One heart. Three mysteries. That’s Mary Chittle’s story.
The 7-year-old girl’s heart suddenly stopped pumping one day. The time and the place that it happened―that’s the first mystery.
No one knows how long her heart had raced like a car at full throttle. She went to school, ran and played and kept up with her sisters and brother.
Seemed a little tired, maybe. Had a cough. But other than that, Mary showed no sign that her heart was pounding boom-boom-boom, 200 beats a minute, day in and day out. She looked the picture of a healthy little girl. Not someone on the verge of sudden cardiac arrest.
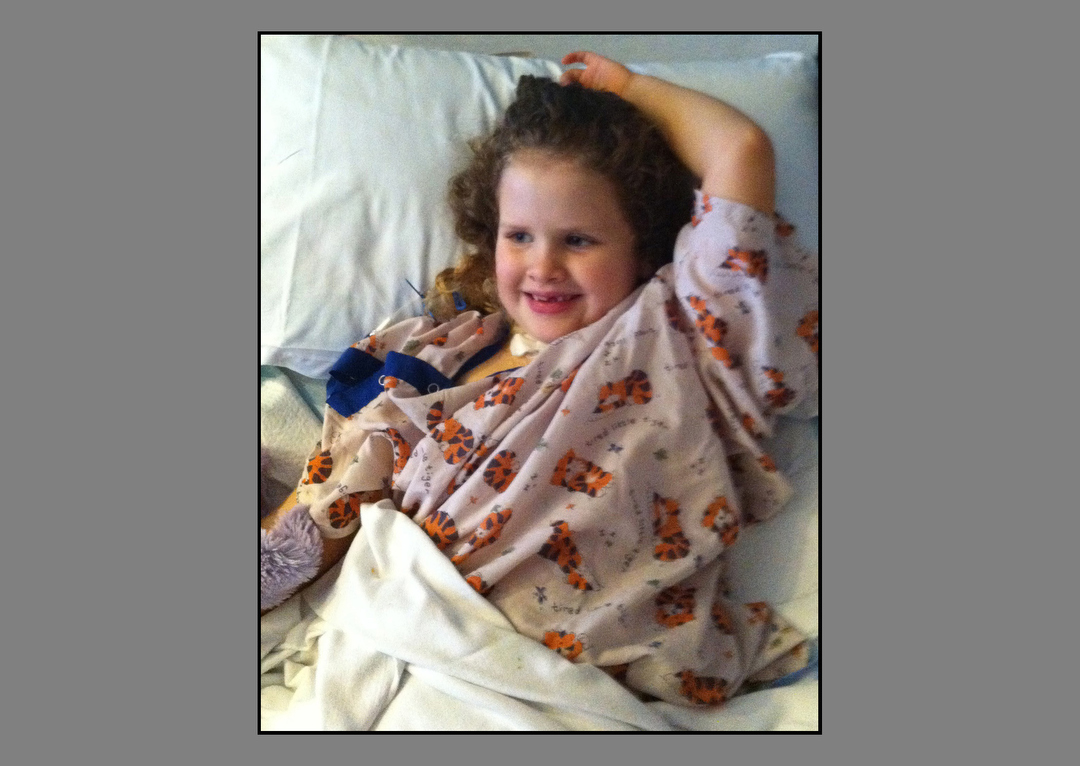
But when her heart finally gave out, it could not have picked a better spot. She lay on an operating table at Spectrum Health Helen DeVos Children’s Hospital, surrounded by dozens of doctors, nurses, medical personnel and highly specialized cardiac equipment. Her mom and dad stood beside her, praying and crying.
Even with all that expertise and technology―and love―at the ready, no one can quite explain her survival in that harrowing moment.
That’s the second mystery.
I love them all.
“Something magical happened. Whether it’s God or ―” Darryl Elmouchi, MD, begins to cry.
He can’t tell Mary Chittle’s story without weeping.
A cardiac electrophysiologist, he performed the procedure that tamed her heart’s wild ride, that restored a normal rhythm. That saved a child’s life.
He considers that moment his “greatest save,” even though he struggles to explain how it all turned out.
