped explain some of the minor symptoms she’d been having, such as flutters and breathlessness, for much of her life.
But the Bath, Michigan, resident also learned she had an inoperable condition.
Any attempt at corrective surgery might be fatal.
Her symptoms worsened over the years.
“By now, I was wearing a diaper and using a walker,” she said. “I didn’t want to eat. And I had so much fluid I couldn’t lay flat on my back.”
Her care team initially suspected a double lung transplant might help, but they quickly determined she wasn’t a suitable candidate for transplant.
Eggleston found it hard to ward off despair. Her body’s systems began to fail, including her kidneys.
She remembers that terrible feeling of defeat.
“That’s just not me,” she said. “It bothered me so much that I wasn’t that strong person anymore. My daughter finally pleaded with me, saying, ‘Mom, please don’t give up.'”
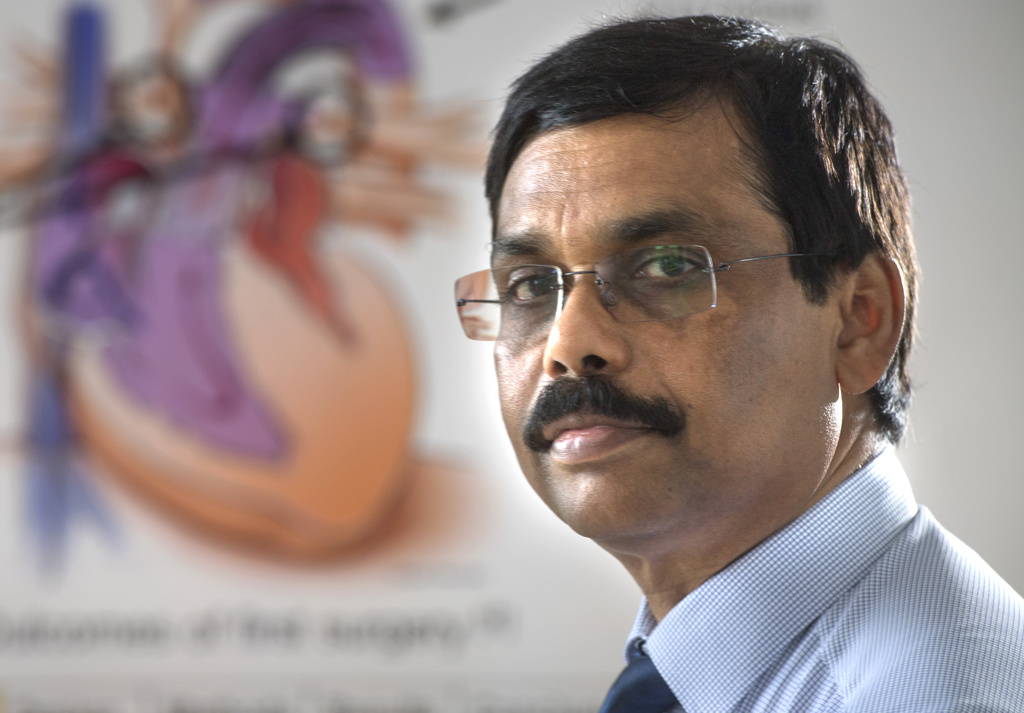
Reda Girgis, MD, medical director of the Lung Transplantation Program referred Eggleston to Joseph Vettukattil, MD, a congenital cardiologist at Spectrum Health Helen DeVos Children’s Hospital.
Dr. Vettukattil has extensive experience repairing heart defects.
“He told me he could fix the hole in my heart,” Eggleston recalled. “I said, ‘No, you can’t. It’s not fixable.’ He said, ‘Yes, I can.'”
Custom from Europe
In a healthy heart, blood comes in through two large veins and then empties oxygen-poor blood into the right atrium or upper chamber.
Blood then flows into the right ventricle as the atrium contracts, which pumps it into the lungs.