But oh, does he rejoice in the outcome. So do the dozens of people on the medical team who worked to get Mary’s heart pumping again.
And so does Mary.
“I love them all,” she says.
Five years have passed since Mary faced her life-and-death crisis.
She’s 12 now. A tennis player, a trombone player, an A-student, a spunky girl with long, wavy brown hair, a kid who likes to tease her dad―in short, a middle-schooler who emerged from the trauma sharp as a tack both mentally and physically.
That’s the third mystery.
One girl. Three mysteries.
A child with congestive heart failure
It began on a winter day. Mary is the third child of Kim and Erick Chittle―whose family included six kids at the time and has since grown to eight. They live on an acre of land in a rolling, wooded subdivision just outside Traverse City, Michigan.
Mary had a bad cough, so her mom called in Mary’s grandfather, who is a physician assistant.
“I felt really tired,” Mary recalls. “I’d been tired for a long time. I’d been getting headaches a lot.”
Her mom worried about strep throat and pneumonia. But as Mary sat on his lap, her grandpa noticed something else: her racing heart.
Her parents took her to a local hospital. There, staff decided to send Mary to Helen DeVos Children’s Hospital in Grand Rapids, Michigan, 140 miles away. Mary remembers being terrified.
“I did not want to go in the helicopter because I couldn’t take a parent with me,” she says.
“She was kind of freaking out,” Kim says. “Her heart rate was already high and she was getting very upset about going without me.”
Instead, staff arranged for Mary and her mom to go by ambulance to the airport, where the two took a flight to Grand Rapids. Erick drove down to meet them.
By the time Mary arrived at the hospital, she’d already suffered the effects of the rapid-fire heartbeat. She was a first-grader with congestive heart failure.
I didn’t know what to ask. I didn’t know what to hope for.
Typically, the body’s own pacemaker regulates heart rate. But any cells in the heart can send out electrical impulses.
One little area in Mary’s heart started firing at 230 beats a minute. And whatever is fastest in the heart wins, Dr. Elmouchi says. That rapid heart rate takes a toll on the heart muscle.
“It’s kind of like taking your car and driving it from here to California at red-line the whole time,” he says. “By the time you get there, your engine’s not going to be good. That’s what happened to Mary’s heart.”
Medications failed to lower her heart rate. Pediatric cardiologist Kim Lee, MD, and cardiologist Andre Gauri, MD, told the Chittles they wanted to do a study of the heart to find the spot that was misfiring. Dr. Gauri would do an ablation―or “zap it” to stop the electrical impulses.
On Monday, Feb. 20, they took Mary to a cath lab at the Spectrum Health Fred and Lena Meijer Heart Center, which adjoins Helen DeVos Children’s Hospital. Mary went under anesthesia, and Dr. Gauri was about to start the procedure when she went into cardiac arrest. Her quivering heart ceased to pump blood.
‘Jesus, save my daughter’
When Dr. Elmouchi heard the “code blue,” he ran to the cath lab.
“There were probably 40 people there, people from the children’s hospital, people from the adult hospital. Everyone was crying,” he says. “For about two hours, she would get CPR for like 20 minutes because her heart would stop working. They would shock her, and they would try all these things and she would come back a little, and then she would go down again.”
Mary’s dad, in a waiting room, found his way into the lab. He grabbed Mary’s shoulder and prayed: “Jesus, save my daughter. Christ, save my daughter. Jesus, save my daughter.”
Kim came in the room, and Erick led her to Mary, so tiny in the midst of the throng of caregivers. A Catholic priest arrived. He gave Mary last rites, and with her parents, prayed the Litany of the Saints and the Chaplet of Divine Mercy.
“Her heart was down for 45 minutes,” Erick says. “They had someone on her chest the entire time, keeping her heart moving.”
Ultimately, the doctors decided to put her on a heart-lung machine called extracorporeal membrane oxygenation, or ECMO. The machine, connected with tubes inserted into her carotid artery, took over the job of pumping blood through Mary’s body. It stabilized her―at least temporarily.
As they wheeled Mary from the cath lab, Erick recalls a doctor saying, “Thank God for small mercies.”