Once the lungs replace the oxygen, it flows into the left atrium and then the left ventricle, which pumps it to the entire body.
Normally, that results in equal amounts of blood in each direction, Dr. Vettukattil said.
But the hole in Eggleston’s heart meant that, all her life, her lungs had been receiving three to four times more blood than the body.
This caused a constant, excessive pressure—and it was the source of her worsening symptoms.
In Eggleston’s case, the heart defect manifested as lung pressure.
“She was really unwell,” Dr. Vettukattil said. “The fluid was accumulating in her body and she couldn’t walk. She couldn’t breathe.”
She was diagnosed with atrial septal defect-associated pulmonary hypertension, a misunderstood and inappropriately managed cardiac defect which occurs mainly in women. The reason why almost 80% of patients with this condition are women is still unclear, Dr. Vettukattil said.
Eggleston’s heart had a large hole—about 40 millimeters, or an inch and half.
“We couldn’t completely close it,” the doctor said. “Her heart wouldn’t be able to cope with the sudden change in the hemodynamics.”
Instead, in June 2019, he performed what’s called a fenestrated atrial septal defect closure, using a Fenestrated Atrial Septal Defect (FASD) Occluder from a European manufacturer. The investigational device, made by Occlutech, a Swedish company, is not yet approved for use in the United States by the Food and Drug Administration.
The FDA granted compassionate-use authorization for use of the FASD Occluder in Eggleston due to her clinical condition.
Rather than opting for open-heart surgery, Dr. Vettukattil inserted the device by threading a wire through an artery near her groin.
In 45 minutes, he reduced the gaping hole in Eggleston’s heart to 8 millimeters.
The catheterization procedure, done at Helen DeVos Children’s Hospital, goes quickly. But the body’s recovery is slow.
Children typically bounce back faster, often within six months. Adult hearts may never return fully to normal, but they do improve.
“The damage has been done to the heart for a long period,” Dr. Vettukattil said.
Much of his work focuses on pediatric patients, but it’s common for heart defects to show up much later in life. He has performed cardiac catheterizations on patients as old as 82.
Congenital heart defects are the most common birth anomalies, affecting about 1% of children born each year.
The Centers for Disease Control and Prevention estimates roughly 1 million children and 1.4 million adults have such defects.
Getting her life back
While her pulmonary arterial hypertension will never fully disappear, Eggleston has gradually felt the benefits of the procedure.
“Within a month, I wasn’t constantly sleeping anymore,” she said. “I still needed the oxygen at first, but then less and less.”
She still uses a portable tank when she goes out for walks.
“It took a year for my heart to get back to the normal size,” she said. “But I can clean the house. I get on the treadmill.”
She and her husband are traveling again, their eyes set on Orange Beach, Alabama, for some time in the sun.
And where she once took three medications to treat her pulmonary hypertension, she’s down to one.
She often pinches herself as she contemplates just how different her life is today.
“I know I’m 66, but I don’t feel it,” she said. “I feel like Dr. Vettukattil gave me another 30 years to enjoy life.”
She continues to monitor her heart rate and oxygen levels.
She and Dr. Vettukattil hope the device in her heart gains approval from the FDA. More people may then learn about the treatment over time.
“It’s this one little piece of hardware that changes everything,” Eggleston said.
Dr. Vettukattil has since fitted the new devices in five patients, all women.
“We have broken the myth that there is nothing that can be done to help them,” Dr. Vettukattil said. “And we believe this procedure will become more common as a result.”