“What do you mean?” he asked, incredulous.
“This has been going on for weeks,” the doctor said. “If her heart was bound to stop, it could have stopped in your backyard. Anywhere. But it stopped here, with all of us to do this for her.”
Ah, Erick thought. Maybe that is a mercy.
They made a slow, solemn trek back with Mary and the ECMO machine to her room. Erick recalls looks of sorrow on the faces of staff as they passed.
“It was like a defeated army coming home,” he says.
Her doctors worried about the impact on her other organs, from 45 minutes of on-and-off CPR. They lowered her body temperature to protect her brain.
“She was bloating. She was cold. She didn’t look or feel like our daughter,” Erick says.
Kim prayed, but struggled to find the words.
“I didn’t know what to ask. I didn’t know what to hope for,” she says. “I didn’t know what to think.”
Like swatting a fly, except …
Mary still needed an ablation, or the heart would not stop misfiring.
On Tuesday, the day before Ash Wednesday, Dr. Elmouchi prepared for the second attempt.
Although he had done the procedure hundreds of times, Mary’s case presented a special challenge.
Dr. Elmouchi, now chief medical officer of Spectrum Health Hospital Group, explained to the Chittles that he had never performed an ablation on a child who was on a heart-lung machine. He knew of few cases where that had been done. But even if they could find a medical center with specialists who had experience with the procedure, Mary was too fragile to be transferred.
When they told me everything was going to be OK, I broke down. I don’t remember who was holding me.
In fact, Dr. Elmouchi and the other physicians did not even want to move Mary to the adjoining Meijer Heart Center for the procedure. Instead, they turned an operating room at Helen DeVos Children’s Hospital into a cardiac cath lab. Staff from Biosense Webster, the company that makes the equipment, pitched in.
“An army of people disassembled an entire laboratory from the adult hospital and brought it over to the pediatric hospital,” he says. “And this is incredibly sensitive electrical equipment.”
In the meantime, an army of prayer warriors did their part. In Grand Rapids, family and close friends gathered. In Traverse City, where Erick is the principal of St. Francis High School, students prayed the rosary.
In Rome, the pope prayed for Mary at daily Mass―at the request of a friend with a connection to the Vatican.
The source of Mary’s trouble was a condition called atrial tachycardia. The rogue electrical impulses originated in a tiny spot in the upper chambers of the heart. As he mapped the heart, Dr. Elmouchi pinpointed the location.
In most cases, the problem occurs in the right upper chamber, but Mary’s lay in the upper left, a much harder place to reach.
To complicate matters further, it originated at the tip of the left atrial appendage, a section of the heart that hangs like a little windsock off the atrium.
It is paper-thin.
“If you held it up, you could see through it,” he says. “You are taught you never put wires or catheters in that appendage and you never burn in it because you could burn a hole or poke a hole through it. And that would be catastrophic.”
Using a catheter threaded into a blood vessel, he had to reach that spot and hit it hard enough to knock it out―but without breaking through that paper-thin tissue.
He felt like he was trying to swat a fly on a balloon with a pin.
“And it worked,” he says with relief.
Within five minutes of ablating the trouble spot, the monitor showed Mary’s heart rate and pulse moving in unison―a sign that her heart rate had returned to normal. The cath lab team erupted into cheers and high-fives.
Dr. Elmouchi went to the waiting room to meet with Mary’s parents and family.
“I was kind of speechless,” he says, choking with emotion as he recalls the moment. “I just gave the thumbs-up, and everybody started screaming and crying.”
John Huntington, MD, the pediatric anesthesiologist, used his phone to take a video of the monitor showing Mary’s heart rate. A nurse took it out to her parents.
“I cried,” Erick says. “When they told me everything was going to be OK, I broke down. I don’t remember who was holding me.”
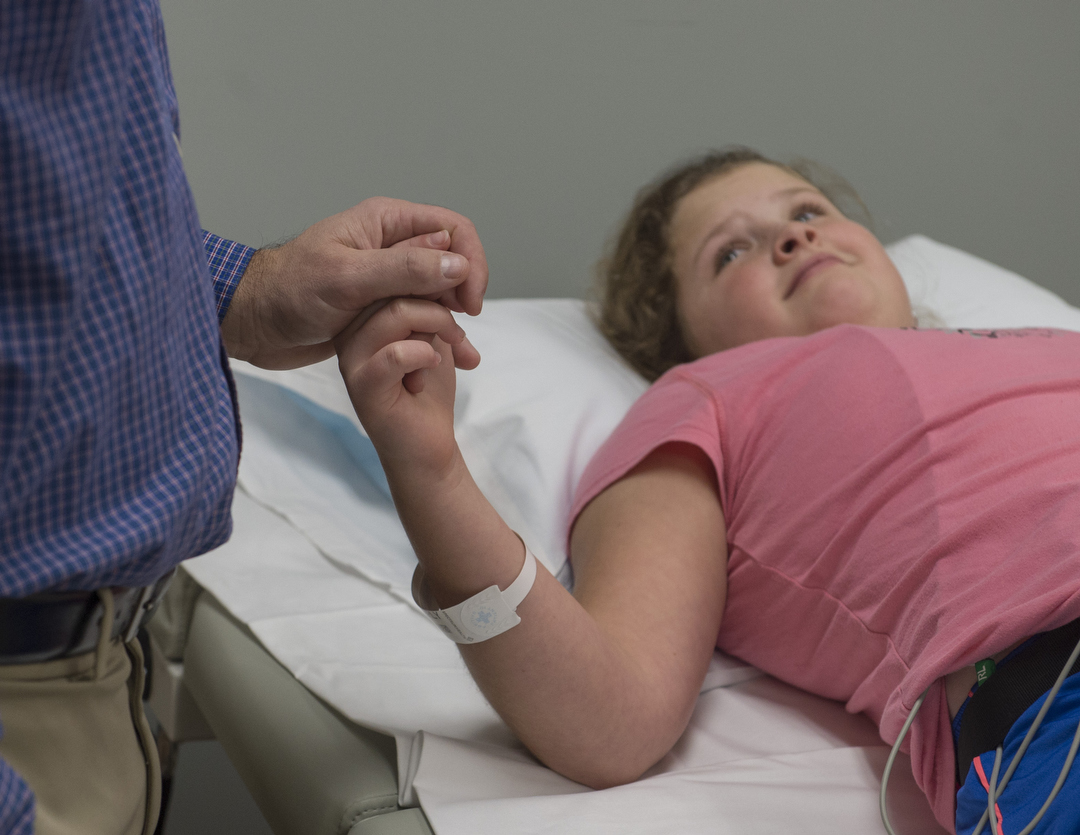
Mary looks at her dad as he recalls that moment. “I cannot imagine you doing that,” she says.
‘Unbelievable’ recovery
As Mary returned to her room after the procedure, a question hung in the air: How would this affect her long-term?
Two days later, they removed the ECMO machine. Mary’s heart continued to beat and pump steadily.
Then, they prepared to remove the ventilator. Kim remembers a nurse cautioning her not to get her hopes too high.
The fact that she survived and is perfect―that’s unbelievable.
“Don’t expect her to open her eyes and say, ‘Mommy,’” she said. “She may not say ‘Mommy’ for two weeks. Or ever again.”
But when the tube was still in, Kim saw Mary mouth the word “Mama.”
And as soon as the tube came out, Mary spoke. “I want to go home,” she said.
She had to learn to walk again. Erick has a video showing her first, painful steps. But her mind remained sharp. Already an avid reader at 7, she enjoyed reading the many cards and letters from home. She even corrected some spelling errors.
The medical team told the Chittles she likely would stay in the hospital two weeks after the procedure. And she would probably need two weeks of therapy at a rehabilitation hospital, as well. She beat both projections.
On March 1, 12½ days after she arrived, she went home from the hospital.
As Mary rebounded, the Chittles heard more than one nurse call her survival a miracle. A doctor told them, “There’s more than medicine going on here. There’s more than science.”