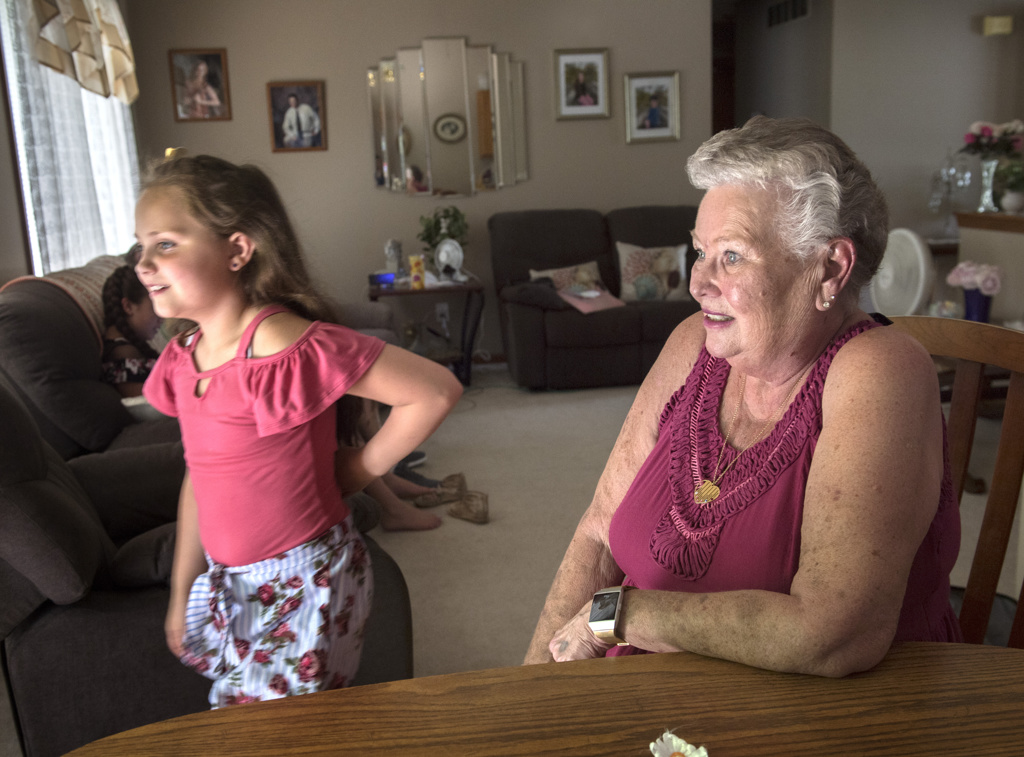
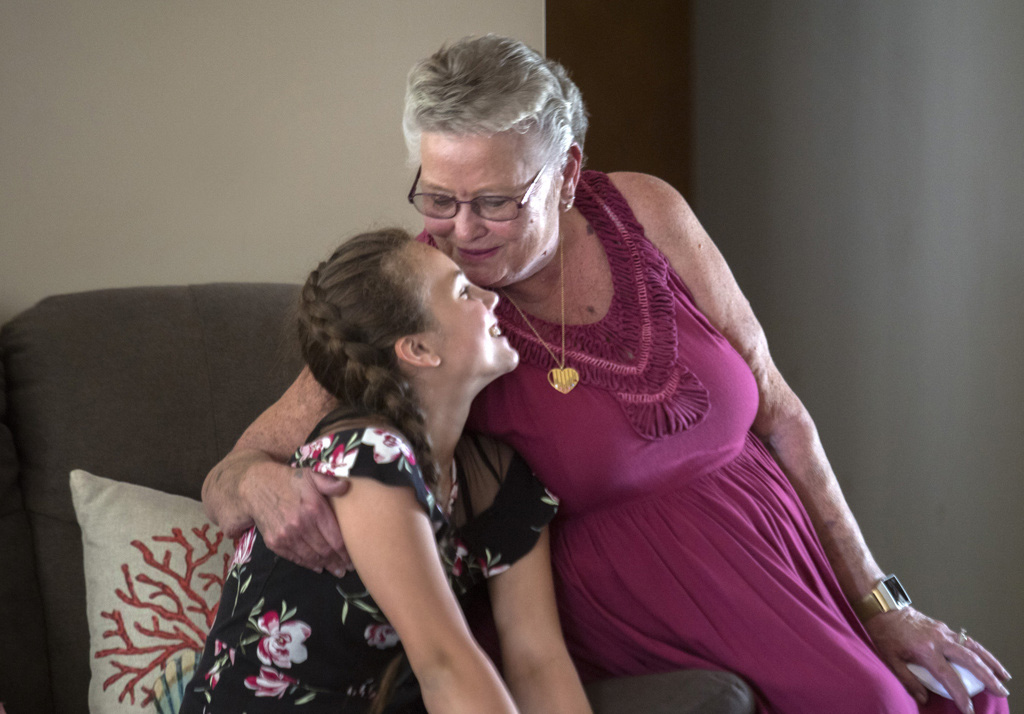

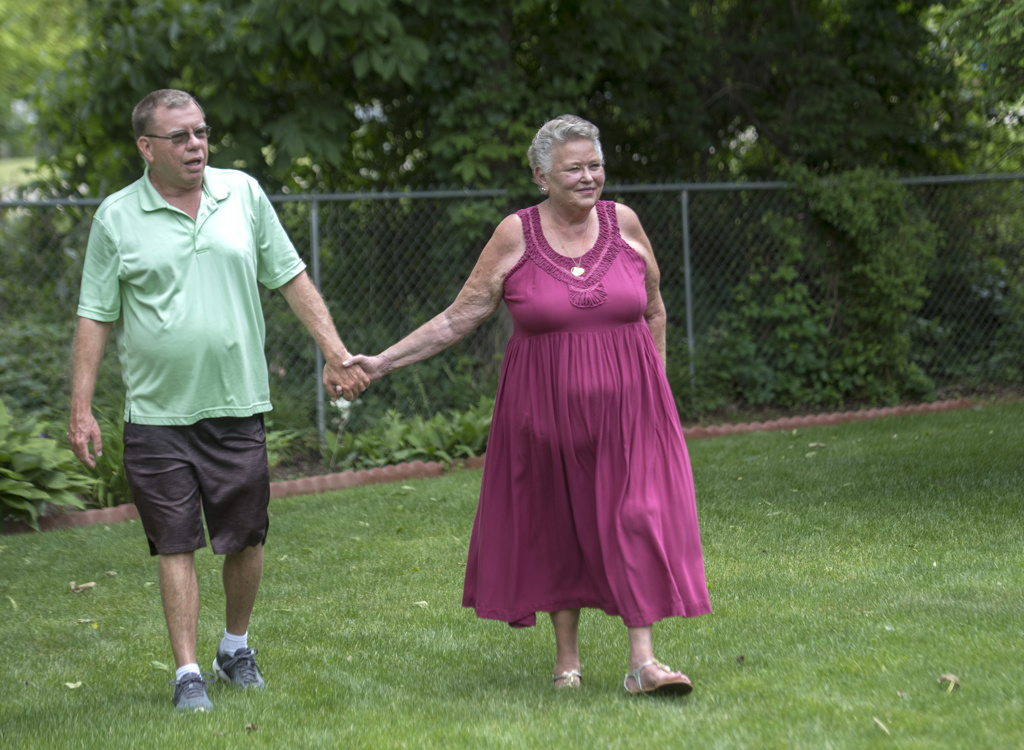









 /a>
/a>
 /a>
/a>
 /a>
/a>
Wonderful Doctor!! Love the story and
the outcome!! Enjoy life🙏
Thanks Dr.Vettukattil God Bless You!!
I was very intrigued when I saw this message. I have been diagnosed with a very small hole in my heart from birth. I also have lung issues as well as CHF. And have been told nothing can be done. I also have asthma and sleep apnea, I have O2 to use when I need it. At times I am very short of breath but my O² meter says like 96. Any ideas? Thank you
Please discuss with your provider. He or she will have the best personalized solutions available for you. Wishing you the best.