“Honestly, we probably would have said, even if she had major problems afterward, the fact that she survived would have been a miracle,” Dr. Elmouchi says. “The fact that she survived and is perfect―that’s unbelievable.”
The anesthesiologist who cared for Mary during both operations has no doubt about what happened. And the ramifications went beyond one little girl’s heart.
“I met Mary and the Chittles at a point in my life where I had faith in medicine and our abilities as physicians, but very little faith in God,” Dr. Huntington says. “The Chittles’ faith and Mary’s strength were an inspiration that I could not ignore or write off.”
Mary’s recovery pushed him to develop a strong faith.
“I am convinced a miracle happened and a small handful of us were able to witness it,” he said. “Mary’s story changed me forever.”
Five-year follow-up
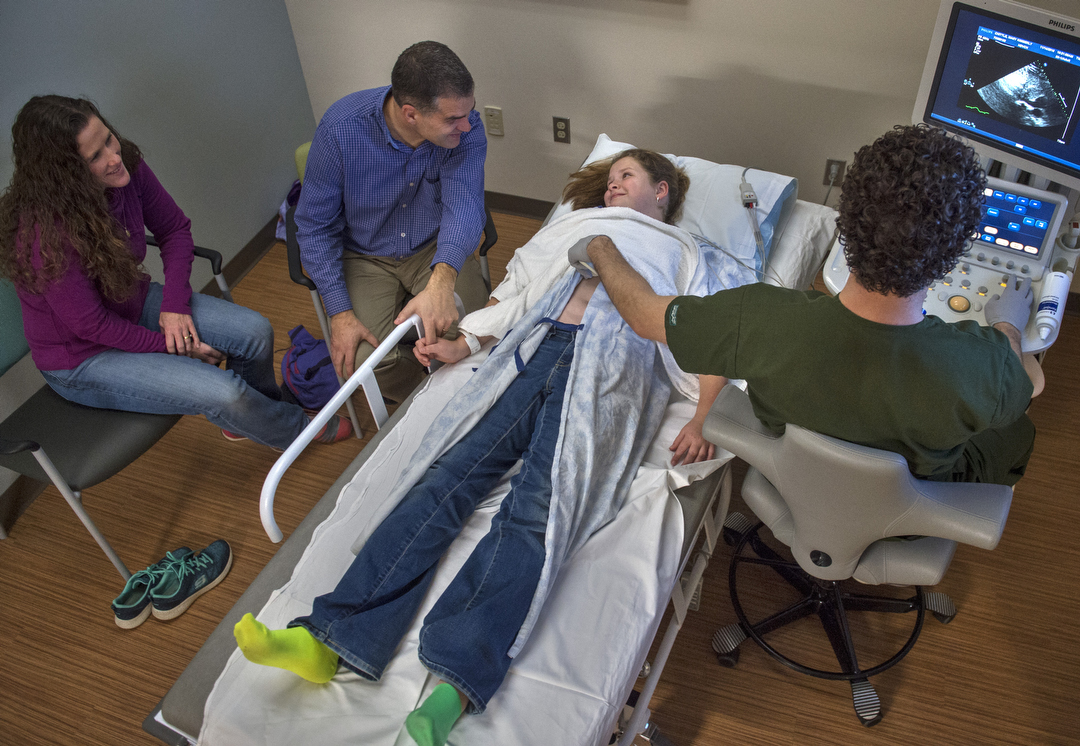
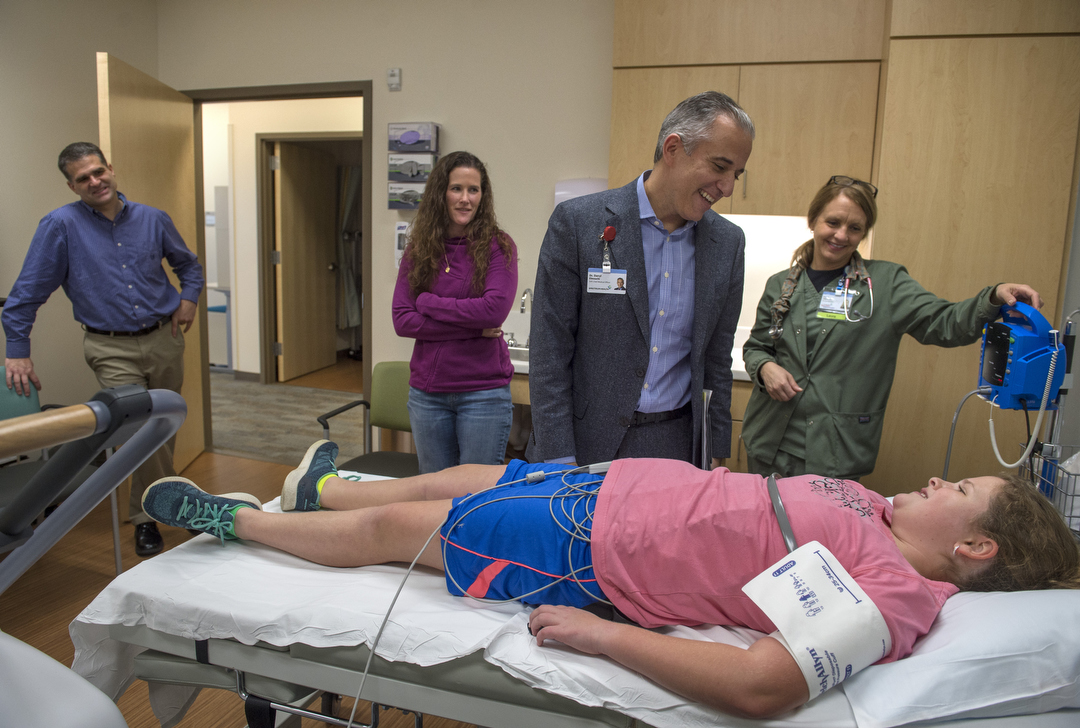
On a recent morning, five years after her heart stopped, Mary returns for a checkup. In an exam room at the Congenital Heart Center at Helen DeVos Children’s Hospital, which didn’t exist when she was younger, she walks on a treadmill for an exercise stress test.
Around her neck hangs a gold chain with a medal of Mary, the mother of Jesus. Her mother gave it to her after the ordeal five years ago. She has worn it ever since.
Dr. Lee asks questions: “Do you ever get a pain in your chest or a pain in your heart? Ever feel your heart beating weird like it’s beating irregularly or fluttering? Ever get dizzy?”
No, no and no, Mary responds.
The test, as well as an ultrasound of her heart, show no problems.
“Amazing,” Dr. Lee says. “Normal function. Normal exercise test. Remarkable.”
Mary still has a hole between the upper chambers of her heart―created as part of the procedure years ago that saved her life―but it’s small and Dr. Lee says it may close on its own over time.
He advises Mary not to scuba dive, but other than that, she has no restrictions on activity. He asks her parents to bring her back in a few years, when she starts high school, for her next checkup.
“The question I’m sure that’s in your head is could the tachycardia come back,” he tells Mary. “I think it’s so unlikely. But if it does, it causes symptoms. You will feel like your heart is racing.”
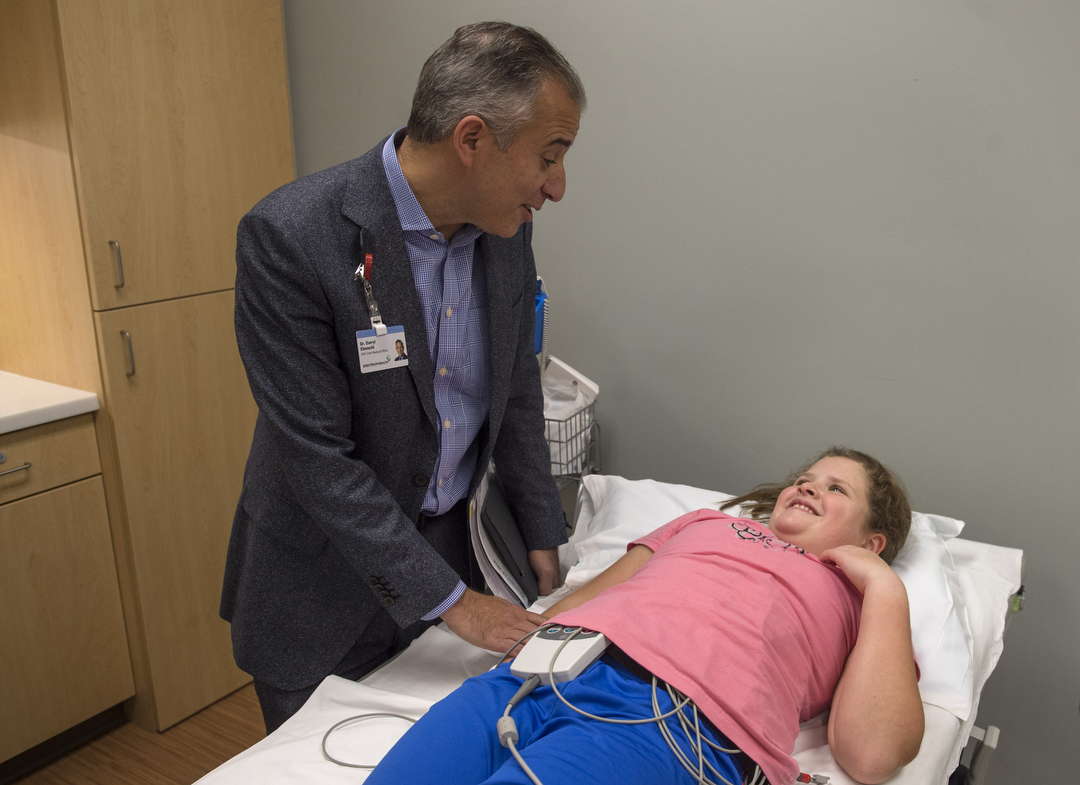
Dr. Elmouchi stops by. He marvels at how much Mary has grown. He asks if she has started driving yet. Mary laughs. “No,” she says.
To see her thriving is deeply rewarding for him.
“Essentially, I could stop working, and I’ve done what I need to do,” he says.
Before returning home, the Chittles have one last stop. They meet Dr. Huntington, Mary’s pediatric anesthesiologist, for a milkshake in the lobby of Helen DeVos Children’s Hospital.
Mary tells him she still has the three stuffed animals he gave her. Each puppy was a reward for a different procedure.
“You are doing so well,” Dr. Huntington says. “You are an inspiration to me.”
As the Chittles prepare to go home, they think back to those days in 2012, when Mary’s life hung in the balance. It was hard to believe then that they would reach this day, when they would return with their healthy, happy daughter for a doctor visit that would feel like a joyful reunion of old friends.
“It sure didn’t seem like it,” Erick says. “It sure didn’t seem like it.”
How do her parents think she survived?
“By the grace of God,” Erick says.
“And the prayers of many people,” Kim says.
Erick nods. “And the wonders of the doctors and nurses there.”





























 /a>
/a>
 /a>
/a>
 /a>
/a>
What an absolutely amazing story!
Agreed, Samantha. 🙂
What a beautiful testimony to His wonders! Thank you for sharing giving glory where it is due, not just to the wonderful medical team (who certainly deserve it!) but to God as well! Prayers for Marys continued healing!
I am sure the Chittles welcome your prayers! Thank you for reading and commenting.
I’ll be sure not to read an article like this while at my desk.. I had to have tissues brought to me 🙂 What an incredible testimony to God’s mercies, and to our incredible team at Spectrum. Thank the Lord for Helen DeVos Children’s Hospital, and for Mary’s incredible recovery.
No worries, Nikolas, we keep tissues handy at our desks, too. We’re so glad you’re a Health Beat ambassador and that you’re a part of the Spectrum Health family. 🙂
Praise be to God and thankfulness to our Blessed Mother, the skilled medical team, and the prayers of the faithful
You would think I’d learn not to read these stories while at work. But I do, every time, and I cry, every time. And think to myself “How amazing to be a part of this world.”
Although these stories are often hard to read, each and every one of them makes me thankful for the life I live, the faith I have, and the opportunity to focus on the good which is all around us if we will only see.
Thank you, Erin, so much for your kind words. We’re glad you are part of the Spectrum Health Beat family! 🙂
Praise and thanks to our Heavenly Father for giving your daughter a true miracle! Thank you for sharing this inspiring and amazing story!
What a wonderful outcome for such a terrible event. Thank you for sharing this with us. I needed to hear this story today. 🙂
Thank you, April! It’s really an honor to be able to share this story!
Thanks for posting this story. So glad this little girl is doing so well. Very uplifting to see the effects of so many coming together to pray for her.
Thank you, Jill! We consider ourselves blessed to be able to share this amazing story on Health Beat! Feel free to share Health Beat with your friends and family members. 🙂
A beautiful story and very well-written. At times I could hardly breathe! Thankful, joyful sobs wanted out. I especially appreciate the moving testimony to God’s presence and power.
Thank you, Harvey for your glowing review of the article. We’re glad to have you as a Health Beat reader!
What a truly moving and inspiring story about the Chittle family! It’s just one of many miracles that happens daily at Helen DeVos Children’s Hospital. It speaks to the power of prayer and the work of angels in our lives. God bless our staff and families!
Thanks be to God in answer to all our desperate prayers to save our twin grandsons at 23 and 1/2 weeks in the womb of our daughter. The setting was the NICU for 5 and 6 months. 13 years and handsome, strong, smart, loving, priceless lives! Can we have higher praise than that given to God and DeVos Children’s Hospital? I think not! Love you all.
Wow! What a wonderful testimonial. Thank you, John, for reading Health Beat and for sharing your family’s journey. So glad your twin grandsons are doing so well! Cheers, Cheryl
John I remember that so well. I was coaching T Ball with Caty and Dave and all of a sudden I am the head coach. Michael and Noah are sure a blessing to the Weitzl family. We sure said a lot of prayers for the family
Wow praise be to god! Prayer is such a powerful tool. So happy for the Chittle Family
God is so good. We remember both situations so well. Lots of prayer warriors out there. Thank you, thank you God for all you do. Frank and Evelyn Tenbusch
Indeed. Thank you so much for reading and commenting.
What a great experience of God’s grace.
Great Docs and God’s leading. How Blessed.
Well written and thanks to the wonderful staff at Helen DeVos Childrens Hospital
This story not only shows how great our God is but also how far SH will go to save a precious life. To move the cath lab into the operating room…took my breath away, not an easy task.
Spectrum Health really does have the ‘best of the best’ of clinicians and support staff.
God is good all time!
What an absolutely remarkable story! Reading this I am struck at how persistent Marys care givers were. How willing Dr. Elmouchi was to go outside convention over and over, even as far as moving the operating room not the patient. Wow! The care for the parents, the fact that Dr. Huntington, I believe was his name, took the video of her heart beating… all of these really just astounding pieces in this story. And after ALL of the hard work of the staff of all the caretakers involved I was thrown off that humbly the doctors gave credit to The Lord!!! Wow!
As Covid continues to rage on, being a part of the Grand Rapids community I have turned to Spectrum for updates, news, and guidelines to follow. Which means Dr. Elamuchi although I’ve never met him, has become a familiar face on my iPhone screen. Hearing this confirms our community is in good hands getting trusted advise!
As a believer in Our Lord I see his soft heart throughout this story willing to be led rather than rigidly sticking within the box.
What a beautiful story! Praising The Lord in how he used so many to heal little Mary.
I feel blessed to have read this story. I work in IT at Corewell and stories like these remind me why I love working here. Thank you for sharing.
well, now i’m crying. as a believer, i read this and i see mary, a pope who agreed to pray and a God who is bigger than any of us will ever understand. of course (absolutely, of course), the team chosen to perform this miracle was the very best. what a beautiful testament to the talent and compassion of our team members at (now) corewell health. just, wow.
This placed a severe and critical condition problem which aims to surge advanced technique which challenges the medical doctor research.